Interventional cardiology represents a rapidly evolving subspecialty within cardiology, dedicated to the diagnosis and treatment of cardiovascular diseases using minimally invasive, catheter-based procedures. Unlike traditional open-heart surgery, interventional cardiologists utilize advanced imaging techniques and specialized instruments introduced through small incisions, typically in the groin or wrist, to access and treat conditions affecting the heart and blood vessels. This approach offers significant advantages, including reduced recovery times, lower risk of complications, and often, a quicker return to normal activities.
The field is characterized by its relentless pursuit of innovation, with new technologies and techniques constantly emerging to address an ever-wider spectrum of cardiac ailments. From opening blocked arteries to repairing faulty heart valves, interventional cardiology plays a pivotal role in improving the lives of millions worldwide. This article delves into the core of interventional cardiology, exploring its fundamental principles, the common procedures performed, the critical technologies that enable these interventions, and the future trajectory of this dynamic medical discipline.
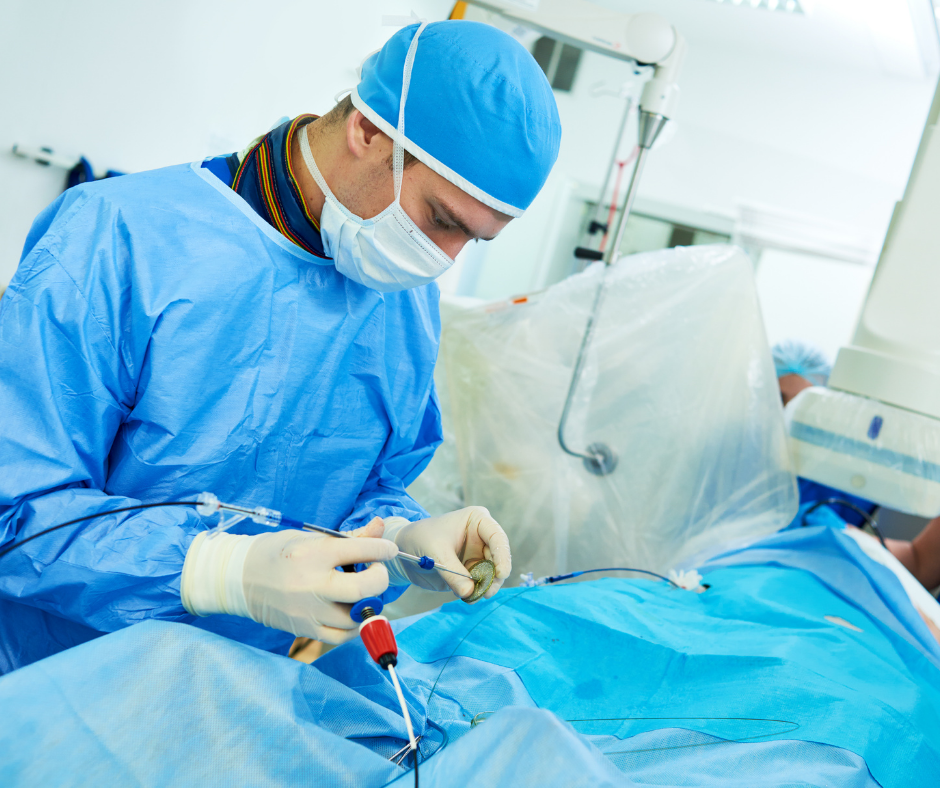
The Pillars of Interventional Cardiology: Diagnosis and Treatment
At its heart, interventional cardiology is about precise diagnosis and effective treatment delivered with minimal invasiveness. The procedures are guided by sophisticated imaging modalities, allowing cardiologists to visualize the intricate structures of the heart and its vasculature in real-time. This detailed insight is crucial for identifying the exact nature and location of the disease, paving the way for tailored and effective interventions.
Diagnostic Coronary Angiography: The Foundation of Intervention
The cornerstone diagnostic procedure in interventional cardiology is coronary angiography. This process involves injecting a contrast dye through a catheter placed in the coronary arteries. X-ray imaging, known as fluoroscopy, then captures the flow of the dye, revealing any blockages, narrowings, or abnormalities within the coronary arteries. The information gathered from angiography is paramount in determining the need for and the type of intervention required. It allows for a clear visualization of the extent of atherosclerotic plaque, the precise location of stenotic lesions, and the overall health of the arterial system. Without this detailed anatomical understanding, performing a targeted intervention would be impossible. Angiography is not merely a diagnostic tool; it is often the prelude to an immediate therapeutic intervention, seamlessly transitioning from assessment to action.
