The sensation of a herniated disk is often described as a sharp, shooting pain that can radiate down the leg or arm, depending on the location of the herniated disk. It can also feel like numbness, tingling, or weakness in the affected limb. The pain can range from a dull ache to an intense, debilitating sensation, and it may be aggravated by certain movements or positions.
Understanding the Anatomy of the Spine
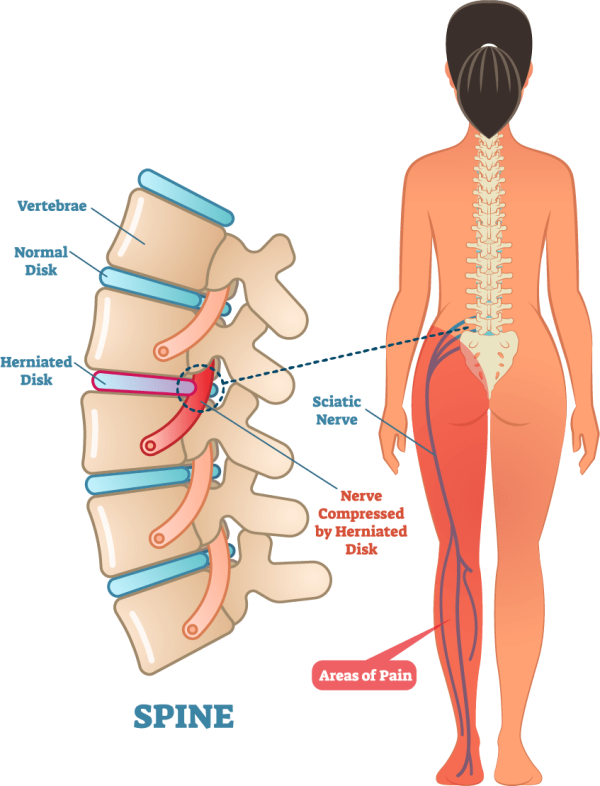
The spine is a complex structure composed of vertebrae, intervertebral disks, nerves, muscles, and ligaments. The intervertebral disks are cushion-like structures that sit between the vertebrae, acting as shock absorbers and allowing for flexibility. Each disk has an outer fibrous ring called the annulus fibrosus and a gel-like inner core called the nucleus pulposus.
The Role of Intervertebral Disks
Intervertebral disks are crucial for spinal health and function. They provide cushioning and support, absorb shock from everyday activities like walking and jumping, and allow for a wide range of motion in the spine. Their ability to absorb impact and distribute pressure is essential for preventing damage to the vertebrae and surrounding nerves.
Spinal Nerves and Their Pathways
The spinal cord, a bundle of nerves, runs through the vertebral column. Nerves branch out from the spinal cord to control all bodily functions, including sensation, movement, and organ function. When a herniated disk occurs, it can compress or irritate these delicate nerves, leading to a variety of symptoms. The specific symptoms experienced depend on which nerve root is affected and the extent of the compression.
The Mechanics of a Herniated Disk
A herniated disk, also known as a slipped or ruptured disk, occurs when the soft inner material of the disk pushes through a tear or weak spot in the outer fibrous ring. This protrusion can then press against nearby spinal nerves, causing pain and other neurological symptoms.
