Understanding Gestational Age and Risk Factors
The term “high-risk pregnancy” is often associated with advanced maternal age, and for good reason. While chronological age is a significant factor, it’s crucial to understand that the underlying physiological changes and potential complications are what define a high-risk pregnancy, regardless of whether they are directly attributable to age or other contributing factors. Gestational age, specifically, plays a pivotal role in assessing pregnancy outcomes and potential challenges. A pregnancy is typically considered high-risk if there’s an increased likelihood of complications for the mother, the baby, or both. These complications can manifest during pregnancy, labor, or even postpartum.

Advanced Maternal Age and Its Implications
The commonly cited threshold for advanced maternal age is typically 35 years old. While many women in their late thirties and forties have perfectly healthy pregnancies and babies, the statistical likelihood of certain risks increases as a woman ages. These risks include:
- Chromosomal Abnormalities: The risk of having a baby with a chromosomal condition, such as Down syndrome (Trisomy 21), Edwards syndrome (Trisomy 18), and Patau syndrome (Trisomy 13), increases significantly with maternal age. This is due to a higher probability of errors occurring during egg cell division.
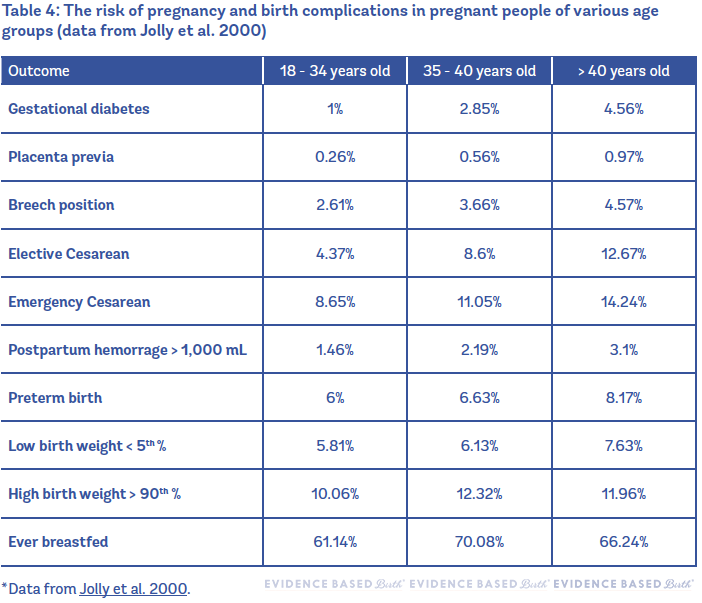
- Pregnancy Complications: Women over 35 are at a higher risk for developing conditions like gestational diabetes and preeclampsia. Gestational diabetes is a type of diabetes that develops during pregnancy, and preeclampsia is a serious condition characterized by high blood pressure and signs of damage to other organ systems, most often the liver and kidneys.
- Miscarriage and Stillbirth: The risk of pregnancy loss, including miscarriage (loss of the fetus before 20 weeks of gestation) and stillbirth (fetal death after 20 weeks of gestation), also tends to be higher in older mothers.
- Cesarean Delivery: Due to potential complications and longer labor times, women of advanced maternal age may have a higher likelihood of requiring a cesarean delivery.
- Fertility Challenges: While not a direct risk during pregnancy, it’s important to note that fertility can decline with age, potentially leading to longer conception times or the need for assisted reproductive technologies, which themselves can sometimes be associated with certain pregnancy considerations.
Beyond Age: Other Defining Factors of High-Risk Pregnancy
It is a critical misconception to solely attribute “high-risk” status to maternal age. Numerous other factors can contribute to or independently define a high-risk pregnancy. Understanding these factors is vital for comprehensive prenatal care and management.
Pre-existing Medical Conditions
Existing chronic health issues can significantly impact a pregnancy. These include:
- Hypertension (High Blood Pressure): Chronic hypertension can increase the risk of preeclampsia, placental abruption (where the placenta separates from the uterus before birth), and fetal growth restriction.
- Diabetes Mellitus: Both type 1 and type 2 diabetes, if not well-controlled, can lead to birth defects, macrosomia (a baby larger than average), and complications like preeclampsia.
- Heart Disease: Conditions affecting the heart can make the physical demands of pregnancy more challenging and increase the risk of complications for both mother and baby.
- Kidney Disease: Impaired kidney function can affect the body’s ability to manage fluid balance and waste removal, which are crucial during pregnancy.
- Autoimmune Disorders: Conditions like lupus or rheumatoid arthritis can pose risks to the developing fetus and complicate pregnancy management.
- Thyroid Disorders: Both hyperthyroidism (overactive thyroid) and hypothyroidism (underactive thyroid) can affect fetal development and maternal health if not properly managed.
Reproductive History and Previous Pregnancies
A woman’s past reproductive experiences can be strong indicators of future risks.
- Previous Preterm Birth: A history of delivering a baby prematurely (before 37 weeks of gestation) significantly increases the risk of another preterm birth.
- Previous Preeclampsia or Eclampsia: Women who have experienced these conditions in a prior pregnancy are at a higher risk of recurrence.
- Previous Cesarean Delivery: While not always a direct risk factor for the pregnancy itself, it dictates delivery options for subsequent pregnancies. Multiple C-sections can increase risks of placenta previa and placenta accreta.
