The human heart, a marvel of biological engineering, relies on a sophisticated electrical system to maintain its rhythm. When this system falters, it can lead to serious health consequences. One such critical condition is a third-degree heart block, also known as complete heart block. While traditionally understood through a medical lens, the advent and rapid evolution of technology have revolutionized how we detect, monitor, and even manage such complex cardiac arrhythmias. This article delves into the technological innovations that illuminate the understanding and clinical response to third-degree heart block.

Decoding the Electrical Symphony: The Technological Foundation of Cardiac Rhythms
The heart’s rhythmic beating is orchestrated by a series of electrical impulses. This intricate dance begins in the sinoatrial (SA) node, the heart’s natural pacemaker, which generates an electrical signal that travels through the atria, causing them to contract. This signal then reaches the atrioventricular (AV) node, a critical junction that delays the impulse slightly before transmitting it to the ventricles. This delay is crucial, allowing the atria to empty fully into the ventricles before the ventricles contract. The impulse then travels down the bundle of His and Purkinje fibers, triggering the powerful contraction of the ventricles that pumps blood throughout the body.
The Role of Electrocardiography (ECG) in Unveiling Rhythm Disturbances
At the forefront of understanding cardiac electrical activity is the electrocardiogram (ECG). This non-invasive diagnostic tool has been instrumental in identifying all types of heart blocks, including third-degree. An ECG records the electrical activity of the heart over a period of time using electrodes placed on the skin. The resulting waveform provides a graphical representation of the heart’s electrical conduction pathway.
Understanding the ECG Signatures of Third-Degree Heart Block
In a healthy heart, the ECG displays a predictable pattern: a P wave (representing atrial depolarization), followed by a QRS complex (representing ventricular depolarization), and then a T wave (representing ventricular repolarization). A consistent relationship exists between the P waves and the QRS complexes, indicating that the electrical signal is being conducted normally through the AV node.
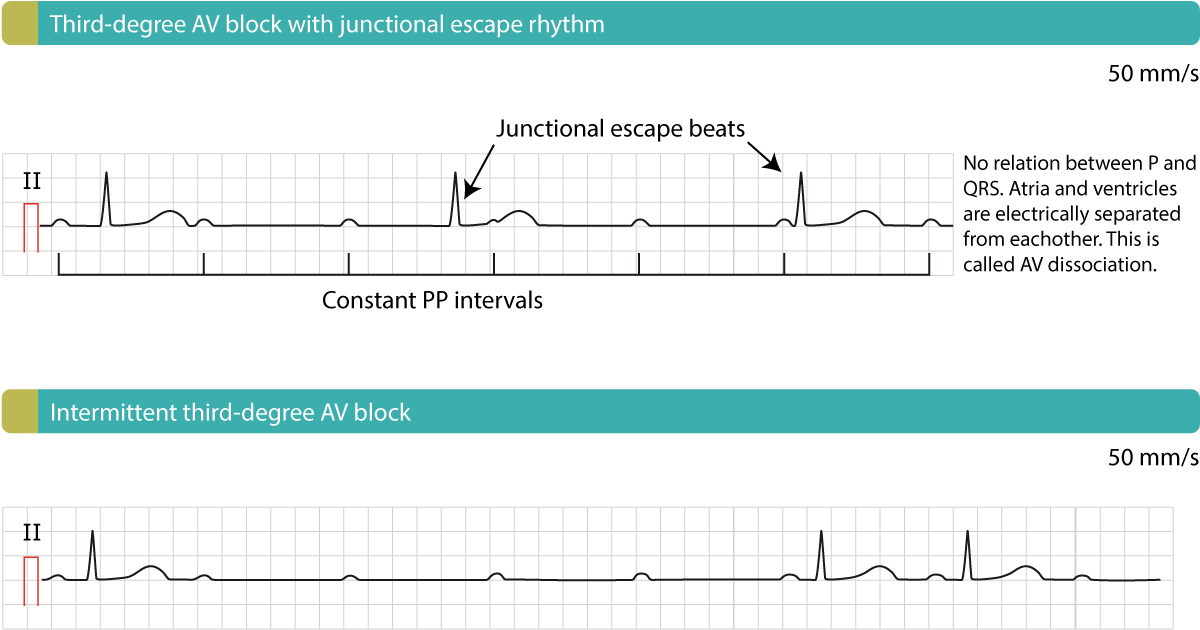
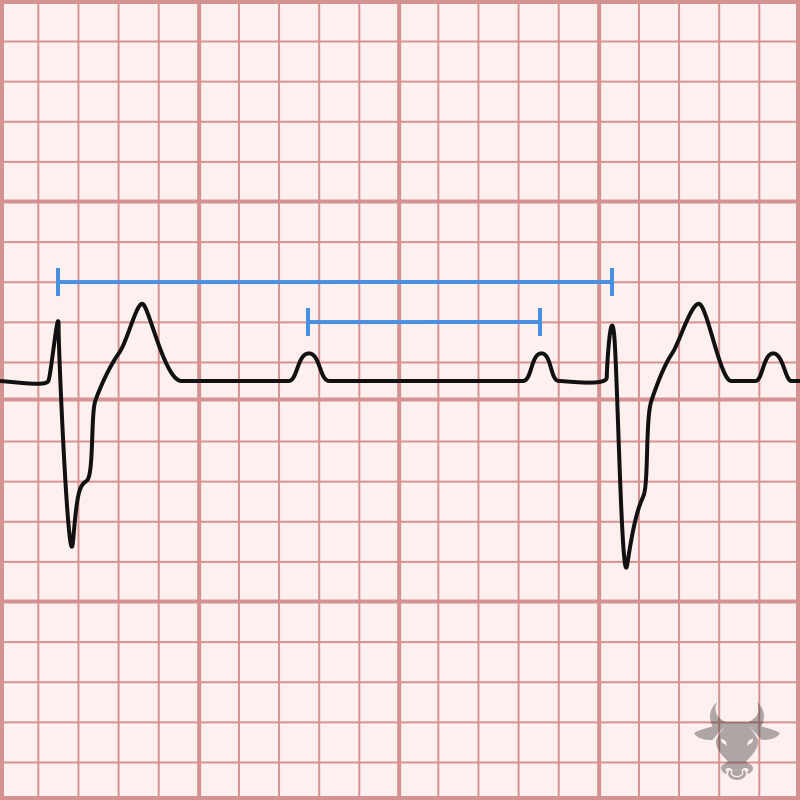
However, in third-degree heart block, a complete dissociation occurs between atrial and ventricular activity. The AV node completely blocks the electrical impulses from the SA node from reaching the ventricles. As a result, the atria continue to beat independently, driven by the SA node, and the ventricles initiate their own, slower escape rhythm, originating from a lower junction within the His-Purkinje system.
On an ECG, this manifests as:
