Wisdom teeth, the last set of molars to emerge, typically appear in the late teens or early twenties. While for some, they erupt without issue and integrate seamlessly into the bite, for a significant portion of the population, their arrival can signal a host of potential complications. The decision of whether or not to have wisdom teeth surgically removed is a common dental dilemma, and understanding the potential consequences of leaving them in place is crucial for informed decision-making. This article delves into what can transpire when wisdom teeth are left unaddressed, exploring the various scenarios that might unfold.
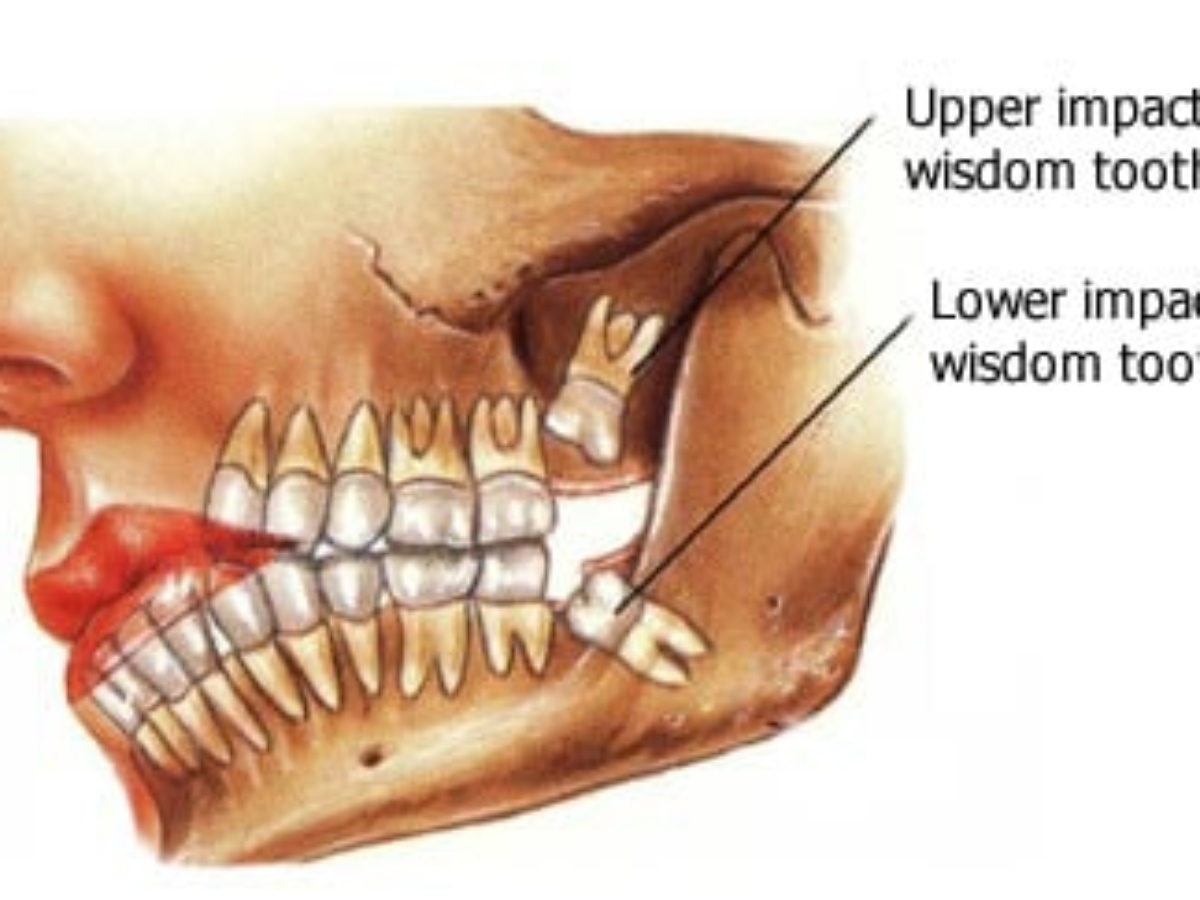
The Anatomy of an Eruption: Why Wisdom Teeth Cause Problems
Wisdom teeth, also known as third molars, are evolutionary remnants. Their large size and late eruption often clash with the limited space available in the modern human jaw. This anatomical misfit is the root cause of many of the problems associated with them.
