Understanding the Early Signs of Gum Disease
Gingivitis, the initial stage of periodontal disease, is a common yet often overlooked inflammatory condition affecting the gums. While its name might sound intimidating, understanding its visual cues is the first and most crucial step in prevention and treatment. Unlike more advanced stages of gum disease, gingivitis is typically reversible with proper oral hygiene. The key to preserving your oral health lies in recognizing the subtle—and sometimes not-so-subtle—changes in your gum tissue. This guide will delve into the visual characteristics of gingivitis, empowering you to identify it early and take proactive measures.

The Healthy Gum Baseline
Before we examine what gingivitis looks like, it’s essential to establish a clear picture of healthy gums. Healthy gum tissue is typically a vibrant coral pink, firm to the touch, and fits snugly around the teeth without bleeding. There should be no swelling, recession (pulling away from the teeth), or persistent bad breath. The gum line should be well-defined, creating a protective collar around each tooth. This healthy state is a testament to effective daily oral hygiene practices, including regular brushing and flossing, and professional dental cleanings. It signifies an absence of significant bacterial plaque buildup and inflammation.
Visual Indicators of Gingivitis
When gingivitis begins to take hold, the visual landscape of your gums starts to change. The primary culprits are bacteria that accumulate in dental plaque, an invisible sticky film that constantly forms on teeth. If this plaque is not removed through diligent brushing and flossing, it can irritate the gums, triggering an inflammatory response. This inflammation manifests in several distinct ways:
Color Changes: From Pink to Red and Beyond
Perhaps the most striking visual indicator of gingivitis is a change in gum color. Healthy gums are a soft, even coral pink. As inflammation sets in, this color begins to deepen, progressing through shades of red.
- Mild Inflammation: Initially, you might notice a slightly brighter pink hue, particularly along the gum line. This can be subtle and easily dismissed.
- Moderate Inflammation: As the inflammation intensifies, the gums will take on a more distinct bright red or even a purplish-red appearance. The color change is often more pronounced around the base of the teeth and may extend upwards.
- Advanced Inflammation: In more severe cases of gingivitis, the redness can become almost crimson. The gums may also appear shiny rather than their usual matte texture, indicating a loss of their natural firmness.
It’s important to note that these color changes are a direct result of increased blood flow to the area as the body attempts to fight the bacterial invasion. This increased vascularity is what causes the gums to appear redder than normal.
Swelling and Puffiness: The Loss of Firmness
Another hallmark of gingivitis is swelling, also known as edema. Healthy gums are firm and resilient. When inflamed, they lose this firmness and become noticeably puffy or enlarged.
- Subtle Puffiness: In the early stages, the swelling might be slight, making the gum line appear slightly rounded or thicker than usual.
- Visible Enlargement: As gingivitis progresses, the gums can become significantly swollen, obscuring the natural contours and even slightly covering the crowns of the teeth. This enlargement can create “false pockets” between the teeth and gums, which can trap more plaque and bacteria, perpetuating the cycle of inflammation.
- Edematous Appearance: The swollen tissue often takes on a smooth, shiny, and sometimes boggy texture, a stark contrast to the firm, matte surface of healthy gums. This loss of definition at the gum line is a critical sign to look out for.
Bleeding: A Red Flag
One of the most common and concerning visual signs of gingivitis is bleeding gums. While a small amount of bleeding might seem insignificant, it is a clear indication that the gum tissue is inflamed and damaged.
- Spontaneous Bleeding: Bleeding gums can occur spontaneously, meaning they bleed even without any provocation. You might notice blood on your toothbrush after brushing, on your dental floss, or even in your saliva after eating or drinking.
- Bleeding During Oral Hygiene: More commonly, bleeding occurs during brushing or flossing. If you experience bleeding when you gently clean your teeth, it is a strong signal that gingivitis is present. It’s crucial to remember that even though bleeding is happening, it is vital to continue brushing and flossing gently to remove plaque – the underlying cause of the bleeding. Stopping oral hygiene out of fear of bleeding will only exacerbate the problem.
- Color of Blood: The blood is typically bright red, indicating fresh bleeding, a sign that the inflammation is active.
