The human spine is a marvel of biological engineering, providing both structural support and incredible flexibility. At its core, this intricate system relies on a series of interconnected bones called vertebrae. Between each vertebra, nestled on the posterior aspect, are pairs of small, synovial joints known as facet joints. These joints, much like the more familiar joints in your knees or hips, are lined with cartilage and lubricated by synovial fluid, allowing for smooth, controlled movement of the spine. However, like any joint in the body, facet joints are susceptible to injury, inflammation, and degeneration, leading to chronic pain that can significantly impact a person’s quality of life. This is where a facet joint injection comes into play, offering a targeted therapeutic intervention.

A facet joint injection is a minimally invasive medical procedure designed to diagnose and treat pain originating from these specific spinal joints. It involves injecting a therapeutic solution directly into the facet joint capsule or the surrounding nerves that transmit pain signals from the joint. This procedure serves a dual purpose: diagnostically, by identifying which facet joint is the source of pain, and therapeutically, by delivering medication to reduce inflammation and alleviate discomfort. Understanding the anatomy of the facet joint, the reasons for the injection, the procedure itself, and the potential benefits and risks is crucial for anyone considering this treatment option.
Anatomy and Function of the Facet Joints
To fully appreciate the role of a facet joint injection, it’s essential to first grasp the fundamental anatomy and biomechanical function of the facet joints themselves. These paired joints are located on either side of the posterior aspect of each vertebra, forming a crucial part of the spinal column’s structural integrity and range of motion.
The Structure of a Facet Joint
Each facet joint is a true synovial joint, meaning it possesses a joint capsule, articular cartilage, and synovial fluid. The joint capsule is a fibrous sac that encloses the joint, providing stability. The articular surfaces of the vertebrae, known as facet facets, are covered by hyaline cartilage, a smooth, resilient tissue that allows for low-friction movement. This cartilage acts as a shock absorber and facilitates gliding between the bony surfaces. The synovial membrane lines the inner surface of the joint capsule and produces synovial fluid, a viscous lubricant that nourishes the cartilage, reduces friction, and contributes to joint mobility.
The orientation of the facet joints varies throughout the spine, influencing the type and range of motion possible in each region. In the cervical spine (neck), the facet joints are oriented more horizontally, allowing for a wide range of rotation and flexion/extension. In the thoracic spine (upper back), they are oriented more sagittally, facilitating rotation. In the lumbar spine (lower back), the facet joints are oriented in a sagittal-coronal plane, predominantly limiting rotation while allowing for flexion and extension.
Biomechanical Significance and Common Pathologies
The facet joints play a critical role in controlling spinal movement, preventing excessive flexion, extension, and rotation, and providing segmental stability. They bear a significant portion of the axial load, especially during extension and rotation. This constant stress, combined with the aging process, trauma, or repetitive movements, can lead to the breakdown of the articular cartilage, a condition known as osteoarthritis or facet joint arthropathy.
When the cartilage wears down, the bones of the facet joint can rub directly against each other, leading to inflammation, pain, and the formation of bone spurs (osteophytes). This degenerative process can irritate the surrounding nerves, including the medial branch nerves that innervate the facet joints and the sinuvertebral nerves within the spinal canal, contributing to localized back pain, referred pain (pain that radiates to other areas like the buttocks or thighs), and stiffness. Other conditions that can affect facet joints include facet joint syndrome, facet joint hypertrophy (enlargement), and facet joint cysts.
Indications for a Facet Joint Injection
Facet joint injections are not a universal solution for all back pain. They are specifically indicated for individuals whose pain is demonstrably originating from the facet joints. A thorough diagnostic process is essential to confirm this origin before proceeding with an injection.
