Neuro-ophthalmology is a specialized sub-discipline of ophthalmology and neurology that focuses on the intricate relationship between the visual system and the nervous system. It bridges the gap between these two complex fields, diagnosing and managing a wide array of conditions that affect vision through neurological pathways. These can include disorders of the optic nerve, brain, and muscles that control eye movement. Essentially, a neuro-ophthalmologist is a physician who has completed extensive training in both eye care and neurological disorders, allowing them to understand and treat visual problems that stem from the brain or the nerves connecting the eye to the brain.
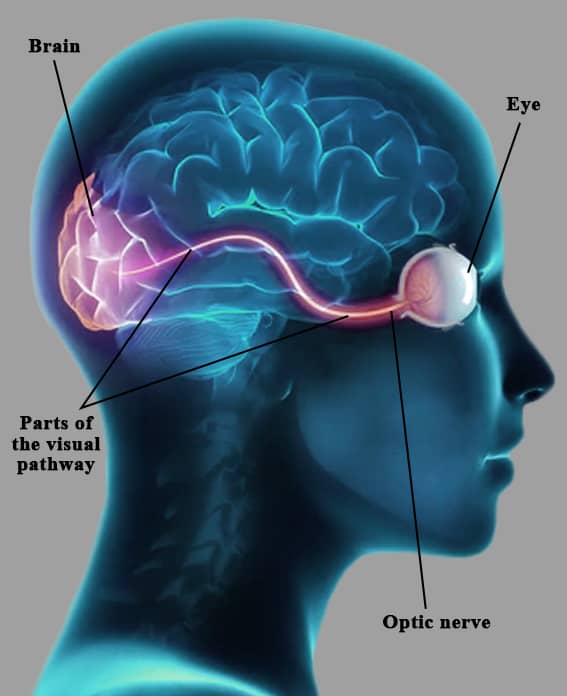
The visual system is a marvel of biological engineering, involving not only the eyes themselves but also a vast network of nerves and brain structures. Light enters the eye and is converted into electrical signals by the retina. These signals are then transmitted along the optic nerve to the brain, where they are processed to form images and allow us to perceive the world around us. Any disruption along this pathway, whether in the eye, the optic nerve, the brain’s visual cortex, or the control mechanisms for eye movements, can lead to visual disturbances. Neuro-ophthalmologists are uniquely equipped to unravel these complex connections and pinpoint the source of visual dysfunction.
Their expertise is crucial for patients presenting with symptoms such as sudden vision loss, double vision, blurred vision, blind spots, visual field defects, abnormal eye movements, and drooping eyelids. These symptoms, while seemingly originating in the eye, can often be indicators of more serious underlying neurological conditions like brain tumors, strokes, multiple sclerosis, or inflammatory diseases. Conversely, some neurological conditions can manifest with subtle or overt visual changes that are best evaluated by a neuro-ophthalmologist.
The Scope of Neuro-Ophthalmological Practice
The diagnostic arsenal of a neuro-ophthalmologist is diverse, encompassing detailed patient history, a thorough ophthalmological examination, and often, a comprehensive neurological assessment. They are skilled in interpreting the results of various specialized tests that help elucidate the cause of visual problems. This often involves understanding how specific anatomical structures in the visual pathway function and how their impairment can lead to distinct clinical presentations.
The Neuro-Ophthalmological Examination
A typical neuro-ophthalmological evaluation begins with a detailed history, delving into the patient’s symptoms, their onset, progression, and any associated neurological or systemic issues. This is followed by a meticulous eye exam, which includes visual acuity testing, color vision assessment, and evaluation of pupillary responses. A critical component is the assessment of visual fields, which can reveal blind spots or areas of reduced vision that a patient may not be consciously aware of. This is often done using perimetry, a test that maps the entire scope of vision.
Furthermore, the examination includes a funduscopic evaluation, where the doctor uses an ophthalmoscope to visualize the retina and the optic nerve head. Swelling of the optic nerve (papilledema), pallor (indicating nerve damage), or other abnormalities seen at the optic disc can be crucial clues to underlying neurological disease. Assessment of eye movements is also vital, looking for limitations, involuntary movements (nystagmus), or misalignment of the eyes (strabismus). Drooping of the eyelids (ptosis) can also be a significant finding.
Diagnostic Technologies and Tests
To further investigate suspected conditions, neuro-ophthalmologists utilize a range of advanced diagnostic technologies.
Imaging Techniques
- Magnetic Resonance Imaging (MRI): MRI is indispensable in neuro-ophthalmology. It provides detailed cross-sectional images of the brain and optic nerves, allowing visualization of tumors, inflammation, strokes, demyelination (as seen in multiple sclerosis), and structural abnormalities that can affect vision. Specialized MRI sequences can further enhance the detection of subtle lesions.
- Computed Tomography (CT) Scan: While MRI is often preferred for soft tissues, CT scans are useful for evaluating bony structures of the orbit and skull, detecting calcifications, and in emergent situations where MRI may not be readily available.
- Optical Coherence Tomography (OCT): OCT is a non-invasive imaging technique that provides high-resolution, cross-sectional views of the retina and the optic nerve head. It is invaluable for quantifying retinal nerve fiber layer thickness, detecting optic nerve swelling or atrophy, and monitoring disease progression.
Neurophysiological Tests
- Visual Evoked Potentials (VEPs): VEPs measure the electrical activity in the brain in response to visual stimuli. This test assesses the integrity of the visual pathways from the eye to the visual cortex of the brain, helping to identify delays or abnormalities in signal transmission that may not be apparent on routine examination.
