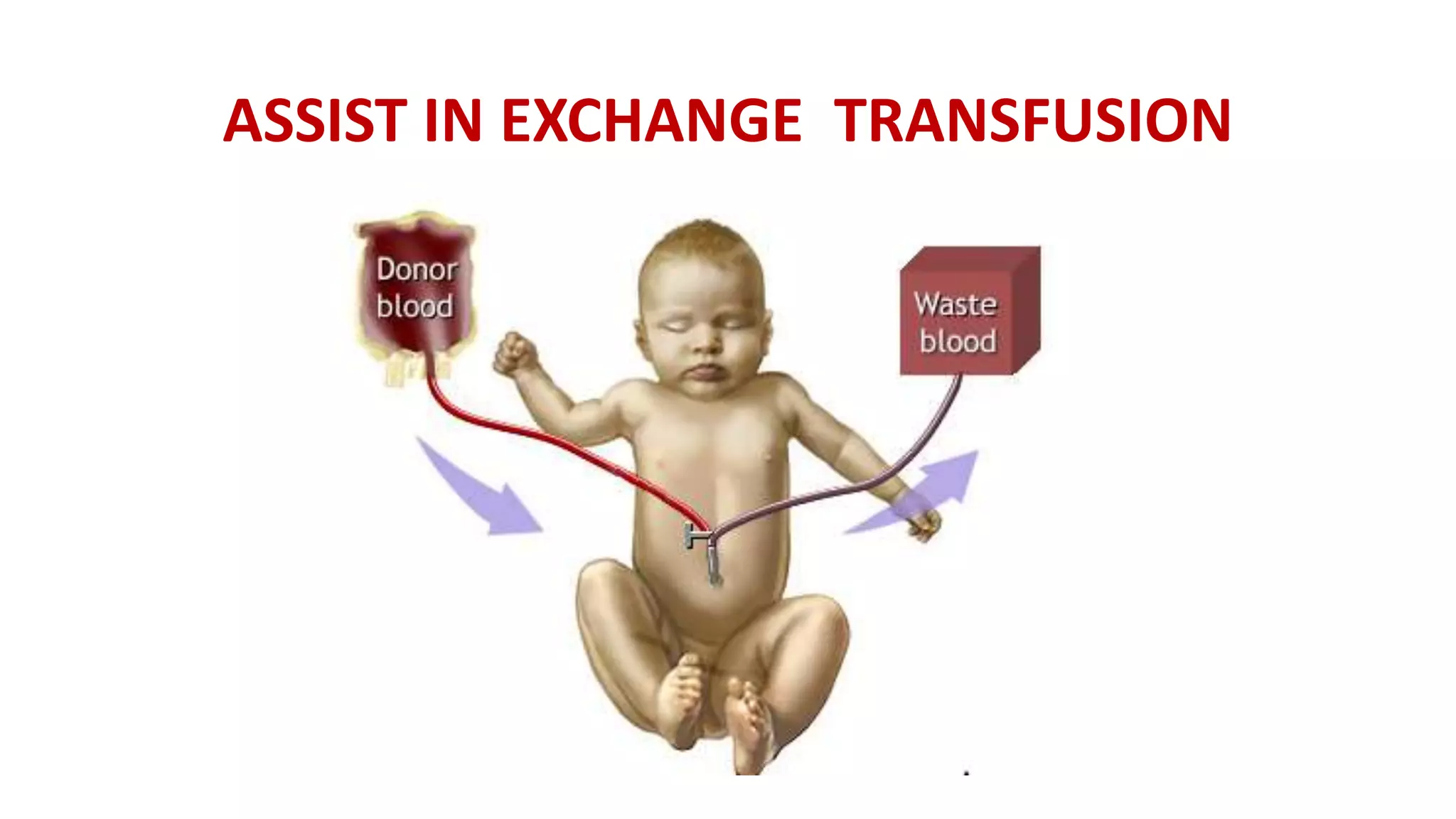
Exchange transfusion is a critical medical procedure primarily used in neonatology to address severe conditions such as hyperbilirubinemia (jaundice) and certain blood incompatibilities. It involves the replacement of a newborn’s blood with donor blood, effectively removing bilirubin and antibodies that can cause significant harm if left untreated. While seemingly straightforward, the procedure is intricate, requiring careful management and a deep understanding of its indications, contraindications, techniques, and potential complications.
