The phrase “what does a breast tumor look like” immediately brings to mind medical imaging. While the literal visual appearance of a tumor can vary significantly, the underlying question is about how we detect, visualize, and characterize these anomalies. This is where advanced camera and imaging technology plays a crucial role, providing doctors with the tools to see beyond the surface and understand the intricacies of breast tissue. This article will delve into the various imaging modalities used in breast health, exploring their principles, how they “look” at potential tumors, and the technological advancements that continue to refine our ability to diagnose and treat.
The Foundation of Detection: Mammography and Ultrasound
Mammography, the cornerstone of breast cancer screening, and ultrasound, a vital complementary tool, represent the foundational technologies for visualizing breast tissue and potential abnormalities. Both rely on different principles to create images, offering distinct perspectives on what a breast tumor might look like.
Mammography: A Detailed View Through X-rays
Mammography utilizes low-dose X-rays to create detailed images of the breast. The process involves compressing the breast between two plates, which spreads the tissue and reduces the amount of radiation needed, while also providing a clearer image by minimizing overlap of structures.
How Mammography Visualizes Tumors
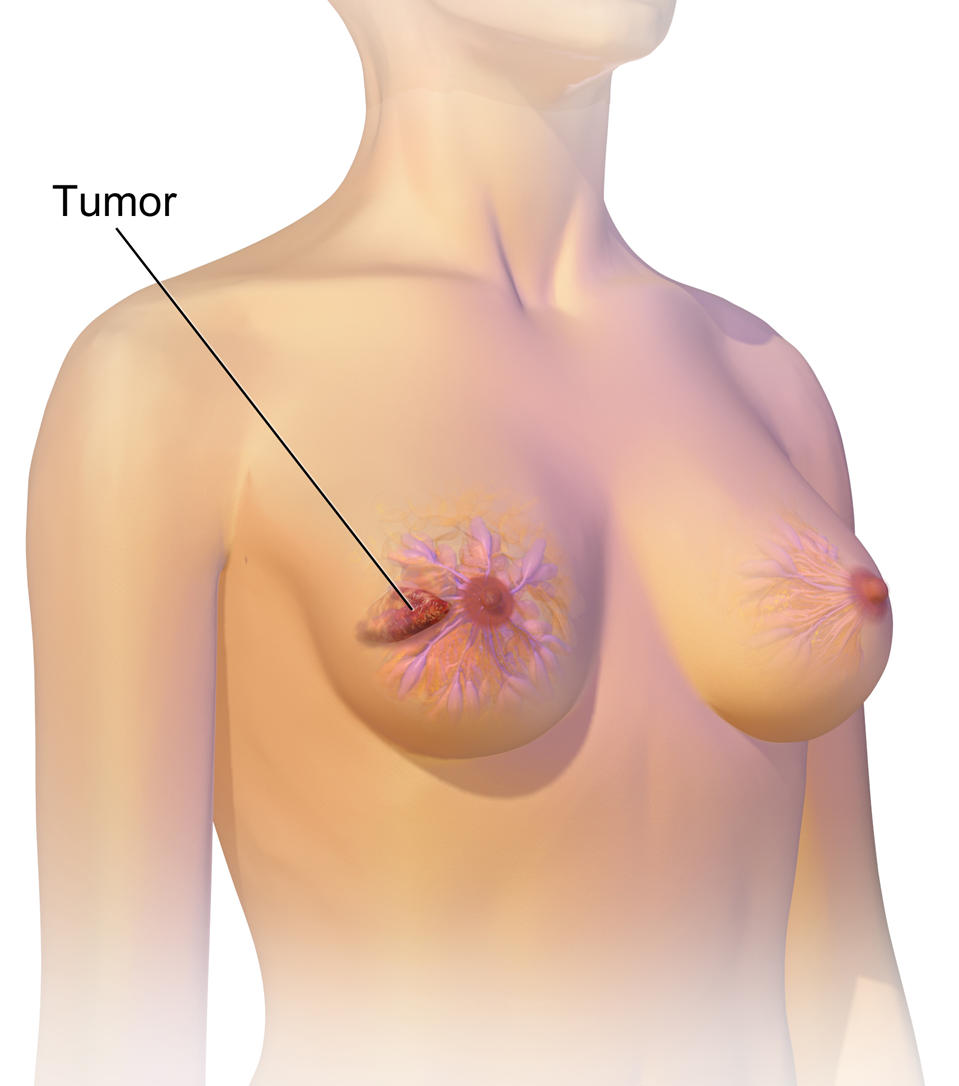
In a mammogram, a tumor typically appears as an area of abnormal density that stands out against the surrounding breast tissue. This can manifest in several ways:
- Masses: These are the most common findings. They can be round, oval, or irregular in shape. The margins of a mass are particularly important for radiologists. Well-defined, smooth margins might suggest a benign (non-cancerous) growth, while irregular, spiculated (star-shaped), or ill-defined margins are more suspicious for malignancy. The internal texture of the mass can also provide clues; a dense, solid appearance is often noted for tumors.
