Testosterone, often mistakenly perceived as solely a male hormone, plays a vital and multifaceted role in the physiology of women. While present in significantly lower concentrations than in men, this potent androgen is crucial for maintaining numerous bodily functions, influencing everything from sexual health and mood to bone density and muscle mass. Understanding its actions in the female body is essential for appreciating the intricate hormonal balance that underpins women’s overall well-being and can provide context for various health discussions and potential therapeutic interventions.
The production of testosterone in women primarily occurs in the ovaries and the adrenal glands, with a smaller amount synthesized in peripheral tissues. Its effects are mediated through androgen receptors distributed throughout the body. These receptors bind to testosterone, triggering specific cellular responses that impact various systems. The dynamic interplay of testosterone with other hormones, such as estrogen and progesterone, further modulates its influence, creating a complex endocrine landscape that supports female health across the lifespan.
Hormonal Production and Regulation in Women
The female endocrine system is a finely tuned network, and testosterone production is an integral, albeit often under-discussed, component. Unlike the more widely publicized roles of estrogen and progesterone in female biology, testosterone’s contributions are equally significant for a woman’s physical and psychological health.
Ovarian and Adrenal Synthesis
The primary sources of testosterone in women are the ovaries and the adrenal glands. The ovaries, the principal female reproductive organs, produce not only estrogen and progesterone but also a notable amount of androgens, including testosterone. This production is regulated by the hypothalamic-pituitary-gonadal (HPG) axis, with luteinizing hormone (LH) playing a key role in stimulating androgen synthesis in the ovarian theca cells.
The adrenal glands, situated atop the kidneys, are also a significant contributor to a woman’s testosterone levels. They produce androgens as part of the adrenal cortex’s steroidogenesis pathway, alongside cortisol and other essential hormones. This production is influenced by adrenocorticotropic hormone (ACTH) from the pituitary gland. While the ovaries are generally considered the main source, the adrenal contribution becomes more prominent relative to ovarian production after menopause, when ovarian function declines.
The Role of SHBG and Free Testosterone
Testosterone circulates in the bloodstream in both bound and unbound forms. A significant portion of testosterone is bound to sex hormone-binding globulin (SHBG), a protein synthesized by the liver. It also binds to albumin, another liver-produced protein, albeit with lower affinity. The remaining testosterone is free, meaning it is not bound to any protein and is readily available to bind to androgen receptors and exert its physiological effects. This free or unbound testosterone is often referred to as “bioavailable” testosterone, as it represents the fraction that is biologically active.
The balance between bound and free testosterone is crucial. SHBG levels can fluctuate based on various factors, including age, hormonal status (e.g., pregnancy, menopause), and certain medical conditions. Higher SHBG levels lead to more testosterone being bound, thus reducing the amount of free testosterone available for cellular action. Conversely, lower SHBG levels result in higher free testosterone. The accurate assessment of testosterone’s impact often involves considering not just total testosterone but also free or bioavailable testosterone, alongside SHBG levels.
Physiological Functions of Testosterone in Women
Testosterone, despite its lower concentrations in women, exerts a profound influence on a wide array of physiological processes. Its impact is felt across multiple systems, contributing to sexual function, energy levels, mood regulation, and physical strength.
Sexual Health and Libido
One of the most recognized roles of testosterone in women is its contribution to sexual desire, or libido. While estrogen is also crucial for sexual function, testosterone acts as a key driver of sexual interest and arousal. It plays a role in stimulating and maintaining clitoral sensitivity and can influence the physiological responses associated with sexual activity, including vaginal lubrication.
The intricate relationship between testosterone and libido means that changes in testosterone levels can significantly impact a woman’s sexual well-being. Declines in testosterone, which can occur with aging, childbirth, certain medical treatments, or conditions like hypothalamic amenorrhea, are often associated with reduced sexual desire. Conversely, addressing testosterone deficiency in certain contexts can lead to improvements in libido and overall sexual satisfaction. The presence of androgen receptors in the brain areas associated with sexual motivation further underscores its direct impact on sexual drive.
