The Evolving Role of the Nurse Case Manager
Nursing case management is a critical, multifaceted approach to healthcare delivery that focuses on optimizing patient outcomes, ensuring efficient resource utilization, and promoting patient advocacy. At its core, it involves a coordinated process of assessment, planning, implementation, coordination, monitoring, and evaluation of a patient’s care, often across various healthcare settings and over an extended period. The nurse case manager acts as a central point of contact, bridging gaps between patients, families, physicians, insurers, and other healthcare providers. This role has evolved significantly from its origins, adapting to the increasing complexity of healthcare systems, the growing prevalence of chronic diseases, and the imperative to control rising healthcare costs while maintaining high-quality care.

The contemporary nurse case manager is not merely a coordinator but a skilled clinician, a strategic planner, and an empathetic advocate. They leverage their clinical expertise to understand the intricate medical needs of their patients, while simultaneously navigating the labyrinthine landscape of insurance policies, regulatory requirements, and community resources. This dual focus allows them to develop individualized care plans that are both clinically appropriate and financially sustainable. The ultimate goal is to ensure that patients receive the right care, at the right time, in the right setting, with the least amount of duplication or waste.
Historical Context and Evolution
The concept of case management in nursing emerged in response to the fragmented nature of healthcare delivery, particularly in the mid-20th century. Early forms of case management often focused on specific populations, such as individuals with mental health conditions or developmental disabilities, aiming to ensure access to necessary services and prevent institutionalization. As healthcare systems grew more complex and the costs escalated, the need for systematic care coordination became more pronounced across all patient populations.
The rise of managed care in the late 20th century further propelled the development and formalization of nursing case management. Insurers sought to control costs by managing the utilization of healthcare services, and nurse case managers were instrumental in this effort. They assessed patient needs, determined the appropriateness of care, and facilitated transitions between different levels of care, such as hospital discharge to home health services or skilled nursing facilities.
In the 21st century, the role of the nurse case manager has expanded beyond cost containment to encompass quality improvement, patient safety, and the promotion of patient self-management. With the increasing emphasis on value-based care, nurse case managers are integral to achieving better health outcomes for populations, improving the patient experience, and reducing per capita costs of healthcare. They are increasingly involved in chronic disease management programs, post-acute care coordination, and care for vulnerable populations facing social determinants of health.
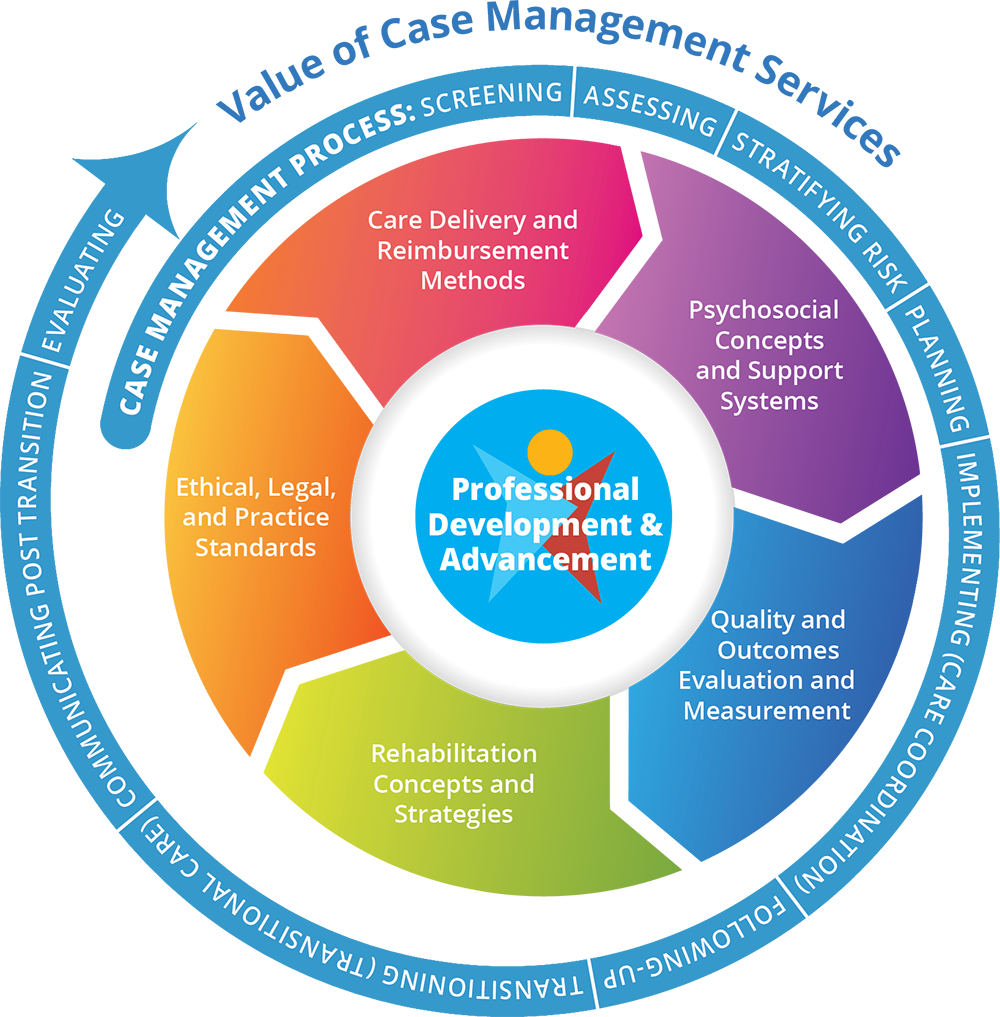
Core Functions and Responsibilities
The nurse case manager’s responsibilities are diverse and dynamic, requiring a blend of clinical acumen, interpersonal skills, and organizational prowess. These functions are interconnected and contribute to a holistic approach to patient care.
