Dark spots on the face, often referred to as hyperpigmentation, are a common dermatological concern affecting individuals of all ages and skin tones. While visually bothersome, understanding their origins and the underlying biological processes is crucial for effective management and prevention. This article delves into the science behind these pigmentary changes, focusing on the cellular mechanisms, triggers, and how advancements in imaging and observational technologies can contribute to their identification and study.
Understanding Melanin and Hyperpigmentation
At the heart of dark spots lies melanin, the pigment responsible for the color of our skin, hair, and eyes. Melanin is produced by specialized cells called melanocytes, located in the epidermis, the outermost layer of our skin. The production and distribution of melanin are complex processes influenced by genetics, hormones, and environmental factors. When these processes are disrupted, leading to an overproduction or uneven distribution of melanin, hyperpigmentation occurs.

Melanocytes: The Pigment Producers
Melanocytes are dendritic cells that reside in the basal layer of the epidermis. Their primary role is to synthesize melanin through a process called melanogenesis. This process involves a series of enzymatic reactions, with tyrosinase being a key enzyme. Once synthesized, melanin is packaged into organelles called melanosomes, which are then transferred to surrounding keratinocytes, the main cells of the epidermis. This transfer of melanosomes distributes the pigment throughout the epidermal layers, providing a natural defense against ultraviolet (UV) radiation. The amount and type of melanin produced (eumelanin, which is brown-black, and pheomelanin, which is red-yellow) contribute to our diverse skin tones.
Types of Hyperpigmentation
Hyperpigmentation can manifest in various forms, each with distinct causes and appearances. Understanding these distinctions is the first step in addressing the issue effectively.
Post-Inflammatory Hyperpigmentation (PIH)
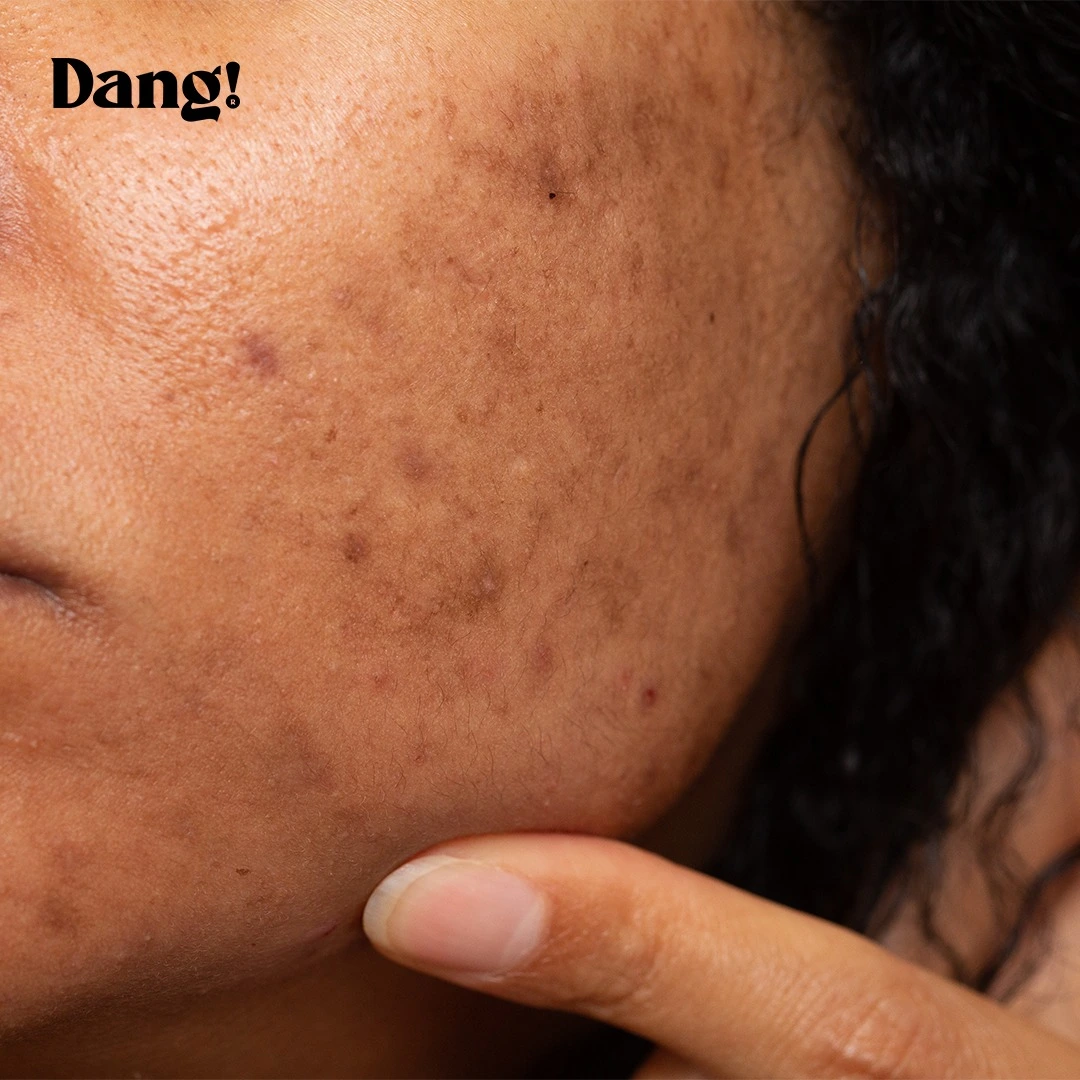
PIH is a common consequence of skin inflammation. When the skin experiences an injury or irritation, such as acne breakouts, eczema, psoriasis, or even minor cuts, the inflammatory process can trigger an increase in melanin production. Melanocytes become stimulated, leading to the deposition of excess melanin in the affected area. The color of PIH can range from light brown to dark brown or black, depending on the individual’s skin tone and the severity of the inflammation. PIH is often temporary, with the dark spots gradually fading over time as the skin naturally renews itself. However, the duration of fading can vary significantly, sometimes taking months or even years.
