Human Papillomavirus (HPV) screening refers to medical tests used to detect the presence of the human papillomavirus, a common group of viruses that can cause various health problems, including cervical cancer, genital warts, and other cancers. The primary focus of HPV screening is to identify high-risk HPV infections in women, as these infections are the leading cause of cervical cancer. Early detection through HPV screening allows for timely intervention, significantly reducing the risk of developing precancerous lesions and invasive cancer. This proactive approach has revolutionized cervical cancer prevention, shifting the paradigm from treatment to early detection and management.
Understanding HPV and Its Impact
Human Papillomavirus is a diverse group of over 200 related viruses, with more than 40 of them being spread through sexual contact. While many HPV infections are transient and clear on their own without causing any health issues, certain high-risk HPV types can persist and lead to cellular changes. These changes, if left undetected and untreated, can progress over years to become cancerous. The most well-known and significant consequence of persistent high-risk HPV infection is cervical cancer. However, high-risk HPV types are also associated with vulvar, vaginal, penile, anal, and oropharyngeal (throat) cancers. Low-risk HPV types, on the other hand, are typically responsible for the development of genital warts.
The Nature of HPV Infections
HPV is incredibly common. In fact, most sexually active individuals will contract HPV at some point in their lives, though they may never know it. The virus is spread through skin-to-skin contact, most commonly during vaginal, anal, or oral sex. It’s important to note that HPV can be transmitted even when an infected person has no visible warts or symptoms. The immune system is usually capable of clearing most HPV infections within two years. However, in a minority of cases, the infection can persist. It is these persistent infections with specific high-risk HPV types that pose a threat and are the target of screening efforts.