Assessment and Planning
The case management process begins with a comprehensive assessment of the patient’s medical, psychosocial, and functional status. This goes beyond a routine clinical assessment to encompass a broader understanding of the patient’s life situation, including their living environment, support systems, financial resources, and cultural beliefs.
- Clinical Assessment: Evaluating the patient’s current health status, diagnoses, treatment plans, medications, and potential complications.
- Psychosocial Assessment: Understanding the patient’s emotional well-being, coping mechanisms, mental health status, and any barriers to care stemming from psychological factors.
- Functional Assessment: Determining the patient’s ability to perform activities of daily living (ADLs) and instrumental activities of daily living (IADLs), which informs the need for supportive services and equipment.
- Resource Assessment: Identifying available patient and family resources, including financial, social, and community support.
Based on this comprehensive assessment, the nurse case manager develops an individualized care plan in collaboration with the patient, their family, and the healthcare team. This plan outlines specific goals, interventions, and expected outcomes.
Coordination and Implementation
Coordination is arguably the most visible and essential function of the nurse case manager. They act as the central hub, ensuring seamless communication and collaboration among all stakeholders involved in the patient’s care.
- Interdisciplinary Collaboration: Facilitating communication and shared decision-making among physicians, nurses, therapists, social workers, pharmacists, and other healthcare professionals.
- Service Facilitation: Arranging for necessary medical services, equipment, and supplies, such as home health visits, physical therapy, durable medical equipment, or prescription medications.
- Transition Management: Planning and executing smooth transitions of care between different settings, such as hospital discharge to home, transfer to a rehabilitation facility, or admission to a long-term care facility. This involves ensuring appropriate handoffs, follow-up appointments, and medication reconciliation.
- Patient and Family Education: Providing education on the patient’s condition, treatment plan, medications, self-care strategies, and available resources to empower them to actively participate in their care.
Monitoring and Evaluation
The nurse case manager continuously monitors the patient’s progress toward their care goals and evaluates the effectiveness of the care plan. This iterative process allows for adjustments as needed.
- Outcome Monitoring: Tracking the patient’s clinical status, functional improvement, and adherence to the treatment plan.
- Resource Utilization Review: Ensuring that healthcare resources are being used efficiently and appropriately, avoiding unnecessary services or duplicate testing.
- Plan Revision: Modifying the care plan based on the patient’s changing needs, progress, or any identified barriers.
- Quality Assurance: Contributing to the overall quality of care by identifying areas for improvement in processes and outcomes.