- Calcifications: Tiny calcium deposits can appear as bright white spots on a mammogram. While many calcifications are benign and related to aging or benign conditions like fibrocystic changes, microcalcifications clustered in a specific pattern, especially if they are pleomorphic (varying in shape and size) or linear, can be an early indicator of malignancy, often ductal carcinoma in situ (DCIS).
- Architectural Distortion: Sometimes, a tumor doesn’t form a distinct mass but causes a disruption in the normal pattern of breast tissue. This can appear as a focal distortion or a pulling in of tissue, which might be missed if not carefully examined.
The effectiveness of mammography lies in its ability to detect subtle changes. Radiologists are trained to identify these specific visual cues, comparing current mammograms to previous ones to spot any new or evolving abnormalities. The quality of the mammogram, influenced by the imaging equipment and the radiologist’s expertise, is paramount in accurately visualizing these subtle signs.
Ultrasound: Sound Waves for Soft Tissue Clarity
Breast ultrasound uses high-frequency sound waves to create images of the breast. It is particularly useful for imaging dense breast tissue, where mammograms can be less effective, and for differentiating between solid masses and fluid-filled cysts.
How Ultrasound Illuminates Tumors
Ultrasound provides a different visual representation of breast tumors compared to mammography:
- Echogenicity: Ultrasound images display tissue based on how sound waves are reflected back. Tumors are often described by their echogenicity relative to the surrounding fat and glandular tissue.
- Hypoechoic: Most malignant tumors appear hypoechoic, meaning they reflect fewer sound waves and thus appear darker on the screen than the surrounding tissue.
- Isoechoic: Some tumors appear similar in echogenicity to the surrounding tissue, making them harder to detect.
- Hyperechoic: Benign tumors, such as some fibroadenomas, can sometimes be hyperechoic, appearing brighter.
- Shape and Margins: Similar to mammography, the shape and margins of a lesion seen on ultrasound are critical. Irregular shapes and indistinct or spiculated margins are concerning for malignancy. Smooth, oval, or lobulated shapes with well-defined margins are more characteristic of benign lesions.
- Orientation: A key feature noted in ultrasound is the orientation of a mass. A mass that is taller than it is wide (anti-parallel to the skin line) is more suspicious than one that is wider than it is tall (parallel to the skin line).
- Posterior Acoustic Features: Ultrasound can also show what happens to the sound waves behind the mass. Acoustic enhancement (a brighter area behind the mass) can be seen with cystic lesions, while acoustic shadowing (a dark area behind the mass) can occur with both benign and malignant solid masses, though it is often associated with more aggressive tumors.
Ultrasound is invaluable for characterizing a suspicious finding identified on a mammogram. It can definitively determine if a lump is a fluid-filled cyst (which is almost always benign) or a solid mass that requires further investigation.
Beyond the Basics: Advanced Imaging Techniques
While mammography and ultrasound are the workhorses of breast imaging, advancements in imaging technology have introduced more sophisticated methods that offer even greater detail and insight into breast tissue and potential tumors. These techniques are often used when initial imaging is inconclusive or for specific clinical scenarios.
MRI: A Deeper Dive into Tissue Characteristics
Magnetic Resonance Imaging (MRI) is a powerful diagnostic tool that uses magnetic fields and radio waves to create highly detailed, cross-sectional images of the breast. It does not use ionizing radiation, making it a valuable option for certain patient groups and diagnostic questions.
How MRI Visualizes and Characterizes Tumors
Breast MRI excels at providing functional and detailed anatomical information, revealing what a tumor looks like in terms of its enhancement patterns and diffusion characteristics:
- Contrast Enhancement: The most common type of breast MRI involves the injection of a contrast agent, typically gadolinium-based. Cancerous tumors often have a different blood supply and vascular permeability than normal tissue. After the contrast injection, malignant tumors tend to enhance rapidly and intensely, and then often show a “washout” pattern, where the contrast is quickly cleared from the lesion. Benign lesions typically enhance more slowly and uniformly and do not show this rapid washout.
- Morphology: Like other imaging modalities, the shape and margin characteristics of lesions on MRI are assessed. Irregular shapes and spiculated or irregular margins are suspicious for malignancy.
- Diffusion-Weighted Imaging (DWI): This specialized MRI technique measures the random motion of water molecules within tissues. Cancerous cells are often densely packed, restricting the movement of water. DWI can identify these areas of restricted diffusion, which often correspond to malignant tumors, and can help differentiate them from benign lesions.