Diagnosing Facet Joint Pain
The primary diagnostic purpose of a facet joint injection is to pinpoint the specific facet joint or joints responsible for a patient’s pain. This is achieved through a process of diagnostic blocks. Before administering the therapeutic medication, a local anesthetic is injected into the suspected facet joint or around the medial branch nerves that supply it. If the patient experiences significant and temporary pain relief following this diagnostic injection, it strongly suggests that the targeted facet joint is indeed the source of their discomfort. This information is invaluable for guiding further treatment decisions.
Therapeutic Goals of the Injection
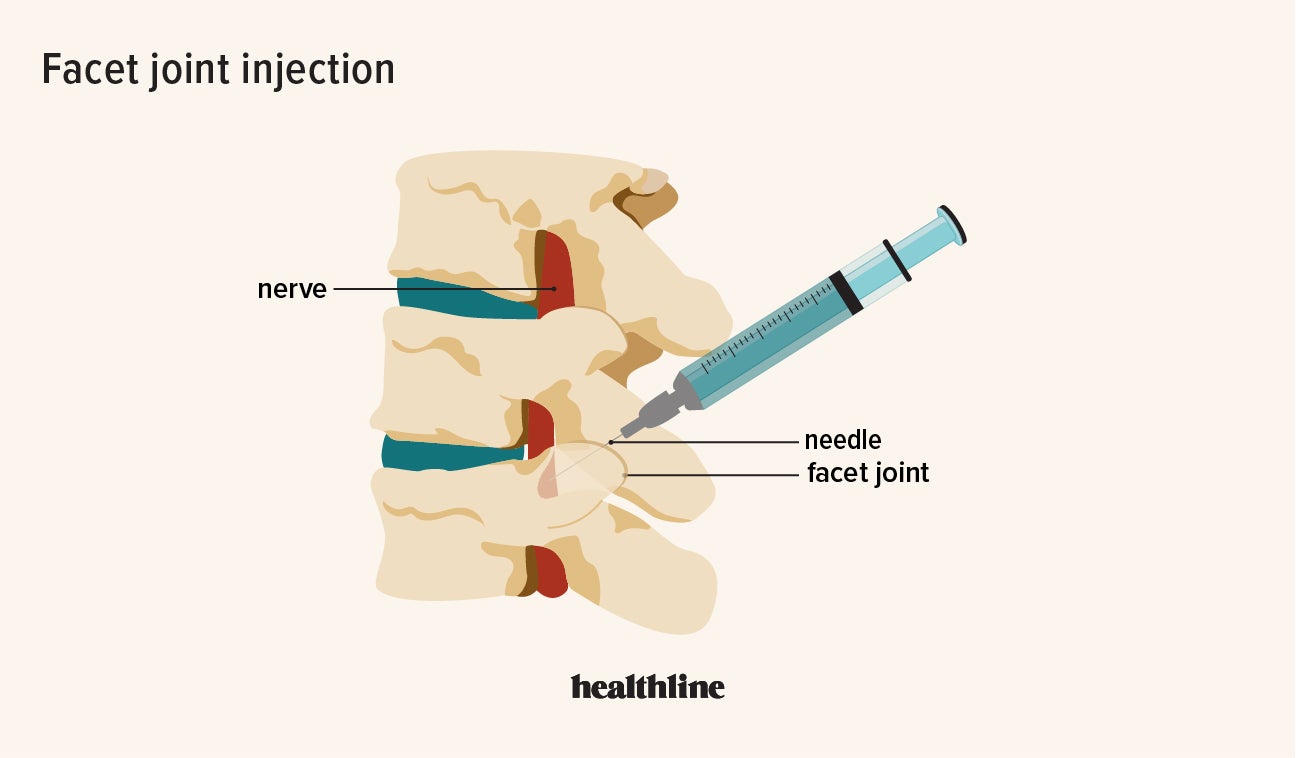
Beyond diagnosis, facet joint injections aim to provide therapeutic relief. The therapeutic solution typically comprises two components: a local anesthetic and a corticosteroid. The local anesthetic provides immediate, albeit temporary, pain relief by numbing the area. The corticosteroid is a potent anti-inflammatory medication that works to reduce swelling and irritation within the facet joint and around the affected nerves. This reduction in inflammation can break the cycle of pain and muscle spasm, allowing for improved mobility and function. The goal is to provide a window of relief during which patients can engage more effectively in physical therapy and other rehabilitation exercises, which are crucial for long-term pain management and functional recovery.
