A hiatus hernia, also known as a hiatal hernia, is a medical condition where a portion of the stomach protrudes upward through the diaphragm, a large muscle that separates the abdomen from the chest. The diaphragm has a small opening, called the esophageal hiatus, through which the esophagus passes to connect to the stomach. In a hiatus hernia, this opening becomes abnormally enlarged, allowing the upper part of the stomach to bulge into the chest cavity. While many hiatus hernias are small and cause no symptoms, larger hernias can lead to significant discomfort and health complications. Understanding the causes, symptoms, diagnosis, and treatment of hiatus hernia disease is crucial for effective management and improved quality of life for affected individuals.
Anatomy and Physiology of the Diaphragm and Esophagus
To comprehend hiatus hernia disease, it is essential to understand the normal anatomical relationship between the esophagus and the diaphragm. The esophagus, a muscular tube, serves as the conduit for food and liquids to travel from the pharynx (throat) to the stomach. It traverses the neck, chest (thorax), and then passes through the diaphragm to enter the abdominal cavity.
The diaphragm itself is a dome-shaped muscle located at the base of the chest cavity, playing a critical role in respiration. It contracts during inhalation, flattening and increasing the volume of the chest cavity, which draws air into the lungs. During exhalation, it relaxes, returning to its dome shape and decreasing chest volume, expelling air.
Crucially, the diaphragm has a natural opening, the esophageal hiatus, through which the esophagus passes. This opening is typically surrounded by muscle fibers of the diaphragm. The lower esophageal sphincter (LES), a ring of muscle at the junction of the esophagus and stomach, functions as a valve. It normally remains closed to prevent the acidic contents of the stomach from flowing back into the esophagus. This antireflux barrier is vital in maintaining esophageal health.
The Esophageal Hiatus
The esophageal hiatus is a muscular aperture within the diaphragm. Its size and integrity are paramount in preventing gastrointestinal contents from migrating into the thoracic cavity. The surrounding diaphragmatic muscles provide support and contribute to the function of the LES.
The Lower Esophageal Sphincter (LES)
The LES is a specialized band of muscle that acts as a one-way valve. Its primary role is to relax to allow food to pass from the esophagus into the stomach and then to contract to prevent the reflux of stomach contents back into the esophagus. The LES’s ability to maintain a tight seal is influenced by various factors, including pressure gradients, hormones, and neural signals.
The Role of Intra-abdominal Pressure
