The Mean Corpuscular Hemoglobin (MCH) blood test is a crucial component of a complete blood count (CBC), providing vital insights into the health of your red blood cells. While the title itself might seem purely medical, understanding MCH can indirectly connect to broader technological advancements, particularly in areas like remote sensing and diagnostics. For the purpose of this discussion, we will focus on the technological applications and implications that can be inferred from such a diagnostic test, framing it within the broader context of Tech & Innovation.
This exploration will delve into how innovative technologies are enhancing our ability to interpret and utilize diagnostic information like MCH, paving the way for more precise, personalized, and accessible healthcare solutions. We will examine the underlying principles, technological advancements that support its interpretation, and future implications.
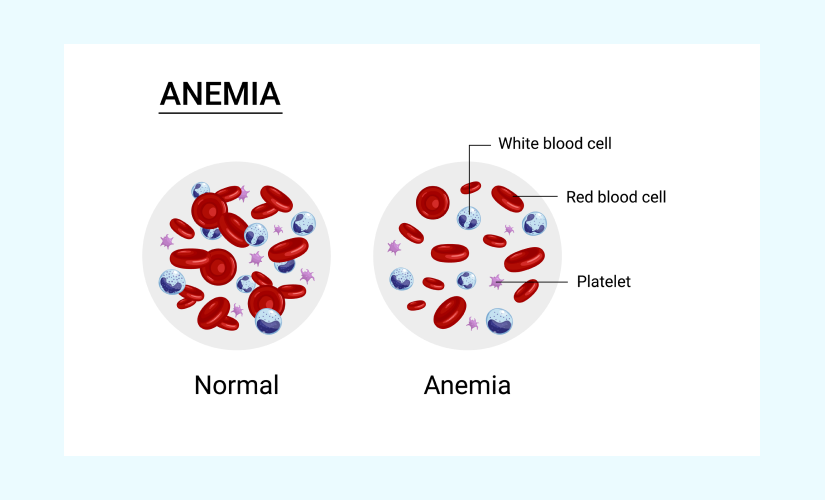
Understanding the Fundamentals of MCH
At its core, the MCH test measures the average amount of hemoglobin found within a single red blood cell. Hemoglobin is the protein responsible for carrying oxygen from the lungs to the rest of the body. Therefore, MCH is a direct indicator of the hemoglobin concentration within your erythrocytes. This seemingly simple measurement can reveal a great deal about your body’s ability to transport oxygen and can be a significant marker for various health conditions, most notably different types of anemia.
The Role of Hemoglobin and Red Blood Cells
Red blood cells, or erythrocytes, are the workhorses of oxygen transport. Produced in the bone marrow, these biconcave discs are packed with hemoglobin. A healthy red blood cell is essential for maintaining adequate oxygen levels throughout the body, which in turn fuels all cellular functions. When the number of red blood cells, their size, or their hemoglobin content is abnormal, it can signal underlying health issues. The MCH test, by focusing on the average hemoglobin content per cell, helps differentiate between various causes of anemia and other blood disorders.
How MCH is Measured and Interpreted
The MCH value is typically reported in picograms (pg) per cell. A standard CBC panel will include MCH alongside other red blood cell indices such as Mean Corpuscular Volume (MCV) and Mean Corpuscular Hemoglobin Concentration (MCHC). These values are determined using automated hematology analyzers, sophisticated pieces of medical technology. These analyzers use a combination of electrical impedance and light scattering to count cells and measure their properties.
Interpreting MCH involves comparing the patient’s result to established reference ranges, which can vary slightly between laboratories. Deviations from these ranges, whether high or low, prompt further investigation. A low MCH value, often seen in microcytic anemias (where red blood cells are smaller than normal), suggests that each red blood cell is carrying less hemoglobin than it should. Conversely, a high MCH value, typically associated with macrocytic anemias (where red blood cells are larger than normal), indicates that individual red blood cells are carrying an above-average amount of hemoglobin.
Technological Advancements in Hematology Diagnostics
The ability to precisely measure and interpret MCH, and other red blood cell indices, is a testament to the rapid advancements in biomedical technology. These innovations have transformed diagnostic laboratories from manual, time-consuming processes to highly automated, accurate, and efficient operations. This evolution directly impacts patient care by providing faster results and enabling more informed clinical decisions.
Automated Hematology Analyzers: The Backbone of MCH Measurement
Modern hematology analyzers are complex instruments that leverage a range of technologies to perform CBCs. They utilize principles like:
- Electrical Impedance: As cells pass through a small aperture, they disrupt an electrical current. The magnitude of this disruption is proportional to the cell’s volume, allowing for accurate MCV determination.