- Electromyography (EMG) and Nerve Conduction Studies: In cases of suspected neuromuscular junction disorders affecting eye movements or eyelid function, these tests can help identify abnormalities in nerve and muscle function.
Other Specialized Tests
- Lumbar Puncture (Spinal Tap): Analysis of cerebrospinal fluid (CSF) can help diagnose inflammatory or infectious conditions affecting the central nervous system, such as meningitis or multiple sclerosis, which can indirectly impact vision.
- Blood Tests: A wide range of blood tests may be ordered to identify systemic inflammatory conditions, autoimmune diseases, infections, or nutritional deficiencies that can affect the visual system.
Common Conditions Managed by Neuro-Ophthalmologists
The breadth of conditions treated by neuro-ophthalmologists is extensive, covering a spectrum from common ailments with neurological underpinnings to rare and complex syndromes. Their expertise is sought when the cause of a visual symptom is unclear or when a visual problem is a manifestation of a broader neurological disorder.
Optic Nerve Disorders
The optic nerve is a common site for pathology impacting vision.
- Optic Neuritis: This is an inflammation of the optic nerve, often associated with multiple sclerosis. Symptoms typically include sudden vision loss, pain with eye movement, and decreased color vision.
- Ischemic Optic Neuropathy: This occurs when blood flow to the optic nerve is compromised, leading to sudden, painless vision loss. It can be anterior (affecting the optic disc) or posterior.
- Papilledema: Swelling of the optic nerve head due to increased intracranial pressure. This is a critical sign that requires prompt investigation into the cause of elevated pressure within the skull.
- Optic Nerve Atrophy: Degeneration of the optic nerve, which can result from various causes including trauma, inflammation, compression, or genetic conditions. It often leads to permanent vision loss.
- Toxic and Nutritional Optic Neuropathies: Certain medications, toxins, or nutritional deficiencies (e.g., vitamin B12 deficiency) can damage the optic nerve.
Disorders of Eye Movement and Eyelid Function
The intricate muscular and neural control of eye movements and eyelid position can be disrupted by neurological conditions.
- Nystagmus: Involuntary, repetitive rhythmic movements of the eyes. This can be congenital or acquired due to neurological lesions, inner ear problems, or certain medications.
- Diplopia (Double Vision): Occurs when the eyes are not properly aligned, leading to the perception of two images of a single object. Causes can range from cranial nerve palsies (affecting the nerves controlling eye muscles) to conditions affecting the neuromuscular junction (like Myasthenia Gravis) or brainstem lesions.
- Ptosis (Drooping Eyelid): Can be caused by damage to the nerve supplying the eyelid muscle, problems with the muscle itself, or neurological disorders like Myasthenia Gravis or Horner’s syndrome.
- Internuclear Ophthalmoplegia (INO): A specific type of eye movement disorder characterized by impaired adduction (inward movement) of one eye during horizontal gaze, often associated with demyelinating lesions in the brainstem, commonly seen in multiple sclerosis.
Visual Field Defects and Brain Lesions
The processing of visual information occurs in specific areas of the brain, and lesions in these regions can result in specific visual field deficits.
- Chiasmal Disorders: Lesions affecting the optic chiasm, where the optic nerves cross, can cause characteristic visual field defects, such as bitemporal hemianopia (loss of vision in the outer half of the visual field in both eyes), often caused by pituitary tumors.
- Cortical Visual Impairment: Damage to the visual cortex in the occipital lobes of the brain, resulting from stroke, trauma, or hypoxia, can lead to a variety of visual field deficits or even cortical blindness.
- Migraine with Aura: While a common condition, visual disturbances like flashing lights, zigzag lines, or blind spots (aura) preceding or accompanying a migraine headache fall under the purview of neuro-ophthalmology, especially when they are new or unusual.
Increased Intracranial Pressure
Conditions that lead to elevated pressure within the skull can have significant impacts on vision, primarily through papilledema.
- Pseudotumor Cerebri (Idiopathic Intracranial Hypertension): A condition characterized by increased intracranial pressure without a detectable tumor or other obvious cause. Papilledema is a hallmark sign, and if untreated, can lead to permanent vision loss.
- Brain Tumors: Tumors, whether within the brain or pressing on visual pathways, can cause a range of visual symptoms, including papilledema, visual field defects, and optic nerve compression.
The Collaborative Role and Future of Neuro-Ophthalmology
Neuro-ophthalmologists often work closely with other medical specialists, including neurologists, neurosurgeons, endocrinologists, and rheumatologists, to provide comprehensive care for their patients. This multidisciplinary approach is essential for managing complex conditions that involve multiple organ systems. For instance, a patient with suspected multiple sclerosis might be co-managed by a neuro-ophthalmologist for optic neuritis and a neurologist for their overall neurological condition. Similarly, a patient with a pituitary tumor causing visual deficits would involve a neuro-ophthalmologist, an endocrinologist, and potentially a neurosurgeon.
The field is constantly evolving with advancements in neuroimaging, neurophysiology, and our understanding of neurological diseases. The development of more sensitive diagnostic tools and targeted therapies promises to further improve outcomes for patients with neuro-ophthalmic conditions. As our knowledge of the brain-eye connection deepens, neuro-ophthalmology remains a vital specialty dedicated to preserving and restoring the precious gift of sight by unraveling the intricate dialogue between our eyes and our minds.
