In the realm of medical diagnostics and patient management, the International Normalized Ratio (INR) is a crucial metric. While the title might initially seem unrelated to the technical domains of drones and advanced flight technology, understanding INR is fundamentally about monitoring the efficacy and safety of certain medical treatments. For individuals who rely on technologies for maintaining their health or for those who work in fields that intersect with medical monitoring and personal well-being, a high INR can have significant implications. This article will delve into what a high INR signifies, its causes, potential risks, and the management strategies employed to bring it back into a safe and therapeutic range.
Understanding INR: A Foundation for Interpretation
The International Normalized Ratio (INR) is a standardized measurement used to assess how long it takes for a person’s blood to clot. It is particularly important for individuals taking anticoagulant medications, commonly known as blood thinners, such as warfarin (Coumadin). These medications are prescribed to prevent blood clots that can lead to serious conditions like deep vein thrombosis (DVT), pulmonary embolism (PE), stroke, and heart attack.
The Science Behind Blood Clotting
Blood clotting, or coagulation, is a complex physiological process involving a cascade of proteins and enzymes that work in concert to form a clot, thereby stopping bleeding. This process is essential for survival after injury, but an overactive clotting system can be detrimental, leading to the formation of dangerous clots in the bloodstream.
How INR is Measured
INR is derived from the Prothrombin Time (PT) test. PT measures the time it takes for blood to clot. However, PT results can vary significantly between laboratories due to differences in reagents and testing equipment. To standardize these results, the INR was developed. It normalizes the PT ratio by comparing an individual’s clotting time to a control sample and adjusting for the sensitivity of the thromboplastin reagent used. The formula is essentially:
INR = (Patient’s PT / Mean Normal PT) ^ ISI
Where:
- Patient’s PT: The prothrombin time of the patient’s blood sample.
- Mean Normal PT: The average prothrombin time of a healthy reference population.
- ISI (International Sensitivity Index): A factor that accounts for the sensitivity of the thromboplastin reagent used in the test.
The result is a dimensionless number. For individuals not on anticoagulant therapy, the normal INR range is typically between 0.8 and 1.2.
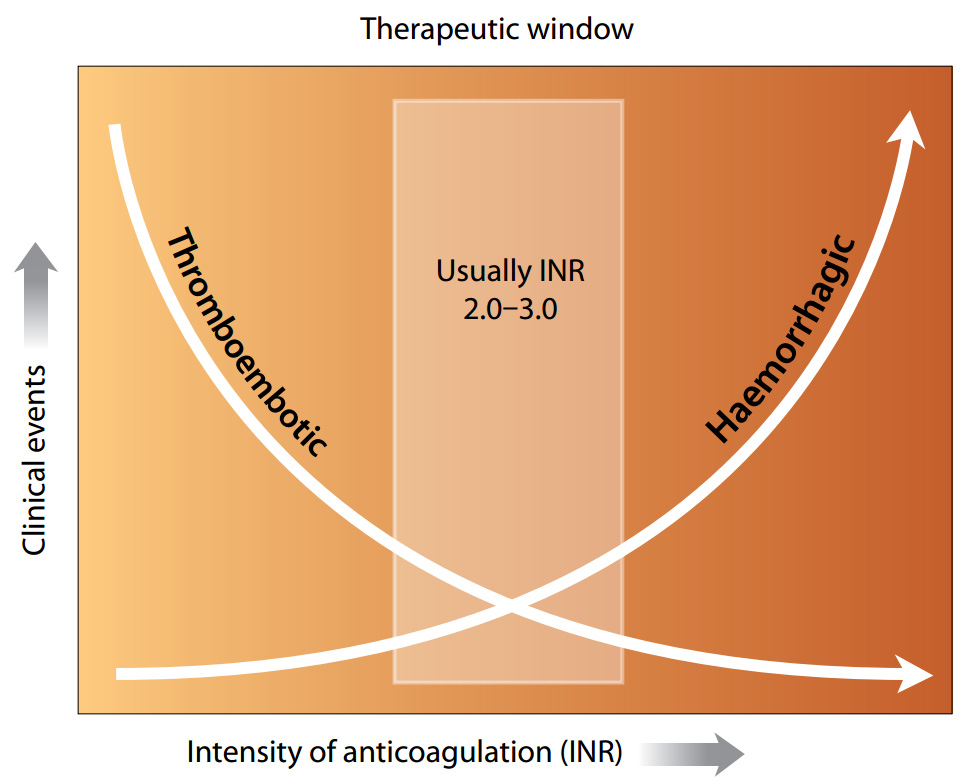
Therapeutic INR Ranges
For patients on anticoagulant therapy, the target INR range is higher and varies depending on the medical condition being treated. For instance:
- Mechanical heart valves: Often require an INR of 2.5 to 3.5.
