In the intricate ecosystem of modern healthcare, where precision, efficiency, and patient well-being are paramount, the role of technology is increasingly vital. Among the sophisticated devices that contribute to optimal patient care, the telemetry unit stands out as a critical component. While the term “telemetry” itself suggests remote measurement and transmission of data, its application within a hospital setting is multifaceted, encompassing continuous physiological monitoring, data analysis, and proactive intervention. Understanding what constitutes a telemetry unit in a hospital is essential for appreciating its impact on patient outcomes, healthcare provider workflows, and the overall advancement of medical technology.

The Core Functionality of Hospital Telemetry
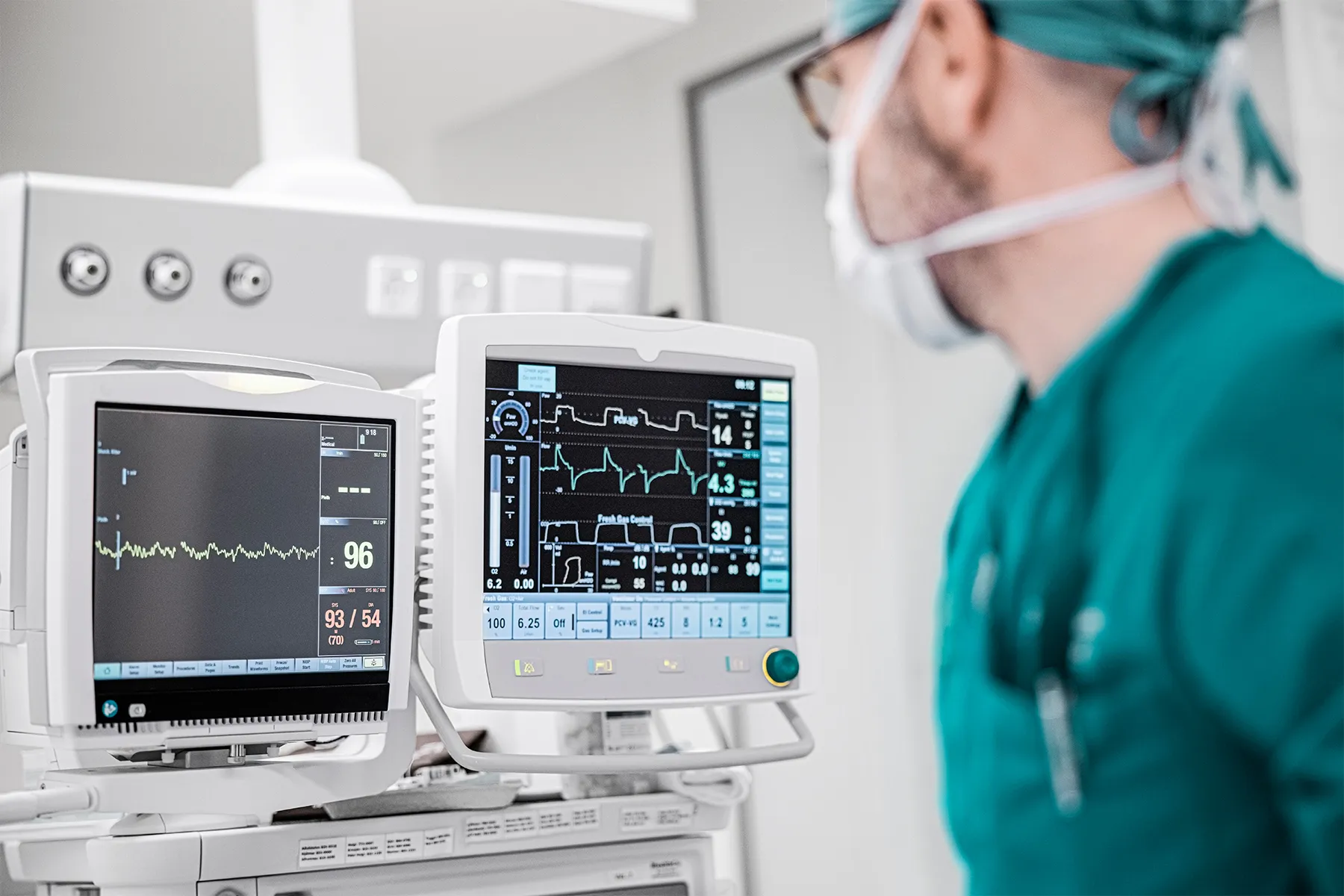
At its heart, a hospital telemetry unit is designed for the continuous, real-time monitoring of a patient’s vital physiological parameters. This goes beyond the intermittent checks typically performed by nursing staff. Instead, telemetry systems capture and transmit data wirelessly from sensors attached to the patient to a central monitoring station, where trained personnel can observe trends, detect abnormalities, and respond swiftly to emergent situations.
