The Spectrum of Surgical Intervention: Defining “Major”
The term “major surgery” is commonly understood in everyday language, but within the medical field, its definition is nuanced and encompasses a range of factors beyond mere complexity. A major surgery is typically characterized by significant invasiveness, prolonged duration, substantial physiological impact, and often, a higher risk profile compared to minor procedures. While there isn’t a single, universally codified definition, several key elements contribute to classifying a surgery as major. These include the extent of tissue manipulation, the need for general anesthesia, the potential for significant blood loss, the risk of post-operative complications, and the length of recovery time required.
The classification of a surgery as major is crucial for various aspects of patient care and healthcare management. It influences pre-operative assessments, the intensity of post-operative monitoring, the need for specialized surgical teams, the utilization of intensive care units, and the allocation of hospital resources. Furthermore, understanding what constitutes a major surgery helps patients comprehend the gravity of their medical situation and the associated recovery process.
Invasiveness and Scope
One of the primary determinants of a major surgery is its degree of invasiveness. Procedures that involve opening large body cavities, such as the abdomen or chest, are almost always considered major. This includes surgeries like open-heart surgery, organ transplantation, extensive abdominal resections, and radical cancer surgeries. The manipulation of multiple organs, extensive dissection of tissues, and the creation of significant incisions all contribute to the classification of invasiveness.
Conversely, minor surgeries, such as a skin biopsy, mole removal, or suturing a small laceration, typically involve superficial tissues, require local anesthesia, and have minimal impact on the body’s overall physiology. The distinction is stark: major surgeries fundamentally alter a patient’s internal environment, while minor ones address localized issues with minimal systemic disruption.
Anesthesia and Physiological Impact
The type of anesthesia employed is another significant indicator of a surgery’s magnitude. Major surgeries almost invariably require general anesthesia, a state of controlled unconsciousness that suppresses the central nervous system. This is necessary to manage pain, immobility, and physiological responses to extensive surgical manipulation. The administration and monitoring of general anesthesia itself represent a significant aspect of major surgical care, demanding specialized anesthesiologists and critical care resources.
The physiological impact of major surgery extends beyond the immediate procedure. It can lead to significant changes in blood pressure, heart rate, respiratory function, and fluid balance. The body undergoes considerable stress, and a robust recovery pathway is essential to help it return to homeostasis. This physiological disruption necessitates close monitoring, often in a post-anesthesia care unit (PACU) or an intensive care unit (ICU) immediately following the procedure.
Risk and Recovery
The inherent risks associated with a procedure are a central component of its classification. Major surgeries, by their nature, carry a higher potential for complications. These can include infection, bleeding, blood clots, organ damage, adverse reactions to anesthesia, and post-operative pain that can be difficult to manage. The statistical probability of these complications, even when the surgery is performed by a skilled team, contributes to its “major” status.
Consequently, the recovery period for major surgeries is significantly longer and more demanding than for minor ones. Patients may require hospitalization for days or even weeks, followed by a prolonged period of rehabilitation at home. This rehabilitation can involve physical therapy, occupational therapy, pain management, and ongoing medical follow-up to ensure proper healing and functional recovery. The extent of the recovery dictates the level of support required from healthcare professionals, family, and caregivers.
Categories of Major Surgeries
The vast landscape of surgical interventions can be broadly categorized to better understand the scope and implications of “major” procedures. While specific procedures may overlap or have sub-classifications, these overarching categories highlight the diverse areas where major surgeries are performed.
Cardiovascular Surgeries
Surgeries involving the heart and major blood vessels fall under the umbrella of cardiovascular surgery. These are often complex and high-risk procedures due to the critical nature of the circulatory system.
Coronary Artery Bypass Grafting (CABG)
One of the most common major cardiovascular surgeries, CABG involves creating new pathways for blood to flow to the heart muscle when the coronary arteries become blocked. This typically requires opening the chest, placing the patient on a heart-lung machine, and harvesting blood vessels from other parts of the body to create the grafts. The recovery period is substantial, often involving several weeks of hospitalization and months of rehabilitation.
Heart Valve Repair and Replacement
Diseased or damaged heart valves can significantly impair the heart’s ability to pump blood efficiently. Repairing or replacing these valves is a major procedure that can involve open-chest surgery or, in some cases, less invasive techniques using catheters. The complexity depends on the valve involved, the extent of damage, and whether it’s a repair or replacement with a mechanical or biological prosthesis.
Aortic Aneurysm Repair
Aneurysms, or bulges in the aorta, are life-threatening if they rupture. Surgical repair involves reinforcing or replacing the weakened section of the aorta. This can be performed via open surgery or endovascular repair, with the latter being less invasive but still classified as a major procedure due to the location and risks associated with the aorta.
