Understanding the Basics of Axillary Temperature Measurement
Axillary temperature, often referred to as underarm temperature, is a method of taking a person’s body temperature by placing a thermometer in the armpit. While it is a common and accessible way to monitor body temperature, it’s important to understand its nuances, advantages, and limitations compared to other measurement methods. This form of temperature taking is particularly favored for infants and young children due to its non-invasive nature and ease of use.
The Physiology Behind Axillary Temperature
The human body maintains a core temperature that is crucial for the proper functioning of its organs and metabolic processes. This core temperature is tightly regulated by the hypothalamus, a region in the brain. When the body’s internal temperature deviates from its set point, mechanisms are activated to either generate or dissipate heat.

The axilla, or armpit, is an area of the body where blood vessels are close to the surface of the skin. This proximity allows for a reading that can reflect the body’s internal temperature. However, the axilla is an external body cavity, meaning the temperature measured here is typically lower than the body’s core temperature. This is because the armpit is exposed to the ambient air, and heat can be lost to the environment. Therefore, axillary temperatures are generally considered less accurate and reliable for reflecting true core body temperature compared to oral, rectal, or ear measurements.
How to Take an Axillary Temperature
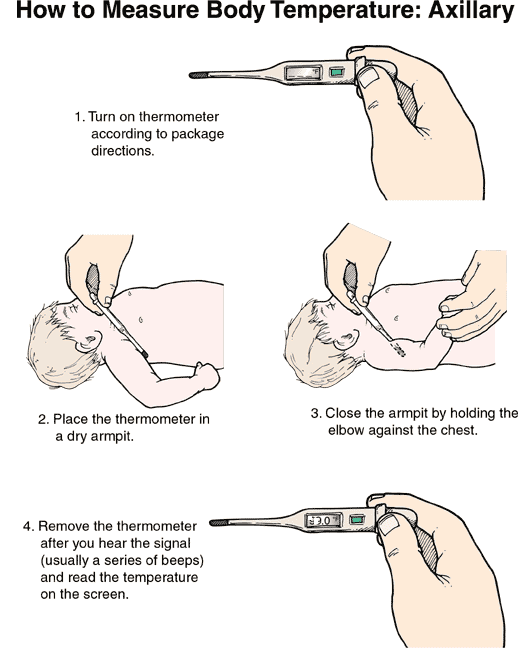
Taking an axillary temperature is a straightforward process that requires a few simple steps:
-
Clean the Thermometer: Before and after each use, clean the thermometer with soap and cool water, or by using an alcohol wipe. If using a digital thermometer, ensure the probe cover is clean or replace it if necessary.
-
Ensure the Armpit is Dry: For an accurate reading, the armpit should be dry. Gently pat it with a clean towel or cloth to remove any sweat or moisture. Moisture can interfere with the thermometer’s ability to make good contact with the skin, leading to an inaccurate reading.
-
Position the Thermometer:
- For mercury or glass thermometers: Place the bulb of the thermometer firmly in the center of the dry armpit, ensuring it touches the skin.
- For digital thermometers: Place the tip of the thermometer probe in the center of the dry armpit, ensuring it touches the skin.
-
Lower the Arm: Once the thermometer is in place, lower the arm down against the side of the body. This action helps to create a closed pocket, trapping heat and ensuring the thermometer is held securely against the skin. The arm should remain relaxed and close to the body for the duration of the measurement.
-
Wait for the Reading:
- Mercury or glass thermometers: These typically require 3 to 5 minutes to obtain an accurate reading. You will need to read the temperature at the mercury line.
- Digital thermometers: These usually beep when the reading is complete, which typically takes between 10 seconds to 1 minute. Follow the manufacturer’s instructions for your specific digital thermometer.
-
Record the Temperature: Once the measurement is complete, remove the thermometer and read the temperature. Record the reading, noting the time and date.
-
Clean the Thermometer Again: After use, clean the thermometer thoroughly as per the manufacturer’s instructions.
Advantages of Axillary Temperature Measurement
Despite its limitations, axillary temperature measurement offers several benefits:
-
Non-Invasive and Comfortable: This is arguably the biggest advantage. It does not require insertion into a bodily orifice, making it the preferred method for infants, young children, and individuals who are uncooperative or uncomfortable with other methods. The gentle nature of the procedure minimizes distress.
-
Ease of Use: The process is simple and can be easily performed by parents, caregivers, or individuals themselves without specialized training.
-
Safety: It eliminates the risks associated with rectal thermometers, such as perforation or discomfort. For those concerned about the potential breakage of glass thermometers, digital options are readily available and safe for axillary use.
-
Accessibility: All that is needed is a thermometer and a dry armpit. This makes it a convenient option in various settings, from home to clinical environments where other specialized equipment might be unavailable.