- Atrial fibrillation or deep vein thrombosis/pulmonary embolism: Typically targeted for an INR of 2.0 to 3.0.
These higher ranges indicate that the blood is thinner and takes longer to clot, thus reducing the risk of dangerous clot formation.
What Constitutes a “High” INR?
A “high” INR refers to a reading that is above the recommended therapeutic range for an individual, or significantly above the normal range for someone not on anticoagulant medication. While the exact definition of “high” depends on the context and the target therapeutic range, generally:
- For individuals NOT on anticoagulants: An INR above 1.2 is considered elevated.
- For individuals ON anticoagulants: An INR above the upper limit of their target range is considered high. For example, if the target is 2.0-3.0, an INR of 3.1 or higher would be considered high.
Severity of High INR
The implications of a high INR are often categorized by the degree of elevation:
- Mildly High INR (e.g., 3.1-4.0): This is a common occurrence for patients on anticoagulants and may not immediately cause symptoms. However, it still increases the risk of bleeding.
- Moderately High INR (e.g., 4.1-5.0): The risk of bleeding becomes more significant.
- Very High INR (e.g., above 5.0): This level poses a substantial and immediate risk of serious bleeding, even from minor injuries.
- Extremely High INR (e.g., above 10.0): This is a medical emergency, carrying a very high risk of spontaneous and severe bleeding.
Causes of a High INR
A high INR indicates that the anticoagulant medication is working too effectively, making the blood too thin. Several factors can contribute to this over-anticoagulation:
1. Medication-Related Factors
- Dosage Errors: Taking more medication than prescribed, either accidentally or intentionally.
- Missed Doses Followed by Overcompensation: If a dose is missed, patients might be tempted to take a double dose later, leading to a spike in INR.
- Interactions with Other Medications: Many medications can interact with warfarin, affecting its metabolism and potency. These include:
- Antibiotics: Certain broad-spectrum antibiotics can kill gut bacteria that produce vitamin K, which is an antagonist to warfarin.
- Antifungal medications: Some antifungals inhibit the enzymes that metabolize warfarin.
- Amiodarone: A common heart rhythm medication that can significantly increase INR.
- Non-steroidal anti-inflammatory drugs (NSAIDs): While not directly affecting INR, NSAIDs can increase the risk of bleeding, especially when combined with a high INR.
- Certain seizure medications (e.g., phenytoin): These can initially decrease INR but later increase it.
- Aspirin: Often taken for cardiovascular prevention, its additive antiplatelet effect can worsen bleeding with a high INR.
- Over-the-Counter (OTC) Medications and Supplements: Acetaminophen (Tylenol) in large doses can affect INR. Many herbal supplements, such as ginkgo biloba, garlic, and ginseng, can also increase bleeding risk and affect INR.
2. Dietary Factors
- Vitamin K Intake: Vitamin K is a direct antagonist to warfarin. Sudden and significant reductions in dietary vitamin K intake can lead to an increased INR. Conversely, sudden increases can decrease INR. Consistency in vitamin K intake (found in leafy green vegetables like spinach, kale, and broccoli) is key for stable INR control.
- Alcohol Consumption: Acute, heavy alcohol consumption can inhibit the metabolism of warfarin, leading to an increased INR. Chronic heavy alcohol use can have variable effects, sometimes increasing and sometimes decreasing INR due to liver damage.