Causes of Disk Herniation
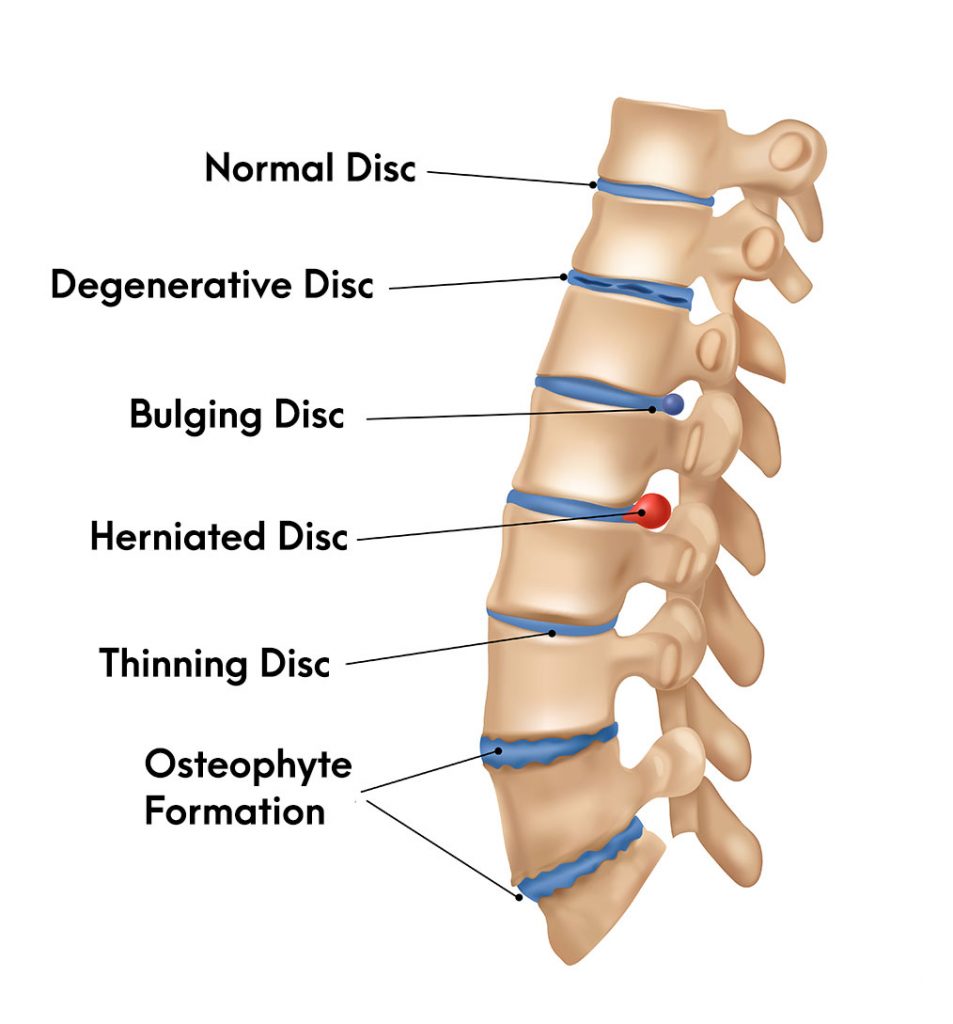
Several factors can contribute to disk herniation. Age-related wear and tear, known as degenerative disk disease, is a common cause. As we age, disks lose water content and become less flexible, making them more prone to tearing. Improper lifting techniques, sudden or forceful movements, and trauma to the spine can also lead to herniation. Obesity and a sedentary lifestyle can also increase the risk by putting extra stress on the spine.
The Process of Disk Protrusion
The process of disk herniation typically begins with a weakening or tearing of the annulus fibrosus. This can happen gradually over time due to degeneration or more suddenly due to an injury. Once the outer layer is compromised, the nucleus pulposus can begin to bulge or push through the tear. If the herniation is significant enough, it can impinge upon a spinal nerve root.
Experiencing the Symptoms of a Herniated Disk
The symptoms of a herniated disk can vary widely depending on the location and severity of the herniation. While pain is the most common symptom, it’s often accompanied by a cascade of other uncomfortable sensations.
Radiating Pain: The Hallmark Symptom
Perhaps the most characteristic symptom of a herniated disk is radiating pain. This pain typically travels along the path of the compressed nerve. For a herniated disk in the lower back (lumbar spine), this often means pain that shoots down the buttock and into the leg, known as sciatica. In the neck (cervical spine), a herniated disk can cause pain that radiates down the arm and into the hand. This radiating pain is often described as sharp, burning, or electric-like.
