The Apgar score is a rapid assessment tool used by healthcare professionals to evaluate the physical condition of a newborn immediately after birth. Developed by Dr. Virginia Apgar in 1952, this scoring system provides a quick snapshot of a baby’s transition from the womb to the outside world. It is not a diagnostic tool for long-term health but rather an indicator of immediate needs and the effectiveness of resuscitation if required. Understanding what constitutes a normal Apgar score is crucial for parents and healthcare providers alike, offering reassurance or signaling the need for prompt intervention.
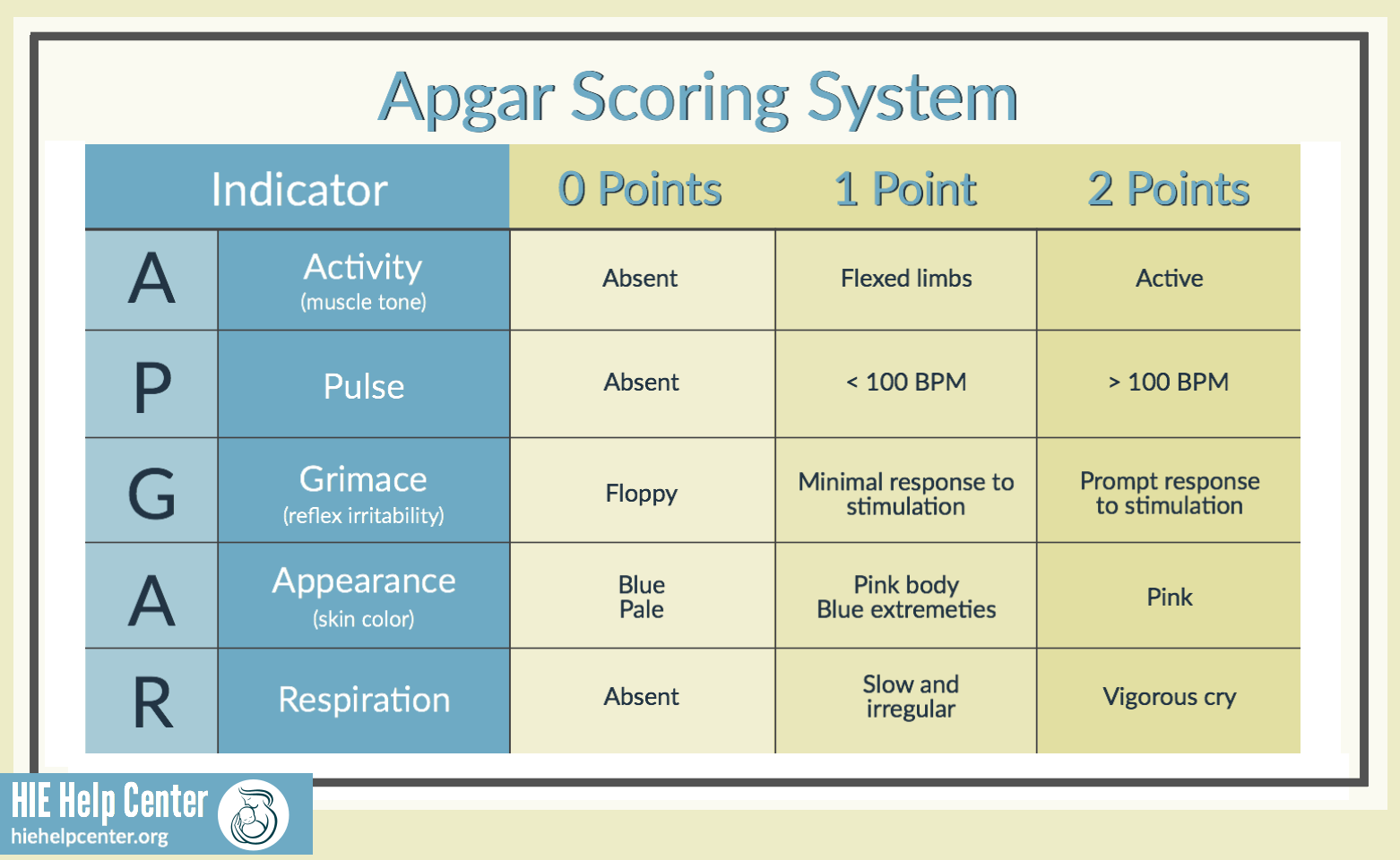