The Facet Joint Injection Procedure
The facet joint injection is a relatively straightforward outpatient procedure performed by pain management specialists, radiologists, or orthopedic surgeons. It is typically done under sterile conditions, with the patient positioned comfortably to allow optimal access to the target area.
Preparation and Anesthesia
Before the procedure, the patient will likely be asked to fast for a few hours. They may also be advised to stop certain medications, particularly blood thinners. The injection site, usually on the back, will be cleaned thoroughly with an antiseptic solution to minimize the risk of infection. Local anesthesia is then administered to numb the skin and superficial tissues at the injection site, ensuring the patient’s comfort during the needle insertion. Patients are typically awake during the procedure, although mild sedation may be offered in some cases to help with relaxation.
Needle Placement and Medication Delivery
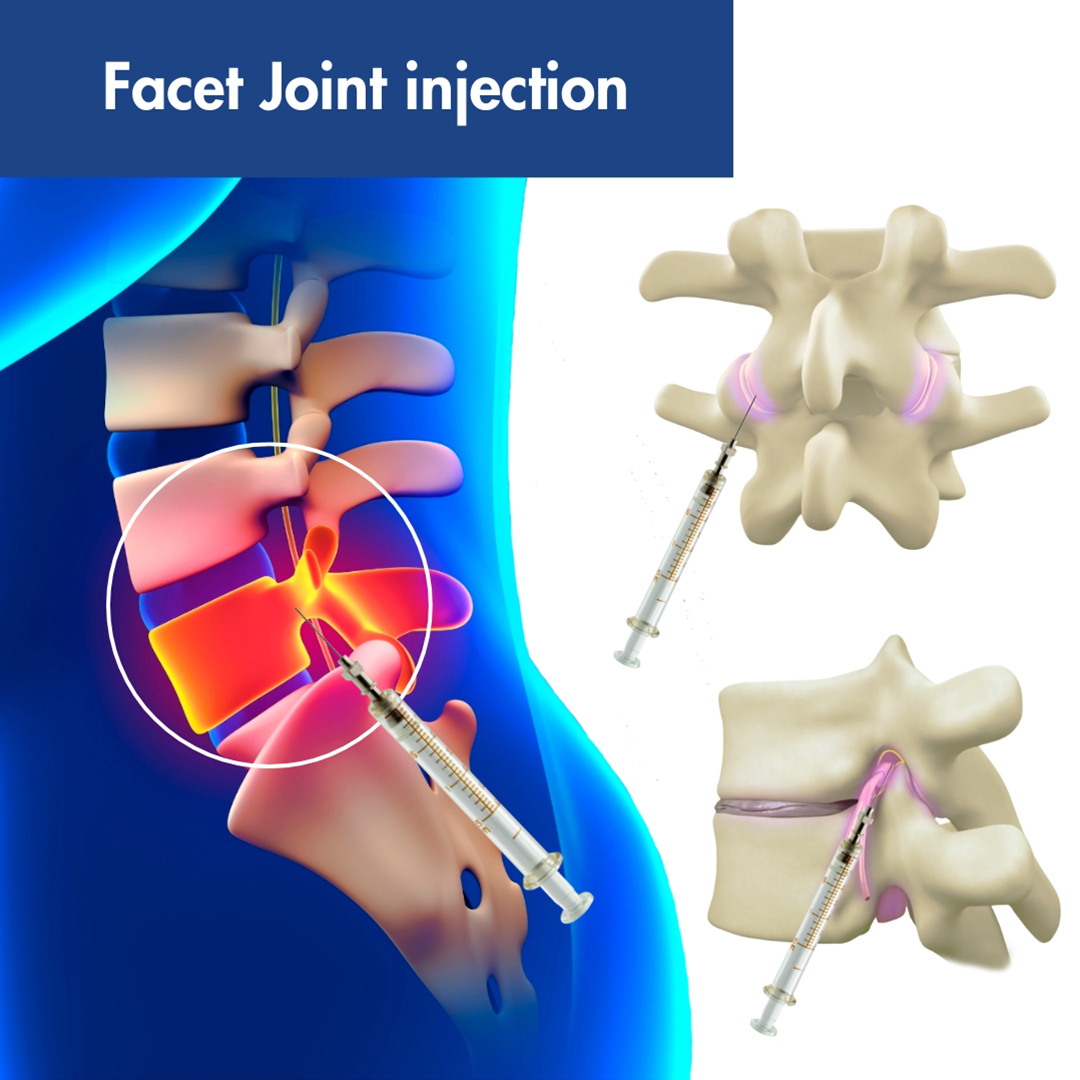
Guided by fluoroscopy (a type of real-time X-ray imaging) or sometimes ultrasound, the physician carefully inserts a fine needle through the skin and tissues to reach the targeted facet joint or the area around the medial branch nerves. Fluoroscopic guidance is critical for ensuring accurate needle placement. The physician injects a contrast dye first to confirm that the needle is positioned correctly within the joint capsule or near the target nerves, allowing the dye to spread appropriately.
Once the correct placement is confirmed, the therapeutic solution, containing the local anesthetic and corticosteroid, is slowly injected. The patient may feel some pressure or a mild discomfort during the injection. The entire procedure typically takes about 15 to 30 minutes. After the injection, the needle is removed, and a small bandage is applied to the injection site.
Post-Procedure Care and Recovery
Following the injection, patients are usually monitored for a short period, typically 15 to 30 minutes, to ensure there are no immediate adverse reactions. They are then free to go home, but it is recommended that they have someone drive them. It is advisable to avoid strenuous activities and heavy lifting for the first 24 to 48 hours. Some patients experience temporary numbness or weakness in the