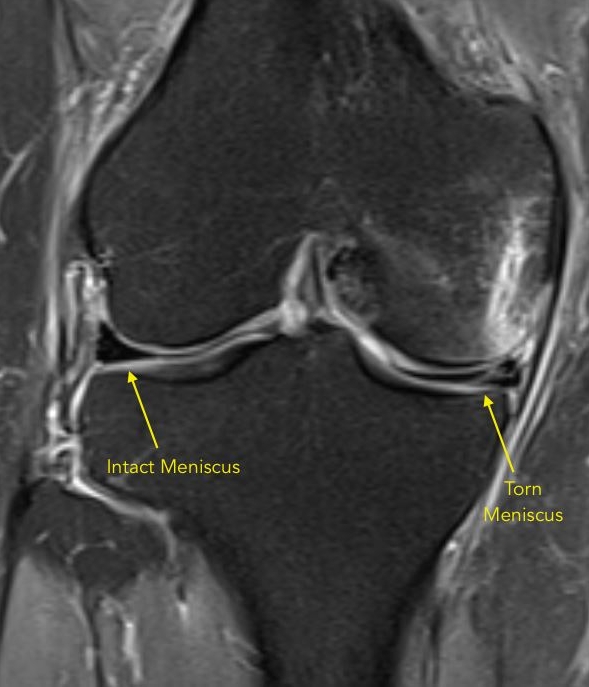
The meniscus, a C-shaped piece of cartilage in the knee, acts as a shock absorber between the thighbone (femur) and shinbone (tibia). Tears in this crucial structure are common, particularly among athletes and individuals with degenerative knee conditions. Diagnosing these tears often relies heavily on Magnetic Resonance Imaging (MRI), a powerful diagnostic tool that offers detailed cross-sectional views of the knee’s internal anatomy. Understanding what a meniscus tear looks like on an MRI is vital for both clinicians and patients to grasp the extent of the injury and inform treatment decisions. This article delves into the visual characteristics of meniscus tears as depicted by MRI, focusing on various imaging sequences and common tear patterns.
The Fundamentals of MRI Imaging for Knee Pathology
MRI utilizes strong magnetic fields and radio waves to generate detailed images of soft tissues. For knee imaging, specific MRI sequences are employed to highlight different tissue characteristics and pathological changes. The most crucial sequences for visualizing the meniscus are those that emphasize fluid and soft tissue contrast, allowing tears to be distinguished from healthy meniscal tissue.
Key MRI Sequences for Meniscus Visualization
-
Proton Density (PD) Weighted Images: These sequences are highly sensitive to fluid. In a healthy meniscus, which is composed of densely packed collagen fibers with minimal free water, it appears as a uniformly dark, triangular structure. PD-weighted images are excellent for detecting fluid accumulation, which is often present in and around a torn meniscus. This fluid can appear as bright (hyperintense) signals within the normally dark meniscus.
-
T2 Weighted Images: Similar to PD-weighted images, T2-weighted sequences are also sensitive to fluid. However, they provide even greater contrast between fluid and other tissues. In T2-weighted images, fluid appears bright (hyperintense). Healthy meniscal tissue should remain dark. The presence of bright signals within the meniscus on T2-weighted images is a strong indicator of a tear. The extent and location of these bright signals can help characterize the type and severity of the tear.
-
Fat-Suppressed Sequences (e.g., PD FS, T2 FS): These sequences are often used in conjunction with standard PD and T2-weighted images. Fat suppression techniques reduce the signal intensity from fatty tissues, thereby enhancing the visibility of fluid and other non-fatty structures. This is particularly useful in the knee because the surrounding tissues are rich in fat. By suppressing the fat signal, any bright signal within the meniscus on fat-suppressed sequences is more clearly identified as being indicative of fluid within a tear.
Understanding Signal Intensity
The appearance of tissues on MRI is described by their signal intensity – how bright or dark they appear on the image.
- Hypointense: A dark signal, typically representing healthy, dense tissue like intact meniscal fibers.
- Hyperintense: A bright signal, typically representing fluid or edema (swelling).
In a healthy meniscus, all signal intensity should be uniformly hypointense (dark) on all sequences, especially PD and T2 weighted images. The presence of focal or diffuse hyperintensity within the substance of the meniscus is the hallmark of a tear.
