The human papillomavirus (HPV) is a common sexually transmitted infection, and while often associated with genital warts, it can also affect the mouth and throat. Understanding what HPV-related lesions look like in the oral cavity is crucial for early detection and management. This article will delve into the visual characteristics of oral HPV infections, focusing on the types of lesions they can cause and the importance of recognizing these signs.
Understanding Oral HPV and Its Manifestations
Oral HPV infections occur when the virus enters the skin or mucous membranes of the mouth, typically through oral sex. While many oral HPV infections are asymptomatic and clear on their own, some can lead to persistent infections that may manifest as visible lesions. These lesions can vary in appearance and location, making them sometimes difficult to distinguish from other oral conditions.
The Spectrum of Oral HPV Lesions
The appearance of oral HPV lesions is largely dependent on the specific type of HPV and the individual’s immune response. The most common visible manifestation of oral HPV is warts, also known as papillomas. These can be further categorized by their appearance and common locations within the oral cavity.
Squamous Cell Papillomas (Common Warts in the Mouth)
Squamous cell papillomas are benign (non-cancerous) growths caused by low-risk HPV types, most commonly HPV 6 and 11. These are the most frequent type of HPV-related lesion found in the mouth.
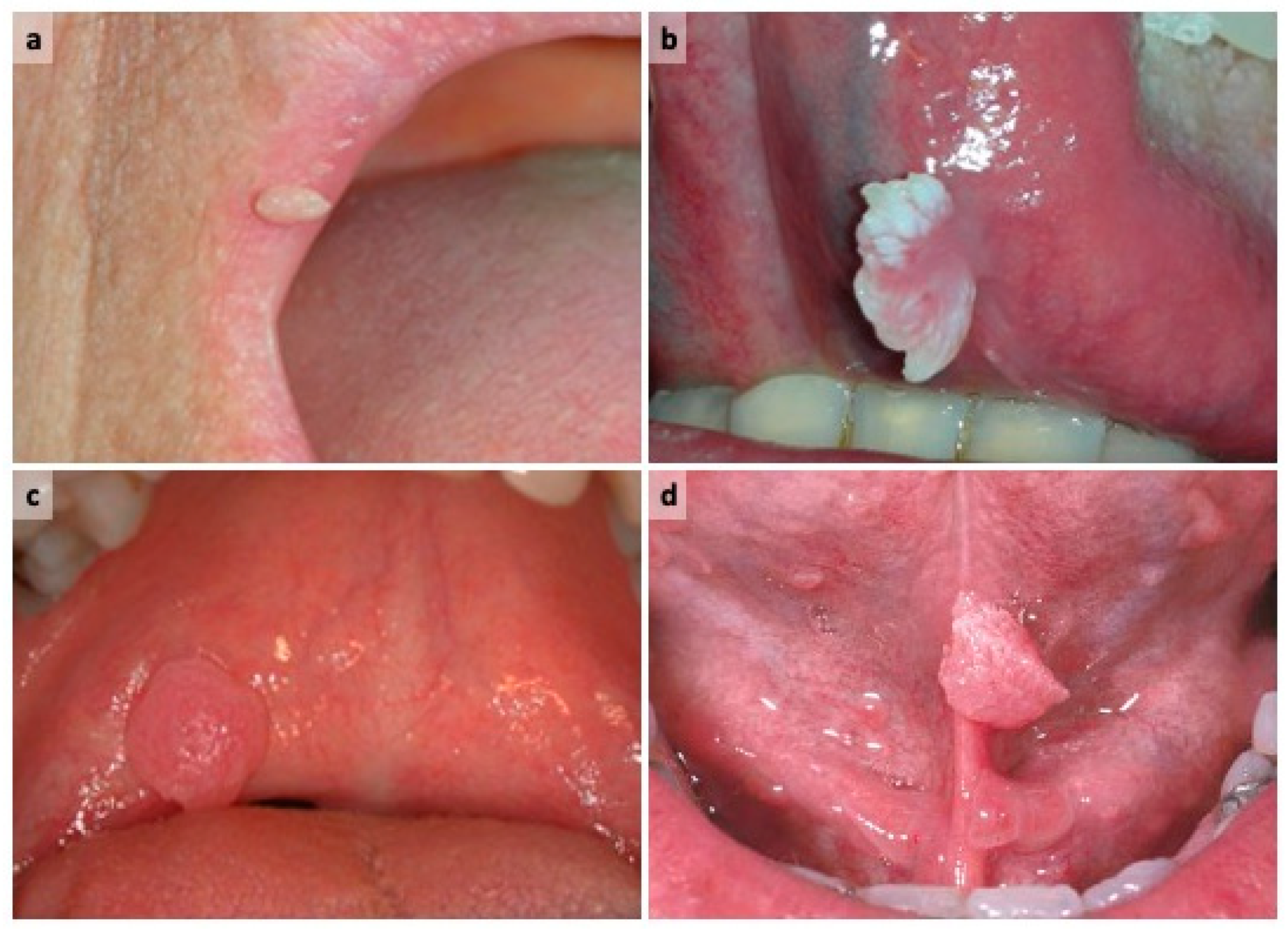
- Appearance: Squamous cell papillomas typically present as single or multiple, small, cauliflower-like or finger-like projections. They are usually pink or flesh-colored, matching the surrounding oral tissue, which can make them subtle. The surface is often rough and irregular, with a papillated (nipple-like) texture.
