Hormone concentrations within the body are not static, chaotic fluctuations. Instead, they are meticulously regulated by a complex interplay of physiological processes, with the endocrine system acting as the central conductor. While numerous factors can influence hormone levels, the ultimate control over their synthesis, release, and degradation, and thus their circulating concentrations, rests primarily with intricate feedback mechanisms and the precise needs of target tissues. Understanding these regulatory pathways is crucial to comprehending human physiology and the basis for many medical conditions.
The Hypothalamic-Pituitary Axis: The Master Regulator
At the apex of this regulatory hierarchy lies the hypothalamic-pituitary axis (HPA axis), a sophisticated control center that governs a vast array of endocrine functions. The hypothalamus, a small but vital region in the brain, acts as the link between the nervous system and the endocrine system. It produces releasing hormones and inhibiting hormones that directly influence the pituitary gland, a pea-sized structure located at the base of the brain.
The Hypothalamus: Sensing and Signaling
The hypothalamus constantly monitors the body’s internal environment, receiving signals related to temperature, nutrient levels, stress, and even the circadian rhythm. Based on this sensory input, it synthesizes and releases specialized hormones that travel through a portal system to the anterior pituitary gland. For example, corticotropin-releasing hormone (CRH) from the hypothalamus stimulates the anterior pituitary to release adrenocorticotropic hormone (ACTH). Similarly, gonadotropin-releasing hormone (GnRH) stimulates the release of follicle-stimulating hormone (FSH) and luteinizing hormone (LH), while thyrotropin-releasing hormone (TRH) triggers the release of thyroid-stimulating hormone (TSH).
The Pituitary Gland: The Central Command
The pituitary gland, often referred to as the “master gland,” is divided into two lobes: the anterior pituitary and the posterior pituitary. The anterior pituitary, as mentioned, produces and secretes a range of tropic hormones that target other endocrine glands. These tropic hormones, in turn, stimulate these peripheral glands to produce and release their own hormones. The posterior pituitary, on the other hand, does not synthesize hormones but stores and releases hormones produced by the hypothalamus, namely antidiuretic hormone (ADH) and oxytocin. The precise release of these pituitary hormones is tightly controlled by the hypothalamus, ensuring that the correct signals are sent to downstream endocrine organs.
Peripheral Endocrine Glands: The Effectors
The tropic hormones from the anterior pituitary travel through the bloodstream to specific target endocrine glands. The adrenal glands, for instance, are stimulated by ACTH to produce cortisol, a key hormone in stress response and metabolism. The thyroid gland, under the influence of TSH, produces thyroid hormones (T3 and T4), which regulate metabolism. The gonads (testes and ovaries) are stimulated by FSH and LH to produce sex hormones like testosterone, estrogen, and progesterone, essential for reproduction and secondary sexual characteristics. The pancreas, regulated by blood glucose levels and other hormonal signals, releases insulin and glucagon, critical for glucose homeostasis.
Negative Feedback: The Primary Control Mechanism
The most pervasive and critical mechanism controlling hormone concentrations is negative feedback. This sophisticated system ensures that hormone levels remain within a narrow, optimal range. In a negative feedback loop, the product of a hormonal pathway inhibits the pathway’s further activity.
