Understanding SGPT and Hemolysis in Medical Diagnostics
The query “what does it mean when AST hemolyzed SGPT” points to a specific scenario encountered in medical laboratory testing, particularly when analyzing blood samples for liver function. To properly interpret this, we must first deconstruct the terms: SGPT, AST, and hemolysis.
SGPT: The Enzyme Formerly Known as ALT
SGPT, or serum glutamic-pyruvic transaminase, is an enzyme that was commonly used to assess liver health. In modern medical terminology, this enzyme is now more accurately referred to as ALT, or alanine transaminase. Both terms refer to the same enzyme, which plays a crucial role in amino acid metabolism. ALT is found in high concentrations within liver cells (hepatocytes). When liver cells are damaged or inflamed, ALT is released into the bloodstream, leading to elevated levels in blood tests. Therefore, ALT (or SGPT) is a key biomarker for detecting liver injury.
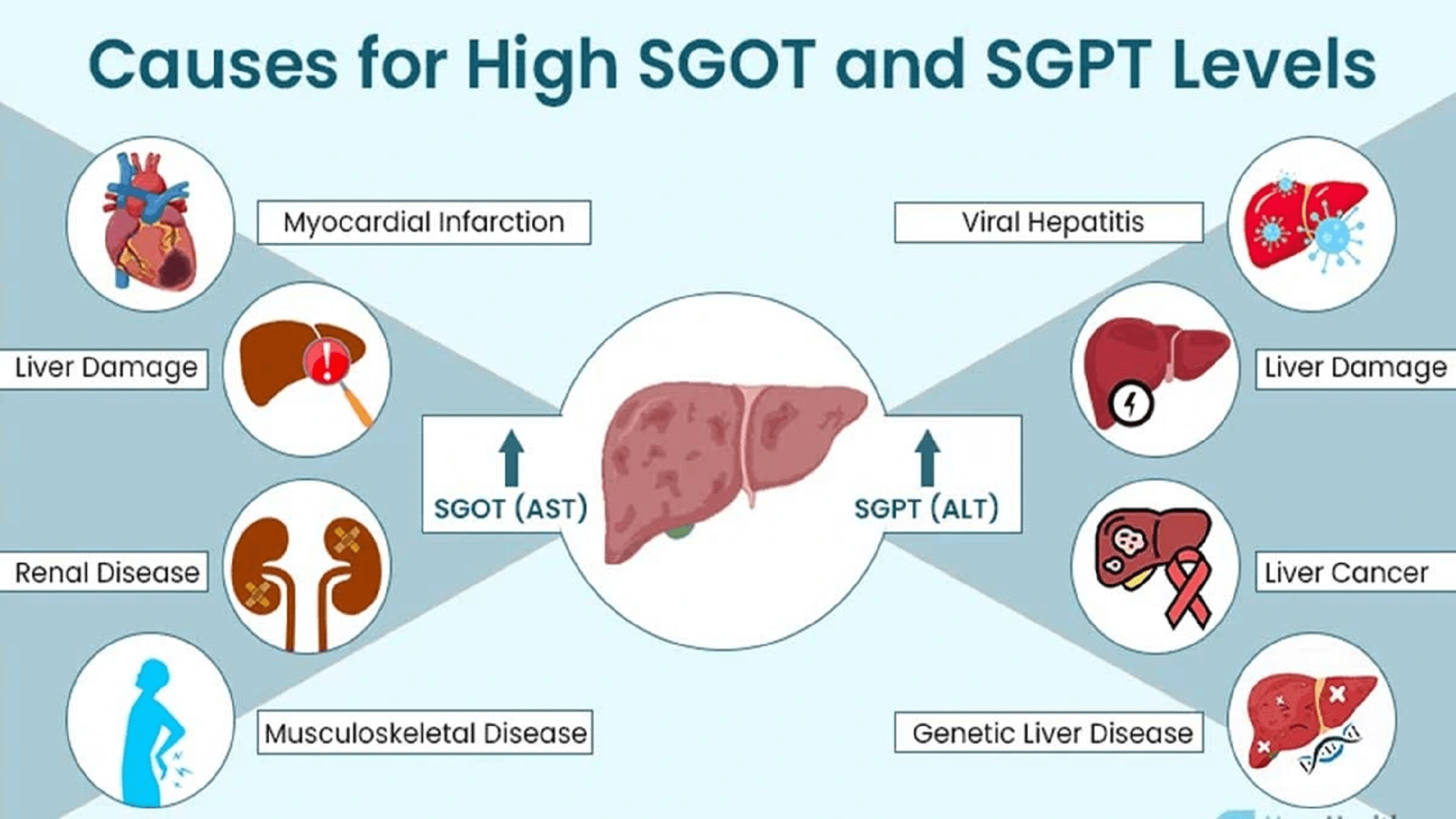
AST: Another Liver Enzyme Indicator
AST, or aspartate transaminase, is another enzyme that is also used to evaluate liver function. Like ALT, AST is found in liver cells, but it is also present in other tissues, including the heart, skeletal muscle, kidneys, and brain. While elevated AST levels can indicate liver damage, they can also be indicative of issues in these other organs. Because AST is found in multiple tissues, ALT is often considered a more specific marker for liver injury than AST. However, the ratio of AST to ALT (the AST/ALT ratio) can provide additional diagnostic clues. For instance, a significantly higher AST than ALT level might suggest a cause of liver damage that also affects other organs, or it could point to alcoholic liver disease.