Insufficient Space and Impaction
The most frequent issue arises from a lack of sufficient space for the wisdom teeth to erupt fully and properly. This can lead to them becoming impacted, meaning they are trapped beneath the gum line or are only partially erupted. Impaction can occur in several ways:
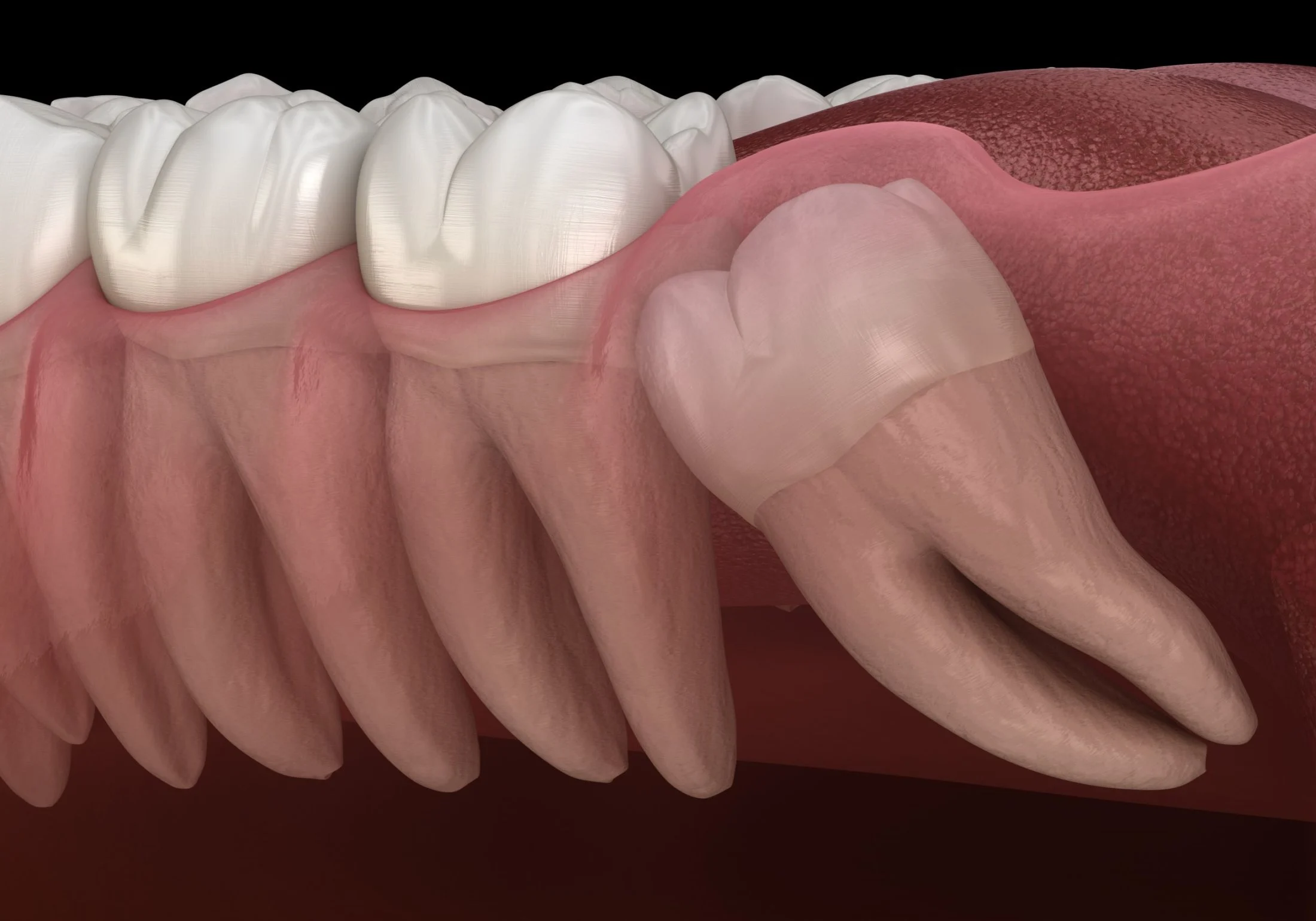
- Mesial Impaction: The tooth is angled forward, towards the front of the mouth. This is the most common type of impaction.
- Distal Impaction: The tooth is angled backward, towards the back of the jaw.
- Vertical Impaction: The tooth is trying to erupt straight up but is blocked by the tooth in front of it.
- Horizontal Impaction: The tooth is lying on its side, often pressing against the root of the adjacent molar.
- Incomplete Eruption: The tooth erupts partially, leaving a flap of gum tissue (an operculum) covering part of the chewing surface.
The consequences of impaction are varied. The pressure exerted by an erupting or impacted wisdom tooth can cause damage to the adjacent second molar, including root resorption, decay, or misalignment. The inability of the tooth to erupt fully also creates a dark, moist environment beneath the gum flap, which is a breeding ground for bacteria.
