The term “high enzymes in liver” refers to an elevated level of certain enzymes, particularly liver enzymes, detected in the blood through a liver function test. These enzymes are crucial proteins that facilitate biochemical reactions within liver cells. When liver cells are damaged or inflamed, they release these enzymes into the bloodstream, leading to higher than normal concentrations. Understanding what causes these elevated levels is essential for diagnosing and managing potential liver conditions.
Understanding Liver Enzymes and Their Significance
Liver enzymes are a group of proteins that play vital roles in the metabolic processes occurring in the liver. When liver cells are healthy, these enzymes are largely contained within the cells. However, any form of damage, inflammation, or disease affecting the liver can cause these cells to rupture, releasing their enzyme contents into the bloodstream. A blood test measures the activity or concentration of these enzymes to assess liver health.
Key Liver Enzymes and Their Roles
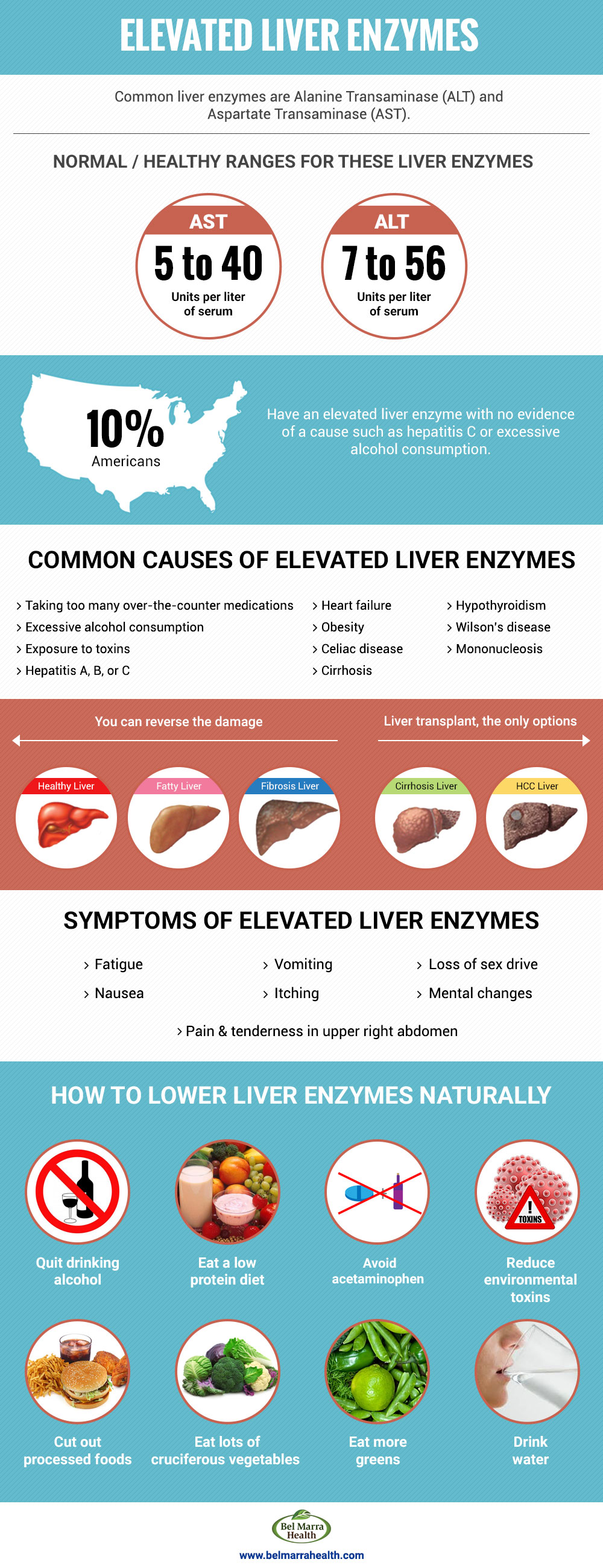
Several key enzymes are commonly measured in liver function tests. Each has specific functions within the liver, and their elevation can point towards particular types of liver damage.