Hemolysis: The Red Blood Cell Predicament
Hemolysis refers to the rupture or destruction of red blood cells, leading to the release of their contents into the surrounding plasma or serum. This can occur both in vivo (within the body) and in vitro (in a collected blood sample).
- In Vivo Hemolysis: This can be a symptom of various medical conditions, such as autoimmune disorders, infections, or genetic red blood cell abnormalities. When hemolysis occurs within the body, it can lead to anemia (a deficiency of red blood cells) and hyperbilirubinemia (an excess of bilirubin, a byproduct of red blood cell breakdown, which can cause jaundice).
- In Vitro Hemolysis: This is a common pre-analytical problem in laboratory testing. It occurs during blood collection, sample handling, or processing. Factors contributing to in vitro hemolysis include:
- Difficult blood draws: Vigorous shaking or frothing of the blood during collection.
- Improper needle size: Using too small a needle can cause red blood cells to shear as they pass through.
- Excessive squeezing of the puncture site: This can force red blood cells into the collection tube under pressure.
- Delayed processing: Allowing the blood to sit for too long before separation of serum or plasma.
- Extreme temperatures: Freezing or excessive heat can damage red blood cells.
- Traumatic centrifugation: High-speed or prolonged centrifugation can lyse red blood cells.
The Impact of Hemolysis on SGPT (ALT) and AST Measurements
When a blood sample undergoes hemolysis, the results of certain laboratory tests can be significantly affected, and this is where the “hemolyzed SGPT” or “hemolyzed AST” indication comes into play.
Why Hemolysis Matters for SGPT and AST
Both SGPT (ALT) and AST are enzymes that are also present in relatively high concentrations within red blood cells. This is a critical point. While their primary diagnostic relevance comes from their release from damaged liver cells into the bloodstream, their presence within red blood cells means that any process that breaks open these cells will release these enzymes into the serum or plasma.
Therefore, in vitro hemolysis can artificially inflate the measured levels of SGPT and AST in a blood sample. If a lab technician notes that a sample is “hemolyzed,” it means that red blood cells have broken down in the collected specimen. Consequently, the SGPT and AST values obtained from such a sample are unreliable because they do not solely reflect liver function; they also reflect the enzyme released from the lysed red blood cells.
Interpreting “Hemolyzed SGPT” or “Hemolyzed AST”
When a laboratory report indicates “hemolyzed SGPT” or “hemolyzed AST,” it is not an interpretation of your liver health. Instead, it is a technical note about the quality of the blood sample that was tested. The laboratory is informing the clinician that the SGPT (ALT) and/or AST results from that specific sample are likely to be falsely elevated due to the presence of hemolysis.
- False Positives: A hemolyzed sample can lead to a falsely elevated SGPT or AST reading, potentially suggesting liver damage where none exists. This can cause unnecessary anxiety for the patient and lead to further, potentially invasive, diagnostic procedures.
- Unreliable Results: Because the results are compromised, they cannot be used for accurate diagnosis or monitoring of liver disease.
What Happens Next?
