A pinched nerve, medically known as nerve compression or entrapment, is a common condition that can cause a range of uncomfortable and sometimes debilitating sensations. Understanding what a pinched nerve feels like is the first step toward effective diagnosis and treatment. The experience is highly individual, varying based on the nerve’s location, the severity of the compression, and the underlying cause. However, several hallmark symptoms are consistently reported by those affected.
The Spectrum of Sensations: Beyond Simple Pain
While pain is often the most prominent symptom, a pinched nerve can manifest in a much broader array of sensory experiences. These sensations are a direct result of the nerve being squeezed, inflamed, or irritated, which disrupts the electrical signals it transmits between the brain and the rest of the body.

Burning and Tingling
One of the most frequently described sensations is a burning or searing feeling. This can range from a mild warmth to an intense, fire-like sensation. It often accompanies a prickling or “pins and needles” feeling, medically termed paresthesia. This tingling sensation is akin to the feeling you get when your foot falls asleep, but it can be persistent and localized to the area served by the compressed nerve. This is because the pressure can interfere with the nerve’s ability to send normal sensory signals.
Numbness and Loss of Sensation
Conversely to burning and tingling, a pinched nerve can also lead to a significant loss of sensation. The affected area may feel numb, as if it’s no longer connected to your body. This numbness can be partial or complete, making it difficult to feel touch, temperature, or pressure. In some cases, individuals might not realize they have injured the area until they accidentally bump or burn it, as the warning signals are dulled or absent.
Radiating Pain
Pain associated with a pinched nerve rarely stays localized. It often radiates along the path of the affected nerve. For instance, a pinched nerve in the neck (cervical radiculopathy) might cause pain that shoots down the arm, into the shoulder, elbow, wrist, and even fingers. Similarly, a pinched nerve in the lower back (lumbar radiculopathy, often referred to as sciatica) can cause pain that travels down the leg, into the foot. This radiating pain is often sharp, shooting, or electric-shock-like.
Weakness and Muscle Atrophy
Beyond sensory disturbances, a pinched nerve can also affect motor function. Nerves carry signals that control muscle movement. When a nerve is compressed, these signals can be disrupted, leading to weakness in the muscles supplied by that nerve. This weakness might make it difficult to perform everyday tasks, such as gripping objects, lifting the foot, or even maintaining balance. Over time, if the compression is prolonged, the affected muscles can begin to waste away, a process called atrophy, becoming visibly smaller and weaker.
Cramping and Spasms
Some individuals experience involuntary muscle contractions, or spasms, in the area affected by the pinched nerve. These cramps can be painful and may occur intermittently or persist. They are another indication that the nerve’s normal signaling to the muscles has been disrupted.
Changes in Temperature Sensation
In addition to feeling touch, nerves also transmit temperature signals. A pinched nerve can alter how you perceive heat and cold. You might feel an area is abnormally hot or cold, even if its actual temperature is normal. Alternatively, you might have a reduced ability to feel temperature at all in the affected region.
Common Locations and Associated Feelings
The specific location of a pinched nerve significantly influences the type and pattern of symptoms experienced.
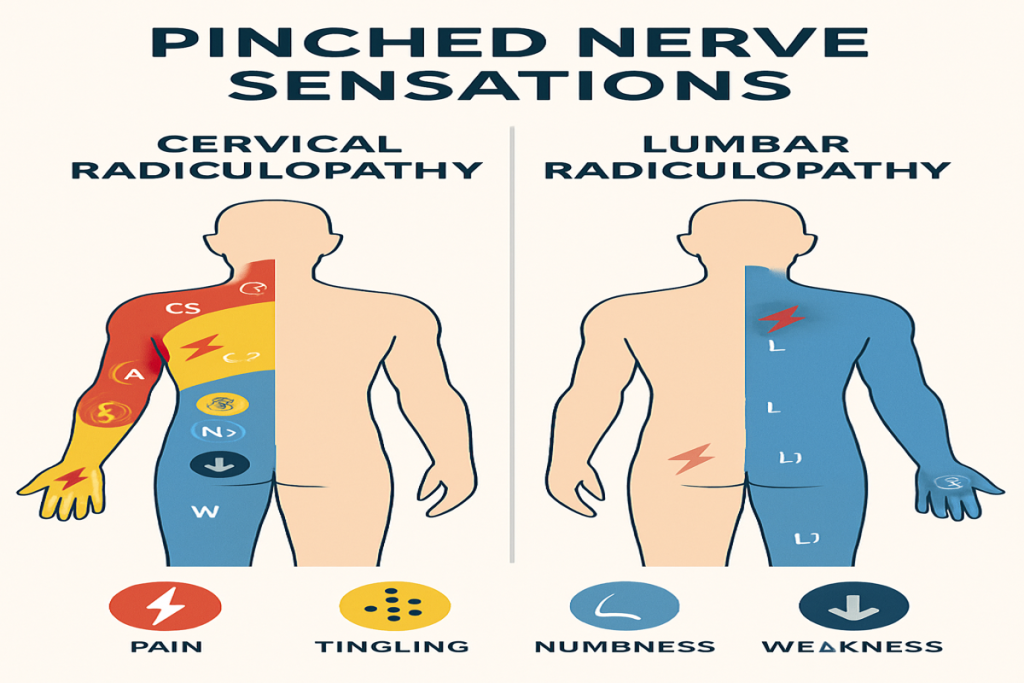
Pinched Nerve in the Neck (Cervical Radiculopathy)
When a nerve root in the cervical spine is compressed, symptoms typically radiate into the shoulder, arm, and hand.