Understanding Hyperbilirubinemia and Its Risks
Hyperbilirubinemia is a common condition in newborns, characterized by elevated levels of bilirubin in the blood. Bilirubin is a yellowish pigment produced during the normal breakdown of red blood cells. In healthy adults, the liver efficiently processes bilirubin, excreting it from the body. However, newborn infants often have immature liver function, making it difficult to clear bilirubin as quickly.
The Role of Bilirubin
Bilirubin exists in two forms: unconjugated (indirect) and conjugated (direct). Unconjugated bilirubin is lipid-soluble and can cross the blood-brain barrier, particularly in newborns whose barrier is still developing. When unconjugated bilirubin levels become excessively high, it can deposit in the brain tissue, leading to a severe and potentially irreversible neurological disorder known as kernicterus. Kernicterus can manifest as a range of symptoms including lethargy, poor feeding, high-pitched cry, arching of the back, seizures, and ultimately, cerebral palsy and hearing loss.
Causes of Severe Hyperbilirubinemia
Several factors can contribute to severe hyperbilirubinemia in newborns, necessitating interventions like exchange transfusion:
- Physiological Jaundice: This is the most common form, occurring in about 60% of full-term and 80% of premature infants. It typically appears after the first 24 hours of life and resolves within a week or two. However, in some cases, it can become severe.
- Breastfeeding Jaundice: This type is associated with insufficient milk intake, leading to dehydration and reduced bowel movements, which slows down bilirubin excretion.
- Breast Milk Jaundice: Less common, this is thought to be caused by substances in the mother’s milk that interfere with bilirubin metabolism.
- Hemolytic Disease of the Newborn (HDN): This is a serious cause of severe jaundice resulting from incompatibility between the mother’s and infant’s blood types. The most common scenario is Rh incompatibility, where an Rh-negative mother carries an Rh-positive baby. During pregnancy or delivery, fetal red blood cells can enter the mother’s circulation, sensitizing her immune system. In subsequent pregnancies, the mother’s antibodies can cross the placenta and attack the fetus’s red blood cells, leading to rapid destruction and a sharp increase in bilirubin. ABO incompatibility is another, generally milder, form of HDN.
- G6PD Deficiency: A genetic enzyme deficiency that can make red blood cells more vulnerable to breakdown, especially when exposed to certain drugs, infections, or foods.
- Sepsis: Bacterial infections can impair liver function and increase bilirubin production.
- Cephalohematoma and Bruising: Significant bleeding under the scalp or extensive bruising can lead to the breakdown of large amounts of red blood cells.
When Phototherapy Isn’t Enough
Phototherapy is the first-line treatment for most cases of neonatal hyperbilirubinemia. It involves exposing the infant to specific wavelengths of light that help convert unconjugated bilirubin into water-soluble forms that can be more easily excreted. However, phototherapy is not always sufficient. If bilirubin levels rise rapidly, reach dangerously high thresholds despite phototherapy, or if the infant shows signs of acute bilirubin encephalopathy, an exchange transfusion becomes necessary.
The Exchange Transfusion Procedure Explained
Exchange transfusion is a complex procedure that requires a sterile environment, skilled personnel, and careful monitoring. It is typically performed in a Neonatal Intensive Care Unit (NICU) or a specialized procedure room.
