Spotting after your period, often referred to as post-period spotting or intermenstrual bleeding, is a common occurrence that can cause concern for many individuals. While it can sometimes be a sign of an underlying medical condition, it is frequently benign and can be attributed to various physiological factors. Understanding the potential causes, associated symptoms, and when to seek medical advice is crucial for managing this type of bleeding. This article delves into the intricacies of spotting after menstruation, exploring its nuances within the realm of gynecological health.
Understanding the Menstrual Cycle and Post-Period Bleeding
The menstrual cycle is a complex interplay of hormones that prepares a woman’s body for potential pregnancy. It typically involves the shedding of the uterine lining (endometrium), resulting in menstruation, followed by ovulation and the thickening of the endometrium in anticipation of implantation. Variations in hormone levels, structural changes within the uterus and cervix, and external factors can all influence bleeding patterns, including spotting that occurs outside of the expected menstrual flow.
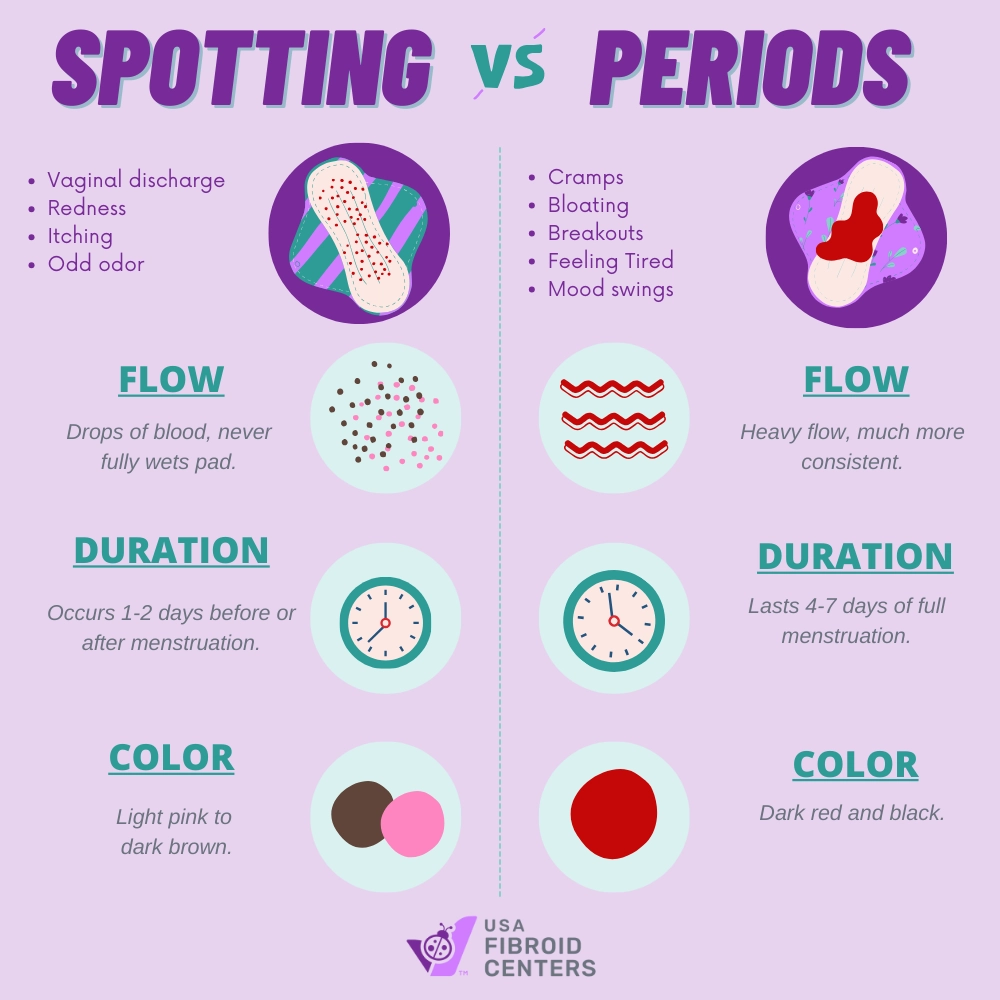
Hormonal Fluctuations
Hormonal imbalances are a primary driver of irregular bleeding, including spotting after a period. The delicate balance between estrogen and progesterone is essential for regulating the menstrual cycle. Disruptions to this balance, whether due to stress, significant weight changes, polycystic ovary syndrome (PCOS), or perimenopause, can lead to the uterine lining shedding irregularly.
