The phrase “voided” in a medical context can be multifaceted, often referring to the act of urination or defecation, or more broadly, to something being rendered invalid or null. Understanding these distinctions is crucial for accurate medical record-keeping, patient communication, and the interpretation of diagnostic information. This article delves into the various medical interpretations of “voided,” focusing on its direct physiological meaning and its implications in administrative and diagnostic processes.
The Physiology of Voiding
At its most fundamental, “voided” in medicine directly relates to the expulsion of bodily waste products from the body. This process is known as voiding, a term commonly used to describe the act of passing urine from the bladder or feces from the bowels.
Urinary Voiding
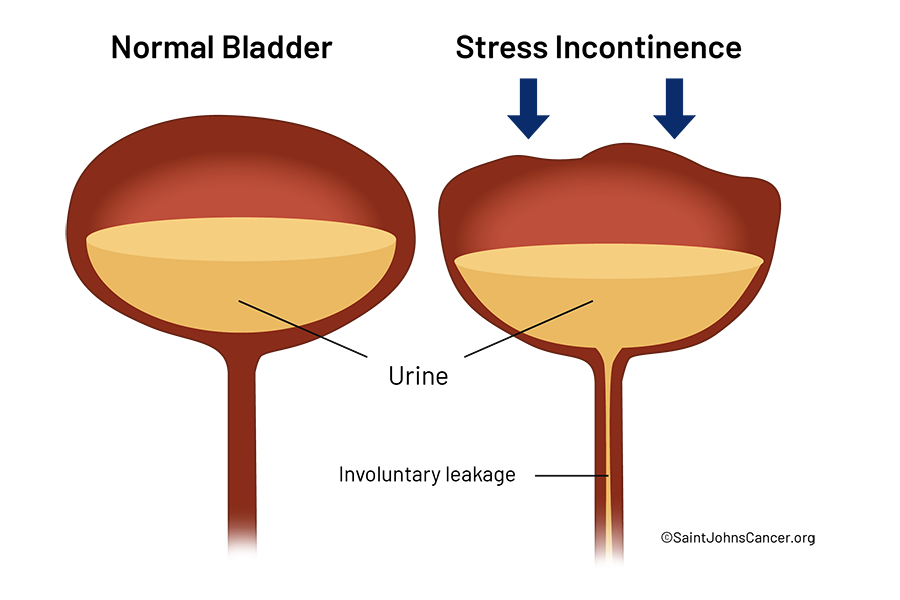
Urinary voiding, or micturition, is the process by which urine is expelled from the urinary bladder through the urethra. This complex physiological function involves the coordinated action of the bladder’s detrusor muscle, the internal and external urethral sphincters, and the nervous system.
The urge to urinate typically arises when the bladder distends with urine, stimulating stretch receptors in the bladder wall. These receptors send signals to the brain, which then triggers the sensation of needing to void. The brain can then voluntarily control the relaxation of the external urethral sphincter, allowing for the passage of urine.
In a medical setting, the term “voided” in relation to urine often appears in the context of intake and output (I&O) charting. This is a critical aspect of patient care, especially for individuals who are dehydrated, have kidney issues, are recovering from surgery, or are experiencing fluid imbalances. Nurses and other healthcare professionals meticulously record the amount of fluid a patient consumes and the amount they void.
For example, a patient might be instructed to “void into the collection hat” to measure their urine output accurately. This measurement is vital for assessing kidney function, monitoring hydration status, and managing conditions like heart failure or acute kidney injury. Deviations from expected voiding patterns—such as anuria (no urine production), oliguria (scanty urine production), or polyuria (excessive urine production)—can be significant indicators of underlying medical problems.
Furthermore, the quality of the voided urine can also be medically relevant. Healthcare providers might note the color, clarity, odor, and presence of any abnormalities, such as blood (hematuria) or pus (pyuria), which can point to infections, kidney stones, or other urinary tract pathologies. A urine sample collected after a patient has naturally voided is often referred to as a “voided urine specimen” and is commonly used for urinalysis and urine culture tests.
Bowel Voiding
Similarly, “voided” can refer to the act of defecation, the expulsion of feces from the rectum. This process involves the coordinated action of the large intestine, rectum, and anal sphincters. The urge to defecate is triggered by the presence of stool in the rectum, leading to signals sent to the brain.
In clinical practice, monitoring bowel movements is essential, particularly for patients who have undergone abdominal surgery, are experiencing gastrointestinal issues, or are at risk of constipation or fecal impaction. Healthcare professionals might ask patients about their bowel habits, including the frequency, consistency, and ease of voiding (defecation).
The term “voided” in this context emphasizes the voluntary or involuntary expulsion of waste. For instance, a post-operative patient might be closely monitored for their first bowel movement after surgery, a milestone often referred to as “passing gas” or “voiding bowels.” This indicates the return of normal gastrointestinal function.
