Dysmotility refers to a broad spectrum of disorders characterized by abnormal or impaired movement within the body’s tubular organs, most commonly affecting the gastrointestinal tract. These conditions disrupt the coordinated muscular contractions, known as peristalsis, that are essential for propelling food, liquids, and waste through these passages. While “dysmotility” can technically apply to any organ with muscular tubing, its primary context in medical literature and patient discussions centers on the digestive system. Understanding dysmotility is crucial for diagnosing and managing a range of often debilitating symptoms that can significantly impact an individual’s quality of life.
The Mechanics of Normal Motility
To comprehend dysmotility, it’s vital to grasp the intricate mechanisms of normal motility. The gastrointestinal tract, from the esophagus to the anus, is lined with smooth muscle layers arranged in circular and longitudinal patterns. These muscles work in concert, guided by a complex interplay of neural and hormonal signals, to facilitate digestion and nutrient absorption.
Peristalsis: The Rhythmic Wave
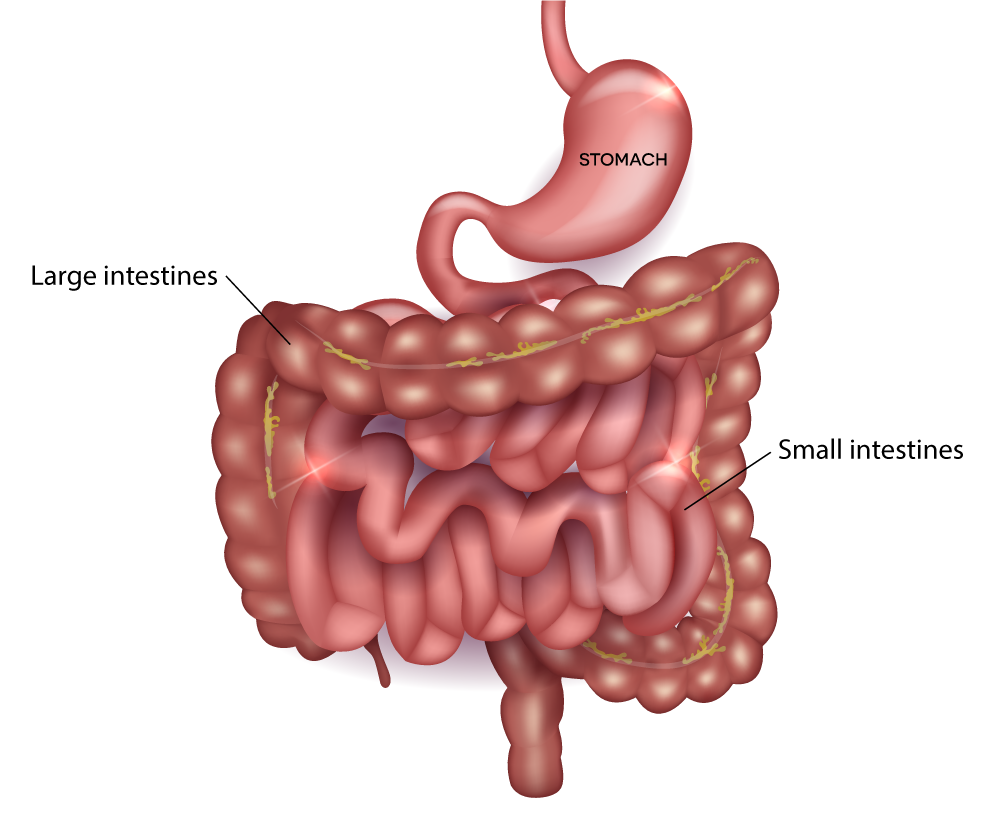
At the heart of gastrointestinal motility is peristalsis. This is a wave-like muscular contraction that pushes contents forward. In the esophagus, peristalsis transports food from the mouth to the stomach. In the stomach, it mixes food with digestive juices and empties its contents into the small intestine. The small intestine uses peristalsis for both mixing chyme with enzymes and propelling it towards the large intestine. The large intestine employs slower, more deliberate contractions for water absorption and forming stool, culminating in defecation.