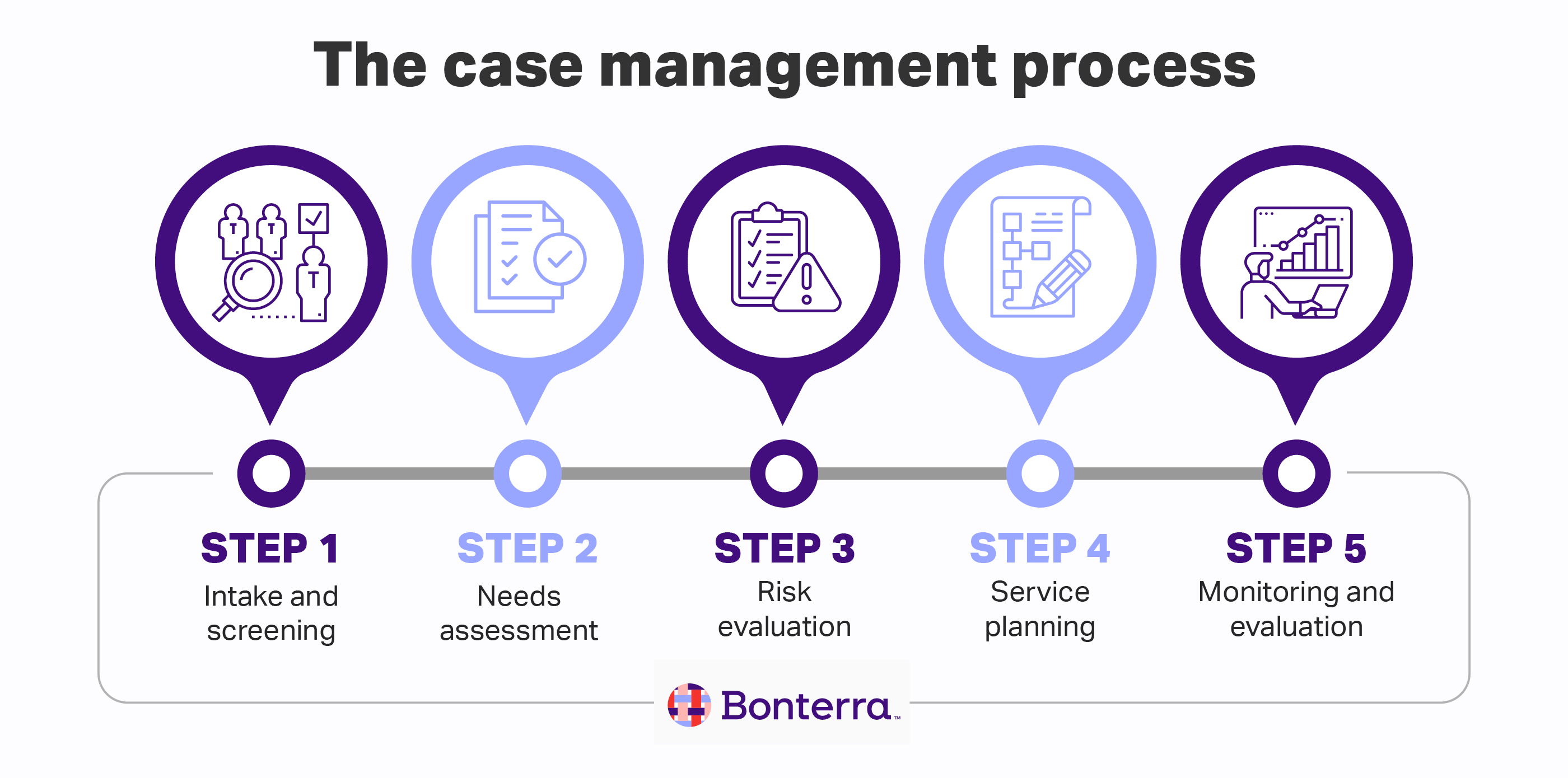
Advocacy
Patient advocacy is a cornerstone of nursing case management. The nurse case manager champions the patient’s rights, needs, and preferences, ensuring their voice is heard within the complex healthcare system.
- Navigating the System: Assisting patients and families in understanding insurance benefits, appealing denied claims, and accessing services that may be difficult to obtain.
- Empowerment: Encouraging patients to take an active role in their healthcare decisions and to express their concerns and preferences.
- Ethical Considerations: Upholding ethical principles by ensuring patient autonomy, confidentiality, and equitable access to care.
Settings and Populations
Nursing case management is practiced across a wide array of healthcare settings and for diverse patient populations, reflecting its adaptability and broad applicability.
Healthcare Settings
- Hospitals: Inpatient case managers work with patients to plan for discharge, coordinate post-hospital care, and ensure a smooth transition to home or another facility. They also manage patients with complex needs who require extensive care coordination during their hospital stay.
- Outpatient Clinics and Physician Practices: Case managers in these settings focus on proactive management of chronic conditions, preventing hospital readmissions, and ensuring patients adhere to treatment plans.
- Home Health Agencies: They coordinate care delivered in the patient’s home, managing a range of needs from wound care to medication management and rehabilitation.
- Rehabilitation Centers: Case managers facilitate recovery by coordinating therapy services, medical care, and discharge planning for patients recovering from illness or injury.
- Skilled Nursing Facilities (SNFs) and Long-Term Care: They manage the ongoing care needs of residents, ensuring their medical, social, and emotional well-being.
- Insurance Companies and Managed Care Organizations: Case managers employed by payers work to manage the care and costs for their members, focusing on utilization review and disease management programs.
- Community Health Centers: They serve underserved populations, addressing a wide range of health and social needs, and connecting patients to necessary resources.