As with urine, the characteristics of the voided stool can provide diagnostic clues. Changes in color, consistency, or the presence of blood or mucus can suggest various gastrointestinal disorders, from simple dietary indiscretions to more serious conditions like inflammatory bowel disease or colorectal cancer.
Voided in the Context of Invalidity or Nullification
Beyond its physiological meaning, “voided” in medicine can also denote that something has been invalidated, canceled, or rendered legally or administratively null and void. This usage is particularly prevalent in administrative, legal, and insurance-related aspects of healthcare.
Voided Medical Records and Documents

Medical records are legal documents, and errors or omissions can lead to their invalidation. If a significant error is discovered in a patient’s chart, such as an incorrect diagnosis, a mistaken entry of medication, or an improper procedure note, the original entry might be “voided.” This doesn’t mean the incorrect information is erased; rather, it is marked as invalid, and a corrected or new entry is made, often with an explanation for the voiding.
This process is crucial for maintaining the integrity of patient information. A voided entry ensures that subsequent decisions and treatments are not based on erroneous data. The original, incorrect entry remains visible, but it is clearly identified as voided, preserving a chronological audit trail. This is a standard practice in healthcare information management systems to ensure accuracy and compliance with regulatory requirements.
Voided Insurance Claims and Payments
In the realm of medical billing and insurance, “voided” often refers to an insurance claim or payment that has been canceled or invalidated. This can occur for several reasons:
- Duplicate Submission: If a claim is submitted multiple times for the same service, subsequent submissions might be voided.
- Incorrect Information: Errors in patient identification, policy numbers, diagnostic codes (ICD-10), or procedure codes (CPT) can lead to a claim being rejected and subsequently voided.
- Patient Eligibility Issues: If it’s later discovered that the patient was not eligible for coverage on the date of service, or if the policy was invalid, the claim might be voided.
- Overpayments or Incorrect Payments: If an insurer has paid a claim incorrectly, either an overpayment or an underpayment, they may issue a “void” of the original payment and reprocess the claim with the correct amount. This is a mechanism to correct administrative errors.
When a claim or payment is voided, it essentially means it is treated as if it never happened. For providers, this can necessitate resubmitting a corrected claim or a new claim, depending on the reason for the void. For patients, it might mean they are responsible for a balance that was initially thought to be covered or was incorrectly adjusted. Understanding the term “voided” in this context is vital for healthcare providers to manage their revenue cycle effectively and for patients to understand their financial responsibilities.
Voided Consents and Agreements
In certain situations, patient consent forms or other agreements within the healthcare setting can be declared “voided.” This might happen if:
- Lack of Capacity: If a patient was found to lack the mental capacity to give informed consent at the time the form was signed, the consent might be voided retrospectively.
- Coercion or Undue Influence: If consent was obtained under duress or undue influence, it could be deemed void.
- Significant Misinformation: If the patient was provided with substantially incorrect or misleading information upon which they based their consent, the consent may be voided.
When a consent is voided, it means that the legal permission granted by that consent is nullified, and any procedures or treatments performed under its authority may be subject to legal review. This highlights the importance of robust informed consent processes in healthcare.
Implications and Importance of Understanding “Voided”
The dual meaning of “voided”—referring to physiological expulsion and administrative invalidation—underscores the importance of context in medical terminology.
For Healthcare Professionals
Accurate documentation is paramount. Healthcare providers must clearly understand the physiological processes of voiding when assessing patients and meticulously record intake and output. When dealing with administrative or legal aspects, properly voiding erroneous entries or claims is essential for maintaining data integrity, compliance, and financial accuracy. Misinterpreting “voided” could lead to diagnostic errors, treatment delays, or financial discrepancies.
For Patients
Patients encountering the term “voided” in their medical records or billing statements should not hesitate to seek clarification from their healthcare providers. Understanding whether it pertains to a bodily function or an administrative correction can alleviate confusion and ensure they are fully informed about their health status and financial obligations. For instance, if a patient sees “voided” next to a lab result, they should inquire if it means the test was invalidated and needs to be repeated. If it appears on a bill, they need to understand if a payment was canceled and if a new balance is due.

In Research and Data Analysis
In medical research, datasets often contain entries that have been voided due to errors, inconsistencies, or specific exclusion criteria. Researchers must be aware of how voided data points are handled to ensure the validity and reliability of their findings. The methodology section of research papers often details how such data is managed.
In conclusion, the term “voided” in medicine is a critical descriptor with distinct physiological and administrative connotations. Whether referring to the fundamental biological act of expelling waste or the administrative act of rendering something invalid, a clear understanding of its meaning is indispensable for effective healthcare delivery, accurate record-keeping, and transparent patient communication.