How Negative Feedback Works
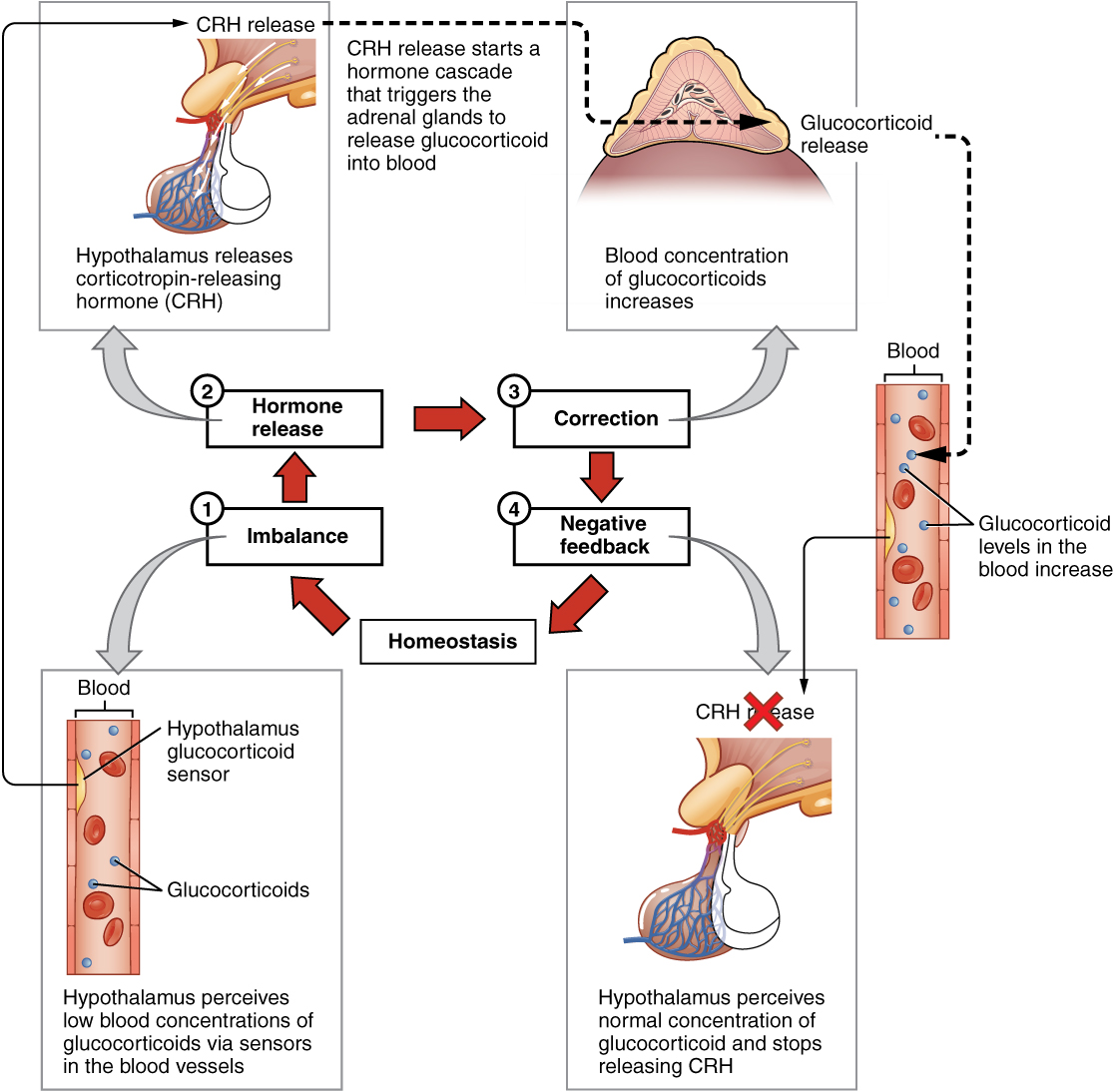
When a target endocrine gland releases its hormone in response to stimulation from the pituitary, this peripheral hormone then circulates throughout the body. High levels of this peripheral hormone will then exert an inhibitory effect on both the hypothalamus and the pituitary gland. This inhibition can manifest in several ways: it can reduce the secretion of releasing hormones from the hypothalamus, decrease the release of tropic hormones from the pituitary, or even reduce the sensitivity of the target gland to stimulation.
For example, when cortisol levels rise in the blood, they suppress the release of CRH from the hypothalamus and ACTH from the pituitary. This reduction in ACTH then lessens the stimulation of the adrenal glands, leading to a decrease in cortisol production. This self-regulatory process prevents excessive hormone accumulation. Conversely, if hormone levels drop too low, the inhibitory signals are reduced, allowing the hypothalamus and pituitary to increase their stimulatory output, thereby raising the hormone concentration back to the set point.
Examples of Negative Feedback
- Cortisol Regulation: High cortisol levels inhibit CRH and ACTH secretion.
- Thyroid Hormone Regulation: High T3 and T4 levels inhibit TRH and TSH secretion.