Percutaneous Coronary Interventions (PCIs): Restoring Blood Flow
Percutaneous coronary interventions, commonly known as angioplasty and stenting, are the most frequently performed procedures by interventional cardiologists. These interventions aim to open blocked or narrowed coronary arteries, thereby restoring adequate blood flow to the heart muscle.
Balloon Angioplasty: The Initial Unblocking
The initial step in many PCIs involves balloon angioplasty. A deflated balloon-tipped catheter is guided through the arterial system to the site of the blockage. Once in position, the balloon is inflated, compressing the atherosclerotic plaque against the artery wall and widening the vessel lumen. This immediate widening alleviates the obstruction, improving blood flow. While effective in opening the artery, balloon angioplasty alone can sometimes lead to restenosis, or re-narrowing, of the artery over time.
Coronary Stenting: Providing Support and Patency
To address the issue of restenosis and provide structural support to the opened artery, coronary stents are routinely employed. A stent is a small, mesh-like tube, typically made of metal, which is mounted on the angioplasty balloon. Once the balloon is inflated, the stent expands and is deployed, acting as a scaffold to keep the artery open. Most modern stents are drug-eluting stents (DES), which are coated with medication that is slowly released to prevent the growth of scar tissue within the stent, further reducing the risk of restenosis. The selection of the appropriate stent – its size, type, and drug coating – is a critical decision made by the interventional cardiologist based on the specific characteristics of the lesion and the patient’s individual needs.
Transcatheter Valve Interventions: A Minimally Invasive Revolution
Beyond coronary artery disease, interventional cardiology has revolutionized the treatment of structural heart diseases, particularly valvular heart conditions. Transcatheter valve interventions offer a less invasive alternative to surgical valve repair or replacement for many patients.
Transcatheter Aortic Valve Implantation (TAVI): A Lifesaving Alternative
Transcatheter aortic valve implantation (TAVI), also known as transcatheter aortic valve replacement (TAVR), has emerged as a groundbreaking treatment for severe aortic stenosis, a condition where the aortic valve narrows, restricting blood flow from the heart. In TAVI, a new artificial valve is delivered via a catheter, usually through the femoral artery in the groin, and deployed within the diseased aortic valve. This procedure has provided a vital option for patients who are at high surgical risk or are not candidates for traditional open-heart surgery, significantly improving their quality of life and longevity. The development of various catheter-based delivery systems and valve designs has made TAVI an increasingly refined and accessible procedure.
Mitral Valve Repair and Replacement: Expanding the Frontier
Interventional cardiology is also making significant strides in treating mitral valve disease. Transcatheter mitral valve repair techniques, such as MitraClip, involve clipping together the leaflets of the mitral valve to reduce leakage (regurgitation). For patients with severe mitral regurgitation who are not candidates for surgery, these procedures offer a valuable therapeutic option. While still under development compared to TAVI, transcatheter mitral valve replacement is also progressing rapidly, promising to further expand the interventional cardiologist’s armamentarium.
The Technological Arsenal: Tools of Precision
The success of interventional cardiology hinges on a sophisticated array of technologies that enable precise navigation, visualization, and intervention within the complex cardiovascular system. These tools have been instrumental in transforming what was once considered the domain of major surgery into a field of minimally invasive precision.
Catheters and Guidewires: Navigating the Vascular Landscape
Catheters are flexible tubes of varying sizes and materials, serving as the primary conduits for delivering other instruments to the target site. Guidewires are ultra-thin, flexible wires used to guide catheters through the tortuous paths of the blood vessels. Interventional cardiologists possess a vast selection of catheters and guidewires, each designed for specific anatomical challenges and procedural requirements. The ability to skillfully manipulate these tools, often navigating through heavily calcified or severely tortuous vessels, is a hallmark of an experienced interventional cardiologist. The development of hydrophilic coatings for guidewires, for example, reduces friction and facilitates passage through tight constrictions.