Alanine Aminotransferase (ALT)
Alanine aminotransferase (ALT), also known as serum glutamic-pyruvic transaminase (SGPT), is an enzyme predominantly found in the liver. It plays a crucial role in the metabolism of amino acids. When liver cells are damaged, ALT is released into the bloodstream, making it a sensitive indicator of hepatocellular injury (damage to liver cells themselves). Elevated ALT levels are often one of the first signs of liver disease, even before symptoms appear. Causes of elevated ALT can range from viral hepatitis and fatty liver disease to certain medications and alcohol abuse.
Aspartate Aminotransferase (AST)
Aspartate aminotransferase (AST), formerly known as serum glutamic-oxaloacetic transaminase (SGOT), is an enzyme found in the liver, heart, muscles, kidneys, and brain. While it is present in the liver, its presence in other tissues means that elevated AST levels can indicate damage to organs other than the liver. In the context of liver health, AST is released into the bloodstream when there is liver cell damage. The AST/ALT ratio can sometimes provide clues about the underlying cause of liver damage. For instance, a higher AST than ALT ratio might suggest alcoholic liver disease, while a higher ALT than AST ratio is often seen in viral hepatitis or non-alcoholic fatty liver disease.
Alkaline Phosphatase (ALP)
Alkaline phosphatase (ALP) is an enzyme primarily found in the liver, bile ducts, bones, and intestines. Elevated ALP levels can indicate issues with the bile ducts or liver, as well as bone disease. In the liver, ALP is involved in bile production and transport. When there is a blockage in the bile ducts or inflammation of the liver that affects bile flow (cholestasis), ALP levels can rise significantly. It’s important to consider other liver enzymes and clinical symptoms to differentiate liver-related ALP elevations from bone-related causes.
Gamma-Glutamyl Transferase (GGT)
Gamma-glutamyl transferase (GGT) is an enzyme found in liver cells and bile ducts. Elevated GGT levels are a sensitive indicator of liver and bile duct disease, particularly in cases involving alcohol abuse or bile duct obstruction. GGT is often elevated when other liver enzymes are also high, and it can remain elevated even after other enzymes have normalized, making it useful for monitoring ongoing liver damage or identifying a history of heavy alcohol consumption.
Causes of Elevated Liver Enzymes
A variety of factors can lead to an increase in liver enzymes, ranging from lifestyle choices and infections to chronic diseases and certain medications. Identifying the underlying cause is critical for effective treatment.
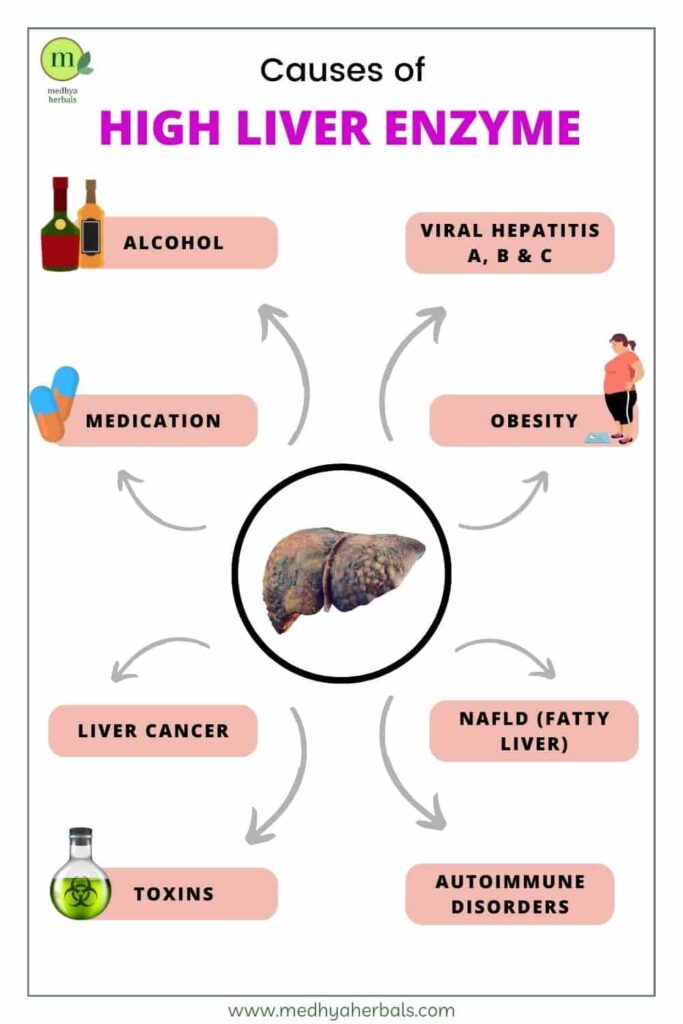
Common Causes and Risk Factors
The reasons behind elevated liver enzymes are diverse and often interconnected. Understanding these common culprits is the first step in addressing the issue.