Physiological Parameters Monitored
The primary focus of telemetry is often cardiac activity. Electrocardiogram (ECG) leads are typically attached to the patient’s chest, allowing for continuous monitoring of heart rate, rhythm, and the detection of potentially life-threatening arrhythmias such as ventricular tachycardia or atrial fibrillation. However, modern telemetry units are frequently equipped to monitor a broader spectrum of vital signs.
- Heart Rate and Rhythm: This is the cornerstone of cardiac telemetry. Irregularities in heart rate or rhythm can be early indicators of cardiac distress, electrolyte imbalances, or medication side effects.
- Oxygen Saturation (SpO2): Non-invasive sensors, often clipped to a finger or earlobe, measure the percentage of hemoglobin in the blood that is saturated with oxygen. This is crucial for patients with respiratory conditions, those recovering from surgery, or individuals experiencing hypoxia.
- Blood Pressure: While not always continuously measured in all telemetry setups, some advanced units can periodically or even continuously monitor blood pressure, providing valuable insights into hemodynamic stability.
- Respiratory Rate: The frequency of breathing can also be monitored, offering further clues about a patient’s respiratory status and overall condition.
- Temperature: In certain critical care scenarios, continuous temperature monitoring via telemetry can be essential for detecting fever or hypothermia.
The data streams from these sensors are transmitted wirelessly, often using secure radio frequencies, to a central monitoring console or directly to bedside monitors and electronic health records (EHRs). This wireless capability is a defining characteristic of telemetry, freeing patients from being tethered to bedside equipment and allowing for greater mobility within the hospital.
Data Transmission and Centralized Monitoring
The “telemetry” aspect refers to the technology that enables the remote transmission of this vital data. Miniature, portable transmitters, often worn by the patient, collect signals from the sensors. These transmitters then send the data to a central monitoring station, typically located in a nurses’ station or a dedicated telemetry monitoring department.
At the central station, specialized nurses or technicians, often referred to as telemetry technicians or cardiac monitor technicians, are responsible for observing the incoming data streams from multiple patients simultaneously. They are trained to recognize normal physiological patterns and, more importantly, to identify deviations that may indicate a worsening condition. This centralized approach allows for a more efficient allocation of skilled personnel and ensures that critical events are not missed due to staff shortages or the demanding workload on individual nursing units.
The monitoring station is equipped with sophisticated software that displays the physiological data in a clear and organized manner. Alarms are a critical feature, programmed to alert monitoring staff when vital signs fall outside predefined parameters or when specific dangerous rhythms are detected. These alarms are designed to be sensitive enough to catch potential problems early while minimizing nuisance alarms that can lead to alarm fatigue.
Applications and Patient Populations
The deployment of telemetry units in hospitals is not uniform; it is strategically applied to specific patient populations and clinical scenarios where continuous monitoring is deemed essential for safety and effective treatment.
Cardiac Patients
The most common application of telemetry is for patients with known or suspected cardiac conditions. This includes individuals admitted with:
- Acute Coronary Syndromes (ACS): Including unstable angina and myocardial infarction (heart attack), where continuous ECG monitoring is crucial for detecting arrhythmias and changes in ischemia.
- Post-Percutaneous Coronary Intervention (PCI) or Coronary Artery Bypass Graft (CABG) Surgery: Patients recovering from these procedures are at risk of cardiac complications and require close observation.
- Heart Failure Exacerbations: Monitoring of rhythm and fluid status indicators can help manage acute decompensation.
- Congenital Heart Disease: Particularly in adults, ongoing monitoring may be necessary to manage arrhythmias or other cardiac anomalies.
- Electrophysiology Studies and Procedures: Patients undergoing evaluation or treatment for heart rhythm disorders often benefit from telemetry.
Respiratory Distress and Post-Operative Care
Beyond cardiology, telemetry plays a significant role in monitoring patients with respiratory compromise or those at high risk during the post-operative period.
- Chronic Obstructive Pulmonary Disease (COPD) Exacerbations: Monitoring oxygen saturation and respiratory rate is vital for patients experiencing acute breathing difficulties.
- Pneumonia and Other Severe Respiratory Infections: Patients with severe lung infections may require continuous oxygen saturation monitoring.
- Post-Surgical Patients: Especially after thoracic or abdominal surgery, patients may be at risk for respiratory depression from anesthesia, pain medications, or the development of pulmonary complications. Telemetry allows for early detection of declining oxygen levels.
- Patients on Certain Medications: Certain drugs, particularly those affecting heart rate, blood pressure, or respiratory drive (e.g., opioids, sedatives), may warrant telemetry monitoring to ensure patient safety.
Neurological Conditions and Seizure Monitoring
In specific neurological contexts, telemetry can also be invaluable.

- Patients at Risk for Seizures: For individuals with epilepsy or those who have experienced seizures, continuous EEG monitoring, which is a specialized form of telemetry, can be used to detect seizure activity even when it is subtle or non-convulsant. While not always considered standard “telemetry,” the principle of remote, continuous physiological data transmission is similar.