Identifying Meniscus Tears on MRI: Classic Appearances
The way a meniscus tear manifests on MRI depends on its type, location, and severity. Radiologists look for specific patterns of signal abnormality within the meniscal fibrocartilage.
Grade of Meniscal Signal Abnormality
A grading system is often used to describe the extent of signal abnormality within the meniscus, which may or may not directly correlate with a definitive tear:
-
Grade 1: Intrasubstance foci of increased signal intensity that do not extend to the meniscal surface. This is often considered a degenerative change rather than a frank tear and represents microscopic changes or edema within the tissue. These signals are typically small and rounded.
-
Grade 2: Linear or wedge-shaped increased signal intensity within the meniscus that does not involve the articular surface. This suggests a more significant intrasubstance tear or degeneration, where the abnormal signal extends in a linear fashion.
-
Grade 3: A tear is definitively identified when the abnormal signal intensity extends to either the superior or inferior articular surface of the meniscus, or both. This means there is a communication of abnormal signal (fluid) from within the meniscus to the joint surface, indicating a full-thickness tear.
It is important to note that Grade 1 and Grade 2 signal abnormalities can sometimes represent degenerative changes rather than a tear that would cause mechanical symptoms. However, Grade 3 signal is unequivocally indicative of a meniscal tear.
Common Tear Patterns and Their MRI Depictions
Meniscus tears can occur in various configurations, each with characteristic appearances on MRI:
-
Radial Tears: These tears run perpendicular to the long axis of the meniscus, extending from the inner margin to the outer margin or vice versa. On MRI, they appear as a linear zone of hyperintensity extending from the free edge towards the periphery. In the sagittal view, they can look like a small, bright line cutting across the meniscus. In the coronal view, they are often best seen as a discontinuity or a bright line extending from the inner to the outer border of the meniscus.
-
Longitudinal Tears (or Vertical Tears): These tears run parallel to the long axis of the meniscus. They are the most common type of meniscal tear. On MRI, a longitudinal tear appears as a linear zone of hyperintensity that runs from the anterior to the posterior horn of the meniscus, or a portion thereof. In sagittal images, a longitudinal tear can be seen as a bright line extending along the length of the meniscus. If the tear is significant enough to displace a fragment of the meniscus, it can lead to a “bucket-handle” tear.
-
Bucket-Handle Tears: This is a severe form of longitudinal tear where a large fragment of the meniscus, typically the posterior horn, is torn and displaced into the intercondylar notch of the knee. On MRI, this is characterized by a significant defect in the posterior horn with a displaced fragment seen anteriorly, often appearing as a linear or curvilinear structure within the intercondylar notch, appearing bright on T2-weighted images. The remaining portion of the posterior horn may appear small or absent.
-
Oblique Tears: These tears run at an angle to the long axis of the meniscus. They often originate from the inner margin and extend towards the outer margin. On MRI, they present as linear hyperintensity that is not strictly parallel or perpendicular to the meniscal fibers.
-
Horizontal Tears: These tears run parallel to the articular surfaces, dividing the meniscus into superior and inferior portions. On MRI, they appear as a horizontal line of hyperintensity within the meniscus. These can sometimes be associated with degenerative changes and may not always extend to the articular surface.
-
Complex Tears: These tears involve combinations of different tear patterns, such as radial and longitudinal components. They can be challenging to fully delineate and often present with extensive areas of abnormal signal intensity.
Beyond the Signal: Additional MRI Findings in Meniscal Tears
While abnormal signal intensity is the primary indicator of a meniscus tear, other findings on MRI can support the diagnosis and provide crucial information about the extent of associated pathology.
Meniscal Displacement and Extrusion
In cases of significant tears, particularly bucket-handle tears, a portion of the meniscus can become displaced. On MRI, this is visualized as the abnormal meniscal fragment occupying a different position within the joint than expected for intact meniscal tissue. Meniscal extrusion, where the entire meniscus appears to bulge or slide outwards from its normal position, can also be observed in some degenerative or traumatic tears, often seen best on coronal images.