Mood, Energy, and Cognitive Function
Beyond sexual health, testosterone significantly influences a woman’s mood, energy levels, and cognitive capabilities. Many women report experiencing increased vitality, improved mood, and enhanced mental clarity with adequate testosterone levels. It is thought to interact with neurotransmitter systems in the brain, potentially affecting serotonin and dopamine pathways, which are critical for mood regulation.
Low testosterone can manifest as fatigue, lethargy, and a general lack of motivation. Women experiencing these symptoms may find their energy levels significantly compromised, impacting their daily functioning and quality of life. Furthermore, cognitive functions such as concentration, memory, and spatial abilities can also be positively influenced by testosterone. While research is ongoing, the observed benefits suggest that testosterone acts as a neuromodulator, contributing to overall brain health and performance.
Muscle Mass, Bone Density, and Body Composition
Testosterone is an anabolic hormone, meaning it plays a role in building and maintaining muscle mass and strength. In women, it contributes to lean body mass and supports muscle development, which is crucial for physical function, metabolism, and overall health. Adequate testosterone levels help preserve muscle tissue and prevent sarcopenia (age-related muscle loss).
In addition to its anabolic effects on muscle, testosterone is also essential for maintaining bone density. It works synergistically with estrogen to promote bone formation and inhibit bone resorption, thereby reducing the risk of osteoporosis and fractures. This role is particularly important as women age and their estrogen levels decline, making testosterone a vital component in maintaining skeletal integrity. Testosterone also influences body composition by promoting fat metabolism and reducing fat deposition.
Clinical Implications and Hormone Therapy
The understanding of testosterone’s roles in women has opened avenues for clinical investigation and therapeutic interventions. While often prescribed for men with hypogonadism, testosterone therapy for women is a more complex area with evolving guidelines and ongoing research.
Testosterone Deficiency and its Symptoms
Testosterone deficiency in women, sometimes referred to as hypoandrogenism, can arise from various causes. These include aging, surgical removal of the ovaries (oophorectomy), certain medications (like GnRH agonists), hypothalamic amenorrhea (often seen in athletes or those with eating disorders), adrenal insufficiency, and certain pituitary disorders.
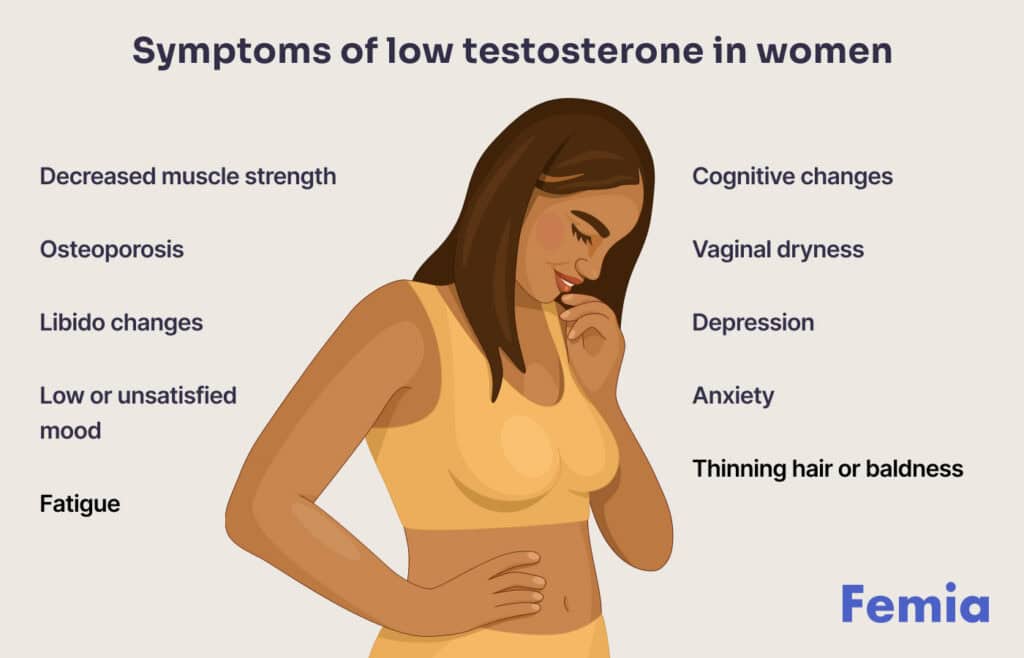
The symptoms of testosterone deficiency in women can be diverse and often overlap with symptoms of other hormonal imbalances or general health issues, making diagnosis challenging. Common complaints include persistent low libido, fatigue, lack of energy, difficulties with concentration, persistent low mood, and decreased physical strength or muscle mass. It’s crucial for healthcare providers to consider testosterone levels when evaluating women presenting with these persistent, unexplained symptoms, especially after ruling out other potential causes.
