The human circulatory system is a marvel of biological engineering, a complex network of vessels and a tireless pump, the heart, responsible for distributing oxygen and nutrients throughout the body while simultaneously removing waste products. A critical, yet often overlooked, aspect of this system is the transportation of deoxygenated blood, the depleted fuel of our cellular engines, back to the lungs for replenishment. This vital journey is undertaken by a specific set of blood vessels, collectively known as the venous system, playing a crucial role in maintaining life itself.
The Pulmonary Artery: A Misnomer of Arterial Duty
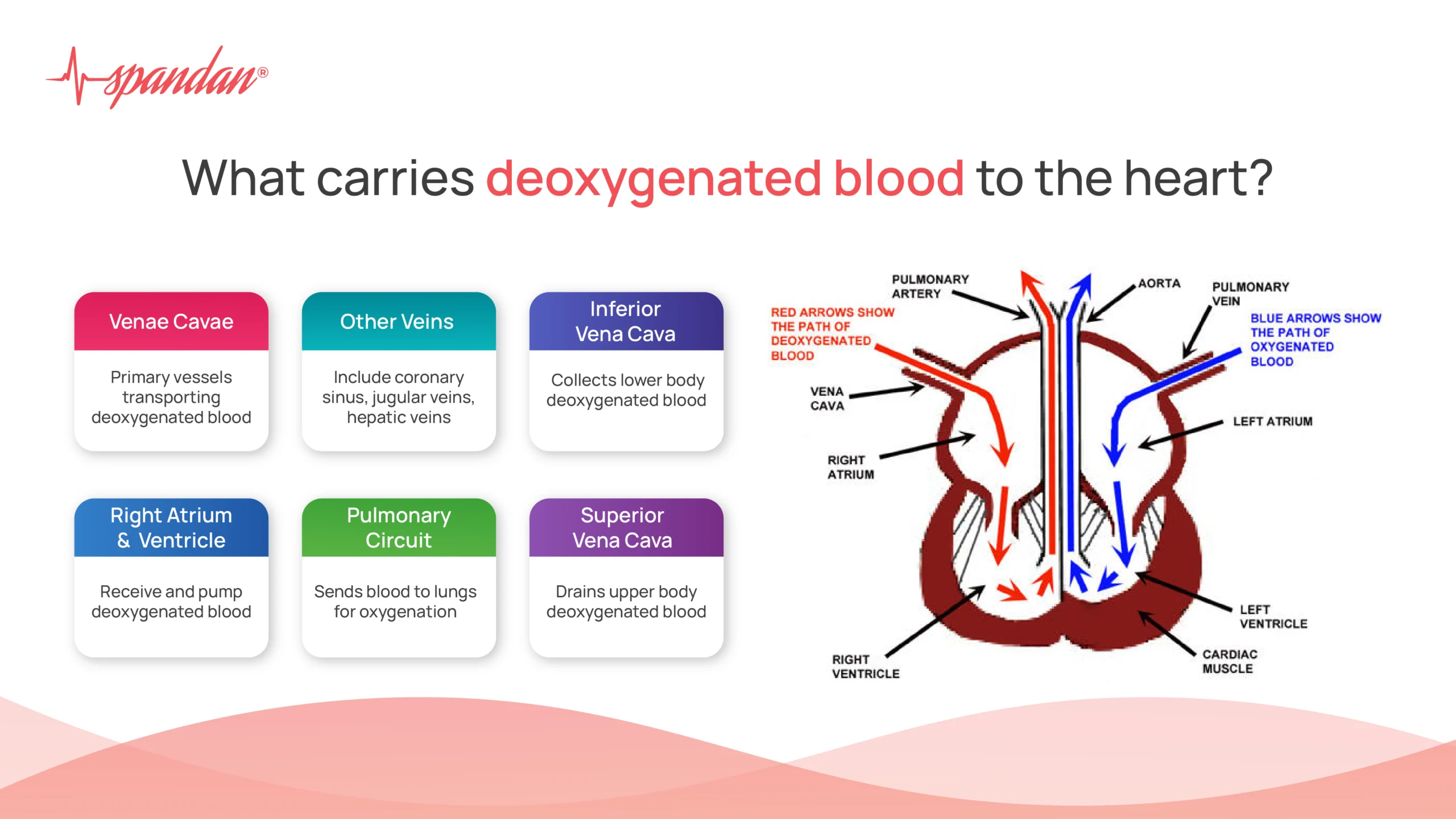
When discussing the vasculature, the term “artery” is typically associated with carrying oxygenated blood away from the heart. However, the pulmonary artery stands as a significant exception to this rule, a testament to the intricate and sometimes counter-intuitive design of the circulatory system. Its primary function is to transport deoxygenated blood from the right ventricle of the heart to the lungs. This deoxygenated blood, having delivered its oxygen payload to the body’s tissues, is rich in carbon dioxide, a waste product of cellular respiration.