Neural Control: The Enteric Nervous System
The gastrointestinal tract possesses its own intrinsic nervous system, often referred to as the “second brain” or the enteric nervous system (ENS). The ENS is a vast network of neurons embedded within the walls of the digestive tract that can operate independently of the central nervous system (CNS). It regulates muscle contractions, blood flow, and secretion. However, the ENS also receives input from the CNS via the vagus nerve and sympathetic nerves, allowing for integration of digestive processes with the body’s overall state.
Hormonal and Chemical Regulation
Beyond neural control, a symphony of hormones and chemical messengers plays a role in regulating motility. For instance, gastrin stimulates stomach acid secretion and motility, while secretin signals the pancreas to release bicarbonate to neutralize stomach acid in the small intestine. Other hormones like cholecystokinin (CCK) influence gallbladder contraction and pancreatic enzyme release, all of which indirectly impact gut movement.
Types and Manifestations of Dysmotility
Dysmotility disorders can manifest in various ways, depending on the affected segment of the gastrointestinal tract and the specific nature of the motility impairment. These impairments can involve either an overactivity or underactivity of muscle contractions.
Esophageal Dysmotility
Dysmotility in the esophagus can lead to difficulties swallowing (dysphagia), a feeling of food sticking in the throat or chest, and chest pain. Common esophageal motility disorders include:
- Achalasia: Characterized by the failure of the lower esophageal sphincter (LES) to relax properly and absent peristalsis in the esophageal body. This obstructs the passage of food into the stomach.
- Diffuse Esophageal Spasm (DES): Involves uncoordinated and excessively strong contractions of the esophagus, which can cause severe chest pain and difficulty swallowing.
- Nutcracker Esophagus (Hypertensive Peristalsis): Defined by high-amplitude, coordinated peristaltic contractions that can still cause significant dysphagia and chest pain.
- Scleroderma Esophagus: A form of esophageal dysmotility often seen in patients with systemic sclerosis, characterized by weak, ineffective peristalsis and a relaxed LES, leading to reflux and dysphagia.
Gastric Dysmotility (Gastroparesis)
Gastroparesis, or delayed gastric emptying, is a primary form of gastric dysmotility. It is characterized by symptoms such as nausea, vomiting, early satiety (feeling full quickly), abdominal pain, bloating, and unintentional weight loss. The impaired movement of food from the stomach to the small intestine can be caused by damage to the nerves or muscles of the stomach.
- Idiopathic Gastroparesis: In many cases, the cause of gastroparesis remains unknown.
- Diabetic Gastroparesis: A common complication of long-standing diabetes, where high blood sugar levels can damage the vagus nerve, which controls stomach muscles.
- Post-surgical Gastroparesis: Can occur after surgery on the stomach, esophagus, or vagus nerve.
- Medication-induced Gastroparesis: Certain drugs, particularly opioids and some antidepressants, can slow down gastric emptying.
Small and Large Intestinal Dysmotility
Dysmotility in the small and large intestines can lead to a wide range of symptoms, often mimicking other functional gastrointestinal disorders.
- Irritable Bowel Syndrome (IBS): While often considered a functional disorder, evidence suggests that underlying dysmotility plays a significant role in the altered bowel habits (diarrhea, constipation, or mixed) and abdominal pain experienced by IBS patients.
- Chronic Intestinal Pseudo-obstruction (CIPO): A rare and severe condition where the intestines exhibit symptoms of obstruction without any physical blockage. This is due to severe dysmotility, leading to abdominal distension, pain, nausea, vomiting, and malabsorption. CIPO can be congenital or acquired.
- Constipation: Can be a symptom of colonic dysmotility, where the muscles of the colon contract too weakly or infrequently to effectively move stool through the bowel.
- Diarrhea: Can also be associated with dysmotility, particularly if there is rapid transit of intestinal contents, preventing adequate water absorption.
Causes and Risk Factors for Dysmotility

The underlying causes of dysmotility are diverse and can range from specific diseases to unknown factors.
Neurological and Muscular Disorders
Direct damage or dysfunction of the nerves controlling gut motility, or the smooth muscle tissue itself, is a common culprit.
- Diabetes Mellitus: As mentioned, long-term diabetes is a leading cause of gastroparesis and can affect other parts of the GI tract.
- Parkinson’s Disease and Multiple Sclerosis: These neurological conditions can impact the ENS and central nervous system control of gut motility.
- Amyloidosis: The buildup of abnormal proteins in organ tissues, including the GI tract, can impair muscle function.