Viral Hepatitis
Viral hepatitis, including Hepatitis A, B, and C, are infections that directly attack the liver, causing inflammation and cell damage. This damage leads to the release of liver enzymes into the bloodstream. Hepatitis B and C, in particular, can become chronic, leading to long-term liver disease, cirrhosis, and even liver cancer if left untreated. Symptoms can include fatigue, jaundice (yellowing of the skin and eyes), abdominal pain, and nausea.
Fatty Liver Disease (NAFLD/NASH)
Non-alcoholic fatty liver disease (NAFLD) is a condition where excess fat accumulates in the liver, not related to excessive alcohol consumption. It is strongly associated with metabolic syndrome, obesity, type 2 diabetes, and high cholesterol. NAFLD can progress to non-alcoholic steatohepatitis (NASH), a more severe form characterized by inflammation and liver cell damage. Elevated ALT and AST are common in both NAFLD and NASH.
Alcoholic Liver Disease
Excessive and prolonged alcohol consumption is a leading cause of liver damage. Alcohol can directly injure liver cells, leading to inflammation, fat accumulation, and eventually cirrhosis. Alcoholic liver disease encompasses a spectrum of conditions, including alcoholic fatty liver, alcoholic hepatitis, and alcoholic cirrhosis. Elevated AST and ALT, often with a higher AST/ALT ratio, are characteristic of this condition.
Medications and Toxins
Many medications, both prescription and over-the-counter, can cause liver damage as a side effect. This includes common drugs like acetaminophen (Tylenol) when taken in excessive doses, statins used to lower cholesterol, and certain antibiotics and antifungals. Exposure to environmental toxins, industrial chemicals, and even certain herbal supplements can also injure the liver. This type of liver injury is often referred to as drug-induced liver injury (DILI).
Autoimmune Hepatitis
In autoimmune hepatitis, the body’s immune system mistakenly attacks healthy liver cells, causing inflammation and damage. This condition can affect people of all ages and genders but is more common in women. Elevated liver enzymes, particularly ALT and AST, are a hallmark of autoimmune hepatitis. Other symptoms can include fatigue, jaundice, abdominal pain, and joint pain.
Genetic Liver Diseases
Certain genetic disorders can predispose individuals to liver problems. Hemochromatosis, a condition where the body absorbs too much iron, can lead to iron overload in the liver, causing damage. Wilson’s disease, a rare genetic disorder, results in an accumulation of copper in the liver, brain, and other organs. These conditions can manifest with elevated liver enzymes as the liver struggles to process these excess substances.
Other Potential Causes
Beyond the common culprits, several other factors can contribute to elevated liver enzymes.
Heart Failure
While primarily a cardiac condition, severe heart failure can lead to reduced blood flow to the liver. This congestion can cause liver damage and a subsequent rise in liver enzymes, particularly AST. This is often referred to as “cardiac hepatopathy.”
Celiac Disease
Celiac disease, an autoimmune disorder triggered by gluten, can sometimes be associated with elevated liver enzymes, particularly ALT. The exact mechanism is not fully understood, but it is believed to be related to inflammation and malabsorption.
Thyroid Disorders
Both an overactive thyroid (hyperthyroidism) and an underactive thyroid (hypothyroidism) can impact liver function and lead to subtle changes in liver enzyme levels.
Muscle Injury
Since AST is also found in muscle tissue, strenuous exercise or muscle injury can lead to a temporary increase in AST levels. This is why doctors often ask about recent physical activity before interpreting AST results.
Diagnosis and Management of High Liver Enzymes
When liver enzymes are found to be elevated, a thorough diagnostic process is initiated to determine the cause and appropriate course of action. This typically involves a combination of medical history, physical examination, further laboratory tests, and imaging studies.