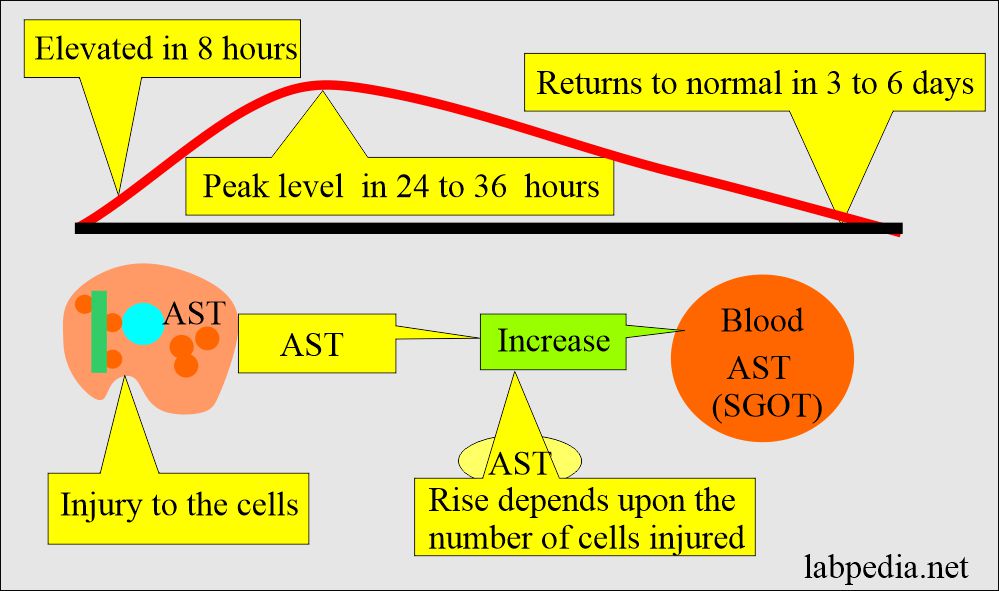
When a sample is flagged as hemolyzed, the standard procedure is to reject the results and request a new blood sample. The clinician will then need to re-draw blood from the patient and have it tested again, this time ensuring that the sample is collected and handled appropriately to prevent hemolysis. It is important for the patient to cooperate with the phlebotomist and inform them if they have experienced issues with blood draws in the past.
Causes and Prevention of In Vitro Hemolysis
Understanding the mechanisms behind in vitro hemolysis is crucial for both healthcare providers and patients to ensure accurate laboratory results.
Common Causes of In Vitro Hemolysis
As mentioned earlier, in vitro hemolysis is a prevalent issue in clinical laboratories, stemming from various points in the sample handling process. Some of the most common culprits include:
- Difficult Venipuncture: Many factors can contribute to a difficult blood draw. This includes patients with small or deep veins, those who are dehydrated, or those who have undergone numerous previous venipunctures, making their veins less prominent. In such cases, the phlebotomist might need to apply more suction or attempt multiple venipunctures, increasing the risk of trauma to the red blood cells.
- Improper Syringe or Needle Usage: Using a needle that is too small for the vein can cause shearing forces on red blood cells as they are drawn into the collection tube. Similarly, if blood is collected using a syringe and then forcefully injected into a collection tube without proper technique, it can lead to hemolysis.
- Excessive Tourniquet Application: While a tourniquet is used to make veins more visible and palpable, leaving it on for too long (typically more than one minute) can cause changes in the blood composition, including red blood cell fragility, and increase the risk of hemolysis.
- Agitation and Mixing: Aggressively shaking or mixing the collected blood can physically rupture red blood cells. While some inversion is necessary to mix anticoagulant with blood in certain tubes, this should be done gently.
- Delayed or Improper Serum/Plasma Separation: Blood is typically centrifuged to separate the red blood cells from the serum (when a clot activator is used) or plasma (when an anticoagulant is present). If this separation is delayed for too long, or if the centrifugation process is too vigorous or prolonged, it can lead to red blood cell lysis.
- Temperature Extremes: Exposing the blood sample to very cold temperatures (freezing) or excessive heat can damage the integrity of red blood cell membranes.
Strategies for Preventing Hemolysis
Preventing hemolysis is a shared responsibility. Phlebotomists play a critical role in sample collection, but patient awareness and cooperation can also be beneficial.
- Phlebotomist Training and Technique: Rigorous training in proper venipuncture techniques, including vein selection, needle insertion angles, and appropriate use of collection devices (syringes vs. vacuum tubes), is paramount. Phlebotomists should be adept at identifying challenging veins and employing techniques to minimize trauma.
- Using Appropriate Collection Devices: Employing the correct needle gauge for the patient’s vein size and using vacuum tubes with the appropriate anticoagulant and fill volume are essential.
- Gentle Handling of Samples: All blood samples should be handled gently. Shaking or vigorous mixing should be avoided. Inversion of tubes with anticoagulants should be done gently but thoroughly.
- Timely Processing: Laboratory protocols should emphasize prompt separation of serum or plasma from the red blood cells after collection. Adhering to recommended centrifugation speeds and times is crucial.
- Patient Preparation and Communication: Patients can contribute by staying hydrated, which can make veins easier to access. They should also inform the phlebotomist of any previous difficulties with blood draws or if they feel anxious, as this can sometimes lead to a more challenging venipuncture.
- Quality Control in Laboratories: Laboratories implement strict quality control measures to monitor sample integrity. This includes visual inspection of samples for signs of hemolysis and having protocols for rejecting hemolyzed specimens.
Clinical Significance Beyond the Technical Anomaly
While “hemolyzed SGPT” is primarily a technical issue indicating sample quality, understanding why this artifact is so problematic delves into the clinical significance of SGPT (ALT) and AST measurements.