- Location: They can appear on various parts of the oral mucosa, including the tongue, palate (roof of the mouth), lips, gums, and inside the cheeks. When they occur on the tongue, they may be more readily noticeable due to the tongue’s constant movement and the texture of the organ.
- Feel: These lesions are generally soft to the touch and may be painless. However, if they grow larger, they can sometimes cause minor discomfort or interfere with chewing or speaking.
- Multiple Lesions: While a single papilloma is common, individuals can develop multiple lesions, especially if their immune system is compromised or if the virus is spread through autoinoculation (spreading the virus from one area of the body to another).
Focal Epithelial Hyperplasia (Heck’s Disease)
Focal epithelial hyperplasia, also known as Heck’s disease, is another benign condition caused by HPV, primarily HPV 13 and 32. It is more common in children and adolescents, particularly in certain geographic regions and among specific ethnic groups.
- Appearance: Lesions in Heck’s disease are typically small, sessile (flat-based) papules or nodules. They are often described as being dome-shaped, smooth, and sometimes translucent. Unlike the cauliflower-like appearance of squamous cell papillomas, Heck’s disease lesions tend to be more uniform in color and texture.
- Location: These lesions are most commonly found on the labial and buccal mucosa (inside of the lips and cheeks), but can also occur on the tongue and gingiva (gums). They often appear in clusters.
- Feel: They are usually soft and asymptomatic, not causing pain or significant discomfort.
- Distinguishing Features: The prevalence of multiple, small, smooth papules in a typical location often helps differentiate Heck’s disease from other oral conditions.
Less Common but Significant Lesions: Oral Warts and Oral Cancer
While the majority of oral HPV lesions are benign, it’s crucial to be aware of the potential for more serious conditions linked to persistent HPV infections, particularly those caused by high-risk HPV types such as HPV 16 and 18.
Condyloma Acuminatum (Genital Wart-like Lesions in the Mouth)
Condyloma acuminatum, commonly known as genital warts, can, in rare instances, occur in the oral cavity as a result of oral sex. These are caused by the same low-risk HPV types that cause genital warts.
- Appearance: Oral condylomata acuminata can resemble squamous cell papillomas but may be larger, more numerous, and have a more pronounced cauliflower-like or branching structure. The surface can be verrucous (warty) and friable (easily crumbled). They can vary in color from pinkish to whitish.
- Location: They can appear on the lips, tongue, palate, and pharynx.
- Potential for Aggravation: These lesions can be more prone to bleeding and can sometimes be associated with discomfort or itching.
Oral Squamous Cell Carcinoma (HPV-Related Oropharyngeal Cancer)
High-risk HPV types, especially HPV 16, are a significant cause of oropharyngeal squamous cell carcinoma (OPSCC), which affects the back of the throat, base of the tongue, and tonsils. While these are not warts in the traditional sense, it is vital to understand that persistent HPV infection can lead to malignancy. Early signs of OPSCC can be subtle and easily mistaken for less serious conditions.
- Appearance: Early signs of oral cancer related to HPV can be varied. They may appear as:
- A persistent sore that does not heal.
- A red or white patch (erythroplakia or leukoplakia) that doesn’t go away.
- A lump or thickening of the tissues in the mouth or throat.
- Pain or difficulty swallowing.
- A change in voice.
- Unexplained numbness in the mouth or throat.
- Location: While HPV-related OPSCC often affects the oropharynx (back of the throat, tonsils, base of the tongue), it can also occur in other oral sites.