The Link Between HPV and Cancer
The oncogenic (cancer-causing) potential of certain HPV types lies in their ability to interfere with the normal cell cycle and DNA repair mechanisms. Specifically, the E6 and E7 proteins produced by high-risk HPV types can inactivate tumor suppressor proteins like p53 and Rb, respectively. This inactivation disrupts the cell’s ability to regulate its growth and division, leading to uncontrolled proliferation and the accumulation of genetic mutations. Over time, these cellular abnormalities can develop into precancerous lesions, and eventually, invasive cancer. The progression from initial HPV infection to detectable cancer typically occurs over many years, providing a crucial window for screening and intervention.
The Role and Methods of HPV Screening
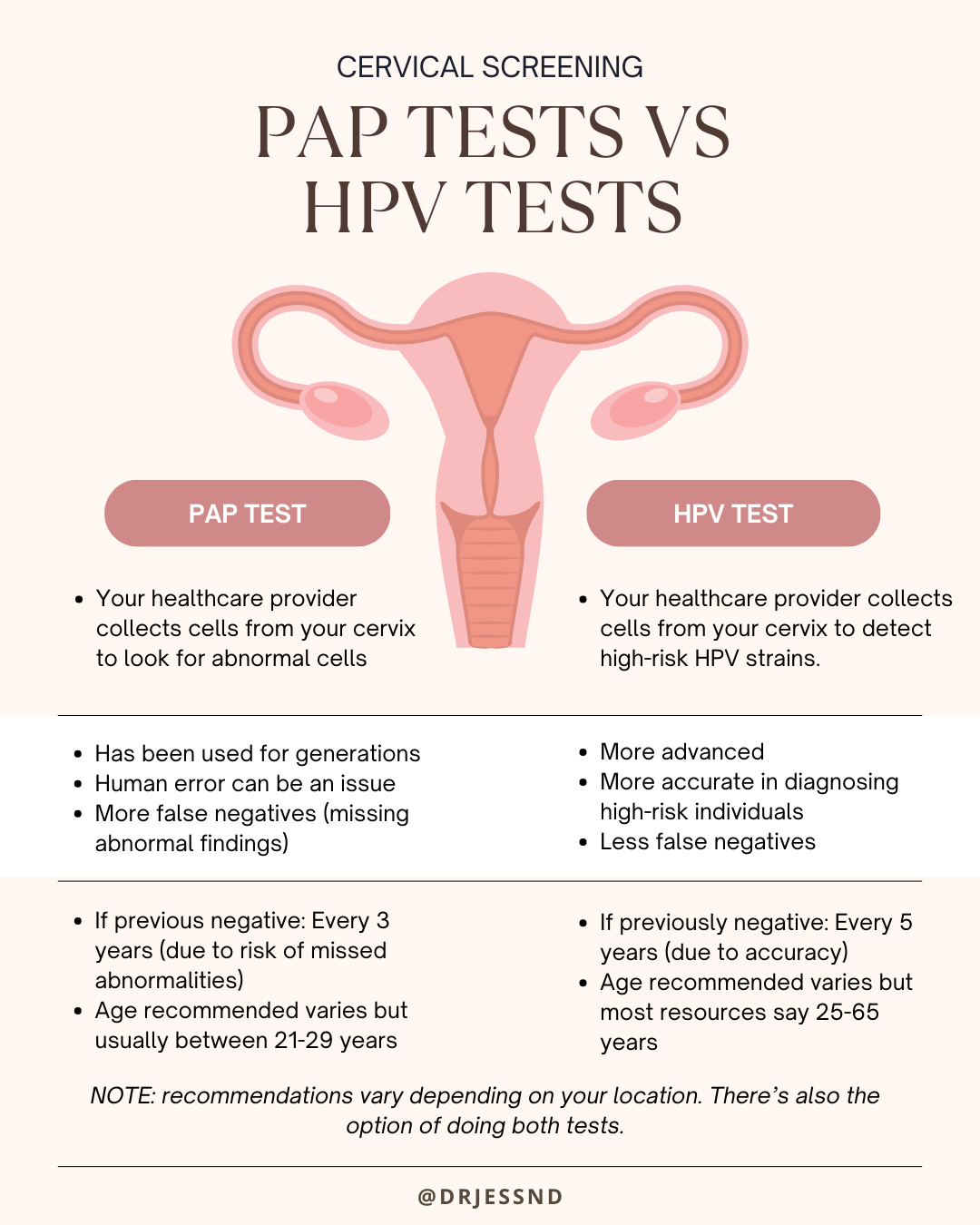
HPV screening is a vital component of cervical cancer prevention strategies worldwide. It complements or, in some cases, replaces traditional Pap smears (cytology) as the primary method for detecting cervical abnormalities. The effectiveness of HPV screening lies in its ability to directly identify the presence of the virus that causes these abnormalities. This proactive approach allows healthcare providers to identify women at higher risk for developing cervical cancer and to manage them accordingly, often with less invasive procedures than might be required if cancer had already developed.
Primary HPV Testing
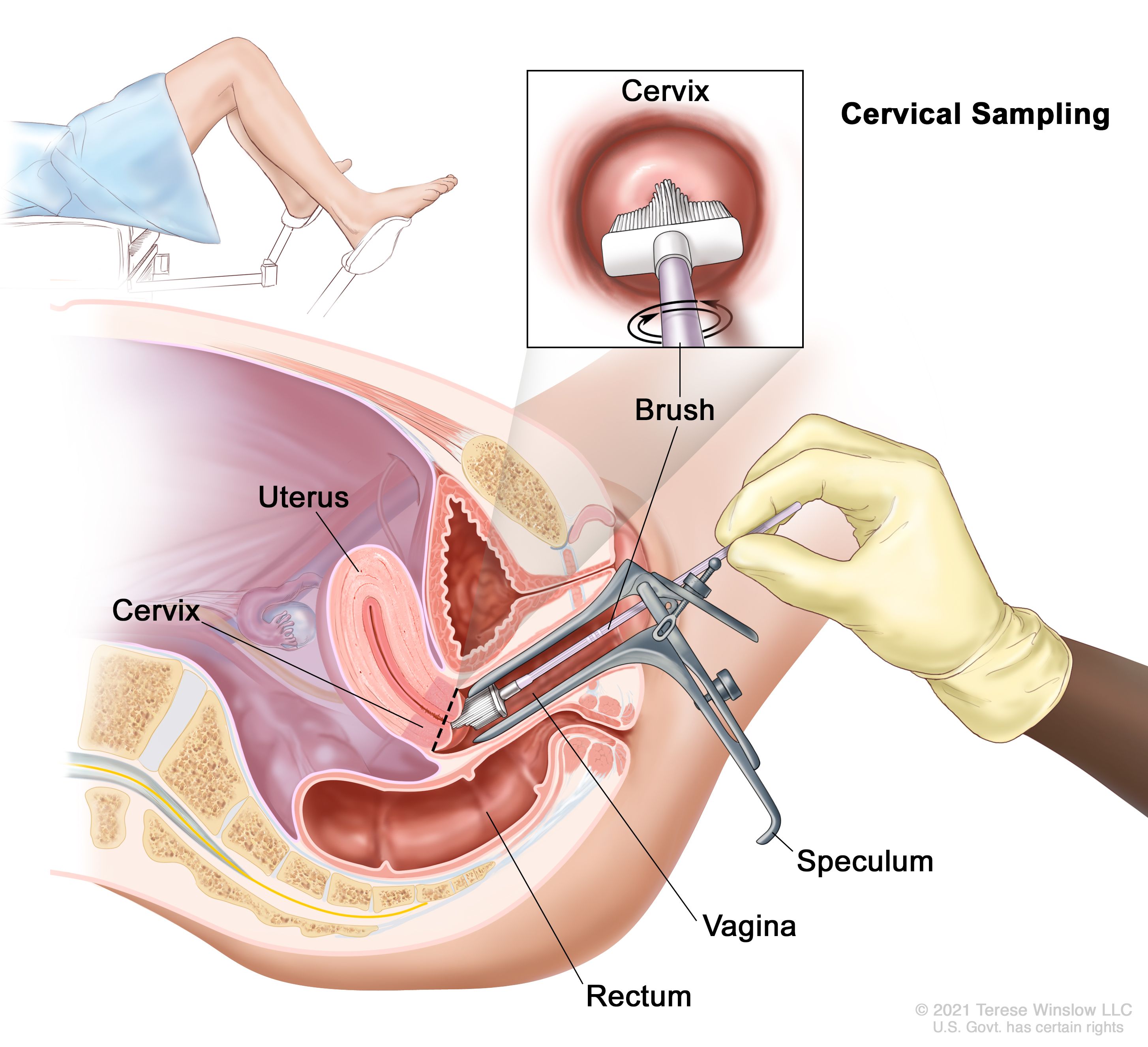
Primary HPV testing is now the preferred method for cervical cancer screening in many countries. This involves directly testing a sample of cervical cells for the presence of DNA or RNA from high-risk HPV types. Unlike a Pap smear, which looks for abnormal cell changes that may or may not be caused by HPV, HPV testing directly detects the virus itself. If a high-risk HPV type is detected, further evaluation is typically recommended. This can involve a co-test with a Pap smear or direct referral for colposcopy (a visual examination of the cervix with a magnifying instrument) and biopsy if necessary. The advantage of primary HPV testing is its high sensitivity in detecting precancerous lesions.