SGPT (ALT) and AST as Liver Health Indicators
As discussed, SGPT (ALT) and AST are vital enzymes for assessing liver health. Elevated levels in the blood are often the first sign of liver damage, which can stem from a wide array of conditions, including:
- Hepatitis: Viral infections (Hepatitis A, B, C), autoimmune hepatitis, or drug-induced hepatitis.
- Cirrhosis: Scarring of the liver due to chronic liver disease.
- Fatty Liver Disease: Non-alcoholic fatty liver disease (NAFLD) and alcoholic fatty liver disease.
- Medication Side Effects: Many medications can be toxic to the liver.
- Alcohol Abuse: Excessive alcohol consumption is a major cause of liver damage.
- Bile Duct Obstruction: Blockages in the bile ducts can lead to liver inflammation.
- Ischemic Hepatitis: Liver damage due to insufficient blood supply.
The degree of elevation, along with the AST/ALT ratio, can provide clues about the underlying cause and severity of the liver condition. For example, a marked elevation might indicate acute injury, while persistently mild elevations could suggest a chronic, indolent process.
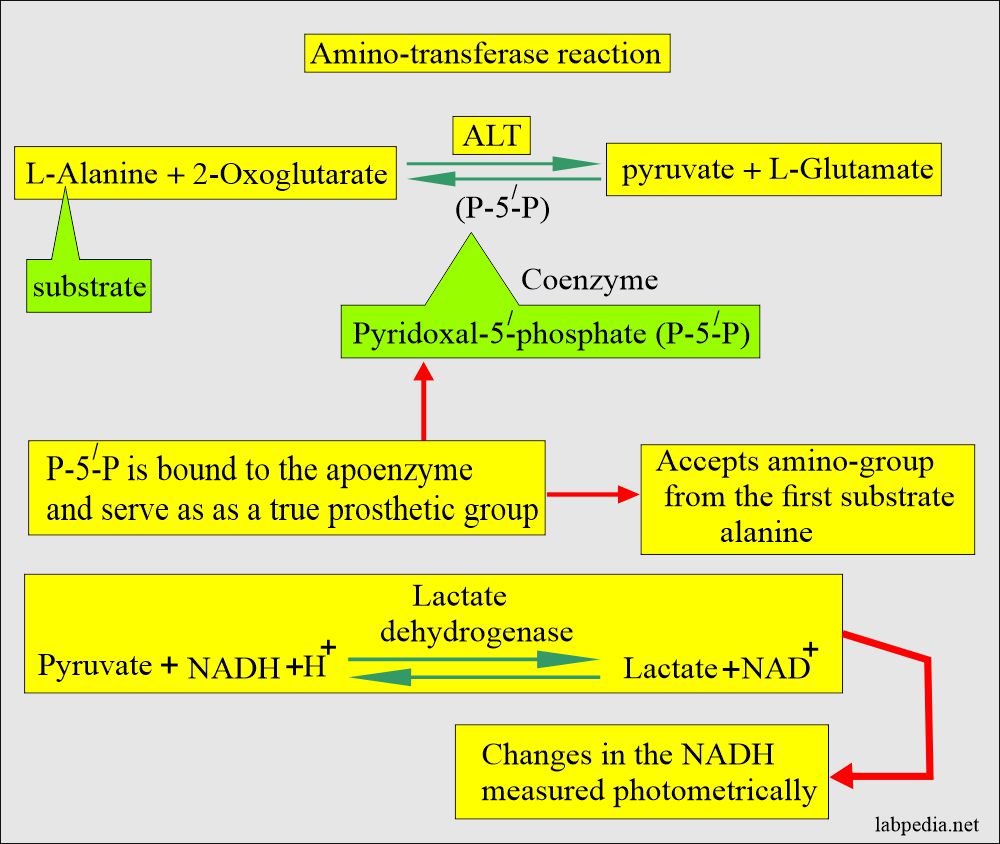
The Danger of Misinterpretation
The presence of in vitro hemolysis can drastically skew these interpretations:
- False Alarm: A falsely elevated SGPT/AST due to hemolysis can lead to unnecessary investigations, anxiety for the patient, and potentially costly medical procedures to rule out liver disease.
- Masking of Underlying Issues: While less common, severe in vitro hemolysis might, in rare circumstances, dilute other analytes, potentially masking other critical findings. However, the primary concern with hemolyzed SGPT/AST is the artificial elevation.
- Delayed Diagnosis: If a hemolyzed sample is not identified and re-tested, a true underlying liver issue might be missed, or its progression might not be accurately monitored, leading to a delay in appropriate treatment.
Therefore, the laboratory’s flagging of a hemolyzed sample is a crucial quality control step. It ensures that the results reported to the clinician are accurate and can be reliably used to make informed medical decisions. When you encounter an indication of “hemolyzed SGPT” or “hemolyzed AST,” it is a signal that the test needs to be repeated, rather than an immediate diagnosis of a liver problem. The focus then shifts to ensuring a pristine sample for accurate assessment.