- Sensations: Burning pain down the arm, tingling in the fingers, numbness in the hand, weakness in the arm or grip.
- Aggravating factors: Certain neck movements, like turning the head or looking up, can worsen the symptoms.
Pinched Nerve in the Lower Back (Lumbar Radiculopathy / Sciatica)
Compression of a nerve root in the lumbar spine often leads to sciatica, characterized by pain radiating down the leg.
- Sensations: Sharp, shooting, or electric pain down the back of the leg, tingling or numbness in the foot, weakness in the leg or foot, difficulty walking or standing for long periods.
- Aggravating factors: Sitting for extended periods, bending forward, coughing, or sneezing can exacerbate the pain.
Carpal Tunnel Syndrome (Pinched Nerve in the Wrist)
The median nerve, which passes through the carpal tunnel in the wrist, can become compressed, leading to carpal tunnel syndrome.
- Sensations: Numbness and tingling in the thumb, index, middle, and part of the ring finger, a burning sensation in the palm, pain that may radiate up the arm, weakness in the hand and difficulty gripping.
- Aggravating factors: Repetitive hand motions, sleeping with the wrist flexed, holding objects for extended periods.
Thoracic Outlet Syndrome (Pinched Nerve in the Shoulder/Neck Area)
This condition involves compression of nerves or blood vessels in the space between the collarbone and the first rib.
- Sensations: Varies widely, but can include pain, numbness, and tingling in the arm and hand, weakness, and a bluish discoloration of the hand.
- Aggravating factors: Lifting the arms overhead, carrying heavy objects, or specific arm positions.
Pinched Nerve in the Elbow (Cubital Tunnel Syndrome)
Similar to carpal tunnel syndrome, but affecting the ulnar nerve as it passes through the cubital tunnel at the elbow.
- Sensations: Numbness and tingling in the ring and little fingers, pain on the inside of the elbow, weakness in the hand.
- Aggravating factors: Keeping the elbow bent for long periods, leaning on the elbow.
Identifying the Cause: What’s Compressing the Nerve?
The feeling of a pinched nerve is a symptom, not a diagnosis. To effectively manage the condition, it’s crucial to identify what is causing the nerve compression. Common culprits include:
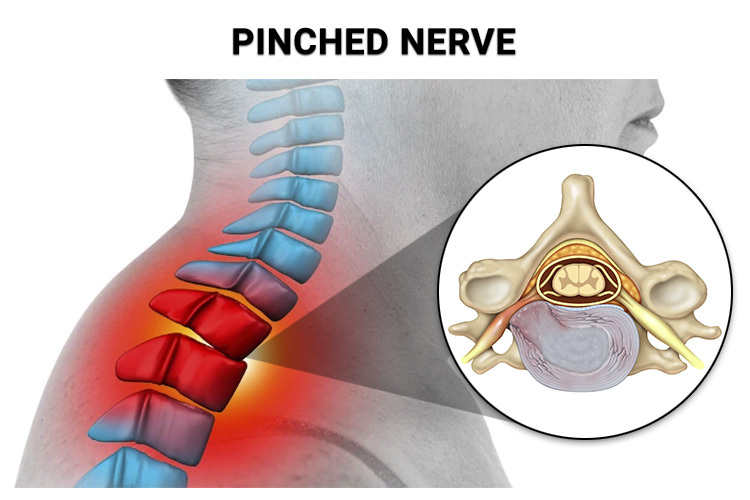
Herniated or Bulging Discs
In the spine, the intervertebral discs act as cushions between the vertebrae. If a disc becomes damaged, it can bulge or rupture, pressing on nearby nerve roots. This is a frequent cause of sciatica and cervical radiculopathy.
Bone Spurs (Osteophytes)
These bony growths can develop on the vertebrae or other bones, narrowing the space where nerves pass through and leading to compression. This is more common in conditions like osteoarthritis.
Swelling and Inflammation
Arthritis, injuries, or overuse can cause inflammation and swelling in tissues surrounding nerves, leading to pressure. Tendinitis and bursitis are examples of inflammatory conditions that can cause nerve compression.
Repetitive Motions
Performing the same movements repeatedly, especially in jobs or hobbies, can lead to overuse injuries that cause swelling and irritation, eventually compressing nerves. Carpal tunnel syndrome is a prime example.
Trauma or Injury
Direct impact, falls, or accidents can cause swelling or misalignment of bones, which can pinch nerves. Fractures can also directly impinge on nerves.
Medical Conditions
Certain medical conditions, such as diabetes, thyroid disorders, and rheumatoid arthritis, can increase the risk of nerve compression due to nerve damage, inflammation, or fluid retention.
When to Seek Medical Attention
While occasional tingling or mild discomfort might resolve on its own, persistent or severe symptoms warrant medical evaluation. It is advisable to consult a healthcare professional if you experience any of the following:
- Persistent or worsening pain: Pain that doesn’t improve with rest or over-the-counter pain relief.
- Significant weakness: Difficulty performing daily tasks due to muscle weakness.
- Numbness or tingling that doesn’t resolve: Continuous loss of sensation.
- Loss of bowel or bladder control: This is a medical emergency and requires immediate attention.
- Symptoms that interfere with sleep or daily activities: When discomfort significantly impacts your quality of life.
A proper diagnosis typically involves a thorough medical history, physical examination, and may include imaging tests like X-rays, MRI, or CT scans, as well as nerve conduction studies and electromyography (NCMG) to assess nerve function. Understanding the nuances of what a pinched nerve feels like empowers individuals to communicate effectively with their healthcare providers, paving the way for accurate diagnosis and effective management strategies.