Associated Knee Pathology
Meniscus tears rarely occur in isolation. MRI is invaluable for identifying associated injuries that can significantly impact treatment and prognosis. Common co-existing pathologies include:
-
Ligamentous Injuries: Tears of the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) are frequently associated with meniscal tears. MRI can clearly depict the integrity of these ligaments.
-
Articular Cartilage Damage: The smooth cartilage covering the ends of the bones can be damaged (chondral defects) or wear away (osteoarthritis). Abnormal signal intensity or thinning of the articular cartilage adjacent to the torn meniscus is readily apparent on MRI.
-
Bone Bruises (Bone Marrow Edema): Impact injuries, often associated with meniscus tears, can cause edema within the bone marrow. These appear as areas of T2 hyperintensity on fat-suppressed sequences.
-
Cysts: Parameniscal cysts are fluid collections that can form along the periphery of a torn meniscus, particularly in the medial meniscus. These appear as well-defined, T2 hyperintense cystic structures adjacent to the meniscus.
Degenerative Changes
It is crucial to differentiate traumatic tears from degenerative tears. Degenerative changes in the meniscus are common with aging and can include thinning, fraying, and signal abnormalities that may not represent a mechanically significant tear. MRI can help identify these subtle changes, often characterized by diffuse, low-grade signal abnormalities and thinning of the meniscal body. The presence of osteoarthritis, including joint space narrowing and osteophytes, often accompanies degenerative meniscal tears.
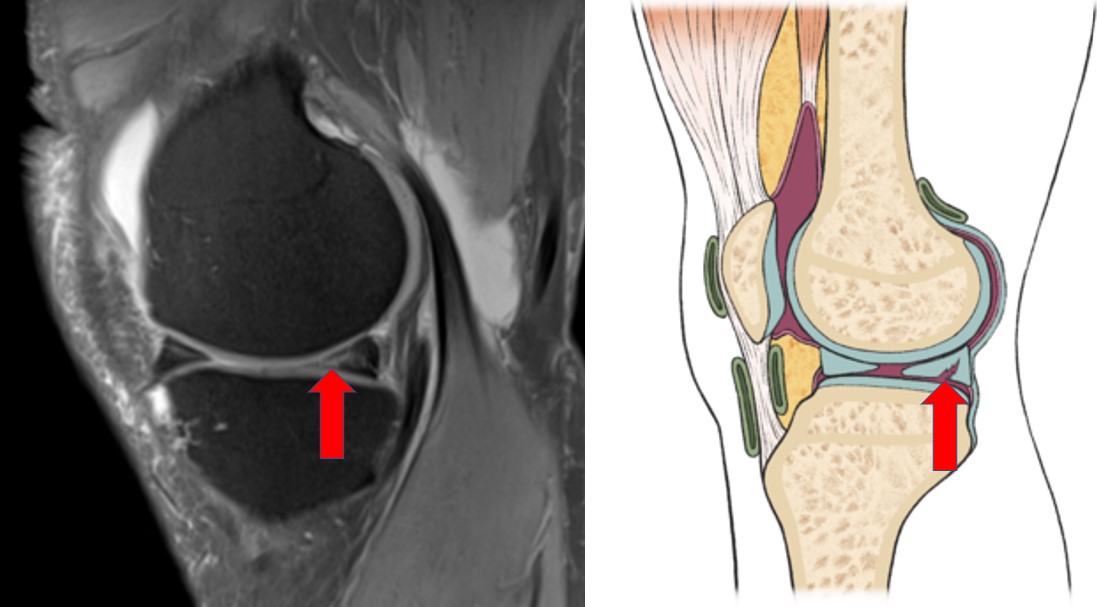
Clinical Correlation: The Importance of Integrating MRI Findings with Symptoms
While MRI is a powerful diagnostic tool, it is essential to remember that it visualizes anatomical changes. The interpretation of an MRI report must always be correlated with the patient’s clinical presentation, including the mechanism of injury, location and nature of pain, swelling, and mechanical symptoms like locking or catching. A significant meniscal tear seen on MRI may be asymptomatic in some individuals, particularly if it represents a chronic degenerative change. Conversely, subtle meniscal abnormalities on MRI might correlate with significant pain and functional limitation in others. Therefore, the radiologist’s report, combined with the orthopedic surgeon’s physical examination and patient history, forms the basis for an accurate diagnosis and appropriate management plan.