Solar Lentigines (Sun Spots/Age Spots)
As the name suggests, solar lentigines are primarily caused by prolonged and cumulative exposure to ultraviolet (UV) radiation from the sun. UV rays stimulate melanocytes to produce more melanin as a protective mechanism. Over time, this leads to an overproduction and uneven distribution of pigment, resulting in discrete, flat, brown or black spots. These are most commonly found on sun-exposed areas like the face, shoulders, arms, and hands. While often referred to as “age spots,” their development is more directly linked to sun exposure history than chronological aging itself.
Melasma
Melasma is a chronic condition characterized by the appearance of large, irregular, brownish-gray patches on the face. It is particularly common in women, especially during reproductive years, and is often associated with hormonal fluctuations. Triggers for melasma include pregnancy (leading to the term “mask of pregnancy”), oral contraceptives, hormone replacement therapy, and even certain cosmetic products. Sun exposure is a significant exacerbating factor, often worsening existing melasma. Melasma can occur in different layers of the skin: epidermal (superficial), dermal (deep), or mixed. The location of the pigment influences its appearance and treatment approach.
Freckles (Ephelides)
Freckles are small, scattered spots that are typically lighter in color than solar lentigines and tend to be more prominent after sun exposure. They are genetically determined and are more common in individuals with fair skin and red or blonde hair. Unlike solar lentigines, freckles are not a sign of sun damage but rather an indication of an individual’s genetic predisposition to pigment production. They tend to fade or disappear during winter months when sun exposure is reduced.
Triggers and Contributing Factors
Beyond the intrinsic production of melanin, various external and internal factors can trigger or exacerbate the formation of dark spots. Understanding these triggers is vital for adopting preventative measures and managing existing pigmentation.
The Role of UV Radiation
Ultraviolet radiation from the sun is arguably the most significant environmental factor contributing to hyperpigmentation. UV rays, particularly UVA and UVB, penetrate the skin and stimulate melanocytes to produce melanin. This protective response, while beneficial in the short term, can lead to long-term consequences if exposure is excessive and cumulative. UV radiation can damage DNA in skin cells, leading to mutations and potentially increasing the risk of skin cancer. Furthermore, it can disrupt the normal melanogenesis process, resulting in uneven pigment distribution and the formation of dark spots. This underscores the importance of daily sunscreen use, even on cloudy days.