HPV Co-testing
HPV co-testing involves performing both an HPV test and a Pap smear on the same sample of cervical cells. This method was a significant advancement over Pap smears alone and remains a recommended screening strategy for certain age groups and in certain healthcare settings. Co-testing combines the ability of HPV testing to identify the presence of the virus with the ability of the Pap smear to detect cellular abnormalities. If either test is positive for high-risk HPV or shows abnormal cells, further investigation is warranted. This approach provides a comprehensive assessment of cervical health.
Self-Collection for HPV Testing
A significant development in HPV screening has been the introduction of self-collection kits. These kits allow women to collect their own vaginal or cervical sample in the privacy of their own home. The collected sample is then mailed to a laboratory for HPV testing. This innovation is particularly impactful for individuals who face barriers to traditional clinic-based screening, such as those in remote areas, those with limited mobility, or those who feel uncomfortable with pelvic exams. Self-collection increases accessibility and can improve screening rates, thereby reaching more women and potentially saving lives.
Interpreting HPV Screening Results and Next Steps
The results of an HPV screening test are crucial in determining the appropriate course of action for a woman’s cervical health management. Understanding what a positive or negative result signifies, and what the subsequent recommendations are, empowers individuals to engage actively in their healthcare. The goal of screening is not to diagnose cancer but to identify individuals who are at increased risk and require further monitoring or treatment.