- Scleroderma: An autoimmune disease that causes thickening and hardening of connective tissues, often affecting the esophagus and intestines.
Medications
A significant number of medications can interfere with gastrointestinal motility.
- Opioid Analgesics: These drugs are well-known for their ability to slow down bowel movements.
- Anticholinergic Medications: Used for conditions like overactive bladder or COPD, these drugs can reduce muscle contractions in the gut.
- Calcium Channel Blockers: While primarily used for cardiovascular conditions, they can sometimes affect GI motility.
- Certain Antidepressants: Especially tricyclic antidepressants, can have anticholinergic effects that impact the gut.
Surgical Interventions
Procedures involving the digestive system, particularly those that affect the vagus nerve or involve significant manipulation of the bowel, can sometimes lead to dysmotility.
- Gastric Surgery: Procedures like gastrectomies or fundoplications can alter normal stomach emptying.
- Esophageal Surgery: Operations on the esophagus can impact its muscular function.
- Bariatric Surgery: While often aimed at weight loss, certain types of bariatric surgery can influence GI transit times.
Infections and Inflammation
Certain infections and inflammatory processes can temporarily or permanently damage the ENS or smooth muscle.
- Viral Gastroenteritis: While usually self-limiting, severe episodes can sometimes trigger persistent motility issues.
- Inflammatory Bowel Disease (IBD): Conditions like Crohn’s disease and ulcerative colitis can cause inflammation that leads to altered motility, although dysmotility is not the primary defining feature.
Idiopathic Dysmotility
In a substantial proportion of cases, the cause of dysmotility remains elusive, leading to the diagnosis of idiopathic dysmotility. Research continues to explore genetic predispositions, subtle immune system dysregulation, and environmental factors that may contribute to these unexplained cases.
Diagnosis and Management of Dysmotility
Diagnosing dysmotility involves a comprehensive approach, including medical history, physical examination, and specialized diagnostic tests. Management strategies aim to alleviate symptoms, improve nutrition, and, where possible, address the underlying cause.
Diagnostic Tools
- Esophageal Manometry: Measures the pressure and coordination of muscle contractions in the esophagus and the function of the LES.
- Gastric Emptying Studies: Radioactive or non-radioactive tests that track the rate at which food leaves the stomach.
- Wireless Motility Capsule (SmartPill): A small, ingestible capsule that measures pressure, pH, and temperature as it travels through the GI tract, providing detailed information about transit times in different segments.
- Barium Swallow/Upper GI Series: X-ray imaging after swallowing barium contrast to visualize the esophagus, stomach, and small intestine.
- Colon Transit Study: Assesses how quickly material moves through the colon, often using radiopaque markers.
- Endoscopy: While not directly measuring motility, endoscopy can rule out structural abnormalities like strictures or tumors that might mimic dysmotility symptoms and can also be used for biopsies to assess nerve or muscle integrity.
Treatment Modalities
The treatment of dysmotility is highly individualized and depends on the specific diagnosis and the severity of symptoms.
- Dietary Modifications: Adjusting meal size, frequency, and texture of food can significantly improve symptoms. For gastroparesis, small, frequent meals of low-fat, low-fiber foods are often recommended.
- Medications:
- Prokinetics: Drugs that enhance GI motility, such as metoclopramide or domperidone (where available), can be prescribed to stimulate contractions.
- Anti-emetics: Medications to control nausea and vomiting.
- Pain relievers: For abdominal pain management.
- Laxatives or stool softeners: For constipation.
- Nutritional Support: In severe cases, individuals may require parenteral (intravenous) or enteral (tube feeding) nutrition to ensure adequate caloric and nutrient intake.
- Surgery: In rare, severe cases of gastroparesis or CIPO that are refractory to medical treatment, surgical options like gastric electrical stimulation (gastric pacing) or feeding tube placement might be considered.
- Lifestyle Adjustments: Avoiding trigger foods, managing stress, and regular, gentle exercise can also play a supportive role in managing dysmotility symptoms.
Understanding dysmotility is a journey into the complex mechanics of the digestive system. While the term itself may sound technical, it encapsulates a range of conditions that profoundly affect how our bodies process food, influencing everything from nutrient absorption to daily comfort. Continued research and evolving diagnostic techniques offer hope for more precise understanding and effective management of these challenging motility disorders.