The pressure within the abdominal cavity, known as intra-abdominal pressure, plays a significant role in maintaining the position of the stomach and the function of the LES. Activities that increase intra-abdominal pressure, such as heavy lifting, straining during bowel movements, coughing, or pregnancy, can exert upward force on the stomach. In individuals with a weakened or enlarged esophageal hiatus, this increased pressure can contribute to the stomach herniating through the diaphragm.
Types and Causes of Hiatus Hernia
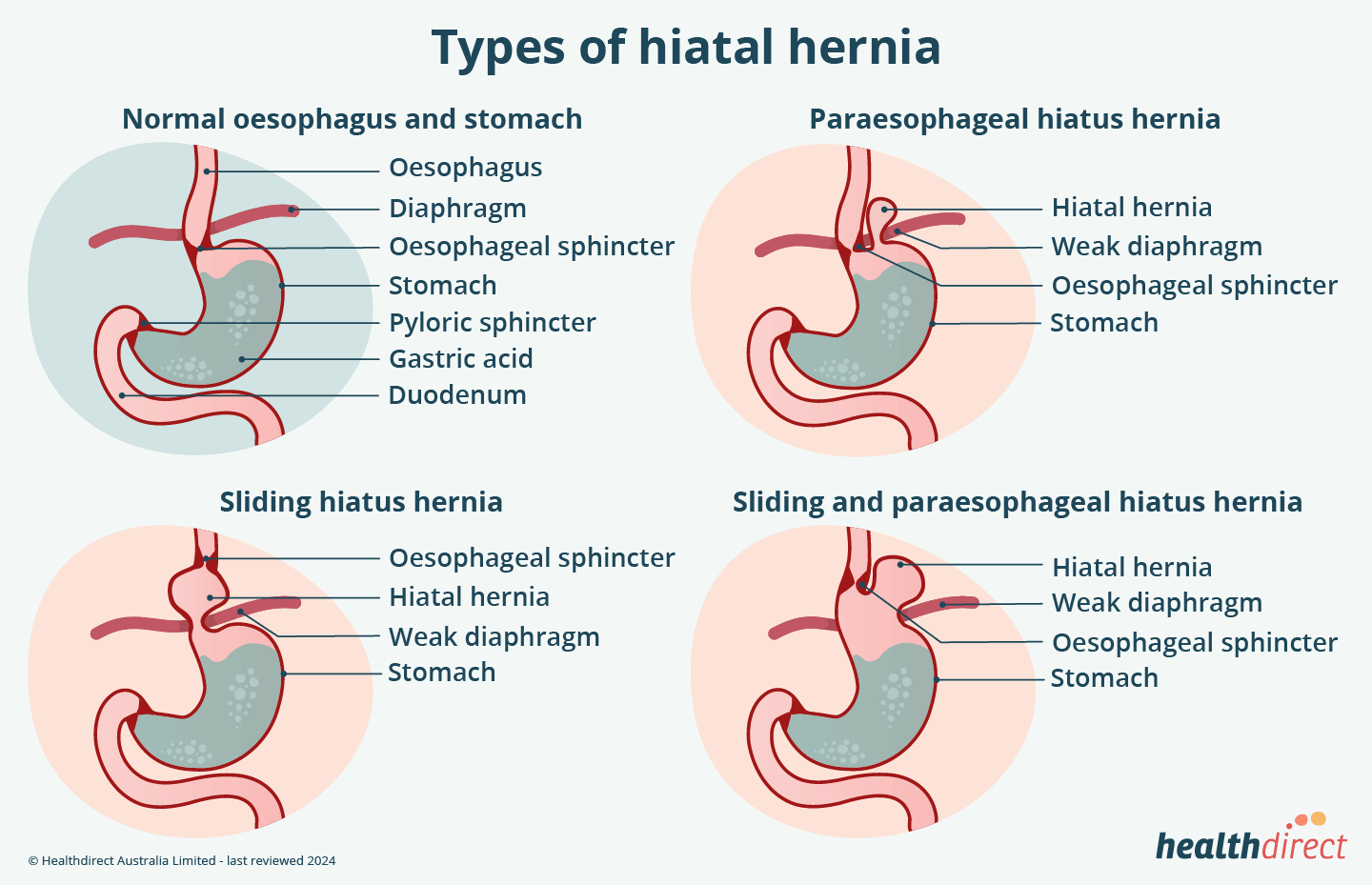
Hiatus hernias are broadly classified into two main types: sliding hernias and paraesophageal hernias. Each type has distinct characteristics and potential implications.
Sliding Hiatus Hernia
The most common type of hiatus hernia, accounting for approximately 95% of cases, is the sliding hiatus hernia. In this type, the junction between the esophagus and the stomach (the gastroesophageal junction) slides upward through the esophageal hiatus into the chest. The hernia is “sliding” because the gastroesophageal junction moves back and forth between the abdomen and the chest. While the gastroesophageal junction itself protrudes, the stomach often remains largely in its normal abdominal position.
Causes of Sliding Hiatus Hernia:
- Increased Intra-abdominal Pressure: As mentioned earlier, prolonged or repeated increases in abdominal pressure are a primary contributing factor. This can be due to:
- Obesity: Excess abdominal fat increases pressure on the stomach.
- Pregnancy: The growing uterus exerts pressure on abdominal organs.
- Chronic Coughing: Conditions like chronic bronchitis or asthma can lead to persistent coughing.
- Straining: Constipation or difficult bowel movements requiring straining.
- Heavy Lifting: Frequent or strenuous physical exertion.
- Vomiting: Forceful expulsion of stomach contents.
- Weakening of Diaphragmatic Muscles: Over time, the muscles of the diaphragm, particularly around the esophageal hiatus, can weaken, making them more susceptible to stretching and enlargement. Age and certain surgical procedures can contribute to this weakening.
- Congenital Factors: In some individuals, the esophageal hiatus may be naturally larger from birth.
Paraesophageal Hiatus Hernia
Paraesophageal hiatus hernias are less common but can be more serious. In this type, a portion of the stomach, typically the fundus (the upper part of the stomach), protrudes through the esophageal hiatus and lies beside the esophagus in the chest cavity. The gastroesophageal junction, however, remains in its normal position below the diaphragm.
There are further sub-classifications of paraesophageal hernias:
- Type II (True Paraesophageal Hernia): The gastroesophageal junction remains in place, but the gastric fundus herniates through the hiatus.
