When experiencing constipation, the desire for relief is paramount. Understanding the different types of laxatives available, their mechanisms of action, and how to choose the most appropriate option is crucial for effective and safe management of this common digestive issue. This article aims to demystify the world of laxatives, guiding you towards an informed decision for your specific needs.
Understanding Constipation and Its Causes
Before delving into laxative options, it’s essential to grasp what constitutes constipation and the factors that contribute to it.
Defining Constipation
Constipation is generally defined as having infrequent bowel movements, typically fewer than three per week, or experiencing difficulty passing stools that are hard, dry, or lumpy. While the frequency can vary slightly from person to person, significant deviations from one’s usual pattern can signal constipation. Symptoms often include straining during bowel movements, a feeling of incomplete evacuation, and abdominal discomfort or bloating.
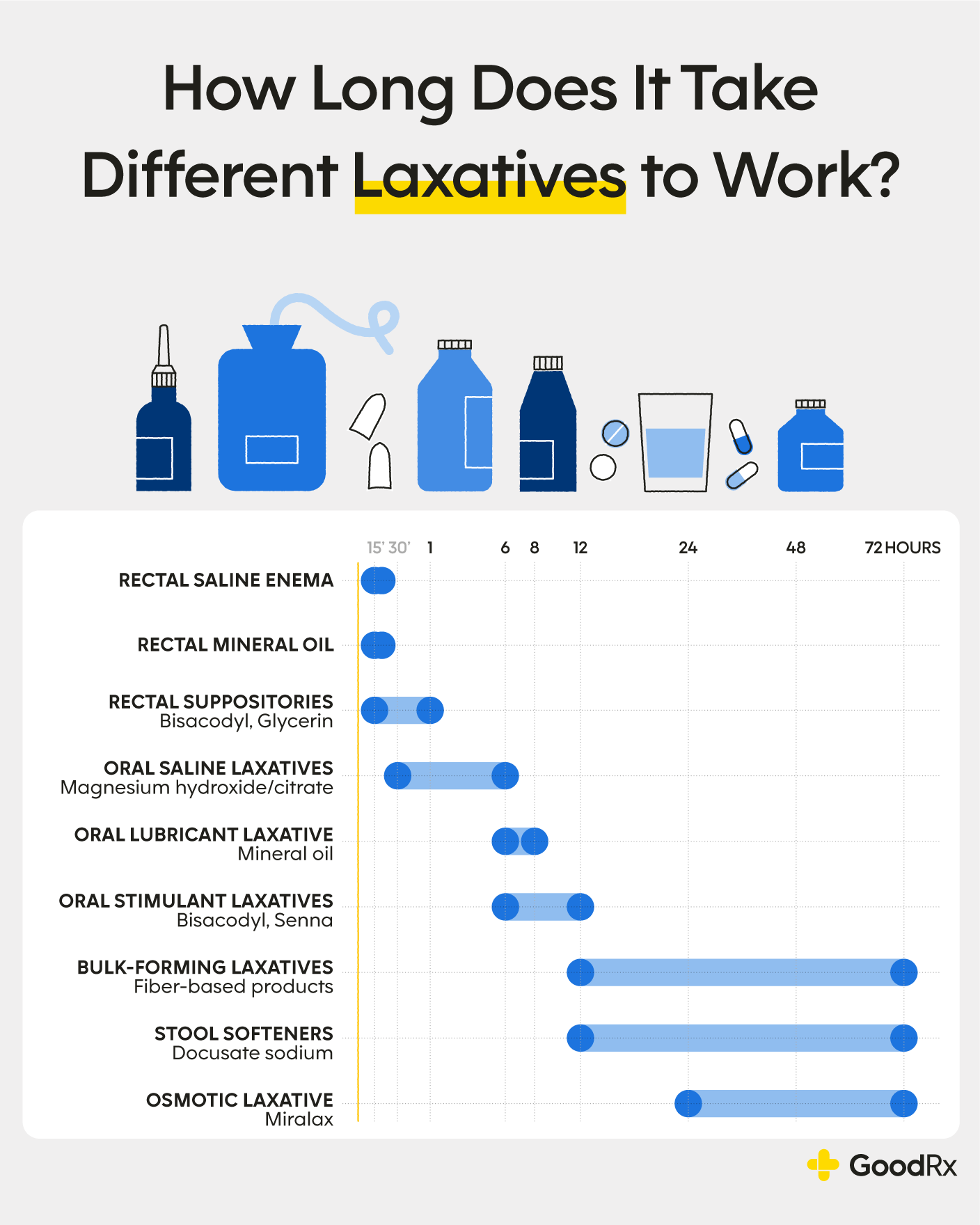
Common Causes of Constipation
A multitude of factors can lead to constipation. Recognizing these causes can be the first step in addressing the issue and may even prevent the need for laxatives in some cases.