Structure and Pathway
The pulmonary artery originates from the superior aspect of the right ventricle. It is a short, wide vessel that quickly bifurcates into the left and right pulmonary arteries, each destined for its respective lung. These primary branches then subdivide into smaller and smaller vessels within the lungs, eventually forming a dense capillary network that surrounds the alveoli – the tiny air sacs where gas exchange takes place. This extensive branching ensures that all the blood passing through the lungs comes into close proximity with the inhaled air, facilitating the efficient uptake of oxygen and the release of carbon dioxide.
The Unique Role of Pulmonary Arteries
Unlike systemic arteries, which carry blood under high pressure due to the powerful contractions of the left ventricle, the pulmonary arteries operate at a much lower pressure. This is because the lungs are located close to the heart, and the resistance to blood flow within the pulmonary vasculature is relatively low. This lower pressure system is crucial for preventing damage to the delicate capillaries within the lungs, which are essential for gas exchange. Furthermore, the thinner walls of the pulmonary arteries reflect this lower pressure environment compared to their systemic counterparts.
The Pulmonary Veins: The Return Journey of Oxygenated Blood
Once the blood has been re-oxygenated in the lungs and has released its carbon dioxide burden, it embarks on its return journey to the heart. This crucial task is performed by the pulmonary veins. Contrary to the naming convention of arteries carrying blood away from the heart and veins carrying blood towards it, the pulmonary veins are distinct in that they carry oxygenated blood from the lungs back to the left atrium of the heart. This is another critical exception that highlights the functional definition of arteries and veins in circulation.
Structure and Pathway
Typically, there are four pulmonary veins, two draining from each lung. These veins collect oxygenated blood from the capillary networks surrounding the alveoli and converge to form larger venous channels. These channels then ascend towards the heart, entering the posterior aspect of the left atrium. The pulmonary veins are relatively thin-walled compared to systemic veins, but their structure is robust enough to handle the flow of oxygenated blood back to the heart at a moderate pressure.
The Significance of Pulmonary Vein Function
The pulmonary veins are vital conduits, ensuring that the freshly oxygenated blood reaches the left side of the heart, ready to be pumped to the rest of the body. The efficiency of this return flow directly impacts the oxygen-carrying capacity of the blood circulating throughout the systemic circulation. Any compromise in the function of the pulmonary veins can lead to a backlog of blood in the lungs, potentially causing pulmonary congestion and impairing overall oxygen delivery to the body’s tissues.
The Microvasculature of the Lungs: The Site of Exchange
While the pulmonary arteries and veins are the major highways for blood transport to and from the lungs, the true magic of gas exchange occurs within the intricate network of capillaries that permeate the lung tissue. This microvasculature represents the interface between the circulatory system and the respiratory system.
Capillary Structure and Function
Pulmonary capillaries are exceptionally thin-walled, often consisting of a single layer of endothelial cells. This thinness, combined with their vast surface area, optimizes the diffusion of gases between the blood and the alveolar air. Oxygen molecules, present in higher concentration in the inhaled air within the alveoli, readily diffuse across the capillary walls into the bloodstream, binding to hemoglobin within red blood cells. Simultaneously, carbon dioxide, a waste product transported from the body’s tissues, diffuses from the blood into the alveoli to be exhaled.
The Alveolar-Capillary Membrane
The barrier separating the alveolar air from the blood in the capillaries is known as the alveolar-capillary membrane. This thin, efficient barrier is crucial for effective gas exchange. Its structure is highly specialized, consisting of the alveolar epithelium, the capillary endothelium, and their fused basement membranes. The narrow space between these layers is minimal, allowing for rapid diffusion of respiratory gases. The integrity and functionality of this membrane are paramount for maintaining adequate oxygen levels in the blood and for eliminating carbon dioxide.
The Role of the Heart: The Driving Force
While the pulmonary artery and veins are the vessels responsible for carrying deoxygenated and oxygenated blood to and from the lungs, respectively, it is the heart that provides the essential force to drive this circulation. The right side of the heart is specifically designed to pump deoxygenated blood to the lungs, a process known as pulmonary circulation.