- Kinetic Curve Analysis: This involves tracking the rate at which contrast enhancement occurs and disappears over time. Different patterns of enhancement and washout (kinetic curves) are associated with specific types of lesions, aiding in their characterization.
Breast MRI is particularly useful for:
- Screening high-risk individuals (e.g., those with a strong family history or genetic predisposition).
- Evaluating the extent of disease in newly diagnosed breast cancer.
- Detecting occult breast cancer (cancer that is visible on imaging but not palpable).
- Assessing the response to neoadjuvant chemotherapy.
PET/CT Scans: Metabolic Activity and Whole-Body Assessment
Positron Emission Tomography (PET) combined with Computed Tomography (CT) offers a unique perspective on tumors by visualizing their metabolic activity. While not typically used for initial detection, it plays a crucial role in staging and monitoring cancer.
How PET/CT Reveals Tumor Characteristics
PET/CT scans use a radioactive tracer, most commonly fluorodeoxyglucose (FDG), which is a sugar analog that is taken up by cells. Cancer cells, with their increased metabolic rate, tend to absorb more FDG than normal cells.
- FDG Uptake: Areas of increased FDG uptake appear as “hot spots” on the PET scan. Malignant tumors typically show higher FDG uptake than benign tissues. This can help identify cancerous lesions and distinguish them from non-cancerous abnormalities.
- Location and Size: The CT component of the PET/CT scan provides detailed anatomical information, pinpointing the exact location and size of the metabolically active areas identified by PET. This fusion of functional and anatomical data is invaluable.
- Metastasis Detection: A key strength of PET/CT is its ability to assess the entire body for the spread of cancer (metastasis). This is crucial for determining the stage of the disease and guiding treatment decisions.
While PET/CT can show what “looks like” a metabolically active tumor, it’s important to note that some benign inflammatory conditions can also show increased FDG uptake, requiring careful interpretation by a nuclear medicine physician.
The Future of Imaging: Enhancing Detection and Precision
The field of medical imaging is continuously evolving, driven by technological innovations that aim to improve diagnostic accuracy, patient comfort, and treatment outcomes. The quest to better understand “what a breast tumor looks like” is at the forefront of these advancements.
Artificial Intelligence and Machine Learning in Imaging
Artificial intelligence (AI) and machine learning (ML) are rapidly transforming medical imaging. Algorithms are being trained on vast datasets of mammograms, ultrasounds, and MRIs to assist radiologists in detecting subtle abnormalities that might be missed by the human eye.
AI’s Role in Visualizing Tumors
AI is being developed to:
- Improve Detection Rates: AI can flag suspicious areas on imaging studies, acting as a “second reader” to reduce the chance of missing a diagnosis. This is particularly useful for detecting microcalcifications or subtle architectural distortions.
- Enhance Image Quality: AI algorithms can be used to reduce image noise, improve resolution, and reconstruct images from limited data, leading to clearer visualizations.
- Automate Measurement and Characterization: AI can automate the measurement of lesion size and other quantitative features, providing consistent and objective data for comparison over time. It can also help predict the likelihood of malignancy based on imaging features.
- Personalize Screening: AI has the potential to analyze individual risk factors and imaging characteristics to personalize screening intervals and modalities for each patient.
The visual output of AI-assisted imaging isn’t a fundamentally different “look” of a tumor, but rather a refined and more confident interpretation of existing visual data. AI highlights areas of concern with greater precision, helping the radiologist to focus on the most critical aspects of the image.
Innovations in Contrast Agents and Molecular Imaging
Research is ongoing to develop new contrast agents and molecular imaging techniques that can provide even more specific information about the biological characteristics of tumors.

Targeted Visualization of Tumor Biology
- Targeted Contrast Agents: Future contrast agents might be designed to specifically bind to certain molecular markers expressed by cancer cells. This would allow for highly targeted imaging, revealing the specific biological makeup of a tumor in unprecedented detail.
- Theranostics: This emerging field combines diagnostics and therapeutics. Imaging agents could be developed that not only visualize a tumor but also deliver a therapeutic dose of radiation or a drug, offering a dual-purpose approach.
These advanced imaging techniques represent a paradigm shift, moving beyond simply seeing the shape and density of a tumor to understanding its molecular landscape. The “look” of a tumor will increasingly encompass its biological activity and specific cellular characteristics, leading to more precise diagnoses and personalized treatment strategies. The continuous innovation in cameras and imaging systems ensures that our ability to visualize and understand breast tumors will only continue to improve, offering hope for earlier detection and more effective interventions.