Inflammation and Skin Injury
As discussed with PIH, any form of skin inflammation or injury can set the stage for hyperpigmentation. This includes:
- Acne: The most common culprit, where the inflammation associated with pimples can lead to PIH. Picking or squeezing acne lesions can worsen inflammation and increase the likelihood and severity of dark spots.
- Eczema and Dermatitis: These inflammatory skin conditions can cause redness, itching, and subsequent PIH once the acute phase subsides.
- Trauma and Wounds: Cuts, burns, insect bites, and other forms of skin trauma can all trigger a melanocytic response, leading to post-injury hyperpigmentation.
- Harsh Skincare Products: Certain aggressive exfoliants, chemical peels, or irritating ingredients can cause micro-inflammation, contributing to PIH.
Hormonal Influences
Hormonal changes play a significant role, particularly in the development of melasma. Fluctuations in estrogen and progesterone levels can stimulate melanocytes. This is why melasma is so prevalent in pregnant women, those taking oral contraceptives, or undergoing hormone replacement therapy. The precise mechanisms by which hormones influence melanogenesis are complex and still under investigation, but it is understood that they can increase the sensitivity of melanocytes to UV radiation and other stimulants.
Genetic Predisposition
While environmental factors are significant, genetics also plays a role in an individual’s susceptibility to hyperpigmentation. Certain individuals are genetically predisposed to producing more melanin or to developing PIH more readily after inflammation. This is evident in the higher prevalence of freckles in fair-skinned individuals and the varying degrees of hyperpigmentation observed across different ethnic groups.
Technological Approaches to Observation and Analysis
While the core understanding of dark spots lies in dermatology and biology, advancements in technology are providing novel ways to observe, analyze, and even contribute to the study of these skin conditions. Imaging technologies, in particular, are becoming increasingly sophisticated, offering non-invasive methods for deeper insights.
High-Resolution Imaging and Digital Dermoscopy
High-resolution cameras, often integrated into digital dermoscopes, allow for detailed visualization of the skin’s surface and subsurface structures. These devices can capture images with exceptional clarity, enabling dermatologists and researchers to meticulously examine the size, shape, color intensity, and distribution of dark spots. Digital dermoscopy, in particular, utilizes magnification and specialized lighting to visualize epidermal and dermal pigmentary changes that might not be apparent to the naked eye. This level of detail is crucial for accurate diagnosis, differentiating between various types of hyperpigmentation, and monitoring treatment efficacy over time. The ability to capture and store high-quality images also facilitates longitudinal studies, tracking the progression or regression of dark spots under different conditions or treatments.

Multispectral and Hyperspectral Imaging
Beyond standard visible light imaging, multispectral and hyperspectral imaging techniques offer a more profound understanding of skin chromophores, including melanin. These technologies capture images across a wide range of electromagnetic wavelengths, from the ultraviolet to the infrared spectrum. Different wavelengths interact with skin components in unique ways. By analyzing the spectral signatures – how much light is absorbed or reflected at each wavelength – researchers can differentiate between various pigments and their depths within the skin.
For instance, specific wavelengths might be particularly sensitive to melanin absorption, allowing for precise mapping of pigment distribution. Other wavelengths can reveal underlying vascularity or collagen structure, which can sometimes be associated with or influence hyperpigmentation. This advanced imaging can help researchers understand:
- Depth of Pigment: Distinguishing between epidermal and dermal melasma, which have different treatment prognoses.
- Melanin Index: Quantifying the amount of melanin present in specific skin areas, providing objective metrics for assessment.
- Underlying Inflammation: Detecting subtle inflammatory changes that may precede or contribute to hyperpigmentation.
While not typically used in direct consumer applications for “dark spots on my face,” these sophisticated imaging modalities are invaluable tools in clinical research settings, aiding in the development of new diagnostic criteria and treatment strategies. They offer a glimpse into the microscopic and biochemical processes occurring beneath the skin’s surface, a frontier in understanding dermatological conditions.