Numbness and Tingling: Nerve Irritation
Alongside pain, individuals may experience numbness and tingling, often referred to as paresthesia. This occurs when the compressed nerve’s ability to transmit sensory signals is disrupted. The area of numbness and tingling usually corresponds to the distribution of the affected nerve. For example, a herniated disk in the lumbar spine might cause numbness in the foot or toes, while a cervical herniation could lead to numbness in the fingers.
Weakness and Loss of Motor Function

In more severe cases, a herniated disk can cause muscle weakness in the affected limb. This happens when the compressed nerve can no longer effectively send signals to the muscles it controls. This weakness can manifest as difficulty lifting the foot (foot drop), a tendency to stumble, or a reduced grip strength in the hand. In very rare and severe instances, compression of multiple nerve roots can lead to more significant motor deficits.
Aggravating Factors and Relief
The pain associated with a herniated disk is often exacerbated by certain movements. Bending, twisting, lifting, or even prolonged sitting or standing can put additional pressure on the disk and nerve, intensifying the symptoms. Conversely, some people find relief in specific positions, such as lying down with their knees bent.
Diagnosing and Managing a Herniated Disk
Accurate diagnosis is crucial for effective treatment of a herniated disk. A healthcare professional will typically conduct a physical examination and may recommend imaging tests to confirm the diagnosis and determine the extent of the herniation.
The Diagnostic Process
A thorough medical history and physical examination are the first steps. The doctor will ask about the nature of the pain, its location, duration, and any aggravating or relieving factors. They will also assess reflexes, muscle strength, and sensation in the affected limbs. To visualize the disk and surrounding nerves, imaging techniques such as MRI (Magnetic Resonance Imaging) are often used, as they provide detailed images of soft tissues. X-rays may be used to rule out other spinal conditions, and CT scans can also be helpful in some cases.
Treatment Options: From Conservative to Surgical
Treatment for a herniated disk typically begins with conservative measures. These often include rest, pain medication (such as NSAIDs or muscle relaxants), physical therapy to strengthen supporting muscles and improve flexibility, and sometimes epidural steroid injections to reduce inflammation around the affected nerve.
Conservative Management
Physical therapy plays a vital role in recovery. Exercises are designed to improve posture, strengthen core muscles, and increase the space between vertebrae, thereby relieving pressure on the nerve. Modifying activities that aggravate the pain is also important.
Surgical Intervention
If conservative treatments do not provide relief or if there are signs of significant nerve compression (such as progressive weakness or loss of bowel or bladder control), surgery may be recommended. Surgical options include microdiscectomy, where the herniated portion of the disk is removed, or laminectomy, which involves removing a portion of the bone to create more space for the nerves.
Living with and Preventing Herniated Disks
While a herniated disk can be a painful and disruptive condition, many individuals experience significant relief with proper treatment and management. Long-term strategies focus on maintaining spinal health and preventing future occurrences.
Lifestyle Adjustments for Spinal Health
Maintaining a healthy weight is crucial, as excess body weight places additional stress on the spine. Regular exercise, particularly activities that strengthen core muscles like the abdomen and back, can provide significant support. Good posture is also important, both when sitting and standing. Proper lifting techniques, which involve using the legs rather than the back, can prevent acute injuries.
The Role of Physical Therapy and Exercise
Continuing with recommended exercises even after the initial pain subsides can help maintain spinal stability and flexibility. A physical therapist can provide personalized exercise programs and guidance on safe movements. Activities like swimming, walking, and yoga, when performed correctly, can be beneficial for overall spinal health.
When to Seek Medical Attention
It’s important to seek medical attention if you experience sudden, severe back or neck pain, pain that radiates down an arm or leg, numbness, tingling, or weakness, or any loss of bowel or bladder control. Early diagnosis and treatment can significantly improve outcomes and help prevent long-term complications.