Pericoronitis: The Inflamed Aftermath
When wisdom teeth only partially erupt, a flap of gum tissue, known as an operculum, can remain over the chewing surface. This area is notoriously difficult to clean effectively, leading to a condition called pericoronitis.
-
Symptoms of Pericoronitis: The onset of pericoronitis can range from mild discomfort to severe pain. Common symptoms include:
- Swelling of the gum tissue around the wisdom tooth.
- Redness and tenderness in the area.
- A foul taste or smell in the mouth due to trapped food particles and bacteria.
- Pain that can radiate to the jaw, ear, or throat.
- Difficulty opening the mouth (trismus).
- In more severe cases, fever and swollen lymph nodes may occur, indicating a more widespread infection.
-
Recurrence: Pericoronitis can be a recurring problem, with flare-ups often triggered by factors like stress, fatigue, or poor oral hygiene. Each episode can cause significant discomfort and may lead to more serious complications if left untreated. Chronic pericoronitis can lead to persistent inflammation and damage to surrounding tissues.
The Cascade of Dental Problems
Beyond immediate pain and inflammation, neglecting wisdom teeth can trigger a cascade of other dental issues, affecting not just the wisdom teeth themselves but the entire oral cavity.
Dental Decay and Cavities
The tight spaces and difficult-to-reach areas around partially erupted or impacted wisdom teeth make them prime targets for dental decay. Food particles and plaque can easily become trapped, providing a feast for cavity-causing bacteria.
- Wisdom Tooth Decay: The enamel on wisdom teeth can be thinner, making them more susceptible to decay. When decay sets in, it can progress rapidly, leading to pain, sensitivity, and eventually the need for fillings or even extraction if the decay is extensive.
- Decay of Adjacent Teeth: The pressure from an impacted wisdom tooth can also push against the adjacent second molar, creating a gap where plaque and food debris can accumulate. This can lead to cavities forming on the second molar, often in a location that is difficult to detect and treat.
Gum Disease and Bone Loss
The accumulation of bacteria and the chronic inflammation associated with pericoronitis can extend beyond the immediate vicinity of the wisdom tooth. This can lead to gum disease (periodontitis) and, in severe cases, bone loss.
- Periodontitis Around Wisdom Teeth: The gingival tissues surrounding wisdom teeth can become inflamed and infected, leading to the formation of periodontal pockets. These pockets harbor bacteria that can damage the supporting bone structure of the teeth.
- Bone Resorption: Over time, the chronic inflammation and infection can cause the bone that anchors the wisdom teeth and adjacent molars to be resorbed, or lost. This can weaken the stability of the teeth and, in extreme cases, lead to the loosening or loss of the second molars.
Cysts and Tumors
While less common, impacted wisdom teeth can also lead to the development of cysts or, very rarely, tumors. The follicular sac surrounding an unerupted tooth can accumulate fluid and expand, forming a dentigerous cyst.
- Dentigerous Cysts: These cysts can grow significantly over time, exerting pressure on the jawbone and surrounding teeth. They can cause jaw swelling, pain, and damage to the roots of adjacent teeth. If left untreated, these cysts can lead to extensive bone loss and even pathological fractures of the jaw.
- Odontogenic Tumors: In extremely rare instances, the cells within the follicular sac can transform into benign or malignant tumors. Early detection and removal are crucial for successful treatment.

The Unforeseen Consequences: Beyond Immediate Dental Pain
The impact of unremoved wisdom teeth can extend beyond the localized oral cavity, influencing overall health and well-being in ways that might not be immediately apparent.
Chronic Pain and Discomfort
For many individuals, the presence of wisdom teeth leads to persistent, low-grade pain or discomfort that they may learn to live with, attributing it to other causes. This chronic pain can subtly, but significantly, affect their quality of life.
- Jaw Aches and Headaches: The pressure exerted by erupting or impacted wisdom teeth can cause discomfort in the jaw joint (temporomandibular joint or TMJ) and lead to tension headaches. These can be persistent and difficult to diagnose without considering the role of the wisdom teeth.
- Referred Pain: Pain from wisdom teeth can also be “referred” to other areas, such as the ear or throat, making it challenging to pinpoint the origin of the discomfort. This can lead to unnecessary medical consultations and treatments.
Impact on Oral Hygiene and Function
The presence of wisdom teeth, especially if they are misaligned or impacted, can significantly hinder effective oral hygiene practices and impact the overall function of the mouth.
- Difficulty in Brushing and Flossing: The posterior location and often crowded positioning of wisdom teeth make them extremely difficult to clean thoroughly. This compromised hygiene contributes to increased plaque buildup, decay, and gum disease.