- Type III (Mixed or Compound Hernia): Both the gastroesophageal junction and the gastric fundus herniate through the hiatus. This is considered a more severe form of paraesophageal hernia.
- Type IV: This rare type involves herniation of other abdominal organs, such as the colon, spleen, or pancreas, into the chest cavity through a large hiatus.
Causes of Paraesophageal Hiatus Hernia:
The causes of paraesophageal hernias are similar to those of sliding hernias, involving increased intra-abdominal pressure and weakening of the diaphragmatic structures. However, the nature of the herniation suggests a more significant defect in the supporting tissues around the hiatus.
Risk Factors
Several factors can increase an individual’s risk of developing a hiatus hernia:
- Age: The incidence of hiatus hernias increases with age, as tissues naturally lose elasticity and strength.
- Obesity: As noted, excess weight significantly raises intra-abdominal pressure.
- Smoking: Smoking can lead to chronic coughing and may also weaken connective tissues.
- Family History: A genetic predisposition may exist in some families.
- Previous Abdominal Surgery: Scarring or weakening of the diaphragm from surgery can be a factor.
Symptoms and Complications of Hiatus Hernia Disease
Many individuals with small hiatus hernias experience no noticeable symptoms. However, larger hernias or those that cause complications can lead to a range of uncomfortable and sometimes serious issues. The symptoms are often related to the mechanical displacement of the stomach and the impaired function of the LES.
Common Symptoms

The most frequent symptom associated with hiatus hernias is gastroesophageal reflux disease (GERD). When the stomach protrudes through the diaphragm, it can weaken the LES, allowing stomach acid and contents to back up into the esophagus. This reflux can cause:
- Heartburn: A burning sensation in the chest, often felt behind the breastbone, which may worsen after eating, when lying down, or bending over.
- Regurgitation: The backward flow of undigested food or sour liquid into the throat or mouth.
- Chest Pain: This can mimic the pain of a heart attack, making it crucial to seek medical evaluation to rule out cardiac issues. The pain is often described as sharp, stabbing, or burning.
- Difficulty Swallowing (Dysphagia): A feeling of food getting stuck in the throat or chest. This can be due to inflammation, scarring, or a physical blockage.
- Belching and Bloating: Excessive gas and a feeling of fullness in the stomach.
- Nausea: A feeling of sickness with an inclination to vomit.
- Sore Throat and Hoarseness: Acid irritation of the throat can cause these symptoms.
- Dry Cough: Persistent coughing, especially at night, can be triggered by acid reflux irritating the airways.
Less Common but Significant Symptoms
In some cases, particularly with paraesophageal hernias, more severe symptoms can arise due to the mechanical effects of the displaced stomach:
- Abdominal Pain: Pain in the upper abdomen, which may be severe or colicky.
- Vomiting: While vomiting can occur with reflux, it can also be a sign of more significant obstruction or twisting of the herniated stomach.
- Anemia: Chronic, slow bleeding from an inflamed or ulcerated esophageal lining can lead to iron-deficiency anemia. This may manifest as fatigue, pale skin, and shortness of breath.
- Shortness of Breath: When a large portion of the stomach herniates into the chest, it can compress the lungs, leading to difficulty breathing, especially during physical exertion.
Potential Complications
If left untreated, hiatus hernias, especially paraesophageal types, can lead to serious complications:
- Esophagitis: Inflammation of the esophagus caused by chronic acid reflux. This can lead to pain, difficulty swallowing, and increased risk of bleeding.
- Strictures: Scarring and narrowing of the esophagus due to chronic inflammation. This can cause severe dysphagia, making it difficult to eat and drink.
- Ulcers: Open sores can develop on the lining of the esophagus or the herniated stomach.
- Bleeding: Ulcers or inflamed tissue can bleed, leading to anemia or, in severe cases, acute hemorrhage.
- Strangulation: This is a rare but life-threatening complication where the blood supply to the herniated portion of the stomach is cut off. It causes severe pain, vomiting, and requires emergency surgery.
- Incarceration: The herniated stomach becomes trapped in the chest and cannot be pushed back into the abdomen. This can lead to severe pain and potential obstruction.
The severity of symptoms and the risk of complications are often related to the size of the hernia, the type of hernia, and the degree of LES dysfunction. Early diagnosis and appropriate management are crucial to prevent these adverse outcomes.
Diagnosis and Treatment of Hiatus Hernia Disease
Diagnosing a hiatus hernia typically involves a combination of medical history, physical examination, and diagnostic imaging. The treatment approach depends on the severity of symptoms, the type of hernia, and the presence of complications.