Imaging Modalities: Visualizing the Invisible
Accurate visualization is paramount for safe and effective interventional procedures. Several advanced imaging modalities are employed to guide the interventions:
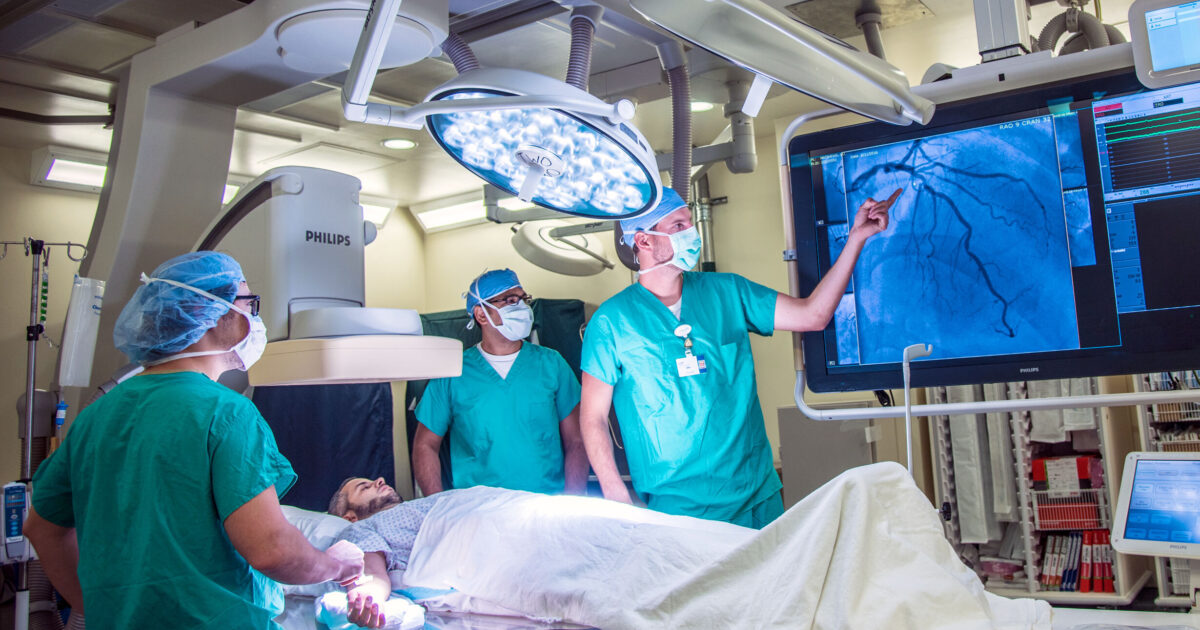
Fluoroscopy: Real-Time X-ray Guidance
Fluoroscopy is the most fundamental imaging technique used in interventional cardiology. It provides real-time, dynamic X-ray images, allowing the cardiologist to visualize the catheters, guidewires, and contrast dye as they move through the vascular system. While crucial, fluoroscopy involves radiation exposure, and interventionalists employ strategies to minimize this, such as using low-dose settings and shielding.
Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT): Peering Inside the Artery
To gain a more detailed, cross-sectional view of the coronary arteries, intravascular ultrasound (IVUS) and optical coherence tomography (OCT) are utilized. IVUS uses sound waves to create images of the arterial wall, providing information about plaque composition, vessel size, and the precise placement of stents. OCT, a more advanced imaging technique, uses light waves to generate ultra-high-resolution images, allowing for detailed visualization of plaque morphology, stent struts, and intimal hyperplasia. These intravascular imaging techniques are invaluable for optimizing stent deployment, assessing the adequacy of lesion coverage, and identifying potential complications that might not be apparent on fluoroscopy alone.
Echocardiography: Assessing Heart Function and Structure
Echocardiography, particularly transesophageal echocardiography (TEE) and intracardiac echocardiography (ICE), plays a crucial role in visualizing the heart’s chambers, valves, and overall function. TEE involves inserting a transducer into the esophagus, providing clear images of the heart’s posterior structures. ICE uses a catheter-based transducer inserted directly into the heart or nearby blood vessels, offering real-time visualization during complex structural interventions like TAVI and mitral valve repairs. This allows for precise guidance of device deployment and assessment of the procedural outcomes.