The Right Ventricle and Pulmonary Artery
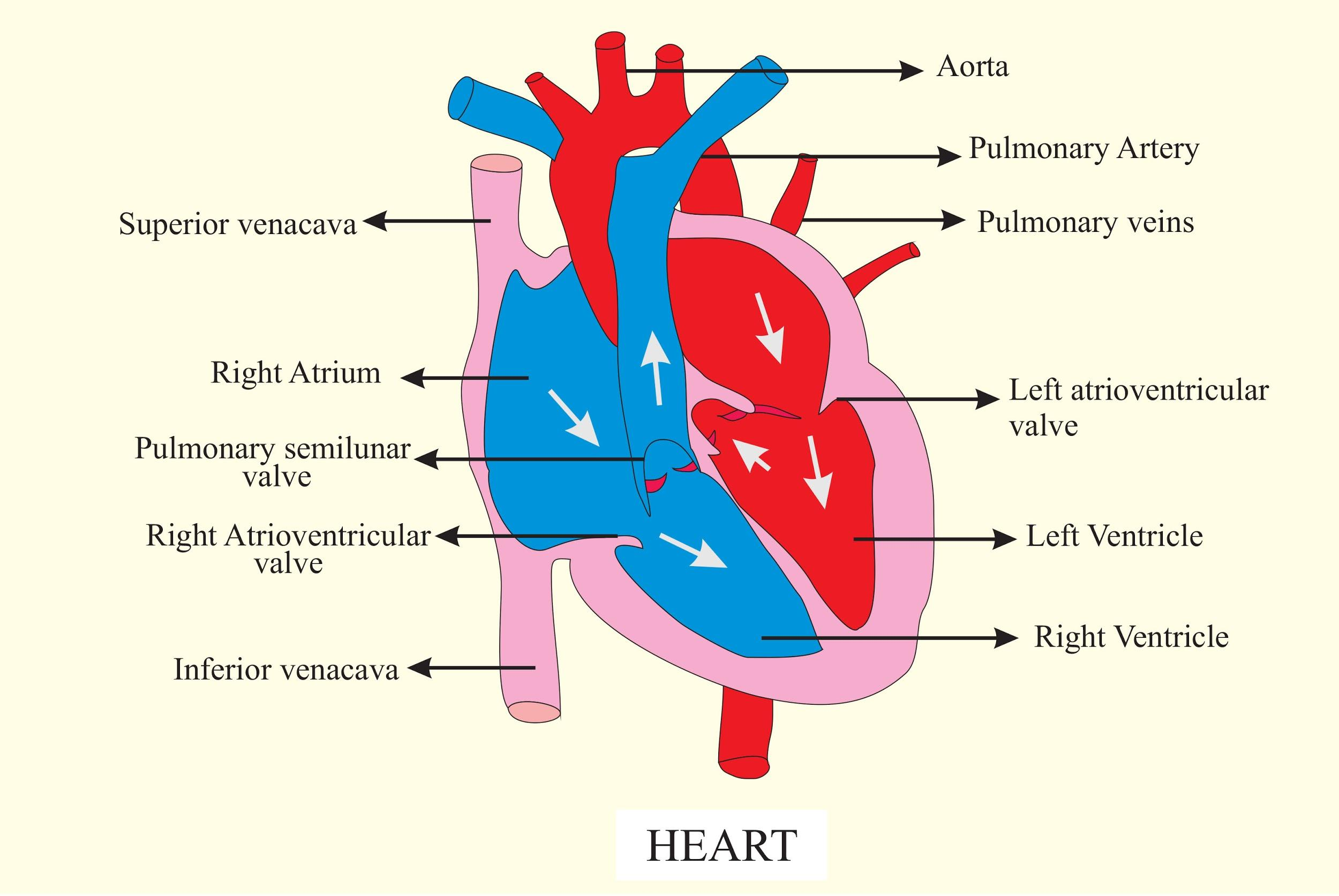
The right ventricle receives deoxygenated blood from the right atrium, which in turn receives it from the body via the superior and inferior vena cava. Upon contraction, the right ventricle forcefully pumps this deoxygenated blood into the pulmonary artery, initiating its journey to the lungs. The rhythmic contractions of the right ventricle ensure a continuous flow of blood through the pulmonary circuit, allowing for constant gas exchange.
The Left Atrium and Pulmonary Veins
Once the blood has been oxygenated in the lungs and returned via the pulmonary veins to the left atrium, the left side of the heart takes over. The left atrium receives this oxygenated blood and, upon contraction, passes it into the left ventricle. The powerful contractions of the left ventricle then propel this oxygenated blood into the aorta, the main artery of the systemic circulation, distributing it to the rest of the body. This coordinated pumping action of both sides of the heart, the pulmonary and systemic circulations, ensures that all tissues receive the oxygen they need to function.
The Continuum of Circulation: A Vital Loop
The circulation of deoxygenated blood to the lungs via the pulmonary artery and the subsequent return of oxygenated blood via the pulmonary veins forms a critical loop within the larger circulatory system. This pulmonary circuit is intrinsically linked to the systemic circulation, which distributes oxygenated blood to the body and returns deoxygenated blood to the heart. Without the efficient transport of deoxygenated blood to the lungs for oxygenation, the systemic circulation would eventually fail, as the body’s tissues would be starved of oxygen. Understanding the specific vessels involved in this vital pulmonary exchange – the pulmonary artery and pulmonary veins – is fundamental to grasping the overall elegance and efficiency of the human circulatory system. This intricate interplay of vessels and the heart ensures that life-sustaining oxygen is continuously delivered and carbon dioxide is effectively removed, a perpetual dance of exchange that sustains us.