Indications for Exchange Transfusion
The decision to perform an exchange transfusion is based on established clinical guidelines, considering the infant’s age, bilirubin levels, rate of rise, presence of risk factors (such as prematurity, sepsis, or hemolysis), and clinical signs of encephalopathy. Generally, indications include:
- Total Serum Bilirubin (TSB) levels exceeding 20 mg/dL in term infants or 15 mg/dL in preterm infants within the first few days of life. These are approximate guidelines and may vary based on specific hospital protocols and the infant’s overall condition.
- Rapid rise in TSB levels (e.g., >0.5 mg/dL per hour).
- Evidence of acute bilirubin encephalopathy (e.g., lethargy, poor suck, hypotonia, high-pitched cry, arching).
- Hemolytic disease of the newborn with a positive direct antiglobulin test (DAT) and falling hemoglobin levels.
Contraindications
While exchange transfusion is a life-saving procedure, it is not without risks. Relative contraindications might include severe cardiorespiratory instability, which could be exacerbated by the fluid shifts involved. The decision is always made on a case-by-case basis, weighing the risks against the potential benefits.
Types of Exchange Transfusion
There are two primary methods of performing an exchange transfusion:
1. Partial Exchange Transfusion
In this method, a small amount of the infant’s blood is withdrawn and replaced with donor blood. This is often used when the primary goal is to reduce bilirubin levels without significantly altering the total blood volume or hemoglobin concentration. It is less common than total exchange.
2. Total Exchange Transfusion
This is the more common and effective method. It involves the stepwise removal of the infant’s blood and its simultaneous replacement with donor blood. The goal is to replace a significant portion of the infant’s blood volume.
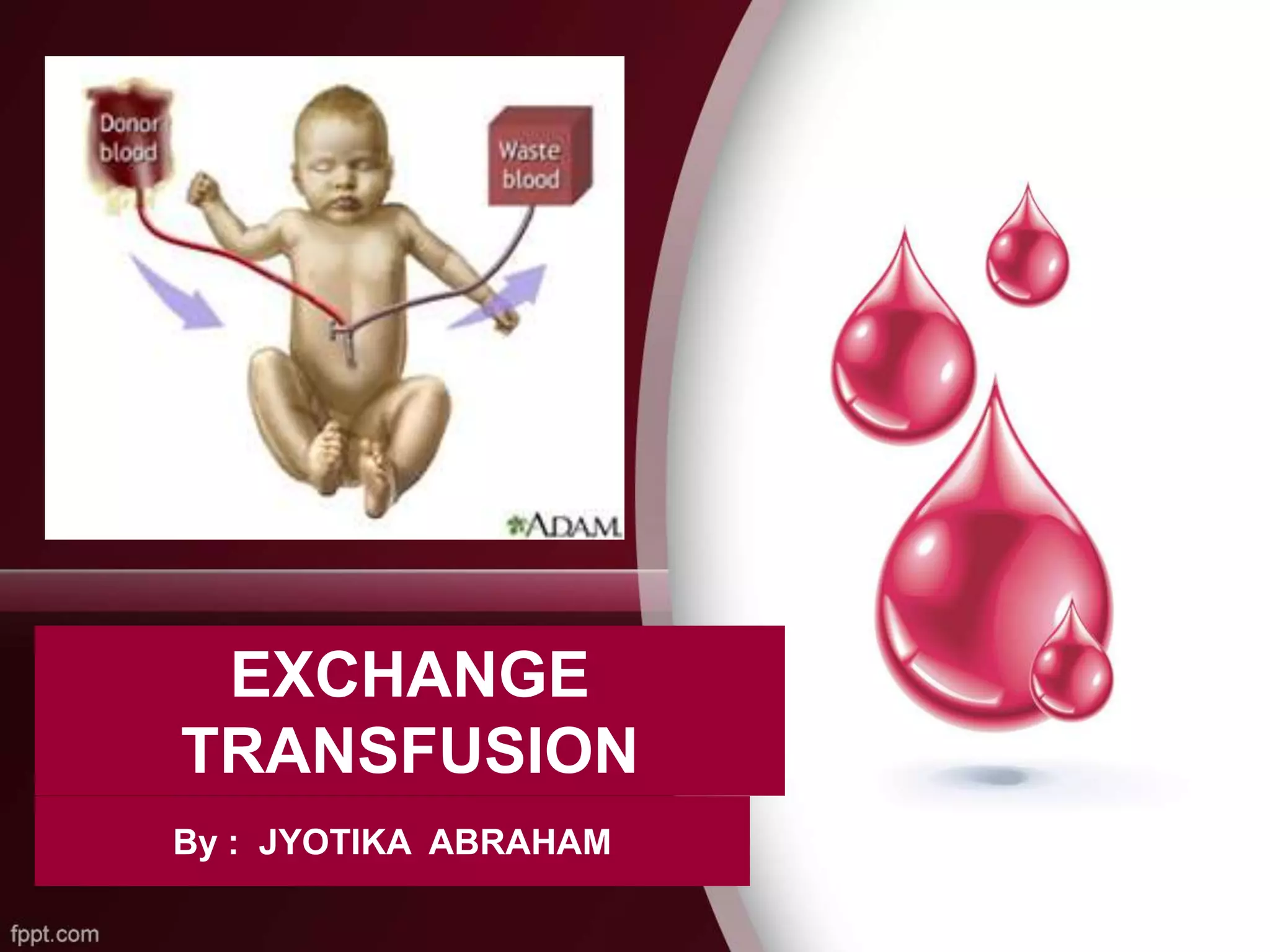
The Procedure Steps
A total exchange transfusion is typically performed using a double-volume exchange, which aims to replace approximately twice the infant’s total blood volume. This is achieved by withdrawing and infusing equal volumes of blood in multiple small aliquots.
-
Preparation:
