Bacterial meningitis is a serious and potentially life-threatening infection that affects the membranes surrounding the brain and spinal cord. While the term “bacterial meningitis” broadly describes the condition, understanding the specific culprits is crucial for diagnosis, treatment, and prevention. This article delves into the primary bacterial species responsible for this formidable illness, exploring their characteristics, modes of transmission, and the impact they have on public health.
The Primary Pathogens: A Trio of Treacherous Microbes
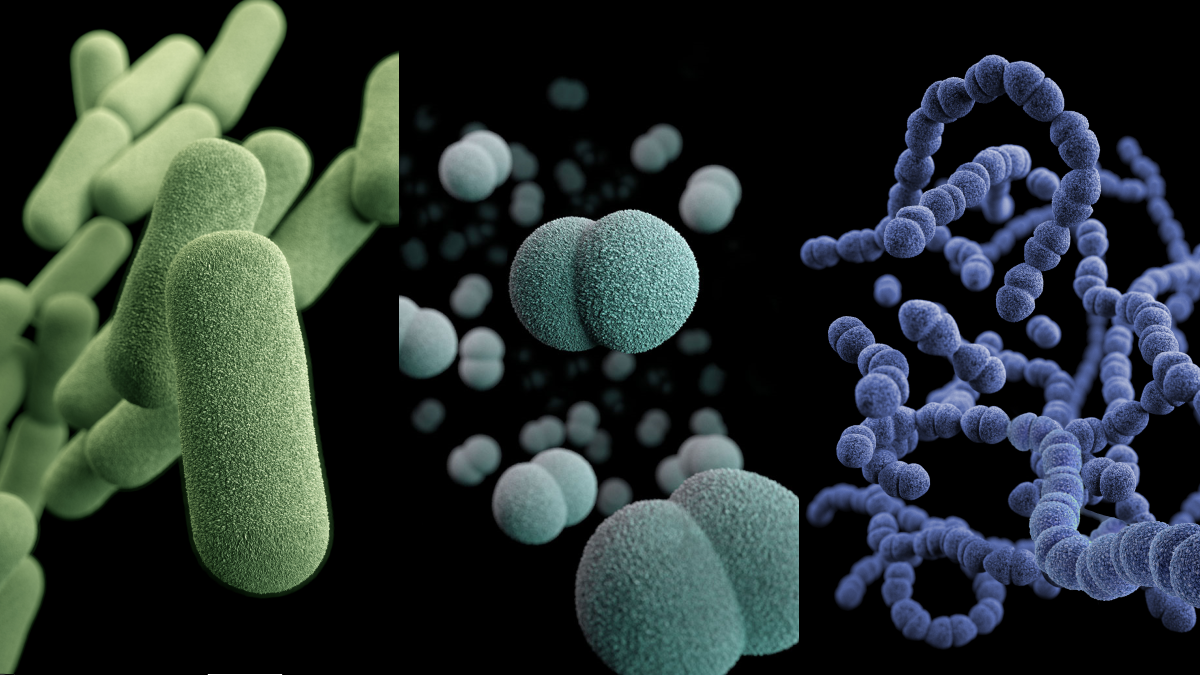
While numerous bacteria can, in rare cases, lead to meningitis, three main types are most commonly implicated and are responsible for the vast majority of cases worldwide. These bacteria possess distinct characteristics that allow them to overcome the body’s defenses and reach the meninges.

Streptococcus pneumoniae: The Pneumococcal Menace
Streptococcus pneumoniae, often referred to as pneumococcus, is a leading cause of bacterial meningitis in adults and children worldwide. This Gram-positive bacterium is a common inhabitant of the human respiratory tract, typically residing in the nose and throat without causing harm. However, under certain conditions, it can invade the bloodstream and travel to the meninges.
Virulence Factors and Mechanisms of Invasion
Streptococcus pneumoniae‘s ability to cause meningitis is attributed to several virulence factors. Its polysaccharide capsule is a key component, providing protection from phagocytosis by immune cells. Different serotypes of S. pneumoniae are distinguished by variations in their capsular polysaccharides, and some serotypes are more commonly associated with invasive diseases like meningitis. Furthermore, pneumococcus produces enzymes such as pneumolysin, which can damage host cells and facilitate the spread of infection. Adhesins on the bacterial surface allow it to bind to and colonize host tissues.