- Regular P waves: The P waves will occur at a regular rate, reflecting the normal firing of the SA node.
- Regular but slower QRS complexes: The QRS complexes will also occur at a regular rate, but significantly slower than the P waves, indicating the independent ventricular rhythm.
- No correlation between P waves and QRS complexes: Crucially, the P waves will bear no consistent relationship to the QRS complexes. A P wave may precede a QRS, fall within it, or follow it. The AV dissociation is the hallmark diagnostic feature.
The rate of the QRS complexes in third-degree heart block is typically much lower than the normal heart rate, often falling below 40 beats per minute, which can lead to symptoms of poor blood flow, such as dizziness, fainting, and shortness of breath. The specific site of the block within the conduction system determines the rate and morphology of the escape rhythm. Blocks higher up in the AV node tend to have faster, narrower QRS complexes, while blocks lower down in the ventricles result in slower, wider QRS complexes.
Wearable Technology and Remote Monitoring: A New Era in Cardiac Care
The evolution of wearable technology has profoundly impacted the management of chronic conditions, and cardiac arrhythmias are no exception. Beyond the clinical setting, sophisticated devices are now capable of continuously monitoring heart rhythms, providing invaluable data for early detection and ongoing management of conditions like third-degree heart block.
Smartwatches and Fitness Trackers: Early Warning Systems
Many modern smartwatches and fitness trackers are equipped with photoplethysmography (PPG) sensors, which can detect changes in blood volume in the wrist, correlating to heart rate. While not as precise as an ECG for diagnosing complex arrhythmias, these devices can flag irregular heartbeats or abnormally slow heart rates.
For individuals at risk of or diagnosed with heart conditions, these wearables can act as an early warning system. If a smartwatch detects a consistently low heart rate or a significant irregularity that deviates from the user’s typical rhythm, it can prompt them to seek medical attention. Some advanced devices even incorporate an ECG function, allowing users to take an on-demand ECG reading when experiencing symptoms, which can then be shared with their physician. This accessibility empowers patients and provides clinicians with more comprehensive data outside of sporadic clinic visits.
Continuous Cardiac Monitoring Devices: The Power of Long-Term Data
For more critical cardiac conditions, or for individuals with a history of significant arrhythmias, continuous cardiac monitoring devices offer a more robust solution. These can range from Holter monitors, which are worn for 24-48 hours, to more advanced implantable loop recorders (ILRs) that can monitor for months or even years.
