The concept of a low histamine diet has gained traction as individuals seek to manage a range of health issues that may be linked to histamine intolerance. While not a formally recognized medical diagnosis, histamine intolerance describes a condition where the body struggles to break down histamine effectively, leading to a buildup of this biogenic amine and a cascade of unpleasant symptoms. Understanding the nuances of histamine, its role in the body, and how dietary choices can influence its levels is crucial for anyone considering or embarking on a low histamine approach to their health.

Histamine is a fascinating molecule. It’s not simply a food component to be avoided; it’s a vital neurotransmitter and mediator produced naturally by the body. Histamine plays a significant role in localized immune responses, acting as the body’s alarm system to signal invaders like pathogens. When allergens or irritants are detected, mast cells and basophils release histamine, triggering inflammation. This inflammation is designed to increase blood flow to the affected area, making it easier for immune cells to reach and neutralize the threat. This process is responsible for the classic allergy symptoms we often associate with histamine: sneezing, itching, runny nose, hives, and swelling.
Beyond immune responses, histamine is also critical for normal physiological functions. It acts as a neurotransmitter in the brain, influencing wakefulness, alertness, and cognitive processes. It plays a role in regulating gastric acid secretion, essential for digestion, and contributes to the dilation of blood vessels, impacting blood pressure and circulation. Therefore, the goal of a low histamine diet is not to eliminate histamine entirely, but rather to reduce the intake of exogenous histamine from food and beverages, and to support the body’s natural histamine-metabolizing processes.
Understanding Histamine Intolerance
Histamine intolerance is often described as a state of imbalance. It occurs when there is an oversupply of histamine relative to the body’s capacity to break it down. This breakdown is primarily facilitated by enzymes, the most prominent being diamine oxidase (DAO), found in the intestinal lining, and histamine N-methyltransferase (HNMT), present in various tissues, including the gut and brain. If these enzymes are insufficient, inhibited, or overwhelmed, histamine can accumulate in the bloodstream and tissues, leading to a spectrum of symptoms that can mimic allergic reactions but without the presence of IgE antibodies.
The symptoms of histamine intolerance can be diverse and often overlap with other conditions, making diagnosis challenging. Common manifestations include:
- Gastrointestinal Issues: Bloating, gas, abdominal pain, diarrhea, constipation, nausea, and vomiting.
- Skin Reactions: Hives, eczema, itching, flushing, and redness.
- Respiratory Symptoms: Nasal congestion, sneezing, wheezing, asthma-like symptoms, and shortness of breath.
- Neurological Effects: Headaches, migraines, dizziness, vertigo, anxiety, insomnia, difficulty concentrating, and fatigue.
- Cardiovascular Manifestations: Palpitations, irregular heartbeat, and changes in blood pressure.
- Menstrual Cycle Irregularities: In women, histamine can influence hormone regulation, potentially exacerbating premenstrual syndrome (PMS) symptoms or causing menstrual cycle disturbances.
It’s important to note that histamine intolerance is not a true allergy. Allergic reactions involve an immune system response triggered by specific allergens. Histamine intolerance, on the other hand, is a metabolic issue where the body’s ability to process histamine is compromised. This distinction is critical, as the management strategies will differ.
Several factors can contribute to histamine intolerance. Genetic predispositions can play a role, leading to reduced DAO or HNMT enzyme activity. Certain medications can inhibit DAO function, increasing histamine levels. Conditions affecting the gut lining, such as inflammatory bowel disease (IBD), celiac disease, or leaky gut syndrome, can impair DAO production and absorption. Even certain gut bacteria can produce histamine, further contributing to the body’s burden. Nutritional deficiencies, particularly in vitamin B6, vitamin C, copper, and zinc, which are cofactors for DAO and HNMT, can also compromise histamine breakdown.
The Principles of a Low Histamine Diet
A low histamine diet aims to reduce the overall histamine load on the body. This involves two primary strategies: minimizing the intake of high-histamine foods and avoiding foods that trigger the body’s own histamine release. It is important to emphasize that this diet is typically implemented temporarily to identify trigger foods and alleviate symptoms, with the goal of gradually reintroducing foods as tolerance improves. It is not intended as a long-term restrictive eating plan without professional guidance.