Estrogen Dominance
An imbalance where estrogen levels are disproportionately high compared to progesterone can lead to a thickened endometrium. When this thickened lining is not adequately supported by progesterone for shedding in a complete menstrual flow, small fragments may break away, resulting in spotting. This can occur after the main period has ended as the body attempts to re-establish hormonal equilibrium.
Progesterone Withdrawal
Conversely, a sudden drop in progesterone levels can also trigger the shedding of the uterine lining. If this withdrawal happens prematurely or incompletely after the period, it can manifest as spotting. This is particularly common during perimenopause, as hormone levels become more erratic.
Uterine and Cervical Factors
The structural health of the uterus and cervix plays a significant role in menstrual regularity and the occurrence of spotting. Conditions affecting these organs can lead to abnormal bleeding patterns.
Cervical Irritation and Polyps
The cervix is a sensitive area, and irritation can lead to spotting. This irritation can stem from various sources, including sexual intercourse, vigorous physical activity, or vaginal infections. Cervical polyps, which are small, non-cancerous growths on the cervix, can also bleed easily, especially after intercourse or straining. These polyps are often friable, meaning they can rupture and bleed with minimal provocation.
Endometrial Polyps and Fibroids
Within the uterus, endometrial polyps (growths in the uterine lining) and uterine fibroids (non-cancerous tumors in the uterine wall) can disrupt the normal shedding of the endometrium. These growths can cause irregular bleeding, including spotting after a period. Fibroids, in particular, can alter the shape of the uterine cavity and increase blood flow to the uterine lining, leading to heavier or more prolonged bleeding and spotting.
Endometriosis and Adenomyosis
Endometriosis, a condition where uterine-like tissue grows outside the uterus, and adenomyosis, where this tissue grows within the uterine wall, can also contribute to spotting. These conditions can cause inflammation and abnormal tissue growth, leading to irregular bleeding patterns, including spotting between periods or after menstruation has officially finished. The hormonal fluctuations of the cycle can cause these aberrant tissues to bleed, mimicking menstrual flow.
Other Potential Causes of Post-Period Spotting
Beyond hormonal and structural issues, several other factors can contribute to spotting after menstruation.
Ovulation
While ovulation typically occurs mid-cycle, some individuals experience light spotting around the time of ovulation. This is often referred to as “mittelschmerz” and is thought to be caused by the rupture of the follicle in the ovary releasing the egg. The small amount of bleeding from the ruptured follicle can sometimes be observed as spotting.
Ovulation Spotting (Intermenstrual Bleeding)
This type of spotting occurs roughly mid-cycle, between the end of one period and the start of the next. While not strictly “after period” spotting, it is closely related to the menstrual cycle’s hormonal shifts. The drop in estrogen that can occur just before ovulation can sometimes cause a slight shedding of the uterine lining, leading to light spotting.
Intrauterine Devices (IUDs)
For individuals using an IUD as a form of contraception, spotting after their period can be a common side effect, particularly in the initial months of use. IUDs can cause changes in the uterine lining and cervix, leading to irregular bleeding. While this often settles down over time, persistent spotting should be discussed with a healthcare provider.
Medications
Certain medications can influence menstrual patterns and lead to spotting. Hormonal contraceptives, such as birth control pills, patches, or injections, can cause spotting, especially when starting or stopping them, or if doses are missed. Blood-thinning medications can also increase the likelihood of bleeding, including spotting.
Pregnancy-Related Causes
Even if pregnancy is not suspected, it’s essential to consider pregnancy-related causes for any spotting that occurs after a period, especially if there’s a possibility of conception.