Cardiac Transplantation
Heart transplantation is the ultimate surgical intervention for end-stage heart failure. It involves removing the diseased heart and replacing it with a donor heart. This is an exceptionally complex and resource-intensive procedure with a high risk of complications, including organ rejection and infection, requiring lifelong immunosuppression and intensive monitoring.
Oncological Surgeries
Cancer surgeries, aimed at removing malignant tumors, often fall into the category of major surgeries, especially when the cancer is advanced or has spread.
Radical Resections
These surgeries involve the complete removal of a cancerous organ or a large section of tissue containing the tumor. Examples include radical mastectomy (removal of the entire breast, lymph nodes, and surrounding tissues for breast cancer), colectomy (removal of part or all of the colon for colorectal cancer), and nephrectomy (removal of a kidney for kidney cancer). The extent of resection is determined by the tumor’s size, location, and invasiveness.
Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy (HIPEC)
For certain advanced abdominal cancers, such as ovarian cancer, cytoreductive surgery aims to remove as much visible tumor as possible. This is often followed by HIPEC, where heated chemotherapy drugs are circulated within the abdominal cavity to kill any remaining microscopic cancer cells. This combined approach is a complex, multi-stage major surgery with significant post-operative recovery demands.
Tumor Debulking
When a tumor cannot be fully removed due to its size, location, or spread, debulking surgery aims to remove the largest possible portion of the tumor. While not curative, it can alleviate symptoms, improve the effectiveness of other cancer treatments like chemotherapy or radiation, and enhance the patient’s quality of life.
General and Abdominal Surgeries

This broad category encompasses a wide array of procedures performed on the abdominal organs, many of which are considered major due to their invasiveness and impact.
Gastric Resection and Bariatric Surgery
Surgeries to remove parts of the stomach, either for cancer (gastric resection) or for weight loss (bariatric surgery like gastric bypass or sleeve gastrectomy), are significant procedures. They involve altering the digestive tract, impacting nutrient absorption and requiring extensive post-operative dietary adjustments and monitoring.
Pancreaticoduodenectomy (Whipple Procedure)
This highly complex surgery is performed to treat cancers of the pancreas, duodenum, or bile ducts. It involves removing the head of the pancreas, the duodenum, the gallbladder, and a portion of the bile duct, and then rejoining the remaining organs to restore digestive function. It is one of the most challenging abdominal surgeries.
Liver Resection and Transplantation
Removing portions of the liver for tumors or other conditions, or performing a full liver transplant, are major surgical feats. The liver’s crucial role in metabolism and detoxification means that such procedures have a profound systemic impact and require extensive post-operative care.
Neurological Surgeries
Surgeries on the brain and spinal cord are inherently major due to the delicate and vital nature of the nervous system.
Craniotomy
Opening the skull (craniotomy) to access the brain for tumor removal, aneurysm clipping, or treating traumatic brain injury is a defining major neurological surgery. The precision required and the potential for devastating neurological deficits underscore its significance.
Spinal Fusion and Decompression
Procedures to fuse vertebrae or decompress the spinal cord for conditions like severe disc herniation, spinal stenosis, or severe scoliosis involve significant manipulation of the spine and can lead to long recovery periods, including extensive physical therapy.
Urological and Gynecological Surgeries
While some urological and gynecological procedures are minor, many are classified as major due to their invasiveness and the organs involved.
Radical Prostatectomy
The surgical removal of the prostate gland for prostate cancer is a major procedure that can impact urinary continence and erectile function. It is often performed via open surgery, laparoscopy, or robotic assistance, but the underlying invasiveness remains.
Hysterectomy with Bilateral Salpingo-oophorectomy
The removal of the uterus, fallopian tubes, and ovaries, often performed for cancer or severe gynecological conditions, is a major surgery with hormonal implications for the patient.
Pre-Operative and Post-Operative Considerations for Major Surgeries
The journey through a major surgery extends far beyond the operating room. Comprehensive pre-operative preparation and meticulous post-operative care are paramount to ensure patient safety, optimize outcomes, and facilitate recovery.
Pre-Operative Assessment and Optimization
Before undergoing a major surgery, patients undergo a thorough assessment to evaluate their overall health and identify any potential risks. This typically includes:
- Medical History and Physical Examination: A detailed review of past medical conditions, current medications, allergies, and a physical exam to assess vital signs, organ function, and general fitness for surgery.
- Diagnostic Tests: Blood tests (including complete blood count, chemistry panels, coagulation studies), urine tests, electrocardiograms (ECGs), chest X-rays, and sometimes more specialized imaging like CT scans or MRIs to get a clear picture of the affected area and overall health.
- Cardiopulmonary Evaluation: For individuals with pre-existing heart or lung conditions, further evaluation by cardiologists or pulmonologists may be necessary to ensure they can tolerate the physiological stress of surgery and anesthesia.