Specialized Devices and Technologies: From Balloons to Biologics
Beyond the basic tools, interventional cardiology employs a vast array of specialized devices and innovative technologies:
Atherectomy Devices: Debulking Plaque
In cases of heavily calcified lesions where balloon angioplasty alone may be insufficient or carry a higher risk, atherectomy devices are used to remove or debulk the obstructive plaque. These devices, which include rotational atherectomy (e.g., Rotablator) and orbital atherectomy, use specialized burrs or blades to grind away calcified material, preparing the artery for subsequent stenting.
Percutaneous Mechanical Circulatory Support (MCS): Bridging to Recovery
During high-risk interventional procedures or in cases of cardiogenic shock, temporary mechanical circulatory support devices can be used to assist the heart’s pumping function. Devices like the Impella heart pump, which is a miniature ventricular assist device inserted via catheter, can provide significant hemodynamic support, allowing the heart to rest and recover or serving as a bridge to definitive treatment or recovery.
Thrombectomy Devices: Clearing Clots
In acute ischemic events like ST-elevation myocardial infarction (STEMI), rapid reperfusion is critical. Thrombectomy devices are used to physically remove blood clots from occluded coronary arteries, restoring blood flow quickly. These devices range from simple aspiration catheters to more advanced mechanical thrombectomy systems.
The Future of Interventional Cardiology: Innovation on the Horizon
The field of interventional cardiology is characterized by its dynamic nature and a constant drive for innovation. Future advancements are poised to further refine existing procedures, expand the scope of interventional treatments, and improve patient outcomes even more dramatically.
Artificial Intelligence and Machine Learning: Enhancing Decision-Making and Precision
Artificial intelligence (AI) and machine learning are increasingly being integrated into interventional cardiology. AI algorithms can analyze large datasets of patient information, imaging studies, and procedural outcomes to predict risks, optimize treatment strategies, and even assist in real-time procedural guidance. From predicting stent thrombosis to identifying optimal landing zones for transcatheter valves, AI promises to augment the skills of interventional cardiologists, leading to more personalized and effective care. Machine learning can also be applied to analyze angiographic images, identifying subtle abnormalities and quantifying lesion severity with greater accuracy.
Advanced Imaging and Sensing: Unprecedented Insights
The development of next-generation imaging technologies will provide even deeper insights into cardiovascular anatomy and physiology. Innovations in intravascular imaging, such as improved resolution and functional assessment capabilities, will enable more precise lesion characterization and treatment planning. Furthermore, the integration of novel sensors into catheters could allow for real-time measurement of parameters like blood flow, pressure, and tissue oxygenation, providing a comprehensive understanding of the cardiovascular environment during interventions.
Biologics and Novel Biomaterials: Beyond Metal Scaffolds
The future of stenting is likely to move beyond traditional metal scaffolds. Research is actively progressing on bioresorbable vascular scaffolds (BVS), which are designed to degrade over time after the artery has healed, potentially reducing long-term complications associated with permanent metallic stents. Additionally, the development of novel biomaterials for valves and other structural heart devices aims to improve durability, reduce thrombogenicity, and enhance biocompatibility. Gene therapy and regenerative medicine approaches are also being explored as potential future avenues for treating cardiovascular diseases, potentially working in conjunction with interventional techniques.

Expansion into New Therapeutic Arenas: Broadening the Scope
Interventional cardiology is continually expanding its reach into new therapeutic areas. Beyond coronary and valvular heart disease, interventionalists are increasingly involved in treating complex congenital heart defects in adults, managing pulmonary hypertension, and addressing peripheral vascular diseases. The development of new devices and techniques will further broaden the scope of conditions treatable through minimally invasive catheter-based approaches, offering hope and improved quality of life to a wider patient population. The integration of robotics in interventional procedures also holds promise for enhancing precision and enabling remote interventions.
In conclusion, interventional cardiology stands as a testament to human ingenuity in combating cardiovascular disease. Through its dedication to precision, minimally invasive techniques, and a relentless embrace of technological advancements, it has transformed the landscape of cardiac care, offering hope and improved outcomes for countless individuals. As the field continues to evolve, the future promises even more sophisticated and life-saving interventions, further solidifying its vital role in modern medicine.