Dietary Factors
- Low Fiber Intake: Fiber adds bulk to stool and helps it retain water, making it softer and easier to pass. A diet lacking in fruits, vegetables, and whole grains is a frequent culprit.
- Inadequate Fluid Intake: Water is essential for softening stool. Insufficient hydration can lead to harder, more difficult-to-pass stools.
- Changes in Eating Habits: Traveling, illness, or significant dietary shifts can disrupt normal bowel function.
Lifestyle Factors
- Lack of Physical Activity: Exercise stimulates intestinal muscle activity, aiding in the movement of waste through the colon. A sedentary lifestyle can slow down this process.
- Ignoring the Urge to Defecate: Regularly postponing bowel movements can lead to the stool becoming harder and more difficult to pass. The body may also become less responsive to the urge over time.
- Stress and Mental Health: The gut-brain axis is a complex connection, and stress, anxiety, and depression can significantly impact digestive regularity.
Medical Conditions and Medications
- Irritable Bowel Syndrome (IBS): While IBS can manifest with diarrhea, constipation-predominant IBS is also common.
- Neurological Disorders: Conditions affecting the nerves that control the intestines, such as Parkinson’s disease or multiple sclerosis, can impair bowel function.
- Hormonal Imbalances: Thyroid problems, particularly hypothyroidism, can slow down metabolism and digestive processes.
- Medications: Numerous medications can cause constipation as a side effect. These include opioid pain relievers, certain antidepressants, iron supplements, antacids containing aluminum or calcium, and some blood pressure medications.
Types of Laxatives and How They Work
Laxatives are broadly categorized based on their mechanism of action. Understanding these distinctions is key to selecting the most appropriate type for your situation.
Bulk-Forming Laxatives
These laxatives work by mimicking the action of dietary fiber. They absorb water in the intestines, swelling to create a softer, bulkier stool that is easier to pass.
- Mechanism: They increase the volume of stool, which distends the colon wall, stimulating peristalsis (muscle contractions that move stool along).
- Examples: Psyllium (Metamucil), methylcellulose (Citrucel), polycarbophil (FiberCon).
- Onset of Action: Typically 12 to 72 hours.
- Considerations: It’s crucial to drink plenty of water when taking bulk-forming laxatives to prevent the risk of obstruction. They are generally considered safe for long-term use if needed.
Osmotic Laxatives
Osmotic laxatives draw water into the colon from surrounding tissues, softening the stool and increasing its volume.
- Mechanism: They work by retaining water in the intestinal lumen, making the stool softer and easier to expel.
- Examples:
- Saline Osmotics: Magnesium citrate, magnesium hydroxide (Milk of Magnesia), polyethylene glycol (MiraLAX).
- Sugar-Based Osmotics: Lactulose, sorbitol.
- Onset of Action: Can range from 30 minutes to 3 days, depending on the specific product and dosage. Polyethylene glycol generally takes 1 to 3 days.
- Considerations: Saline osmotics should be used with caution in individuals with kidney problems, as they can lead to electrolyte imbalances. They are generally effective for short-term relief. Polyethylene glycol is often recommended for longer-term management.
Stimulant Laxatives

Stimulant laxatives work by directly stimulating the nerves in the intestinal wall, causing muscles to contract and move stool along more quickly.
- Mechanism: They irritate the intestinal lining, triggering increased peristalsis and muscle contractions.
- Examples: Bisacodyl (Dulcolax), senna (Ex-Lax, Senokot).
- Onset of Action: Typically 6 to 12 hours.
- Considerations: Stimulant laxatives are generally intended for short-term use only. Chronic use can lead to dependency, where the bowels become reliant on the laxative to function, and can also cause electrolyte disturbances and damage to the intestinal nerves.
Stool Softeners (Emollients)
Stool softeners add moisture to the stool, making it softer and easier to pass without straining. They don’t stimulate bowel movements but rather make the process more comfortable.