- Patients Post-Stroke or with Neurological Injuries: Monitoring vital signs can help detect complications such as changes in blood pressure that could impact neurological recovery.
The decision to place a patient on telemetry is typically made by a physician based on their clinical assessment, the patient’s diagnosis, and the identified risks.
Technological Advancements and the Future of Telemetry
The evolution of telemetry technology has been driven by the need for greater accuracy, reliability, improved patient comfort, and seamless integration into the broader healthcare IT infrastructure.
Miniaturization and Patient Comfort
Early telemetry devices were often bulkier and less comfortable for patients. Modern telemetry transmitters are significantly smaller, lighter, and more discreet. This improved design enhances patient mobility, allows for better sleep and overall comfort, and reduces the likelihood of skin irritation from prolonged sensor wear. The wireless nature of these devices inherently promotes early ambulation, which is crucial for recovery and preventing complications like deep vein thrombosis.
Data Security and Interoperability
As healthcare data becomes increasingly digitized, the security and interoperability of telemetry systems are paramount. Robust encryption protocols are employed to protect patient data during transmission. Furthermore, advanced telemetry systems are designed to integrate with Electronic Health Records (EHRs). This integration allows for the seamless flow of telemetry data into the patient’s chart, providing clinicians with a comprehensive view of the patient’s status and enabling better-informed decision-making.
Sophisticated Alarm Management and Predictive Analytics
A significant area of advancement lies in alarm management. Alarm fatigue, a phenomenon where healthcare providers become desensitized to frequent alarms, can lead to missed critical events. Newer telemetry systems incorporate intelligent alarm features that can:
- Filter Nuisance Alarms: Using algorithms to distinguish between true physiological events and artifact (e.g., patient movement, loose leads).
- Provide Contextual Alarms: Delivering more specific information about the nature of the alarm.
- Implement Dynamic Thresholds: Adjusting alarm limits based on the patient’s current condition and historical data.
Looking ahead, the integration of artificial intelligence (AI) and machine learning into telemetry is poised to revolutionize its capabilities. AI algorithms can analyze vast amounts of historical and real-time telemetry data to identify subtle patterns that may precede a critical event, such as cardiac arrest or sepsis. This allows for a shift from reactive monitoring to proactive intervention, where potential problems can be identified and addressed before they become life-threatening. Predictive analytics can offer early warnings, giving clinical teams more time to intervene and improve patient outcomes.
The Role of the Telemetry Monitoring Team
While the technology itself is sophisticated, the human element remains indispensable in the effective functioning of a hospital telemetry unit. The team responsible for monitoring these patients is critical to translating raw data into actionable clinical insights.
The Telemetry Technician
Often the first line of defense, telemetry technicians are trained to monitor multiple patient waveforms and vital signs from a central station. Their responsibilities typically include:
- Continuous Observation: Vigilantly watching patient data for any deviations from normal.
- Alarm Response: Immediately identifying and responding to alarms, including verifying the alarm with the patient or bedside nurse.
- Documentation: Accurately recording any significant findings, rhythm changes, or events.
- Troubleshooting: Identifying and reporting issues with equipment, leads, or transmitters.
- Communication: Alerting the registered nurse or physician to critical changes in a patient’s condition.
The Registered Nurse
Registered nurses (RNs) working on units where telemetry patients are managed are integral to the process. They work in tandem with telemetry technicians and are responsible for:
- Clinical Assessment: Integrating telemetry data with their own physical assessments and patient history.
- Intervention: Initiating appropriate medical interventions based on telemetry findings and physician orders.
- Patient Education: Explaining the purpose of telemetry monitoring to patients and ensuring they understand how to use the equipment.
- Medication Management: Monitoring the effects of medications on cardiac rhythm and vital signs.
- Collaboration: Communicating effectively with physicians, telemetry technicians, and other members of the healthcare team.
Collaboration and Communication
The success of telemetry monitoring hinges on seamless communication and collaboration between the telemetry monitoring team and the bedside nursing staff. Protocols are established to ensure that alarms are handled efficiently and that critical information is relayed promptly. For instance, a telemetry technician might alert the bedside nurse to a significant change in rhythm, and the nurse would then perform a focused assessment and communicate with the physician. This multi-tiered approach ensures that no critical data point is missed and that timely, appropriate actions are taken to safeguard patient health. The integration of telemetry data into the EHR further enhances this collaborative effort by providing a shared, easily accessible record of the patient’s physiological status.
In conclusion, a telemetry unit in a hospital is a sophisticated system dedicated to the continuous, remote monitoring of vital physiological data. Its primary role is to enhance patient safety by enabling early detection of critical events, particularly in cardiac and respiratory compromised individuals. Through advancements in technology, including miniaturization, improved data security, and intelligent alarm systems, telemetry continues to evolve, promising even more proactive and predictive patient care in the future, all underpinned by the crucial oversight of skilled healthcare professionals.