- Blood Selection: Donor blood must be carefully selected. It should be fresh (usually less than 48-72 hours old), cross-matched with the mother’s serum, and free from any significant antibodies that could react with the infant’s red blood cells. Rh-negative blood is typically used for Rh-isoimmunization cases.
- Equipment: A sterile setup is essential, including catheters (umbilical venous or arterial catheters are commonly used, or peripheral IV lines), syringes, blood administration sets, a warmer for the donor blood, and monitoring equipment for vital signs.
- Sedation and Analgesia: The infant may receive mild sedation to minimize distress and movement.
- Monitoring: Continuous monitoring of heart rate, respiratory rate, oxygen saturation, blood pressure, and temperature is crucial throughout the procedure.
-
Catheterization:
- An umbilical venous catheter (UVC) or an umbilical arterial catheter (UAC) is typically inserted. UVCs are often preferred for infusions, while UACs can be used for withdrawal and monitoring of arterial blood pressure. Peripheral venous catheters are an alternative.
-
The Exchange:
- The procedure involves withdrawing small amounts of the infant’s blood (e.g., 5-10 mL, depending on the infant’s size) through one catheter and simultaneously infusing an equal amount of donor blood through another.
- This process is repeated in a slow, step-by-step manner. This gradual exchange minimizes sudden hemodynamic changes and reduces the risk of complications.
- Throughout the exchange, the infant’s blood gases, electrolytes (especially calcium and potassium), and glucose levels are closely monitored, as these can fluctuate. Calcium levels are particularly important, as citrate, an anticoagulant in donor blood, can bind to calcium, leading to hypocalcemia. Calcium gluconate may be administered as needed.
- The total volume of blood exchanged is typically 160-180 mL/kg, which is about twice the infant’s blood volume.
-
Completion:
- Once the target volume has been exchanged, the catheters are removed, and appropriate pressure is applied to the insertion sites.
- The infant is closely monitored for any immediate complications.
Post-Procedure Care
After an exchange transfusion, the infant requires vigilant observation. This includes:
- Continuous Vital Sign Monitoring: For at least 24 hours.