- Mechanism: They facilitate the mixing of water and fats within the stool, thus softening it.
- Examples: Docusate sodium (Colace), docusate calcium.
- Onset of Action: Can take 1 to 3 days.
- Considerations: Stool softeners are often recommended after surgery or childbirth to prevent straining. They are generally considered gentle and safe for regular use.
Lubricant Laxatives
These laxatives coat the stool and the intestinal lining with a waterproof film, preventing water from being absorbed from the stool and making it easier to pass.
- Mechanism: They lubricate the stool, allowing it to move more smoothly through the intestines.
- Examples: Mineral oil.
- Onset of Action: Typically 6 to 8 hours.
- Considerations: Oral mineral oil should be used with caution as it can interfere with the absorption of fat-soluble vitamins (A, D, E, K) and can cause anal leakage. It is also associated with a risk of aspiration pneumonitis if accidentally inhaled. It is generally recommended for occasional use.
Choosing the Right Laxative for Your Needs
The “best” laxative is a subjective choice that depends on several factors, including the severity and duration of your constipation, your overall health, and any underlying medical conditions.
Factors to Consider When Selecting a Laxative
- Severity and Duration of Constipation: For mild, occasional constipation, dietary changes and bulk-forming laxatives or stool softeners might be sufficient. For more severe or persistent constipation, an osmotic laxative might be more effective. Stimulant laxatives are typically reserved for more stubborn cases and for short-term use.
- Underlying Health Conditions: Individuals with kidney disease, heart failure, or diabetes should consult their doctor before using certain laxatives, particularly saline osmotics, due to potential electrolyte imbalances. Pregnant or breastfeeding individuals should also seek medical advice.
- Medication Interactions: Always inform your doctor or pharmacist about all medications and supplements you are taking, as some laxatives can interact with them.
- Personal Preference and Tolerance: Some individuals may find certain laxatives cause more cramping or discomfort than others. It may take some trial and error to find one that works best for you.
When to Consult a Healthcare Professional
While most cases of constipation can be managed with over-the-counter options, it’s crucial to seek medical attention if you experience any of the following:
- Sudden onset of constipation or a significant change in bowel habits.
- Constipation lasting longer than two weeks.
- Severe abdominal pain, cramping, or bloating.
- Blood in your stool or rectal bleeding.
- Unexplained weight loss.
- Vomiting.
- Inability to pass gas.
- A feeling of incomplete bowel evacuation that persists.
A healthcare professional can help identify the underlying cause of your constipation and recommend the most appropriate treatment plan, which may include prescription medications, lifestyle modifications, or further diagnostic testing.
Lifestyle Modifications and Preventative Measures
While laxatives offer effective relief, addressing the root causes of constipation through lifestyle changes can prevent recurrence and promote long-term digestive health.
Dietary Strategies for Bowel Regularity
- Increase Fiber Intake Gradually: Aim for 25-30 grams of fiber per day. Incorporate more fruits (berries, apples, pears), vegetables (broccoli, carrots, leafy greens), legumes (beans, lentils), and whole grains (oatmeal, brown rice, whole wheat bread).
- Stay Hydrated: Drink plenty of water throughout the day. Aim for at least 8 glasses (64 ounces) of water daily, and more if you are physically active or in a warm climate. Other fluids like herbal teas and clear broths also contribute.
- Consider Probiotics: Foods rich in probiotics, such as yogurt with live and active cultures, kefir, and fermented vegetables, can support a healthy gut microbiome, which may aid in digestion.
The Importance of Physical Activity and Routine
- Regular Exercise: Engage in at least 30 minutes of moderate-intensity exercise most days of the week. Walking, jogging, swimming, and yoga are all beneficial for stimulating bowel function.
- Establish a Bowel Routine: Try to have a bowel movement at the same time each day, preferably after a meal when the digestive system is naturally more active. Don’t ignore the urge to defecate.
- Manage Stress: Explore stress-reduction techniques such as meditation, deep breathing exercises, or spending time in nature. Chronic stress can negatively impact gut health.

When Laxatives Are Not the Solution
It’s important to remember that laxatives are a tool for symptom relief, not a cure for underlying conditions. Over-reliance on laxatives can lead to dependency and mask more serious medical issues. By implementing sustainable lifestyle changes and seeking professional guidance when needed, you can achieve and maintain healthy, regular bowel function.