- Government Agencies and Public Health Departments: Case managers in these sectors often focus on specific public health initiatives, such as chronic disease prevention, maternal and child health, or services for vulnerable populations.
Patient Populations
- Patients with Chronic Illnesses: Individuals with conditions like diabetes, heart failure, COPD, and cancer require ongoing management, education, and coordination to maintain their health and quality of life.
- Elderly Patients: Older adults often have multiple comorbidities, functional limitations, and complex medication regimens, making them prime candidates for case management.
- Patients with Complex Medical Needs: Those with rare diseases, multiple chronic conditions, or significant disabilities require intensive coordination to navigate specialized treatments and services.
- Patients Experiencing Mental Health Challenges: Case managers help individuals with psychiatric conditions access mental health services, medication, and supportive resources, often addressing co-occurring physical health issues.
- Pediatric Patients: Case managers work with children who have chronic illnesses, developmental delays, or special healthcare needs, supporting their families through complex treatment plans and educational challenges.
- Patients with Substance Use Disorders: They assist individuals in accessing treatment, counseling, and recovery support services.
- Patients Facing Social Determinants of Health Barriers: Case managers identify and address issues such as housing instability, food insecurity, lack of transportation, and limited financial resources that impact a patient’s ability to achieve health outcomes.
Benefits and Challenges
The implementation of effective nursing case management yields significant benefits for patients, providers, and the healthcare system as a whole. However, it also presents several challenges that require ongoing attention and solutions.
Benefits
- Improved Patient Outcomes: By ensuring coordinated, individualized care, case management can lead to better adherence to treatment plans, reduced hospital readmissions, fewer emergency department visits, and improved overall health status.
- Enhanced Patient Satisfaction: Patients often report higher satisfaction when they have a dedicated point person who understands their needs, advocates for them, and helps them navigate the system.
- Increased Efficiency and Reduced Costs: Streamlined care coordination, appropriate resource utilization, and prevention of unnecessary services can lead to significant cost savings for both patients and the healthcare system.
- Better Communication and Collaboration: Case managers foster improved communication among healthcare providers, reducing medical errors and promoting a more cohesive care team.
- Empowerment of Patients and Families: Through education and support, case managers empower patients to become active participants in their own care and to manage their health more effectively.
- Support for Healthcare Providers: By managing complex patient needs and coordinating care, case managers can alleviate the burden on physicians and other direct care providers, allowing them to focus on their core clinical responsibilities.
Challenges
- System Fragmentation: Despite the efforts of case managers, healthcare systems can remain fragmented, making it difficult to achieve seamless transitions and consistent communication across different providers and settings.
- Resource Limitations: Inadequate staffing, limited funding for services, and insufficient availability of community resources can impede the effectiveness of case management.
- Data Integration and Interoperability: The lack of integrated electronic health records and data sharing across different organizations can hinder a case manager’s ability to obtain a complete picture of a patient’s care.
- Reimbursement Structures: Traditional fee-for-service reimbursement models may not adequately compensate for the time and effort involved in comprehensive case management, creating financial disincentives.
- Patient Engagement and Adherence: Engaging patients, particularly those with complex psychosocial issues or limited health literacy, and ensuring their adherence to care plans can be challenging.
- Scope of Practice and Role Clarity: Defining the precise scope of practice for nurse case managers and ensuring clarity of roles among different healthcare professionals can sometimes be a source of confusion or conflict.
The Future of Nursing Case Management
The landscape of healthcare is constantly evolving, and nursing case management is poised to adapt and grow to meet future demands. As the population ages, the prevalence of chronic diseases continues to rise, and healthcare systems move towards more value-based and patient-centered models, the role of the nurse case manager will become even more indispensable.
Technological advancements, such as telehealth, remote patient monitoring, and artificial intelligence, are creating new opportunities for case managers to extend their reach and enhance their efficiency. These tools can facilitate more frequent and proactive engagement with patients, identify early warning signs of deterioration, and provide data-driven insights to personalize care plans.
Furthermore, there is a growing recognition of the profound impact of social determinants of health on patient outcomes. Future case managers will likely be increasingly involved in addressing issues such as food insecurity, housing instability, and access to transportation, working collaboratively with social services and community organizations to create truly holistic care solutions.
The emphasis on population health management and preventative care will also shape the future of case management. Nurse case managers will play a vital role in identifying at-risk populations, implementing targeted interventions, and empowering individuals and communities to take greater ownership of their health.
Ultimately, the nursing case manager will remain a vital force in navigating the complexities of modern healthcare, ensuring that patients receive compassionate, coordinated, and effective care that promotes well-being and optimizes outcomes in an ever-changing healthcare environment.