The cornerstone of a low histamine diet is understanding which foods are naturally high in histamine. This can vary significantly based on factors like aging, fermentation, and processing. Generally, the longer a food is stored, fermented, aged, or processed, the higher its histamine content is likely to be.
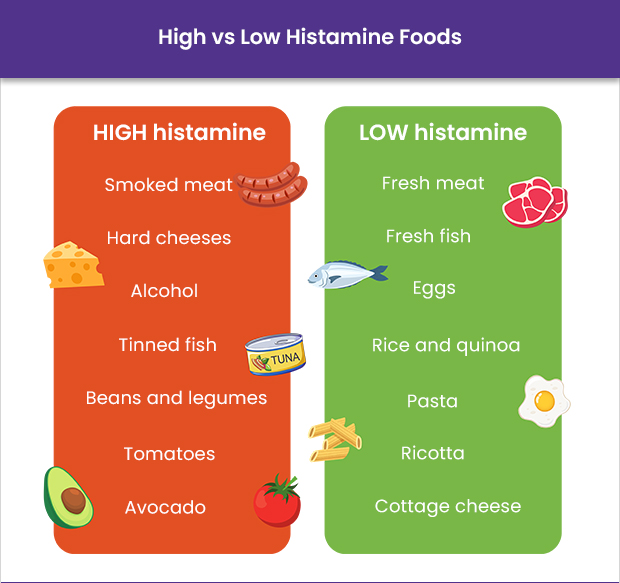
High-Histamine Foods to Consider Limiting or Avoiding:
- Fermented Foods: Sauerkraut, kimchi, yogurt, kefir, kombucha, tempeh, miso, aged cheeses (cheddar, Gruyère, Parmesan, etc.).
- Aged and Cured Meats: Salami, pepperoni, bacon, jerky, smoked meats.
- Certain Fish and Seafood: Canned fish (tuna, sardines, mackerel), smoked fish, shellfish (shrimp, crab, lobster). Freshly caught and frozen fish is generally considered lower in histamine if handled properly.
- Certain Vegetables: Spinach, tomatoes and tomato products (ketchup, paste, sauce), eggplant, avocado.
- Certain Fruits: Citrus fruits (oranges, lemons, grapefruit), strawberries, raspberries, dried fruits (raisins, dates, apricots).
- Alcohol: Especially red wine, beer, and champagne, which are often fermented and can inhibit DAO.
- Vinegars: All types, including balsamic, apple cider, and red wine vinegar.
- Leftovers: Histamine levels increase in foods as they sit, especially protein-rich foods.
- Artificial Colors and Preservatives: Some individuals find these can trigger histamine release.
Foods That Can Trigger Histamine Release (Histamine Liberators):
These foods may not be high in histamine themselves but can cause the body to release its stored histamine.
- Certain Fruits: Citrus fruits, strawberries, pineapple, papaya, kiwi.
- Certain Vegetables: Tomatoes, spinach, eggplant, avocado.
- Nuts and Seeds: Walnuts, cashews, peanuts.
- Chocolate and Cocoa:
- Additives: Food dyes, preservatives, and artificial sweeteners.
- Alcohol:
- Certain Spices: Cinnamon, cloves, paprika, curry powder.

Generally Well-Tolerated Low-Histamine Foods:
Focusing on what can be eaten is just as important as knowing what to avoid.
- Freshly Cooked Meats and Poultry: Beef, chicken, lamb, turkey (ensure they are fresh and not processed or aged).
- Freshly Caught Fish: Cooked immediately after catching.
- Most Fresh Vegetables: Except for those listed as high histamine (e.g., carrots, broccoli, cauliflower, lettuce, cucumber, zucchini, bell peppers, sweet potatoes).
- Most Fresh Fruits: Except for those listed as histamine liberators (e.g., apples, pears, blueberries, melon, peaches, mangoes, grapes).