- Sex Hormone Regulation: High estrogen and testosterone levels can inhibit GnRH, FSH, and LH secretion.
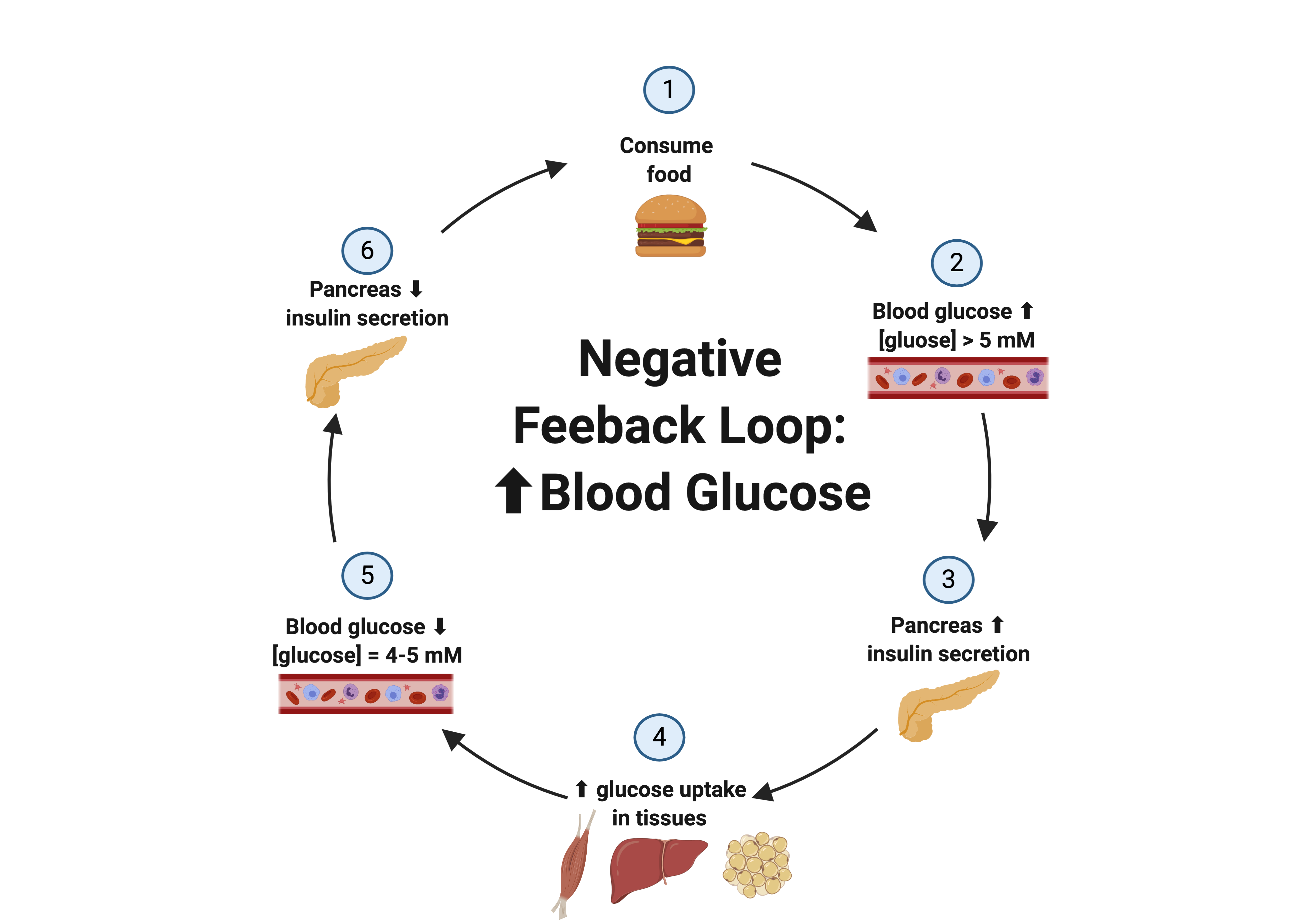
- Insulin and Glucagon Regulation: While not a direct feedback to the HPA axis, insulin and glucagon levels are tightly controlled by blood glucose concentrations, forming a feedback loop within the pancreas.