- Distinguishing from Benign Lesions: The key difference between benign HPV lesions and oral cancer is the persistence and progression of the abnormal tissue. Unlike benign warts that may resolve, cancerous lesions tend to grow, spread, and cause more significant symptoms.
The Importance of Visual Recognition and Professional Diagnosis

Recognizing the visual cues of oral HPV lesions is the first step towards seeking appropriate medical attention. However, it is crucial to emphasize that self-diagnosis is not recommended. Many oral conditions can mimic HPV-related lesions, and only a qualified healthcare professional can provide an accurate diagnosis.
When to Seek Medical Advice
Any new or unusual lesion in the mouth, regardless of its appearance, should be evaluated by a dentist or doctor. Specific reasons to seek immediate medical advice include:
- Persistence: If a lesion has been present for more than two weeks and is not showing signs of healing.
- Changes in Appearance: If a lesion starts to grow, change color, bleed easily, or develop irregular borders.
- Associated Symptoms: If the lesion is accompanied by pain, difficulty swallowing, changes in voice, or unexplained bleeding.
- Multiple Lesions: The presence of multiple lesions, especially if they are growing or causing concern, warrants professional evaluation.
- Known HPV Exposure: If you have a history of HPV infection or know your partner has genital warts, it is wise to be extra vigilant about oral health.
The Diagnostic Process: Beyond Visual Inspection
When you visit a healthcare provider for a concerning oral lesion, they will perform a thorough oral examination. This may involve:
- Visual Inspection and Palpation: The clinician will carefully look at and feel the lesion to assess its size, shape, texture, and borders.
- Medical History: They will ask about your sexual history, any relevant symptoms, and overall health.
- Biopsy: If there is any suspicion of malignancy or for definitive diagnosis of any oral lesion, a biopsy is often performed. This involves taking a small sample of the tissue to be examined under a microscope by a pathologist. This is the gold standard for diagnosing oral cancer and can also confirm the presence of HPV in benign lesions.
- HPV Testing: In some cases, specific HPV DNA tests can be performed on the biopsy sample to identify the presence and type of HPV.
Prevention and Management of Oral HPV
While visual recognition is important for detection, prevention remains a cornerstone of managing HPV infections, including those that can affect the mouth.
Vaccination as a Primary Prevention Tool
The HPV vaccine is highly effective in preventing infections with the most common and oncogenic (cancer-causing) HPV types.
- Targeted Protection: The vaccine protects against HPV types that are responsible for the vast majority of HPV-related cancers, including oropharyngeal cancers, as well as genital warts.
- Recommended Age Groups: The vaccine is recommended for adolescents before they become sexually active. Catch-up vaccination is also available for young adults.
- Ongoing Research: While the vaccine is primarily aimed at preventing new infections, research is ongoing into its potential therapeutic benefits for existing infections.
Safe Sexual Practices
Practices that reduce the transmission of HPV are also crucial for oral health.
- Condom Use: While condoms do not offer complete protection against HPV because the virus can be present on skin not covered by the condom, they can significantly reduce the risk of transmission during oral sex.
- Limiting Number of Partners: Reducing the number of sexual partners can lower the overall risk of exposure to HPV.
- Communication: Open communication with sexual partners about HPV status and history can help inform decisions about risk reduction.
Lifestyle Factors and Immune Support
A strong immune system plays a vital role in clearing HPV infections and preventing the development of lesions.
- Healthy Lifestyle: Maintaining a healthy diet, exercising regularly, getting sufficient sleep, and managing stress can all contribute to a robust immune system.
- Avoiding Smoking and Excessive Alcohol Consumption: These lifestyle factors can impair immune function and increase the risk of developing HPV-related cancers.

Conclusion: Vigilance and Professional Care
The visual appearance of HPV in the mouth ranges from subtle, cauliflower-like growths (papillomas) to more concerning, persistent lesions that could indicate precancerous changes or oral cancer. While many oral HPV infections are benign and resolve on their own, the potential for serious health consequences necessitates vigilance.
Regular oral examinations by dental professionals are essential for early detection of any abnormalities. If you notice any new, persistent, or changing lesions in your mouth, do not hesitate to seek prompt medical evaluation. Understanding what to look for, coupled with preventive measures such as vaccination and safe sexual practices, empowers individuals to protect their oral health and well-being from the potential impact of HPV. Early diagnosis and intervention are key to successful management and prevention of complications.