Transmission and Risk Factors
Pneumococcal meningitis is typically spread through respiratory droplets, via coughing or sneezing, from infected individuals. Close contact and crowded living conditions can increase the risk of transmission. While anyone can develop pneumococcal meningitis, certain groups are at higher risk. These include very young children (especially those under two years old), older adults (over 65), individuals with weakened immune systems (due to conditions like HIV/AIDS, cancer, or organ transplantation), those with chronic illnesses (such as diabetes, lung disease, or kidney disease), and people who have had a recent head injury or surgery.
Clinical Manifestations and Diagnosis
The symptoms of pneumococcal meningitis often develop rapidly and can include sudden onset of fever, severe headache, stiff neck, nausea, vomiting, photophobia (sensitivity to light), and altered mental status (confusion or lethargy). In infants, symptoms might be less specific and include irritability, poor feeding, and a bulging fontanelle. Diagnosis typically involves a lumbar puncture (spinal tap) to obtain cerebrospinal fluid (CSF) for analysis. Gram staining and culture of the CSF can identify S. pneumoniae, and rapid antigen tests can also aid in diagnosis. Blood tests may also reveal signs of infection.
Neisseria meningitidis: The Meningococcal Meningitis Agent
Neisseria meningitidis, commonly known as meningococcus, is another significant cause of bacterial meningitis, particularly in adolescents and young adults. This Gram-negative diplococcus bacterium can also be found in the nasopharynx of healthy individuals, acting as a colonizer. However, when it invades the bloodstream, it can lead to meningococcal disease, which encompasses meningitis and meningococcemia (sepsis).
Diverse Serogroups and Epidemic Potential
Neisseria meningitidis is classified into different serogroups based on its capsular polysaccharides. Serogroups A, B, C, W, and Y are the most common causes of meningococcal disease. Historically, serogroup A has been responsible for large-scale epidemics, particularly in the “meningitis belt” of sub-Saharan Africa. Serogroup B has been a prevalent cause in many developed countries, while serogroups C, W, and Y can also cause sporadic cases and outbreaks. The ability of N. meningitidis to cause epidemics is linked to its efficient person-to-person transmission and the potential for widespread asymptomatic carriage.
Transmission Routes and Outbreak Dynamics
Meningococcal meningitis is spread through direct contact with respiratory and throat secretions from an infected person, typically through close contact such as kissing or sharing eating utensils. It can also spread through airborne droplets from coughing or sneezing. Crowded environments like college dormitories, military barracks, and boarding schools are conducive to the rapid spread of this bacterium, leading to outbreaks.
Recognizing Meningococcal Meningitis
The symptoms of meningococcal meningitis are similar to those of pneumococcal meningitis, including rapid onset of fever, severe headache, stiff neck, and photophobia. However, meningococcal disease can also manifest as a rapidly progressing rash, known as purpura, which is a hallmark of meningococcemia. This rash can be a sign of severe illness and requires immediate medical attention. Diagnosis involves lumbar puncture and CSF analysis, with Gram staining and culture being essential for identifying N. meningitidis.
Haemophilus influenzae type b (Hib): A Success Story of Vaccination
Haemophilus influenzae type b (Hib) was once a leading cause of bacterial meningitis in infants and young children. This small, Gram-negative coccobacillus is a bacterium that can colonize the upper respiratory tract. Before the widespread implementation of the Hib vaccine, Hib meningitis was a devastating disease, causing significant mortality and long-term neurological sequelae.
The Role of the Capsule in Disease
The “b” in Hib refers to the polysaccharide capsule that surrounds the bacterium. This capsule is crucial for its virulence, protecting it from phagocytosis. Different strains of Haemophilus influenzae are classified into types (a-f) based on their capsular antigens. Type b is the most invasive and virulent.
The Impact of the Hib Vaccine
The development and widespread administration of the conjugate Hib vaccine have dramatically reduced the incidence of Hib meningitis. This vaccine works by attaching the Hib capsule to a carrier protein, which enhances the immune response in infants. As a result, Hib meningitis is now relatively rare in countries with high vaccination rates, representing a significant public health triumph. However, it remains a concern in regions with low vaccine coverage.
Transmission and Persistence
Hib is transmitted through respiratory droplets. While vaccination has drastically reduced its impact, unvaccinated individuals, particularly those in areas with limited access to healthcare, remain at risk. The bacterium can persist in the nasopharynx of carriers, allowing for transmission to susceptible individuals.