-
Holter Monitors: These portable devices record the heart’s electrical activity continuously. While a traditional Holter monitor requires the patient to return the device to a clinic for data analysis, newer iterations may allow for wireless transmission of data, enabling real-time or near real-time monitoring. This allows physicians to capture intermittent arrhythmias that might be missed during a standard ECG.
-
Implantable Loop Recorders (ILRs): These small devices are implanted just under the skin and can record cardiac rhythm for extended periods. They are particularly useful for detecting infrequent but significant arrhythmias. ILRs can automatically detect and record abnormal heart rhythms or can be activated by the patient when they experience symptoms. The data is often transmitted wirelessly to a monitoring center, allowing for prompt alerts to healthcare providers if a critical event is detected, such as a dangerously slow heart rate characteristic of third-degree heart block. This technology is invaluable for understanding the true burden of an arrhythmia and guiding treatment decisions.
Artificial Intelligence and Machine Learning in Arrhythmia Detection and Prediction
The exponential growth of data generated by cardiac monitoring devices has paved the way for the application of artificial intelligence (AI) and machine learning (ML) in cardiology. These technologies are transforming the analysis of complex cardiac data, leading to more accurate diagnoses and even predictive capabilities.
AI-Powered ECG Analysis: Enhancing Diagnostic Accuracy
AI algorithms are being trained on vast datasets of ECGs to identify subtle patterns that may be missed by human interpretation. These algorithms can analyze thousands of ECGs rapidly and with a high degree of accuracy, flagging potential abnormalities for review by a cardiologist.
In the context of third-degree heart block, AI can be trained to recognize the specific disassociation between P waves and QRS complexes, the characteristic slow ventricular rate, and other subtle indicators of conduction system disease. This can lead to faster and more definitive diagnoses, particularly in complex or atypical cases. Furthermore, AI can help differentiate between various types of heart block and other arrhythmias that might present with similar symptoms.
Predictive Analytics: Identifying At-Risk Individuals and Future Events
Beyond diagnosis, AI and ML are showing promise in predicting the likelihood of developing certain cardiac conditions or experiencing adverse events. By analyzing a combination of patient data, including ECGs, medical history, and even lifestyle factors, AI models can identify individuals who may be at higher risk for developing conduction abnormalities like third-degree heart block.
This predictive capability can enable proactive interventions. For instance, if an AI algorithm identifies a patient with subtle ECG changes or risk factors suggestive of future conduction system disease, physicians can implement closer monitoring or preventative measures. In patients already diagnosed with third-degree heart block, AI can potentially predict the risk of progression of the block or the likelihood of syncopal episodes, allowing for more personalized and timely treatment adjustments, such as the timely implantation of a pacemaker.
The Future of Cardiac Intervention: Technological Innovations in Treatment
While understanding and monitoring are crucial, the ultimate goal in managing third-degree heart block is effective treatment. Technology plays a pivotal role not only in diagnosis but also in the delivery of life-saving interventions.
Pacemaker Technology: The Gold Standard for Third-Degree Heart Block
For symptomatic third-degree heart block, the implantation of a pacemaker is the definitive treatment. A pacemaker is a small, battery-powered device implanted surgically, typically in the chest, with leads that extend to the heart. It monitors the heart rhythm and delivers electrical impulses when the heart rate falls too low or when a block in the conduction system is detected.
Modern pacemakers are marvels of miniaturization and advanced engineering. They are highly sophisticated and can be programmed to deliver pacing in various modes, optimizing the heart’s function based on the patient’s individual needs.
Leadless Pacemakers and Remote Management: Minimally Invasive Solutions
The evolution of pacemaker technology has moved towards less invasive and more patient-centric solutions. Leadless pacemakers are a significant advancement, eliminating the need for transvenous leads. These tiny devices are implanted directly into the heart chamber via a catheter inserted through a vein. They provide pacing without the visible pulse generator and leads under the skin, offering cosmetic benefits and reducing the risk of lead-related complications.
Furthermore, contemporary pacemakers, including leadless versions, are increasingly equipped with remote monitoring capabilities. Patients can transmit data from their pacemaker to their healthcare provider wirelessly, allowing for continuous assessment of device function and the patient’s cardiac rhythm without the need for frequent clinic visits. This remote management system can detect any issues with the pacemaker or significant changes in the patient’s heart rhythm, enabling swift intervention if necessary. This technological integration ensures continuous oversight and optimized care for individuals living with third-degree heart block.