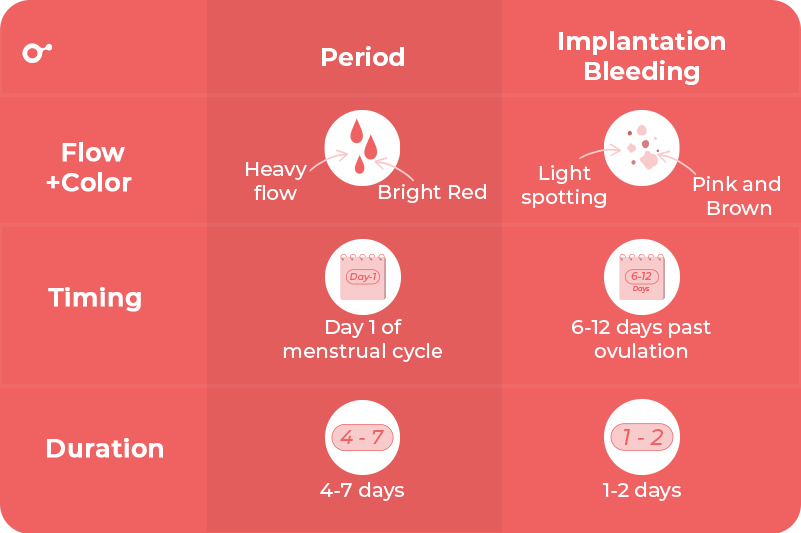
Implantation Bleeding
Early in pregnancy, a fertilized egg may implant in the uterine lining, causing a small amount of bleeding known as implantation bleeding. This typically occurs about 10-14 days after conception and can be mistaken for a light period or spotting after a period.
Ectopic Pregnancy
An ectopic pregnancy, where a fertilized egg implants outside the uterus, is a serious medical emergency. It can cause spotting or bleeding, often accompanied by pelvic pain. Any persistent or heavy spotting, especially with pain, warrants immediate medical attention.
Miscarriage
Early miscarriage can also present with spotting or bleeding. This can occur even before a person realizes they are pregnant.
When to Seek Medical Advice
While spotting after a period is often harmless, it’s crucial to be aware of when it might indicate a more serious issue. Consulting a healthcare professional is recommended in the following situations:
Persistent or Heavy Bleeding
If the spotting is heavy, lasts for more than a few days, or occurs frequently, it’s essential to get it checked. Heavy bleeding can lead to anemia and may signal an underlying condition.
Associated Symptoms
Spotting accompanied by other symptoms such as severe pelvic pain, fever, unusual vaginal discharge, pain during intercourse, or dizziness warrants prompt medical evaluation. These symptoms can indicate infections, ectopic pregnancy, or other serious gynecological problems.
Changes in Menstrual Pattern
A significant and persistent change in your menstrual cycle, including spotting after periods, should be discussed with your doctor. This could be a sign of hormonal imbalances, PCOS, or perimenopause.
Post-Menopausal Bleeding
Any bleeding or spotting after menopause (defined as 12 consecutive months without a period) is considered abnormal and requires immediate medical attention, as it can be a sign of endometrial cancer.
Concerns About Pregnancy
If there’s any possibility of pregnancy, and you experience spotting, it’s important to consult your doctor to rule out complications like ectopic pregnancy or miscarriage.
Diagnosis and Management
A healthcare provider will typically perform a thorough medical history and physical examination, including a pelvic exam. Depending on the suspected cause, further diagnostic tests may be recommended:
Pelvic Exam and Pap Smear
This allows for visual inspection of the cervix and vagina for any abnormalities, infections, or signs of irritation.
Ultrasound
A transvaginal or abdominal ultrasound can help visualize the uterus, ovaries, and fallopian tubes, identifying structural issues like fibroids, polyps, or ovarian cysts.
Blood Tests
Hormone levels can be checked to assess for imbalances, and pregnancy tests can rule out or confirm pregnancy.

Biopsy
If endometrial polyps or other uterine abnormalities are suspected, a biopsy of the uterine lining may be performed to examine the tissue for any cancerous or precancerous changes.
The management of spotting after a period depends entirely on the underlying cause.
- Hormonal Imbalances: May be treated with hormone therapy, lifestyle adjustments, or medications to regulate the cycle.
- Cervical or Uterine Polyps/Fibroids: May require surgical removal depending on their size, location, and the severity of symptoms.
- Infections: Treated with appropriate antibiotics or antifungal medications.
- Contraception-Related: Adjustment of the contraceptive method or patience for the body to adapt.
- Pregnancy-Related Issues: Require specific medical management based on the diagnosis.
In conclusion, spotting after a period can have a wide range of causes, from minor hormonal shifts to more significant medical conditions. While it is often a normal physiological event, it is crucial to monitor your symptoms and consult a healthcare professional if you experience persistent, heavy, or concerning bleeding, especially when accompanied by other symptoms. Early diagnosis and appropriate management can ensure your gynecological health and well-being.