- Chewing Difficulties: If wisdom teeth are causing pain or are improperly aligned, they can interfere with efficient chewing. This can lead to uneven wear on other teeth, digestive issues due to inadequate mastication, and a general discomfort during meals.
- Bite Problems: Over time, the pressure from erupting wisdom teeth can subtly shift other teeth, leading to changes in the bite alignment. This can manifest as crooked teeth, crowding, or an increased risk of grinding (bruxism).
Systemic Health Links: A Developing Understanding
While the direct links are still being explored, emerging research suggests potential connections between chronic oral infections, like those associated with problematic wisdom teeth, and broader systemic health conditions.
- Cardiovascular Disease: Some studies have indicated a correlation between chronic gum inflammation and an increased risk of heart disease. Bacteria from oral infections can potentially enter the bloodstream and contribute to inflammation in blood vessels.
- Diabetes Management: Poor oral health, including infections from wisdom teeth, can negatively impact blood sugar control in individuals with diabetes. Conversely, diabetes can also exacerbate gum disease, creating a challenging cycle.
- Pregnancy Complications: There is some evidence to suggest a link between severe gum disease and an increased risk of premature birth and low birth weight.
The Decision to Remove: When and Why
The decision to remove wisdom teeth is not a one-size-fits-all approach. It is a personalized assessment made in consultation with a dentist or oral surgeon, considering the individual’s specific circumstances and potential risks.
Risk Assessment and Diagnostic Tools
A thorough evaluation is the first step in determining the necessity of wisdom tooth extraction. This involves a combination of clinical examination and advanced imaging techniques.
- Clinical Examination: Your dentist will examine your mouth, assess the position of your wisdom teeth, check for any signs of inflammation or infection, and evaluate the health of your adjacent teeth and gums.
- Dental X-rays: Panoramic X-rays (panorex) and periapical X-rays are crucial diagnostic tools. They provide a detailed view of the entire jaw, showing the position of the wisdom teeth, their roots, their relationship to adjacent structures (nerves, sinuses), and any signs of impaction, decay, or cyst formation. Cone-beam computed tomography (CBCT) scans offer even more detailed 3D imaging for complex cases.
Signs and Symptoms Indicating Removal
While many individuals may have wisdom teeth that cause no immediate issues, certain signs and symptoms strongly suggest that removal is the most prudent course of action.
- Pain or Swelling: Persistent or recurring pain, swelling, or tenderness around the wisdom teeth is a clear indicator of potential problems like pericoronitis or impaction.
- Visible Signs of Infection: Redness, pus discharge, or a foul taste emanating from the wisdom tooth area warrant immediate attention.
- Damage to Adjacent Teeth: X-rays revealing resorption of the roots of the second molars or early signs of decay on these teeth due to wisdom tooth pressure are strong reasons for extraction.
- Cyst Formation: The presence of a cyst, as identified on X-rays, necessitates surgical removal to prevent further damage to the jawbone and surrounding teeth.
- Difficulty with Oral Hygiene: If the position of the wisdom teeth makes effective cleaning impossible, leading to recurrent plaque buildup and potential problems, removal may be recommended.
- Prophylactic Removal: In some cases, especially in younger individuals with high-risk factors for future complications, dentists may recommend prophylactic removal even in the absence of current symptoms. This is to prevent potential future issues.
The Extraction Procedure and Recovery
Wisdom tooth extraction is a common surgical procedure performed by dentists or oral surgeons. The complexity of the procedure and the recovery period can vary depending on the impaction of the teeth.
- Surgical Techniques: The method of extraction will depend on whether the wisdom teeth are fully erupted or impacted. Simple extractions may involve loosening the tooth with an elevator and removing it. Impacted teeth often require surgical exposure, bone removal, and sectioning of the tooth into smaller pieces for easier removal.
- Anesthesia: Local anesthesia is typically used to numb the area. For anxious patients or more complex procedures, sedation or general anesthesia may be offered.
- Post-Operative Care and Recovery: The recovery period typically involves managing pain and swelling with medication and following specific post-operative instructions. This includes a soft diet, avoiding strenuous activity, and maintaining good oral hygiene without disturbing the surgical sites. Most patients can return to their normal activities within a few days to a week.
In conclusion, while not all wisdom teeth cause problems, the potential consequences of leaving them unaddressed are significant and can range from localized pain and infection to more widespread dental issues and even potential impacts on systemic health. Regular dental check-ups and open communication with your dental professional are key to making informed decisions about your oral health, ensuring the well-being of your smile for years to come.