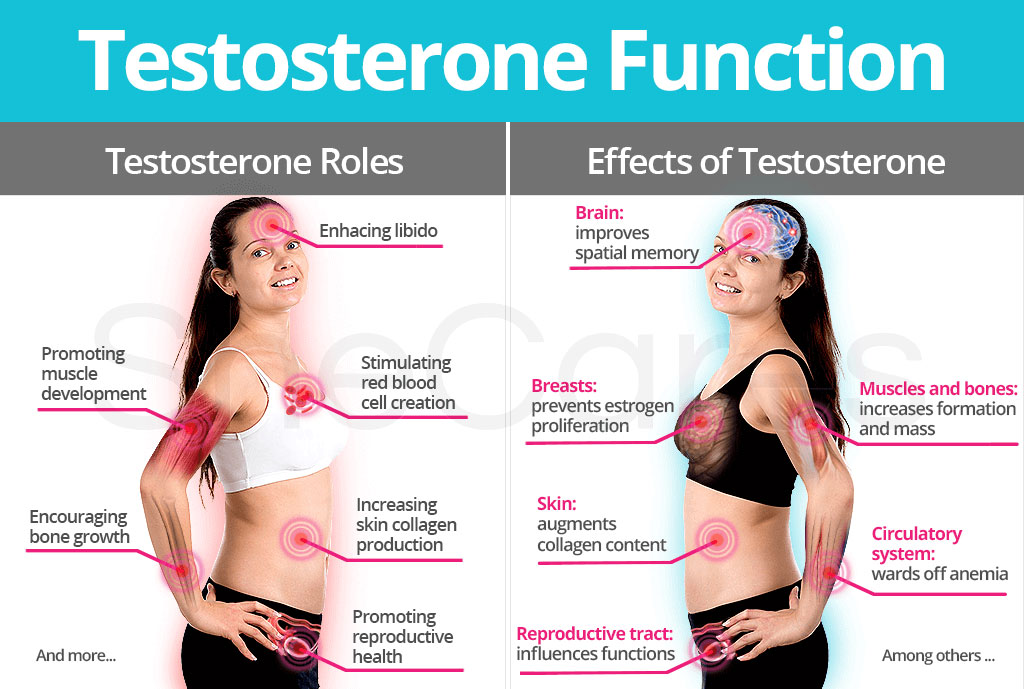
The Use of Testosterone Therapy in Women
Testosterone therapy for women is primarily considered for the treatment of hypoactive sexual desire disorder (HSDD) in postmenopausal women who have already tried and failed other treatments. The goal is to improve sexual desire, arousal, and satisfaction. However, the use of testosterone therapy in women is not without controversy and requires careful consideration.
The available evidence supporting testosterone therapy for HSDD has led to the approval of specific formulations in some regions. However, the optimal dosage, duration of therapy, and long-term safety profile are still subjects of ongoing research and debate. Potential side effects need to be carefully monitored and discussed with a healthcare provider. These can include acne, hirsutism (excessive hair growth), deepening of the voice, and potential adverse effects on lipid profiles or liver function, depending on the formulation used. It is imperative that testosterone therapy for women is prescribed and monitored by experienced healthcare professionals to ensure safety and efficacy, and to individualize treatment based on each woman’s specific needs and health status.