Diagnostic Evaluation
The initial detection of high liver enzymes prompts a deeper investigation into the liver’s health and the potential underlying reasons for the elevation.
Medical History and Physical Examination
A healthcare provider will begin by gathering detailed information about your medical history, including any existing conditions, medications you are taking, alcohol consumption habits, family history of liver disease, and recent lifestyle changes. A physical examination may reveal signs such as jaundice, abdominal swelling, enlarged liver or spleen, or tenderness in the upper right abdomen.
Comprehensive Liver Function Tests
Beyond the initial screening enzymes, a panel of liver function tests provides a more detailed picture of liver health. This can include tests for bilirubin (which indicates how well the liver is processing waste products), albumin and total protein (which reflect the liver’s ability to produce essential proteins), and prothrombin time (which measures how quickly blood clots, indicating the liver’s production of clotting factors).
Further Blood Tests
Specific blood tests may be ordered to investigate potential causes. These can include tests for viral hepatitis markers, autoimmune antibodies, iron levels (for hemochromatosis), copper levels (for Wilson’s disease), and specific genetic tests.
Imaging Studies
Imaging techniques are crucial for visualizing the liver and detecting any structural abnormalities.
Ultrasound
An abdominal ultrasound is a non-invasive test that uses sound waves to create images of the liver. It can help identify fatty infiltration, cysts, tumors, and changes in liver size and texture. It’s also effective in assessing the bile ducts for blockages.
CT Scan and MRI
Computed tomography (CT) scans and magnetic resonance imaging (MRI) provide more detailed cross-sectional views of the liver. These can offer higher resolution in detecting small lesions, assessing the extent of fibrosis or cirrhosis, and evaluating blood flow within the liver.
FibroScan
FibroScan is a specialized ultrasound-based device that measures liver stiffness, providing an estimate of fibrosis (scarring) and steatosis (fat content). It’s a non-invasive alternative to liver biopsy for assessing the severity of liver disease.
Liver Biopsy
In some cases, a liver biopsy may be necessary for a definitive diagnosis. This involves taking a small sample of liver tissue with a needle for examination under a microscope. A biopsy can help determine the type and extent of liver damage, identify specific causes of inflammation or scarring, and guide treatment decisions.
Treatment and Management Strategies
The management of elevated liver enzymes is highly dependent on the underlying cause. Treatment aims to address the root problem, prevent further liver damage, and improve liver function.
Addressing the Underlying Cause
The primary goal of treatment is to tackle the specific condition causing the enzyme elevation.
Lifestyle Modifications
For conditions like fatty liver disease and alcoholic liver disease, significant lifestyle changes are paramount. This includes adopting a healthy diet low in saturated fats and sugar, regular exercise, and achieving and maintaining a healthy weight. For alcoholic liver disease, complete abstinence from alcohol is essential.
Medications
Depending on the diagnosis, specific medications may be prescribed. Antiviral medications are used to treat chronic viral hepatitis. Immunosuppressive drugs may be used for autoimmune hepatitis. Medications to manage underlying conditions like diabetes, high cholesterol, and iron overload are also crucial.
Dietary Changes
Specific dietary recommendations can support liver health. This may involve increasing intake of fruits, vegetables, and whole grains, while limiting processed foods, red meat, and excessive sugar. For individuals with certain genetic disorders, dietary restrictions might be necessary to manage the accumulation of specific substances.
Monitoring and Follow-Up
Regular monitoring is essential to track the effectiveness of treatment and detect any progression of liver disease.
Regular Blood Tests
Follow-up blood tests to monitor liver enzyme levels are crucial. A gradual decrease in enzyme levels often indicates that the treatment is working and the liver is healing. However, persistent elevations may require adjustments to the treatment plan.
Ongoing Medical Care
Patients with chronic liver conditions require ongoing care from their healthcare provider. This may involve regular check-ups, further diagnostic tests, and specialist consultations with hepatologists (liver specialists) or gastroenterologists. Early and consistent medical attention can significantly impact the long-term prognosis of liver disease.
In conclusion, high enzymes in the liver are not a disease in themselves but rather indicators of potential liver distress. A comprehensive approach involving thorough diagnosis and targeted treatment is essential to understand and manage the underlying causes, thereby protecting liver health and overall well-being.