Diagnostic Methods
-
Medical History and Physical Examination: The physician will inquire about your symptoms, including their frequency, intensity, and what makes them better or worse. They will also perform a physical examination to assess for tenderness or abnormalities.
-
Barium Swallow X-ray (Esophagogram): This is often the first imaging test performed. You will drink a liquid containing barium sulfate, a contrast agent that coats the lining of your esophagus and stomach. X-rays are then taken as you swallow, allowing the radiologist to visualize the passage of barium and identify any abnormalities, including a hiatus hernia.
-
Upper Endoscopy (Esophagogastroduodenoscopy or EGD): In this procedure, a thin, flexible tube with a camera (endoscope) is inserted down your esophagus, into your stomach, and the first part of your small intestine (duodenum). The doctor can directly visualize the lining of these organs, identify inflammation, ulcers, or strictures, and assess the function of the LES. Biopsies can also be taken during an endoscopy to rule out other conditions.
-
Esophageal Manometry: This test measures the pressure and coordination of muscle contractions in your esophagus and the LES. It helps assess the strength of the LES and identify any functional problems that may be contributing to reflux.
-
pH Monitoring: This test measures the amount of acid refluxing into your esophagus over a 24-hour period. It is particularly useful in diagnosing GERD and assessing its severity, especially when other tests are inconclusive.
Treatment Strategies
Treatment for hiatus hernia disease aims to alleviate symptoms, prevent complications, and improve the patient’s quality of life.
Lifestyle Modifications
For individuals with mild symptoms, lifestyle changes are often the first line of treatment:
- Dietary Adjustments: Avoiding trigger foods that worsen reflux, such as fatty foods, spicy foods, chocolate, peppermint, caffeine, and alcohol. Eating smaller, more frequent meals can also help.
- Weight Management: Losing excess weight can significantly reduce intra-abdominal pressure and alleviate symptoms.
- Elevating the Head of the Bed: Raising the head of the bed by 6-8 inches (using blocks under the bedposts or a wedge pillow) can help prevent nighttime reflux.
- Avoiding Lying Down After Meals: Waiting at least 2-3 hours after eating before lying down or going to bed.
- Quitting Smoking: Smoking weakens the LES and exacerbates reflux symptoms.
- Avoiding Tight Clothing: Loose-fitting clothing around the abdomen can reduce pressure.
- Managing Constipation: Ensuring regular bowel movements and avoiding straining.
Medications
If lifestyle modifications are insufficient, medications may be prescribed to manage symptoms:
- Antacids: Over-the-counter medications like Tums or Rolaids neutralize stomach acid, providing quick relief for occasional heartburn.
- H2 Blockers (Histamine-2 Receptor Antagonists): Medications such as famotidine (Pepcid) or ranitidine (Zantac, though availability may vary) reduce the amount of acid produced by the stomach. They provide longer-lasting relief than antacids.
- Proton Pump Inhibitors (PPIs): These are the most potent acid-reducing medications and include drugs like omeprazole (Prilosec), lansoprazole (Prevacid), and esomeprazole (Nexium). PPIs block the “pumps” in the stomach lining that produce acid, offering significant relief for persistent GERD and allowing healing of esophageal damage.

Surgical Intervention
Surgery is typically reserved for individuals with severe symptoms that do not respond to medical management, those with complications like strictures or bleeding, or those with large paraesophageal hernias that pose a risk of strangulation or incarceration.
The most common surgical procedure for hiatus hernia repair is fundoplication. In this surgery, the surgeon wraps the upper part of the stomach (the fundus) around the lower esophagus. This reinforces the LES, creating a tighter valve to prevent reflux. Fundoplication can be performed using minimally invasive laparoscopic techniques, which involve smaller incisions and result in faster recovery times.
Other surgical approaches may be used depending on the specific type and complexity of the hernia, including:
- Gastrolysis: Releasing adhesions that may be contributing to the hernia.
- Hernia Repair: Reinforcing the diaphragmatic opening with sutures or surgical mesh.
- Esophageal Lengthening Procedures: In cases of a very short esophagus, the surgeon may need to perform procedures to lengthen the esophagus before or during the fundoplication.
The decision to undergo surgery is made after careful consideration of the risks and benefits, in consultation with a qualified surgeon. Post-operative care and follow-up are essential to ensure successful recovery and long-term symptom control.