injected area, which should resolve within a few hours. Pain relief can be immediate due to the local anesthetic, but the corticosteroid’s anti-inflammatory effects may take a few days to become apparent. Patients are often encouraged to keep a pain diary to track their response to the injection. Follow-up appointments are scheduled to assess the effectiveness of the treatment and discuss further management plans.
Potential Benefits and Risks
Like any medical intervention, facet joint injections offer potential benefits but also carry inherent risks. A thorough discussion with a healthcare provider is essential to weigh these factors.
Expected Outcomes and Benefits
The primary benefit of a facet joint injection is pain relief. For individuals correctly diagnosed with facet joint pain, this procedure can significantly reduce their discomfort, improve their range of motion, and enhance their overall functional capacity. This pain relief can allow patients to participate more fully in physical therapy, exercise programs, and daily activities, which are crucial for long-term spinal health. In some cases, a single injection can provide relief for weeks to months, while others may require a series of injections for sustained benefit. Furthermore, by accurately identifying the pain generator, these injections can guide more specific and effective long-term treatment strategies, potentially avoiding more invasive procedures.
Possible Complications and Side Effects
While generally considered safe, facet joint injections are not without potential risks. These complications are relatively uncommon but can include bleeding at the injection site, infection, nerve damage, allergic reactions to the medications, temporary increased pain, headache (particularly with epidural injections, which share some procedural similarities), and bone infection (osteomyelitis), which is very rare. Systemic side effects from corticosteroids can include temporary elevations in blood sugar levels in diabetic patients, facial flushing, and insomnia. It is important to report any unusual or severe symptoms to your healthcare provider immediately. The decision to proceed with a facet joint injection should be made in consultation with a qualified medical professional who can assess individual risk factors and potential benefits.