- Gluten-Free Grains: Rice, quinoa, oats (if tolerated), millet.
- Dairy Alternatives: Coconut milk, almond milk, rice milk. Fresh, unaged cheeses like ricotta and mozzarella are sometimes tolerated in moderation.
- Herbs: Fresh herbs are generally well-tolerated.
- Oils: Olive oil, coconut oil.
- Sweeteners: Honey, maple syrup in moderation.
Practical Considerations and Preparation:
The freshness of food is paramount. Opt for the freshest ingredients possible and consume them soon after preparation. When cooking, make larger batches and freeze portions immediately rather than refrigerating leftovers for extended periods. This halts the enzymatic activity that increases histamine content.
Reading food labels meticulously is essential. Look out for ingredients like artificial colors, preservatives, and yeast extracts, which can be problematic for some. Be aware that many pre-packaged meals, sauces, marinades, and seasonings can contain hidden histamine triggers or histamine-releasing agents.
Cooking methods also play a role. Simple cooking methods like steaming, baking, or grilling are generally preferred over prolonged cooking or simmering, which can sometimes concentrate or degrade certain compounds in ways that might affect histamine levels.
Implementing and Navigating the Diet
Embarking on a low histamine diet should ideally be done under the guidance of a healthcare professional, such as a registered dietitian or nutritionist specializing in food sensitivities. They can help ensure nutritional adequacy, guide the process of elimination and reintroduction, and identify underlying causes for histamine intolerance.
The typical approach involves an elimination phase, where all high-histamine and histamine-releasing foods are removed for a period of 2-4 weeks. During this time, symptom tracking is crucial. A detailed food and symptom diary can help identify which foods are most strongly associated with a person’s reactions.
Following the elimination phase is the reintroduction phase. This is a systematic process where foods are gradually reintroduced one by one, in small amounts, and at increasing intervals (e.g., every 2-3 days). The goal is to identify individual tolerance levels for specific foods. This iterative process allows for the creation of a personalized, more sustainable eating plan that maximizes dietary variety while managing symptoms.
It’s important to be patient and persistent. Symptoms may not resolve immediately, and some individuals may experience a temporary increase in symptoms as their body adjusts. Focusing on whole, unprocessed foods, ensuring adequate hydration, and managing stress are all supportive elements of this dietary approach.
Beyond diet, other factors can influence histamine levels. Stress, lack of sleep, and strenuous exercise can sometimes exacerbate symptoms for those with histamine intolerance. Addressing these lifestyle factors can complement dietary changes.
Potential Challenges and Long-Term Management
The restrictive nature of a strict low histamine diet can present challenges. Social eating, dining out, and navigating family meals can become complicated. It requires careful planning, open communication with hosts or restaurant staff, and sometimes bringing one’s own food.
Nutritional deficiencies are also a concern if the diet is followed too restrictively for too long without proper planning. Consulting with a professional is vital to ensure adequate intake of all essential vitamins, minerals, and macronutrients.
The ultimate goal of a low histamine diet is not permanent restriction but rather achieving a state of balance and identifying individual triggers. Once a baseline of symptom reduction is achieved, the focus shifts to expanding the diet as much as possible while maintaining symptom control. This might involve finding a threshold for certain foods, understanding that occasional consumption might be tolerated, or identifying specific preparation methods that improve tolerance.
For some, histamine intolerance may be a temporary issue linked to gut healing or medication withdrawal. For others, it may be a more persistent condition requiring ongoing mindful eating. Regardless of the duration, the principles of understanding food composition, listening to one’s body, and working with healthcare professionals form the bedrock of successful management.
In conclusion, a low histamine diet is a dietary strategy aimed at reducing the body’s histamine load by limiting high-histamine foods and histamine-releasing agents. It is a tool for managing the symptoms associated with histamine intolerance, a condition characterized by the body’s impaired ability to break down histamine. By understanding the principles, carefully selecting foods, and implementing a systematic approach to elimination and reintroduction, individuals can navigate this dietary landscape to improve their well-being and regain a better quality of life.