3. Health Conditions
- Liver Dysfunction: The liver is responsible for producing clotting factors and metabolizing warfarin. Impaired liver function can lead to a higher INR because the body cannot effectively process the medication or produce clotting factors.
- Heart Failure: Worsening heart failure can lead to fluid buildup and impaired liver function, which can increase INR.
- Diarrhea or Vomiting: Significant gastrointestinal losses can affect nutrient absorption, including vitamin K, and the body’s ability to metabolize warfarin.
- Fever and Illness: General illness and fever can sometimes increase INR.
4. Genetic Factors
- CYP2C9 and VKORC1 Polymorphisms: Variations in the genes responsible for metabolizing warfarin (CYP2C9) and processing vitamin K (VKORC1) can significantly impact how an individual responds to the drug. Some genetic variants lead to a slower metabolism, requiring lower doses and making them more prone to higher INR readings.
5. Testing Errors
Although less common, errors in the laboratory or point-of-care testing can lead to an inaccurate high INR reading.
Risks Associated with a High INR
The primary and most serious risk of a high INR is bleeding. The thinner the blood, the more difficult it is for the body to stop bleeding, even from minor trauma.
Types of Bleeding
Bleeding can manifest in various ways, ranging from minor to life-threatening:
- Minor Bleeding:
- Nosebleeds (epistaxis) that are prolonged or difficult to stop.
- Bleeding gums during brushing or flossing.
- Easy bruising from minor bumps.
- Prolonged bleeding from small cuts.
- Moderate Bleeding:
- Blood in the urine (hematuria), causing pink or red urine.
- Blood in the stool (melena or hematochezia), appearing as black, tarry stools or bright red blood in the stool.
- Heavy menstrual bleeding in women.
- Vomiting blood (hematemesis).
- Serious/Life-Threatening Bleeding:
- Gastrointestinal Bleeding: Can be occult (undetected) or overt, leading to anemia, weakness, dizziness, and potentially requiring blood transfusions.
- Intracranial Hemorrhage (Brain Bleed): This is the most feared complication. Symptoms can include severe headache, confusion, weakness on one side of the body, difficulty speaking, vision changes, and loss of consciousness. This is a medical emergency.
- Bleeding into Joints (Hemarthrosis): Can cause severe pain, swelling, and stiffness.
- Excessive Bleeding During Surgery or Dental Procedures: This can lead to significant blood loss and complications.
Other Potential Consequences
Beyond direct bleeding, a high INR can necessitate interruptions in anticoagulant therapy, which in turn increases the risk of clot formation that the medication was intended to prevent. This creates a delicate balancing act for healthcare providers.
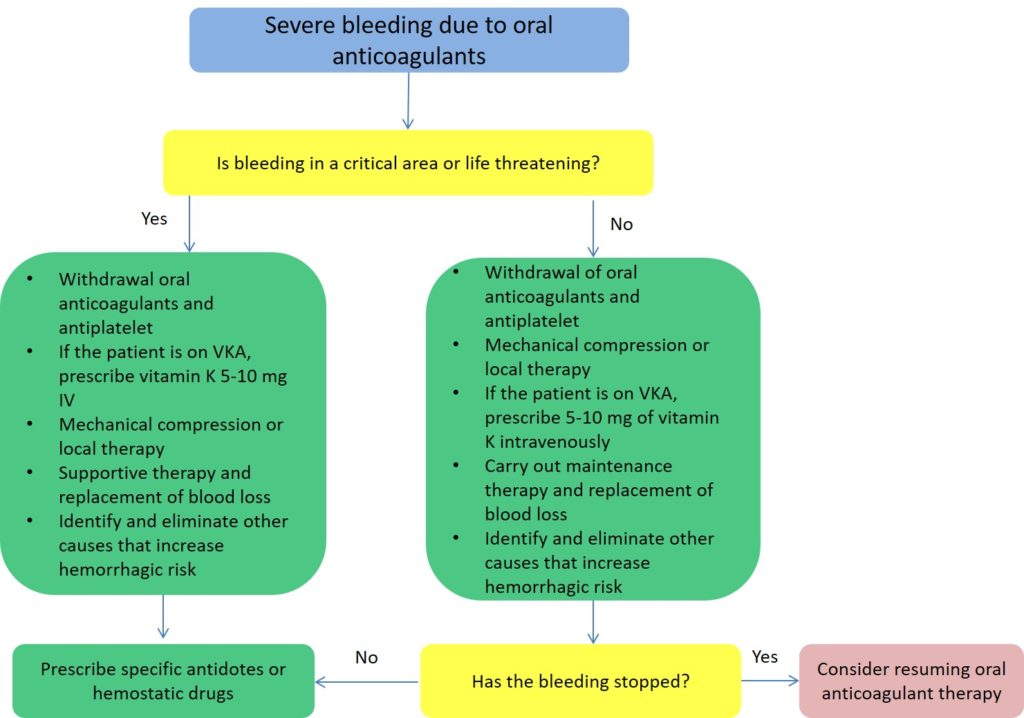
Managing a High INR
Managing a high INR involves a multi-faceted approach aimed at reducing the immediate risk of bleeding and re-establishing safe and effective anticoagulation.