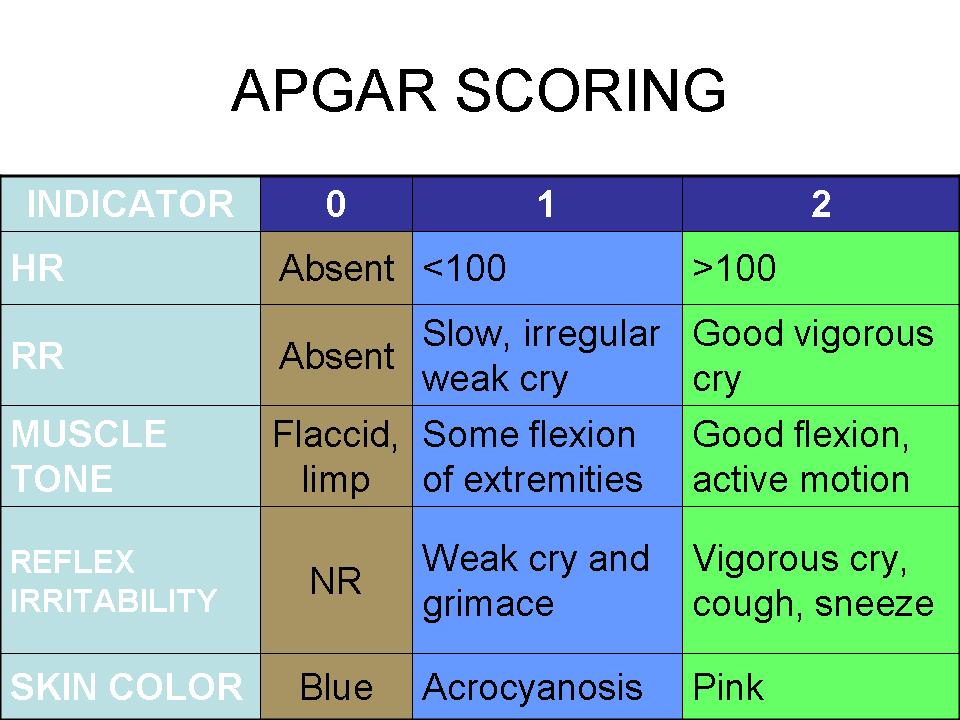
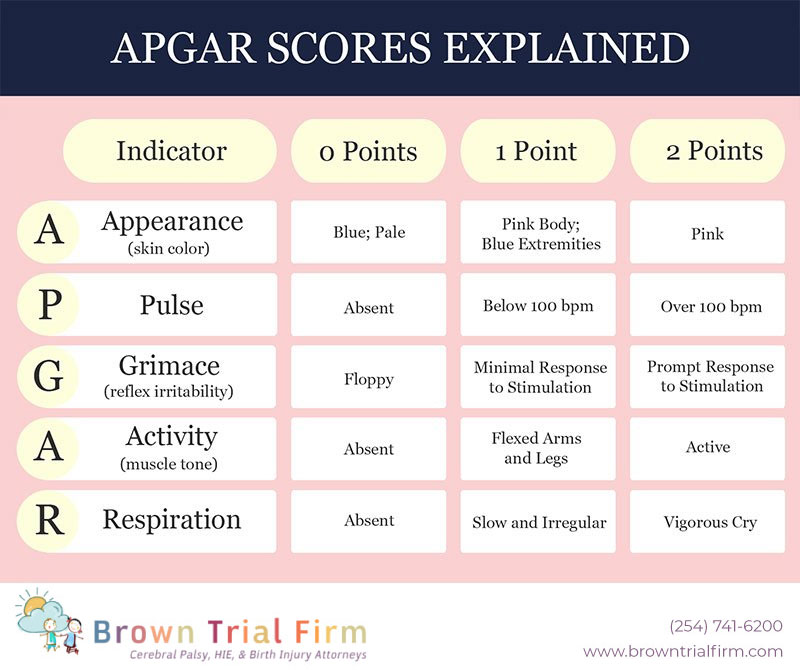
The Apgar score is calculated at one minute and five minutes after birth. In some cases, it may be repeated at ten minutes if the score remains low. The assessment comprises five components, each scored on a scale of 0, 1, or 2. These components are:
-
Appearance (Skin Color): This assesses the baby’s skin color. A score of 2 is given if the skin is uniformly pink. A score of 1 is assigned if the baby has pink extremities but a blueish torso (acrocyanosis), which is common in newborns due to circulatory adjustments. A score of 0 indicates a pale or bluish-all-over appearance.