- Nutritional Assessment: Adequate nutrition is vital for healing. Patients may receive guidance on diet or supplements to optimize their nutritional status before surgery.
- Risk Factor Modification: If modifiable risk factors are identified, such as smoking, obesity, or poorly controlled diabetes, patients will be advised to address these before surgery to minimize complications.
The Surgical Procedure and Anesthesia
The surgery itself is performed by a specialized surgical team, including the surgeon, anesthesiologist, surgical nurses, and technicians. The anesthesiologist plays a critical role in managing the patient’s vital signs, administering anesthesia, and ensuring pain control throughout the procedure. The duration of major surgeries can range from several hours to over a day, depending on the complexity.
Post-Operative Intensive Monitoring and Management
Following a major surgery, patients are typically transferred to a Post-Anesthesia Care Unit (PACU) for close monitoring as they emerge from anesthesia. For more complex or critical procedures, transfer to an Intensive Care Unit (ICU) is common. In the ICU, continuous monitoring of heart rate, blood pressure, oxygen saturation, and respiratory function is performed.
Key aspects of post-operative management include:
- Pain Management: Effective pain control is essential to allow patients to participate in their recovery, including deep breathing exercises and mobilization. This may involve intravenous medications, patient-controlled analgesia (PCA) pumps, or oral pain relievers.
- Fluid and Electrolyte Balance: Intravenous fluids are administered to maintain hydration and electrolyte balance, which can be significantly disrupted by major surgery.
- Respiratory Support: Patients are encouraged to perform deep breathing exercises and use incentive spirometers to prevent lung complications like pneumonia. In some cases, mechanical ventilation may be required initially.
- Early Mobilization: As soon as medically feasible, patients are encouraged to move and ambulate. This helps prevent blood clots, pneumonia, and muscle weakness, and promotes gastrointestinal function.
- Wound Care: Careful attention is paid to surgical incision sites to prevent infection and promote healing. This includes regular dressing changes and monitoring for signs of infection.
- Nutritional Support: Once bowel function returns, patients gradually progress from clear liquids to solid foods. For some major surgeries, specialized dietary plans or nutritional support may be required.
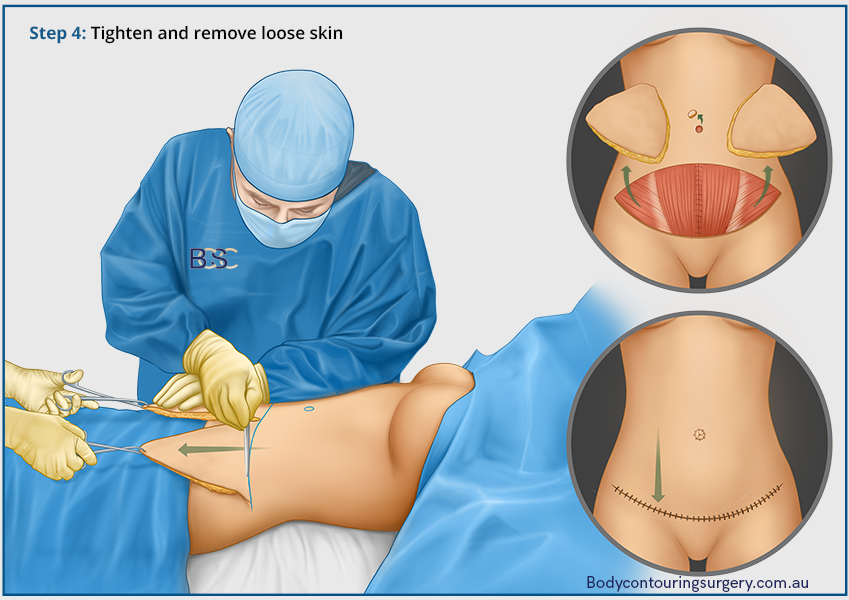
Rehabilitation and Long-Term Recovery
The recovery phase after a major surgery can be lengthy, often extending for weeks or months. This period is crucial for regaining strength, function, and returning to normal activities.
- Physical Therapy: Often a cornerstone of recovery, physical therapists guide patients through exercises to improve strength, flexibility, balance, and mobility.
- Occupational Therapy: For procedures affecting daily living activities, occupational therapists help patients relearn tasks such as dressing, bathing, and preparing meals.
- Psychological Support: The physical and emotional toll of major surgery can be significant. Patients may benefit from counseling or support groups to cope with anxiety, depression, or body image changes.
- Follow-up Appointments: Regular follow-up appointments with the surgical team are vital to monitor healing, manage any lingering symptoms, and address long-term concerns.
The successful navigation of major surgery relies on a collaborative effort between the patient, the surgical team, and their support network, with a strong emphasis on informed consent, diligent preparation, and dedicated post-operative care.
