For many women experiencing chronic pelvic pain, painful periods, or fertility struggles, the search for answers often starts with medical imaging. One of the most common questions asked is: “Can an ultrasound actually see my endometriosis?”
The answer is complex. While a standard ultrasound cannot always detect every “speck” of endometriosis, specialized ultrasound techniques have become powerful tools in the diagnostic process.
Can Ultrasound Detect Endometriosis?
In the past, many doctors believed endometriosis could only be diagnosed through surgery (laparoscopy). However, technology has evolved. While superficial endometriosis (small spots on the lining of the pelvis) is still often invisible on an ultrasound, Deep Infiltrative Endometriosis (DIE) and Endometriomas (cysts) can often be identified by a trained specialist.
Here is what a sonographer or radiologist is looking for when they screen for endometriosis:
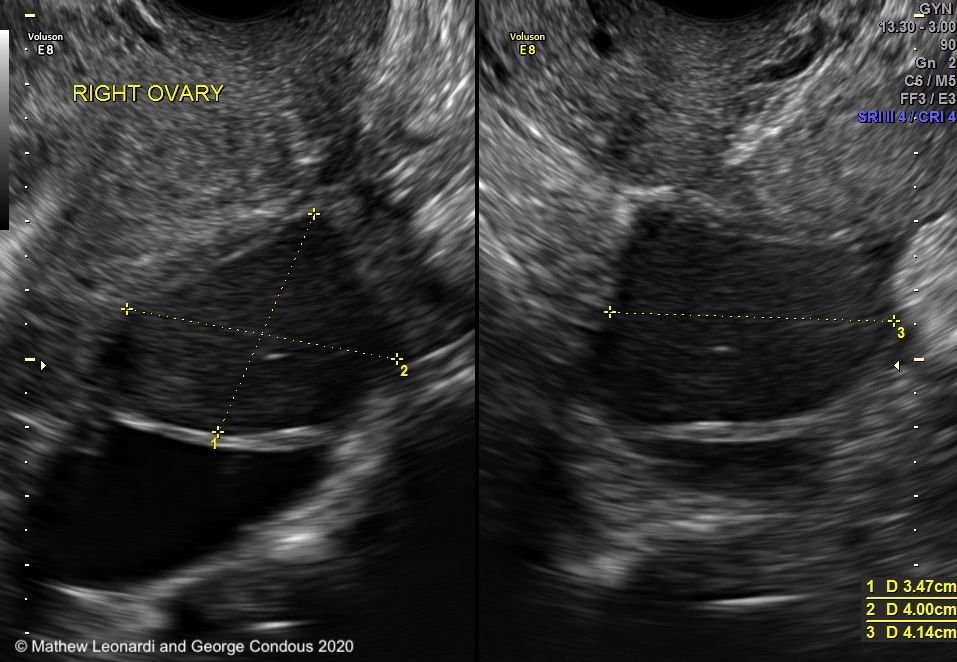
1. Endometriomas (“Chocolate Cysts”)
This is the most common sign of endometriosis seen on an ultrasound. When endometriosis grows on the ovaries, it can form cysts filled with old, dark blood.
- What it looks like: On the screen, these appear as “ground-glass” masses. Unlike simple fluid-filled cysts which look completely black, endometriomas have a fuzzy, uniform grey appearance because of the thick fluid inside.
2. The “Sliding Sign”
A unique part of an endometriosis-specific ultrasound involves the doctor or technician using the ultrasound probe to see how your organs move.
- What it looks like: In a healthy pelvis, the uterus, ovaries, and bowel should “slide” freely against each other. If the organs stay stuck together when the probe is moved, it suggests adhesions (scar tissue) caused by endometriosis.