-
Pulse (Heart Rate): This measures the baby’s heart rate. A normal heart rate for a newborn is typically between 100 and 160 beats per minute. A score of 2 is given if the heart rate is above 100 beats per minute. A score of 1 is awarded if the heart rate is below 100 beats per minute. A score of 0 indicates no detectable heart rate.
-
Grimace (Reflex Irritability): This component assesses the baby’s response to stimulation, such as a gentle flick on the soles of the feet or being suctioned. A score of 2 signifies a strong, active response, such as coughing, crying, or withdrawing from the stimulus. A score of 1 indicates a grimace or a weak cry in response to stimulation. A score of 0 means there is no response to stimulation.
-
Activity (Muscle Tone): This evaluates the baby’s muscle tone and movement. A score of 2 is given for good muscle activity, with spontaneous and active movements. A score of 1 is assigned if there is some flexion of the limbs or minimal movement. A score of 0 indicates limpness and no muscle movement.
-
Respiration (Breathing Effort): This assesses the baby’s breathing. A score of 2 is awarded for a strong, vigorous cry and good respiratory effort. A score of 1 is given for slow or irregular breathing or a weak cry. A score of 0 indicates that the baby is not breathing.
Interpreting the Apgar Score
The total Apgar score is the sum of the scores for each of the five components, ranging from 0 to 10.
Scores at One Minute
The Apgar score at one minute provides an initial assessment of the baby’s transition and the effectiveness of any immediate interventions.
-
A score of 7-10: This is considered a normal Apgar score. It indicates that the baby is transitioning well to life outside the womb and generally does not require significant medical intervention. Most newborns fall into this category.
-
A score of 4-6: This range suggests that the baby may need some assistance with breathing or other bodily functions. The medical team will closely monitor the infant and may provide oxygen, suctioning, or gentle stimulation to encourage the baby to breathe more effectively and maintain their heart rate.
-
A score of 0-3: This low score indicates that the baby is in significant distress and requires immediate medical attention and resuscitation. This might involve providing oxygen, assisted ventilation (breathing support), or chest compressions if the heart rate is critically low.
Scores at Five Minutes
The Apgar score at five minutes is a more reliable indicator of the baby’s condition and the effectiveness of any resuscitation efforts.
-
A score of 7-10: This is considered a normal Apgar score at five minutes and suggests a favorable outcome. The baby is likely stable and continuing to adjust well.
-
A score of 4-6: A score in this range at five minutes indicates that the baby is still experiencing some difficulties but is responding to interventions. Continued close monitoring and support will be provided.
-
A score of 0-3: A persistently low Apgar score at five minutes suggests that the baby remains compromised and may require continued intensive care. The medical team will continue with resuscitation and further assessment to determine the underlying cause of the distress.
Scores at Ten Minutes
If the Apgar score at five minutes is still low (0-3), the assessment will be repeated at ten minutes. A score in this range at ten minutes, especially if it shows improvement, indicates that the resuscitation efforts are starting to be effective. However, continued close monitoring in a neonatal intensive care unit (NICU) may still be necessary depending on the infant’s overall condition.