Negative HPV Test Results
A negative HPV test result, especially when performed as primary HPV testing or co-testing, is generally reassuring. It indicates that high-risk HPV types were not detected in the sample. For most individuals, this means their risk of developing cervical cancer in the near future is very low. The recommended follow-up for a negative HPV test is typically routine screening at the next recommended interval, as advised by their healthcare provider and based on national guidelines. This interval is usually several years, reflecting the slow progression of cervical cancer.
Positive HPV Test Results
A positive HPV test result indicates the presence of one or more high-risk HPV types. It is important to remember that a positive HPV test does not mean a woman has cancer. It signifies a higher risk of developing precancerous changes or cancer in the future. The specific management plan following a positive HPV test depends on several factors, including the type of HPV detected (if the test differentiates between specific high-risk types), the results of any co-tested Pap smear, the woman’s age, and her medical history.
Follow-up for Positive HPV Results
When a high-risk HPV type is detected, the next step typically involves further evaluation to assess for any cervical cell changes. This may include:
- Repeat HPV Testing: Sometimes, a follow-up HPV test may be recommended in 6-12 months to see if the infection has cleared on its own, as many HPV infections do.
- Pap Smear: If a Pap smear was not performed concurrently, it might be recommended.
- Colposcopy: This is the most common next step. A colposcopy allows a healthcare provider to examine the cervix closely with a magnifying instrument called a colposcope. During the procedure, a solution is applied to the cervix that highlights any abnormal areas.
- Biopsy: If abnormal areas are identified during colposcopy, a small tissue sample (biopsy) will be taken for examination under a microscope. This biopsy is crucial for determining if precancerous changes (dysplasia) or cancer is present and, if so, its severity.
Managing Precancerous Lesions
If precancerous lesions are identified through colposcopy and biopsy, treatment is highly effective in preventing them from progressing to cancer. The type of treatment depends on the grade of the lesion and the individual’s circumstances. Common treatment options include:
- Loop Electrosurgical Excision Procedure (LEEP): This procedure uses a heated wire loop to remove abnormal tissue.
- Cryotherapy: This involves freezing and destroying abnormal cells.
- Cold Knife Cone Biopsy: This is a more extensive surgical procedure to remove a cone-shaped piece of abnormal tissue.
Regular follow-up after treatment is essential to ensure that the lesions have been completely removed and to monitor for any recurrence.
Advancements and Future Directions in HPV Screening
The field of HPV screening is continuously evolving, driven by a desire to improve accuracy, accessibility, and patient outcomes. Technological advancements and ongoing research are shaping the future of cervical cancer prevention, making screening more effective and less burdensome.
Improved HPV Test Technologies
Research is ongoing to develop even more precise and comprehensive HPV testing methods. This includes the development of tests that can identify specific high-risk HPV types with greater accuracy, allowing for more tailored management strategies. Furthermore, there is work being done to develop tests that can detect other biomarkers associated with precancerous changes, potentially improving the specificity of screening and reducing unnecessary follow-up procedures. The goal is to identify individuals at highest risk for progression to cancer while minimizing over-diagnosis and overtreatment.
Integration with Other Health Data
The future of HPV screening may involve its integration with other health data and technologies. For example, artificial intelligence (AI) is being explored to analyze Pap smear images and HPV test results, potentially improving diagnostic accuracy and identifying subtle patterns that might be missed by human review alone. Additionally, electronic health records can play a crucial role in tracking screening histories, managing follow-up appointments, and ensuring that individuals receive timely care. This integrated approach promises a more holistic and efficient approach to cervical health management.
Expanding Screening Guidelines and Accessibility
As HPV screening proves its effectiveness, guidelines are being updated to reflect the optimal age to start and stop screening, as well as the recommended screening intervals. There is also a growing emphasis on expanding access to HPV screening, particularly in underserved populations. Initiatives like self-collection kits are key to this effort, aiming to remove barriers and ensure that all women have the opportunity to be screened and protected against cervical cancer. The ultimate aim is to eliminate cervical cancer as a public health problem through comprehensive screening and vaccination strategies.