-
Reduced Risk of Infection: As it’s an external measurement, the risk of transmitting infections between individuals is significantly lower compared to methods involving internal probes, provided the thermometer is cleaned appropriately.
Limitations of Axillary Temperature Measurement
It is crucial to be aware of the drawbacks of axillary temperature measurement to interpret the readings accurately:

-
Lower Accuracy: Axillary temperatures are generally lower than core body temperatures. This is because the armpit is an external area exposed to the environment, leading to heat dissipation. A reading of 97.6°F (36.4°C) axillary might be considered normal, whereas the same temperature orally would be considered low.
-
Variability: Readings can be significantly influenced by external factors such as ambient room temperature, how tightly the arm is held against the body, and the presence of sweat or moisture. This makes readings less consistent and harder to rely on for precise diagnosis.
-
Longer Measurement Time (for some thermometers): While digital thermometers are quick, traditional mercury or glass thermometers require a longer waiting period (3-5 minutes) to obtain a reading, which can be challenging with restless children.
-
Not Ideal for Rapid Fever Detection: Due to the lag in temperature reflection from the core to the axilla, axillary measurements may not be the best choice for quickly identifying a rapidly rising fever.
-
Requires Patient Cooperation: While less invasive, the patient still needs to hold their arm still for a period to ensure an accurate reading, which can be difficult for very young or active individuals.
Normal Axillary Temperature Ranges and Interpretation
Interpreting axillary temperatures requires an understanding of their typical range and how they compare to other measurement sites. A normal axillary temperature is generally considered to be between 97.6°F (36.4°C) and 99.6°F (37.6°C).
However, it’s important to note that:
- Axillary readings are typically 0.5°F to 1°F (0.3°C to 0.6°C) lower than oral readings.
- Axillary readings are typically 1°F to 2°F (0.6°C to 1.2°C) lower than rectal readings.
When using axillary temperature to assess for fever, healthcare professionals often consider a temperature of 100.4°F (38°C) or higher as a sign of fever, though this can vary depending on the patient’s age and overall condition. It is crucial to consider the child’s overall well-being. A child with an axillary temperature of 99.5°F (37.5°C) who is lethargic, irritable, or showing other signs of illness might warrant medical attention, while a child with the same temperature who is active and well may not.
When in doubt, or if you suspect a fever, it is always best to consult a healthcare provider. They may recommend using a different method of temperature measurement for a more accurate assessment, especially for infants and young children.
When is Axillary Temperature the Preferred Method?
Given its characteristics, axillary temperature measurement is often the preferred method in specific scenarios:
-
Infants and Young Children: For babies and toddlers, the non-invasive nature of axillary temperature taking is a significant advantage, reducing anxiety and discomfort for both the child and the caregiver.
-
Individuals with Special Needs: People with developmental disabilities, cognitive impairments, or those who are generally uncooperative may find axillary temperature measurement to be the most feasible and least distressing option.
-
Routine Screening: For general health monitoring or initial screening where an exact core temperature is not immediately critical, axillary temperature can provide a baseline indication of whether further investigation is needed.
-
Post-Surgical Patients: In some post-operative cases, avoiding invasive procedures might be a priority, making axillary temperature a suitable alternative for monitoring.
-
When Other Methods Are Contraindicated: If a person has a nasal injury, has recently eaten or drunk something hot or cold (for oral readings), or has earwax buildup (for ear readings), axillary temperature might be the safest and most practical alternative.
Comparing Axillary Temperature to Other Methods
Understanding how axillary temperature compares to other common methods provides a clearer picture of its utility:
-
Oral Temperature: Measured under the tongue, oral temperature is generally considered more accurate than axillary. However, it requires the person to keep their mouth closed and refrain from eating or drinking for a period before and during measurement. It is not suitable for infants, unconscious individuals, or those with breathing difficulties.
-
Rectal Temperature: This is considered the most accurate method for measuring core body temperature, especially in infants and young children. It involves inserting a lubricated thermometer into the rectum. While highly accurate, it is invasive and can be uncomfortable or distressing.
-
Tympanic (Ear) Temperature: Measured in the ear canal, this method provides a quick reading that is close to core body temperature. However, accuracy can be affected by earwax buildup, ear infections, or improper insertion. It’s not recommended for infants under 3 months old.
-
Temporal Artery (Forehead) Temperature: These thermometers scan the forehead and are very quick and non-invasive. They are generally reliable but can be affected by sweat, ambient temperature, and the correct placement of the scanner.
In summary, while axillary temperature measurement is a convenient and accessible method, its readings are generally lower and less precise than core body temperature measurements. It is best used as an initial screening tool or when other methods are not feasible or appropriate, always keeping in mind its inherent limitations when interpreting the results.