Factors Influencing Apgar Scores
Several factors can influence a newborn’s Apgar score, and it’s important to remember that a lower score does not automatically imply long-term problems.
Gestational Age
Premature babies often have lower Apgar scores, particularly at one minute. This is because their bodies are not yet fully developed, and they may struggle with temperature regulation, breathing, and muscle tone. For instance, a premature infant might have a good heart rate and reflex irritability but weaker muscle tone and less vigorous breathing, leading to a lower score.
Maternal Health Conditions
Certain maternal health conditions during pregnancy can affect the baby’s well-being at birth. These can include:
- Preeclampsia or Gestational Diabetes: These conditions can impact fetal growth and development, potentially leading to a more challenging transition.
- Infections: Maternal infections can sometimes affect the baby, leading to fetal distress.
- Substance Use: The use of alcohol or drugs during pregnancy can significantly impact a newborn’s physical condition and Apgar score.
Labor and Delivery Complications
Complications during labor and delivery can also influence the Apgar score:
- Nuchal Cord (Umbilical Cord Around the Neck): While often benign, a tightly wrapped nuchal cord can sometimes restrict oxygen flow.
- Placental Abruption or Placenta Previa: These serious conditions can lead to reduced oxygen supply to the fetus.
- Prolonged Labor or Difficult Delivery: These situations can sometimes cause stress to the baby, impacting their immediate condition.
- Meconium Aspiration: If the baby inhales meconium (fetal stool) during labor or delivery, it can cause respiratory distress.
Medications Administered to the Mother
Certain medications given to the mother during labor can affect the baby’s respiratory drive and muscle tone. For example, strong pain relievers or sedatives administered close to delivery might lead to a temporarily lower Apgar score.
What a Normal Apgar Score Means and Doesn’t Mean
A normal Apgar score (7-10) is a reassuring sign that the newborn is transitioning well from intrauterine life to extrauterine life. It indicates that the baby’s vital systems are functioning adequately and that they are likely to adapt without significant immediate medical intervention. Parents can generally feel relieved when their baby receives a good Apgar score.
However, it is crucial to understand what a normal Apgar score does not mean. It is not a predictor of the baby’s future intelligence, development, or overall health. A baby with a perfect 10/10 Apgar score could still develop health issues later in life, just as a baby with a lower initial score can grow up to be perfectly healthy.
Conversely, a low Apgar score is not a guarantee of long-term problems. Many newborns who initially receive low scores are successfully resuscitated and go on to thrive. The medical team’s ability to intervene quickly and effectively is paramount. The score is simply a tool to assess the immediate need for medical support.
The Role of the Medical Team
The Apgar score empowers the healthcare team to make swift, informed decisions about a newborn’s care. It allows for:
- Rapid Assessment: Provides a standardized way to assess the newborn’s status.
- Identification of At-Risk Infants: Quickly identifies babies who require immediate attention.
- Monitoring of Interventions: Helps gauge the effectiveness of resuscitation efforts.
- Communication: Offers a common language for healthcare professionals to communicate the baby’s condition.
The healthcare providers performing the Apgar assessment are trained to recognize subtle signs and symptoms. They consider the score in conjunction with other clinical observations. If a baby’s score is concerning, the medical team will initiate appropriate interventions and continue to monitor the infant closely. This might involve placing the baby in an incubator to maintain body temperature, providing respiratory support, or conducting further diagnostic tests to understand any underlying issues.
Conclusion
The Apgar score remains an indispensable tool in obstetrics and neonatology. It is a quick, objective measure that guides immediate postnatal care. A normal Apgar score, typically between 7 and 10 at both one and five minutes, signifies a healthy transition for the newborn. However, it is essential to interpret the score within the broader context of the baby’s overall condition and the care provided by the medical team. While a low score necessitates prompt intervention, it does not predetermine a child’s future health. The Apgar score is a snapshot in time, a critical first step in ensuring a healthy start for every newborn.