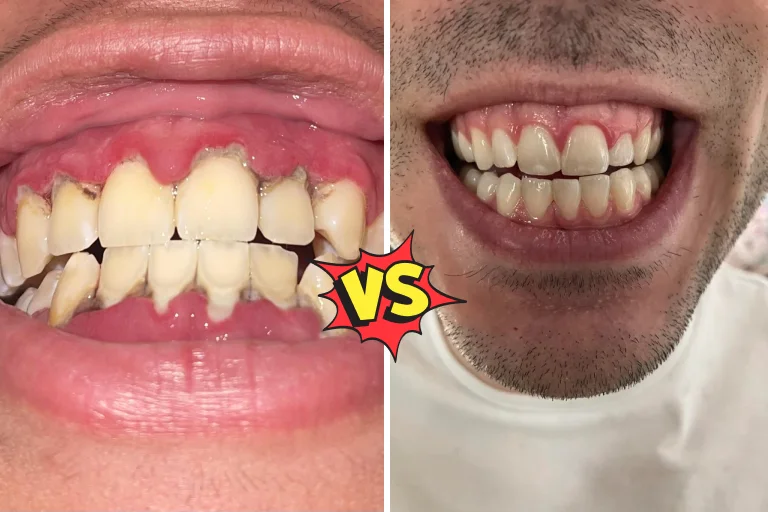
Changes in Gum Contour: Receding or Enlarged Gums
While receding gums are often associated with more advanced gum disease (periodontitis), gingivitis can also lead to subtle changes in gum contour.
- Enlargement: As mentioned earlier, significant swelling can make the gums appear larger and more prominent.
- Early Recession: In some cases, particularly if the inflammation is chronic or there are other contributing factors, the gum tissue might begin to pull away from the teeth. However, significant gum recession is more characteristic of periodontitis, where the bone supporting the teeth is also affected. With gingivitis, the underlying bone remains intact.
Halitosis (Bad Breath): The Olfactory Clue
While not strictly a visual sign, persistent bad breath, or halitosis, is a common companion to gingivitis. The bacteria that cause plaque buildup and inflammation also produce volatile sulfur compounds, which are responsible for the unpleasant odor. If you or someone else notices a persistent foul smell emanating from your mouth, even after brushing, it can be a strong indicator of gingivitis or other oral health issues.
Differentiating Gingivitis from Periodontitis
It is crucial to distinguish gingivitis from periodontitis, its more severe counterpart. While both involve gum inflammation, periodontitis signifies a more advanced stage where the supporting structures of the teeth, including the bone and ligaments, are also being destroyed.
| Feature | Gingivitis | Periodontitis |
|---|---|---|
| Gum Appearance | Red, swollen, puffy, may bleed easily | Reddish-purple, swollen, or sometimes pale |
| Gum Attachment | Remains attached to the teeth | Detaches from the teeth, forming pockets |
| Bone Loss | None | Present, visible on X-rays |
| Tooth Mobility | None | May be present, teeth can loosen |
| Reversibility | Reversible with proper hygiene | Not reversible, but progression can be managed |
| Primary Cause | Plaque accumulation | Plaque, genetic factors, systemic diseases |
Understanding these differences highlights the importance of treating gingivitis promptly. By addressing the inflammation in its earliest stages, you can prevent it from progressing to periodontitis, a condition that can lead to tooth loss.
The Role of Dental Professionals
While self-examination is valuable, regular visits to your dentist or dental hygienist are paramount for accurate diagnosis and effective treatment. Dental professionals have the expertise and specialized tools to detect gingivitis, even in its very early stages, and to assess its severity.
During a dental examination, they will:
- Visually inspect your gums: Looking for the characteristic signs of redness, swelling, and bleeding.
- Measure gum pockets: Using a periodontal probe, they will measure the depth of the space between your gums and teeth. In gingivitis, these pockets will be shallow (typically 1-3 mm), whereas in periodontitis, they will be deeper.
- Assess bleeding points: Noting where and how easily your gums bleed during the examination.
- Take X-rays (if necessary): To check for any signs of bone loss, which would indicate periodontitis.
Your dental professional will then provide personalized recommendations for improving your oral hygiene routine and may perform a professional dental cleaning to remove plaque and tartar that you cannot remove at home.

Prevention and Management: Taking Control
The good news about gingivitis is that it is almost entirely preventable and, when caught early, completely reversible. The cornerstone of prevention and management is consistent and effective oral hygiene.
- Brushing: Brush your teeth at least twice a day for two minutes each time, using a soft-bristled toothbrush and fluoride toothpaste. Pay special attention to cleaning along the gum line, where plaque tends to accumulate. Angle the brush bristles towards the gum line and use gentle, circular motions.
- Flossing: Floss daily to remove plaque and food particles from between your teeth and under the gum line, areas that your toothbrush cannot reach.
- Mouthwash: An antimicrobial mouthwash can be a helpful adjunct to brushing and flossing, helping to reduce bacteria in the mouth. However, it should not be considered a replacement for mechanical cleaning.
- Regular Dental Check-ups: Schedule regular dental appointments for professional cleanings and check-ups. These visits allow your dental team to remove hardened plaque (tartar) and monitor your oral health.
- Healthy Lifestyle: A balanced diet and avoiding smoking can also contribute to better gum health. Smoking is a significant risk factor for gum disease.
By being vigilant about the visual signs of gingivitis and committing to a consistent oral hygiene routine, you can protect your gums, maintain a healthy smile, and prevent the progression to more serious dental problems. Recognizing what gingivitis looks like is not just about spotting a problem; it’s about empowering yourself to take action and preserve your oral well-being.