- History of Miscarriage or Stillbirth: While often emotionally distressing, a history of multiple miscarriages or a stillbirth may warrant closer monitoring in subsequent pregnancies to identify and address potential underlying causes.
- Gestational Diabetes in a Previous Pregnancy: This indicates a predisposition to developing gestational diabetes in future pregnancies.
Lifestyle and Environmental Factors
Certain aspects of a woman’s lifestyle and environment can also elevate pregnancy risk.
- Smoking, Alcohol, and Drug Use: These substances can have severe adverse effects on fetal development, leading to birth defects, low birth weight, premature birth, and even miscarriage or stillbirth.
- Poor Nutrition: Inadequate intake of essential nutrients can compromise fetal growth and development and impact maternal health.
- Exposure to Environmental Toxins: Exposure to certain chemicals, radiation, or infections can pose risks to the developing fetus.
- Obesity or Underweight: Both extremes of body weight can be associated with increased risks of gestational diabetes, preeclampsia, birth defects, and delivery complications.
- Stress: Chronic, high levels of stress can potentially affect pregnancy outcomes.
Multiple Gestations
Carrying twins, triplets, or more babies presents a unique set of challenges and significantly increases the risk profile of a pregnancy.
- Higher Rates of Preterm Birth: Multiple fetuses often lead to earlier labor and delivery.
- Increased Risk of Gestational Diabetes and Preeclampsia: The physiological demands on the mother’s body are substantially higher.
- Fetal Growth Discordance: In some cases, one or more fetuses may not grow at the same rate, requiring careful monitoring.
- Higher Likelihood of Cesarean Delivery: Due to the complexities of delivering multiple babies.
Monitoring and Management of High-Risk Pregnancies
Identifying a pregnancy as high-risk is not a cause for alarm but rather an indication for enhanced monitoring and tailored care to ensure the best possible outcomes for both mother and baby. The management of high-risk pregnancies involves a multidisciplinary approach, often requiring collaboration between obstetricians, maternal-fetal medicine specialists (perinatologists), neonatologists, genetic counselors, and other healthcare professionals.
Advanced Prenatal Screening and Diagnostics
For pregnancies identified as high-risk, particularly due to maternal age or family history, advanced screening and diagnostic tests are often recommended.
- Genetic Screening: Non-invasive prenatal testing (NIPT) using maternal blood can screen for common chromosomal abnormalities like Down syndrome. Other screening methods include ultrasound measurements (e.g., nuchal translucency) and biochemical markers.
- Diagnostic Genetic Testing: If screening tests indicate a higher risk, or if a woman desires definitive answers, diagnostic tests such as chorionic villus sampling (CVS) or amniocentesis can be performed to analyze fetal chromosomes.
- Detailed Ultrasound Examinations: Beyond routine anatomy scans, high-risk pregnancies may benefit from more frequent and detailed ultrasounds to monitor fetal growth, development, and well-being, including assessing placental function and amniotic fluid levels.
- Fetal Echocardiography: This specialized ultrasound focuses on the baby’s heart structure and function, recommended if there is a family history of congenital heart defects or if maternal conditions might affect fetal cardiac development.
Specialized Maternal Care
Women with high-risk pregnancies will often receive more frequent and specialized prenatal care.
- Frequent Medical Appointments: Regular check-ups allow for continuous monitoring of maternal health, including blood pressure, weight, and screening for gestational diabetes and preeclampsia.
- Medication Management: If pre-existing conditions are present, medications may need to be adjusted or prescribed specifically for pregnancy to manage them safely and effectively.
- Lifestyle Modifications: Healthcare providers will offer guidance on optimal nutrition, safe exercise, and the absolute avoidance of harmful substances like tobacco and alcohol.
- Monitoring Fetal Movement: Women may be advised to monitor fetal movements, reporting any significant decrease or change immediately.
Fetal Monitoring Techniques
Advanced technologies are used to assess fetal health and detect potential distress.
- Non-Stress Tests (NSTs): These tests monitor the baby’s heart rate in response to its own movements, assessing oxygenation.
- Biophysical Profiles (BPPs): This combines an NST with an ultrasound to evaluate fetal breathing, movement, muscle tone, and amniotic fluid volume, providing a comprehensive picture of fetal well-being.
- Doppler Ultrasound: This technique assesses blood flow in the umbilical cord and fetal blood vessels, helping to detect potential issues with placental function.

Delivery Planning
The birth plan for a high-risk pregnancy is often carefully orchestrated to ensure the safest possible delivery.
- Timing of Delivery: In some cases, if fetal well-being is compromised or maternal health is deteriorating, an earlier delivery might be recommended, either vaginally or via Cesarean section.
- Hospital Choice: Delivery at a hospital with a Level III or Level IV Neonatal Intensive Care Unit (NICU) is often recommended for high-risk pregnancies, ensuring immediate access to specialized care for newborns who may require it.
- Mode of Delivery: The decision for vaginal or Cesarean delivery is made based on a comprehensive assessment of risks and benefits, considering factors such as maternal health, fetal position, and the specific complications present.
In conclusion, while advanced maternal age is a significant demographic associated with increased pregnancy risks, it is one of many factors that define a high-risk pregnancy. A holistic approach, considering pre-existing medical conditions, reproductive history, lifestyle, and the presence of multiple gestations, is crucial. With diligent monitoring, advanced diagnostics, and personalized care plans, most high-risk pregnancies can achieve positive outcomes, ensuring the health and well-being of both mothers and their babies.