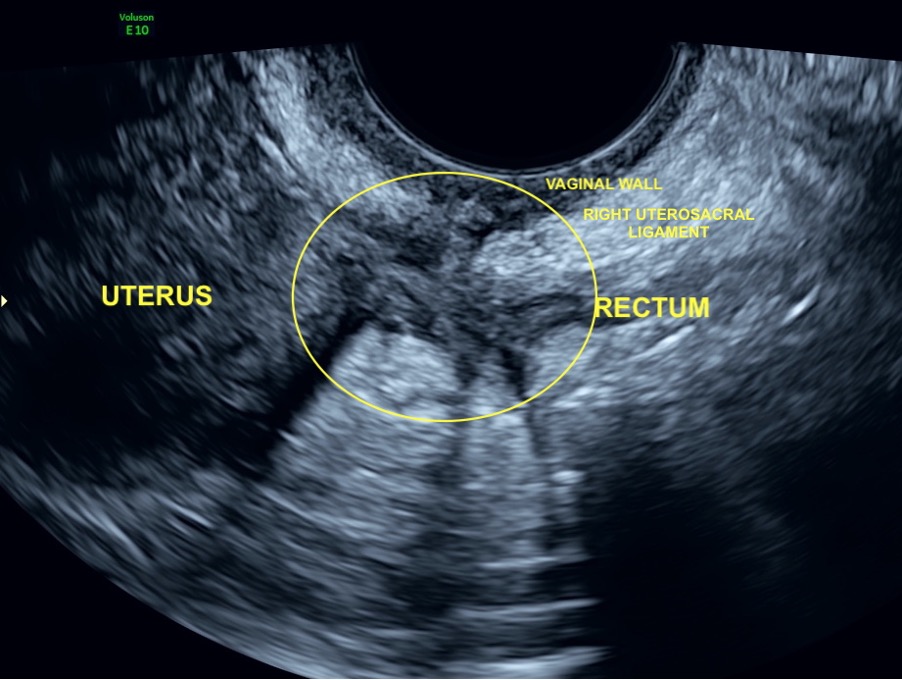
3. Deep Infiltrative Endometriosis (DIE) Nodules
This occurs when the disease grows deeper (usually more than 5mm) into the tissues surrounding the uterus.
- What it looks like: These often appear as dark, irregular-shaped shadows or “nodules” on the ligaments behind the uterus, the wall of the bladder, or the bowel wall. They may look like a thickening of the tissue where it shouldn’t be.
4. “Kissing Ovaries”
When endometriosis is severe, it can cause enough inflammation and scarring that the ovaries are pulled toward each other behind the uterus.
- What it looks like: On the ultrasound, the ovaries will appear to be touching or “kissing.” This is usually a strong indicator of deep pelvic endometriosis.

5. Displacement of Organs
Endometriosis often pulls organs out of their natural position. A radiologist might notice that the uterus is tilted unusually or that an ovary is “fixed” to the pelvic wall or the back of the uterus.
The Type of Ultrasound Matters
Not all ultrasounds are created equal when it comes to endometriosis:
- Transabdominal Ultrasound: (The one where they rub gel on your stomach). This is generally not helpful for diagnosing endometriosis, as it cannot see the pelvic structures in enough detail.
- Transvaginal Ultrasound (TVUS): This is the gold standard for imaging. The probe is closer to the pelvic organs, providing a much clearer picture.
- Specialized “Endometriosis Protocol” Ultrasound: This is an advanced TVUS performed by a specialist (usually a high-level sonologist or gynecologist) who specifically looks for bowel nodules and organ mobility.
What If My Ultrasound Is “Normal”?
It is vital to remember that a normal ultrasound does not mean you do not have endometriosis.
Small, superficial lesions (peritoneal endometriosis) are almost always invisible on an ultrasound. If you have severe symptoms but a “clear” scan, your doctor may still recommend an MRI or a diagnostic laparoscopy to get a definitive answer.
Summary
Ultrasound is a fantastic, non-invasive first step. It is excellent at finding cysts, deep nodules, and adhesions. However, it requires a skilled eye and specialized equipment. If you suspect you have endometriosis, ensure you are seeing a specialist who understands how to interpret these subtle “shadows” on the screen.
Tips for your appointment:
- Ask for an expert: Ask if the person performing the scan is experienced in mapping endometriosis.
- Be specific about pain: Tell the sonographer where your pain is most intense so they can focus on those areas.
- Prepare for a TVUS: Be prepared for an internal (transvaginal) scan, as this provides the necessary detail.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a healthcare professional for diagnosis and treatment.