- Flow Cytometry: This advanced technique involves passing cells in a fluid stream through a laser beam. Light scatter patterns (forward and side scatter) provide information about cell size, granularity, and complexity. This is crucial for differentiating various white blood cell types and can also contribute to red blood cell analysis.
- Optical Detection: Photometric methods are used to measure the hemoglobin concentration within lysed red blood cells. By analyzing the light absorption of hemoglobin in solution, the total hemoglobin can be determined, which, when combined with red blood cell counts, allows for the calculation of MCH and MCHC.
These automated systems significantly reduce the risk of human error, increase throughput, and provide a wealth of data that can be integrated into electronic health records for longitudinal tracking and analysis.

Artificial Intelligence and Machine Learning in Data Interpretation
The sheer volume of data generated by hematology analyzers presents an opportunity for artificial intelligence (AI) and machine learning (ML) algorithms. These technologies are increasingly being deployed to:
- Improve Accuracy and Efficiency: AI can analyze complex patterns in CBC data, identifying subtle anomalies that might be missed by human review, especially in high-volume labs. ML models can be trained on vast datasets to predict the likelihood of specific conditions based on a patient’s MCH and other indices.
- Flag Abnormalities: Sophisticated algorithms can proactively flag potentially critical results, alerting laboratory professionals and clinicians for urgent attention. This is particularly valuable in identifying early signs of serious hematological diseases.
- Personalize Reference Ranges: AI can analyze patient demographics, clinical history, and genetic information to establish more personalized reference ranges for MCH and other parameters, leading to more accurate diagnoses for individual patients.
- Aid in Differential Diagnosis: By correlating MCH values with other CBC parameters and clinical symptoms, AI can assist clinicians in narrowing down the possible causes of an abnormal MCH, streamlining the diagnostic pathway.
The integration of AI into hematology diagnostics represents a significant leap forward, moving beyond simple data reporting to intelligent data interpretation and actionable insights.
The Future of Red Blood Cell Diagnostics and Broader Implications
The ongoing evolution of diagnostic technologies, driven by innovations in areas like microfluidics, biosensors, and point-of-care testing, promises to make MCH analysis and other blood tests more accessible, faster, and even more informative. The principles underlying MCH measurement and interpretation have far-reaching implications beyond traditional clinical settings, touching upon fields like remote sensing and advanced monitoring.
Point-of-Care (POC) Testing and Decentralized Diagnostics
The drive towards point-of-care testing is revolutionizing healthcare delivery. Imagine a future where a simple finger prick blood sample can be analyzed for MCH and other critical parameters not just in a central laboratory, but in a doctor’s office, a remote clinic, or even at home. Microfluidic devices, often powered by miniaturized analytical engines, are enabling this decentralization.
These POC devices leverage advanced materials and micro-fabrication techniques to perform complex assays with minimal sample volume and rapid turnaround times. For MCH analysis, this could translate to:
- Immediate Feedback: Allowing clinicians to make treatment decisions in real-time during a patient visit.
- Improved Access in Underserved Areas: Bringing essential diagnostic capabilities to regions with limited access to traditional laboratory infrastructure.
- Enhanced Chronic Disease Management: Enabling patients with conditions like anemia to monitor their MCH levels regularly from home, fostering proactive health management and reducing the need for frequent clinic visits.
This trend mirrors the broader technological push in various sectors towards miniaturization, increased portability, and enhanced user-friendliness.

Integration with Wearable Technology and Remote Monitoring
The convergence of medical diagnostics and wearable technology is an exciting frontier. While current wearables primarily focus on vital signs like heart rate and SpO2, future iterations could incorporate biosensors capable of analyzing blood components. Although direct, non-invasive MCH measurement is still some way off, the principles of analyzing physiological markers could be applied.
The concept of remote sensing, which involves collecting information about an object or phenomenon without physical contact, has parallels in how we can potentially monitor health from afar. Just as drones equipped with advanced sensors can gather data about environmental conditions, future integrated wearable systems could continuously or periodically collect subtle physiological indicators that correlate with blood parameters like MCH.
For example, technologies might evolve to detect changes in skin tone, capillary refill time, or oxygenation patterns that are indirectly indicative of hemoglobin levels. This could lead to:
- Early Warning Systems: Alerting individuals and healthcare providers to potential health issues before symptoms become severe.
- Continuous Health Surveillance: Providing a more comprehensive understanding of an individual’s health status over time.
- Personalized Interventions: Enabling timely and targeted interventions based on real-time physiological data.
While this is a more futuristic outlook, the foundational technological principles – precision measurement, data analysis, and remote information gathering – are already driving innovation in fields like MCH testing and beyond. The journey from understanding a simple blood test like MCH to harnessing advanced technological capabilities for proactive and pervasive health monitoring underscores the transformative power of innovation.