Positive Feedback: A Less Common but Important Mechanism
While negative feedback is the dominant regulatory mechanism, positive feedback loops also exist, albeit less frequently. In positive feedback, the product of a process amplifies the process itself, leading to a surge or escalation of activity. These are typically employed for specific, time-limited events that require a rapid and dramatic increase in hormone levels.
Examples of Positive Feedback
- Oxytocin and Childbirth: During labor, the pressure of the baby’s head on the cervix stimulates nerve endings. These signals are sent to the hypothalamus, which triggers the release of oxytocin from the posterior pituitary. Oxytocin, in turn, causes stronger uterine contractions, which further increase pressure on the cervix, leading to more oxytocin release. This escalating cycle continues until the baby is born, at which point the stimulus is removed, and the feedback loop ceases.
- Luteinizing Hormone (LH) Surge: In the female reproductive cycle, rising estrogen levels during the follicular phase initially exert negative feedback on GnRH and LH. However, as estrogen levels reach a critical threshold and are maintained for a sufficient period, they paradoxically switch to positive feedback, triggering a massive surge of LH. This LH surge is the crucial signal that initiates ovulation.
Other Influencing Factors on Hormone Concentrations
While the hypothalamic-pituitary axis and feedback mechanisms are the primary controllers, a multitude of other factors can influence hormone concentrations, acting as modulators or triggers for these regulatory systems.
Circadian Rhythms
Many hormones exhibit significant daily fluctuations, aligning with the body’s internal biological clock, known as the circadian rhythm. For instance, cortisol levels are typically highest in the early morning, promoting alertness and energy mobilization, and gradually decline throughout the day. Melatonin, a hormone involved in sleep regulation, shows a reverse pattern, increasing in darkness. These rhythms are primarily influenced by light exposure, which is signaled to the suprachiasmatic nucleus in the hypothalamus, the master circadian pacemaker.
Nutritional Status and Metabolism
The availability of nutrients and the body’s metabolic state profoundly impact hormone concentrations. For example, prolonged fasting or caloric restriction can alter the secretion of hormones involved in appetite regulation (e.g., ghrelin, leptin) and energy expenditure (e.g., thyroid hormones). Blood glucose levels are a direct regulator of insulin and glucagon secretion from the pancreas.
Stress
Both acute and chronic stress can significantly impact hormone concentrations, primarily through the activation of the HPA axis. The release of CRH, ACTH, and cortisol increases in response to stressors, mobilizing the body’s resources for a “fight or flight” response. Chronic stress can lead to sustained elevations of cortisol, which can have detrimental effects on various bodily systems.
Age
Hormone levels change naturally throughout the lifespan. Puberty is marked by the surge of sex hormones, while aging is often associated with declines in the production of certain hormones, such as growth hormone and sex hormones. These age-related changes are part of the natural developmental and aging processes.
Disease States
Numerous diseases directly affect hormone production or the body’s response to hormones. Endocrine gland disorders, such as hypothyroidism (underactive thyroid) or hyperthyroidism (overactive thyroid), diabetes mellitus (impaired insulin regulation), and Cushing’s syndrome (excess cortisol), are prime examples of how disease can disrupt normal hormone concentrations. Autoimmune diseases can also target endocrine glands, leading to hormone deficiencies.

Medications and External Substances
Pharmacological agents can directly influence hormone concentrations by mimicking hormones, blocking hormone receptors, or interfering with hormone synthesis or degradation. For example, hormone replacement therapy aims to restore deficient hormone levels, while certain medications can block the action of hormones like estrogen in conditions such as breast cancer. Environmental toxins and dietary supplements can also have unintended consequences on endocrine function.
In conclusion, while many external and internal factors can influence hormone levels, the most significant control over hormone concentrations is exerted by the sophisticated feedback mechanisms orchestrated by the hypothalamic-pituitary axis. These intricate regulatory systems, primarily negative feedback, ensure that hormones are released precisely when and where they are needed, maintaining physiological homeostasis and the overall health and function of the organism.