1. Immediate Actions
- Hold or Reduce Medication Dose: The first and most common step is to temporarily stop taking the anticoagulant or reduce the dose, as advised by a healthcare professional.
- Vitamin K Administration: For significantly high INRs, especially above 5.0, or in cases of active bleeding, a dose of vitamin K may be administered. Vitamin K works by counteracting the effects of warfarin. It can be given orally or intravenously, with intravenous administration acting more rapidly. The dose of vitamin K is crucial; too much can make it difficult to regain therapeutic anticoagulation later.
- Blood Products: In cases of active, severe bleeding, fresh frozen plasma (FFP) or prothrombin complex concentrate (PCC) may be administered to rapidly provide clotting factors and reverse the anticoagulant effect. FFP contains all clotting factors, while PCC contains concentrated clotting factors, including prothrombin.
2. Lifestyle and Dietary Adjustments
- Dietary Consistency: Patients on warfarin are advised to maintain a consistent intake of vitamin K-rich foods. Sudden changes should be avoided, and any new dietary habits should be discussed with a healthcare provider.
- Alcohol Moderation: Limiting alcohol consumption, especially binge drinking, is important for stable INR.
- Medication Review: A thorough review of all medications, including OTC drugs, supplements, and herbal remedies, is essential to identify and avoid potential interactions.
3. Regular Monitoring
- Frequent INR Testing: When INR is high or unstable, more frequent blood tests are required to monitor its trend. Once the INR is back within the therapeutic range, regular monitoring can resume at the previously established intervals.
- Patient Education: Comprehensive education for patients is paramount. They need to understand the signs and symptoms of bleeding, the importance of adhering to medication schedules, dietary recommendations, and when to seek medical attention.
4. Exploring Alternative Anticoagulants
For some individuals who experience frequent INR fluctuations or have difficulty maintaining a stable therapeutic range, healthcare providers may consider switching to newer direct oral anticoagulants (DOACs). These medications, such as rivaroxaban, apixaban, dabigatran, and edoxaban, generally have more predictable pharmacokinetics, fewer drug and food interactions, and do not typically require routine INR monitoring. However, they are not suitable for all patients, particularly those with mechanical heart valves.

Conclusion: Vigilance and Collaboration
A high INR is a critical indicator that requires prompt attention and careful management. It signals an increased risk of bleeding, a complication that can range from minor inconvenience to a life-threatening emergency. Understanding the factors that contribute to a high INR, whether they are related to medication, diet, or underlying health conditions, is the first step towards effective prevention and management. For individuals on anticoagulant therapy, maintaining open communication with their healthcare team, adhering to prescribed regimens, and being vigilant about potential warning signs are crucial for ensuring their safety and well-being. Through regular monitoring, informed lifestyle choices, and timely medical intervention, a high INR can be effectively addressed, allowing patients to continue benefiting from the protective effects of anticoagulant therapy while minimizing the associated risks.