Less Common but Still Significant Bacterial Causes
While the aforementioned bacteria are the most common culprits, other bacteria can also cause meningitis, often in specific populations or under particular circumstances.
Listeria monocytogenes: The Foodborne Threat
Listeria monocytogenes is a Gram-positive bacterium that can cause listeriosis, an infection that can manifest as meningitis, particularly in pregnant women, newborns, older adults, and individuals with weakened immune systems. Unlike many other meningitis-causing bacteria, Listeria monocytogenes is found in the environment and can be transmitted through contaminated food.
Food Contamination and Transmission
Listeria is commonly found in soil, water, and the feces of animals. It can contaminate a wide range of foods, including unpasteurized dairy products, raw or undercooked meats, poultry, seafood, and raw fruits and vegetables. Pregnant women are particularly susceptible to listeriosis, and infection can lead to miscarriage, stillbirth, premature delivery, or life-threatening infection in the newborn.
Unique Presentation and Treatment Challenges
Listeria meningitis can present with a broader range of symptoms than other forms of bacterial meningitis, including confusion, behavioral changes, and even neurological deficits like cranial nerve palsies or ataxia. Diagnosis involves CSF analysis, and treatment requires specific antibiotics.
Group B Streptococcus (Streptococcus agalactiae): A Neonatal Concern
Group B Streptococcus (GBS), or Streptococcus agalactiae, is a leading cause of bacterial meningitis and sepsis in newborns. While GBS can colonize the vaginal and rectal tracts of healthy women without causing illness, it can be transmitted to infants during childbirth, leading to early-onset neonatal disease.
Vertical Transmission and Screening
GBS is transmitted from mother to baby during labor and delivery. To prevent neonatal GBS disease, pregnant women are typically screened for GBS colonization in the later stages of pregnancy. If a woman is found to be positive for GBS, she is administered antibiotics intravenously during labor to reduce the risk of transmission to her infant.
Neonatal Meningitis and Long-Term Effects
Neonatal GBS meningitis can lead to severe illness, including respiratory distress, fever, and lethargy. Survivors may experience long-term complications such as hearing loss, developmental delays, and learning disabilities. Prompt diagnosis and treatment are critical for improving outcomes.
The Importance of Identification and Prevention
Understanding the specific bacteria responsible for bacterial meningitis is paramount for effective clinical management and public health strategies. Accurate identification of the causative agent through diagnostic tests guides appropriate antibiotic therapy, as different bacteria respond to different medications. Furthermore, this knowledge underpins the development and implementation of preventative measures, most notably vaccination.
The Power of Vaccines: A Cornerstone of Prevention
Vaccination remains the most effective tool for preventing several forms of bacterial meningitis. Vaccines are available against Streptococcus pneumoniae (pneumococcal vaccines), Neisseria meningitidis (meningococcal vaccines targeting various serogroups), and Haemophilus influenzae type b (Hib vaccine). Widespread vaccination programs have significantly reduced the incidence of these diseases, saving countless lives and preventing long-term disabilities. Continuous efforts to develop and improve vaccines, including those that target emerging strains or offer broader protection, are crucial for ongoing disease control.

Public Health Measures and Early Recognition
Beyond vaccination, public health initiatives play a vital role in controlling the spread of bacterial meningitis. These include promoting good hygiene practices, such as frequent handwashing, to reduce transmission of respiratory pathogens. Education about the signs and symptoms of meningitis is also essential, empowering individuals to seek medical attention promptly. Early recognition and diagnosis are critical for initiating timely treatment, which can significantly improve prognosis and reduce the risk of severe complications. Public health surveillance systems are vital for monitoring disease trends, identifying outbreaks, and informing public health responses.
In conclusion, bacterial meningitis is a complex and formidable infectious disease caused by a variety of bacteria. While Streptococcus pneumoniae, Neisseria meningitidis, and historically Haemophilus influenzae type b have been the most significant threats, understanding less common pathogens like Listeria monocytogenes and Group B Streptococcus is also crucial, especially in vulnerable populations. Through a combination of robust vaccination programs, effective public health strategies, and prompt medical intervention, the burden of bacterial meningitis can be further reduced, protecting individuals and communities from this potentially devastating illness.