- Serial Bilirubin Levels: To assess the effectiveness of the procedure and monitor for rebound elevations.
- Blood Count: To check hemoglobin and hematocrit levels.
- Electrolyte Monitoring: Especially calcium and potassium.
- Assessment for Complications: Including signs of infection, bleeding, or cardiac instability.
Potential Complications and Risks
Despite being a vital intervention, exchange transfusion carries inherent risks. These can range from minor to life-threatening.
Common Complications
- Hypocalcemia: As mentioned, citrate in donor blood binds calcium, potentially leading to a drop in serum calcium levels. Symptoms can include irritability, muscle twitching, and in severe cases, seizures.
- Hypoglycemia: Fluctuations in blood glucose can occur.
- Apnea and Bradycardia: These can be triggered by the procedure itself or by changes in temperature or fluid balance.
- Thrombocytopenia: A decrease in platelet count can occur, increasing the risk of bleeding.
- Arrhythmias: Irregular heart rhythms can develop.
- Temperature Instability: The donor blood needs to be warmed to prevent hypothermia in the infant.
Serious Complications
- Infection: Introducing bacteria from the donor blood or through the catheters.
- Air Embolism: If air enters the transfusion line.
- Pulmonary Hemorrhage: Particularly in very premature infants.
- Necrotizing Enterocolitis (NEC): A serious gastrointestinal condition.
- Vascular Complications: Such as thrombosis or damage to blood vessels at the catheter insertion site.
- Graft-versus-Host Disease (GVHD): A rare but severe complication where donor lymphocytes attack the infant’s tissues. This is more common in immunocompromised infants or when using blood from a relative.
- Cardiac Arrest: In rare, severe cases.
The risk of complications is higher in premature or critically ill infants. Meticulous technique, careful patient selection, and vigilant monitoring by experienced healthcare professionals significantly mitigate these risks.
Alternatives and Future Directions
While exchange transfusion remains a cornerstone treatment for severe neonatal hyperbilirubinemia and certain blood disorders, ongoing research and advancements are exploring alternative and adjunctive therapies.
Innovations in Phototherapy
Improvements in phototherapy technology, including more efficient light sources (e.g., LED lights) and delivery systems (e.g., fiberoptic blankets, Biliblankets), can enhance bilirubin breakdown and potentially reduce the need for exchange transfusions in some cases. The ability to administer phototherapy even when the infant is being fed or held by parents can also improve its effectiveness.
Pharmacological Interventions
Medications like phenobarbital have been used to induce liver enzymes and enhance bilirubin conjugation, although their use in the immediate management of severe jaundice is limited. Newer agents, such as tin-mesoporphyrins, which inhibit heme oxygenase (an enzyme involved in bilirubin production), are being investigated for their potential to reduce bilirubin levels and possibly prevent the need for exchange transfusion.
Improved Antenatal Management
For Rh and ABO incompatibilities, meticulous antenatal care, including monitoring fetal well-being, administering Rho(D) immune globulin (RhoGAM) to Rh-negative mothers, and performing intrauterine transfusions, can help manage hemolytic disease before birth, thus reducing the severity of jaundice at birth and potentially avoiding exchange transfusion.
Advances in Donor Blood Management
Research into the optimal storage and preparation of donor blood for exchange transfusions aims to minimize complications like electrolyte imbalances and immunologic reactions.

Conclusion
Exchange transfusion is a powerful, albeit invasive, medical intervention that plays a critical role in saving the lives of newborns suffering from severe hyperbilirubinemia and certain blood disorders. Understanding its indications, the intricate procedure, and its associated risks is paramount for neonatologists and pediatricians. While advancements in phototherapy and pharmacological agents continue to evolve, exchange transfusion remains an indispensable tool in the management of life-threatening neonatal conditions, ensuring that infants have the best possible chance for a healthy future. The careful balance of its life-saving benefits against its potential risks underscores the importance of experienced clinical judgment and vigilant post-procedural care.
