Endocrinology, a specialized branch of medicine, focuses on the intricate network of glands and hormones that govern a vast array of bodily functions. An endocrinology doctor, or endocrinologist, is a medical physician who dedicates their expertise to diagnosing and treating conditions related to the endocrine system. This system is a complex communication network, with hormones acting as chemical messengers that travel through the bloodstream to regulate processes such as metabolism, growth and development, tissue function, sexual function, reproduction, sleep, and mood.
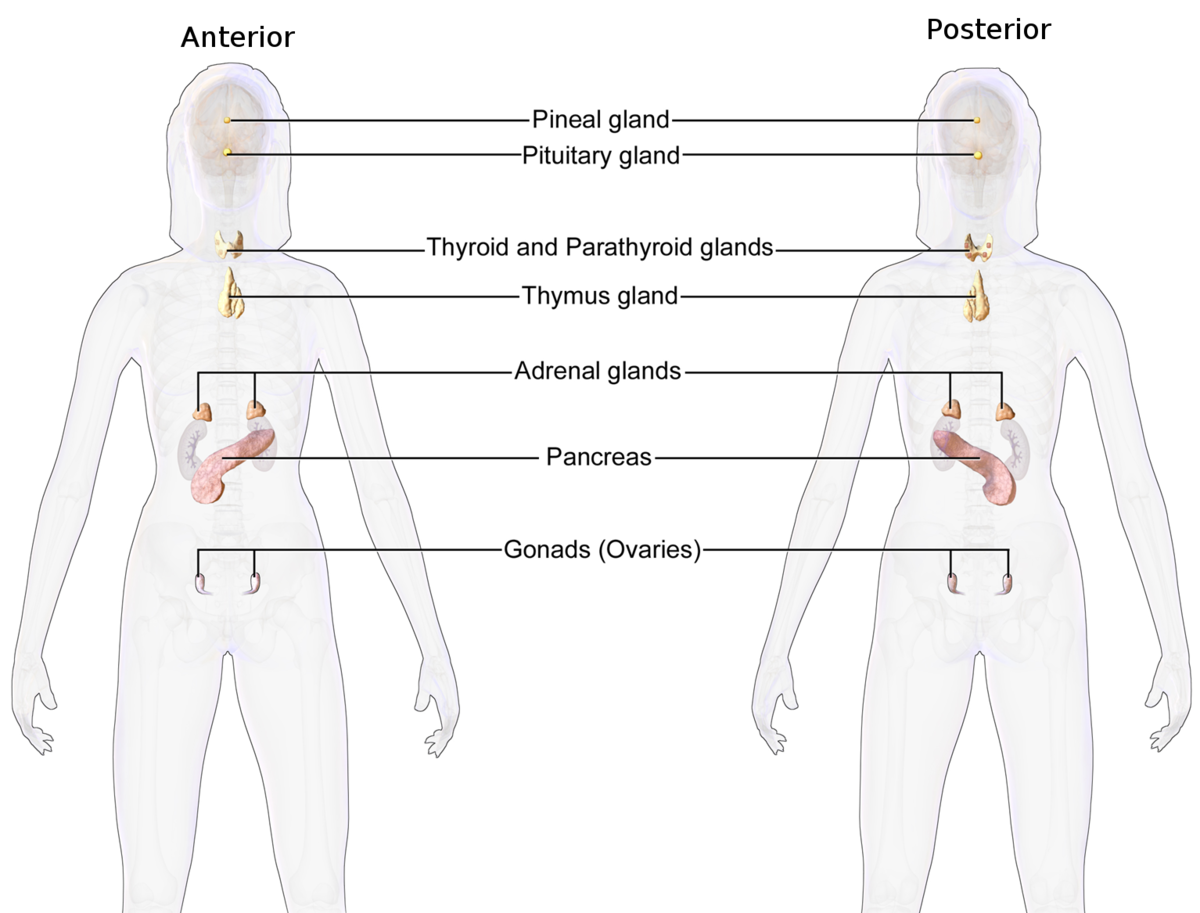
The endocrine system comprises several glands, each producing specific hormones that have far-reaching effects. Key glands include the hypothalamus and pituitary gland in the brain, the thyroid and parathyroid glands in the neck, the adrenal glands located atop the kidneys, the pancreas within the abdomen, and the ovaries and testes in the reproductive system. When these glands produce too much or too little of a particular hormone, or when hormone receptors malfunction, a spectrum of health issues can arise. Endocrinologists are the specialists equipped to unravel these complex hormonal imbalances and devise effective treatment strategies.

The Scope of Endocrinology
The practice of endocrinology is remarkably broad, encompassing a multitude of conditions that affect people of all ages. From common ailments to rare genetic disorders, the endocrinologist’s diagnostic toolkit and therapeutic approaches are essential for maintaining overall health and well-being. Their work is crucial for managing chronic diseases and improving the quality of life for millions of individuals worldwide.
Diabetes Mellitus
Perhaps the most widely recognized condition treated by endocrinologists is diabetes mellitus. This chronic metabolic disorder is characterized by elevated levels of glucose (sugar) in the blood. There are several types of diabetes, including Type 1, Type 2, and gestational diabetes, each with distinct causes and management protocols.
Type 1 Diabetes
Type 1 diabetes is an autoimmune condition where the body’s immune system mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. Insulin is a vital hormone that helps glucose from food move from the bloodstream into cells to be used for energy. Without sufficient insulin, glucose builds up in the blood, leading to hyperglycemia. Endocrinologists manage Type 1 diabetes by prescribing insulin therapy, often through injections or an insulin pump, and educating patients on blood glucose monitoring, diet, and exercise.
Type 2 Diabetes
Type 2 diabetes is the most common form, accounting for approximately 90-95% of all diabetes cases. It is characterized by insulin resistance, where the body’s cells do not respond effectively to insulin, and eventually, the pancreas may not produce enough insulin to keep blood glucose levels normal. Risk factors for Type 2 diabetes include genetics, obesity, physical inactivity, and age. Treatment typically involves lifestyle modifications such as diet and exercise, oral medications to improve insulin sensitivity or production, and in some cases, insulin therapy.
Gestational Diabetes
Gestational diabetes develops during pregnancy in women who did not have diabetes before. It poses risks to both the mother and the baby, including an increased chance of cesarean delivery, high blood pressure for the mother, and developmental issues for the baby. Endocrinologists monitor and manage gestational diabetes, often through diet and exercise, and may prescribe medication if necessary to control blood glucose levels.
Thyroid Disorders
The thyroid gland, located in the neck, produces thyroid hormones (thyroxine or T4 and triiodothyronine or T3) that regulate metabolism, influencing heart rate, body temperature, and energy levels. Dysfunction of this gland can lead to a range of problems.
Hypothyroidism
Hypothyroidism occurs when the thyroid gland does not produce enough thyroid hormones. This can lead to a slowed metabolism, causing symptoms such as fatigue, weight gain, feeling cold, dry skin, constipation, and depression. The most common cause of hypothyroidism in many parts of the world is Hashimoto’s thyroiditis, an autoimmune disease. Treatment involves hormone replacement therapy with synthetic thyroid hormone (levothyroxine).
Hyperthyroidism
Hyperthyroidism, conversely, is a condition where the thyroid gland produces too much thyroid hormone. This speeds up the body’s metabolism, leading to symptoms like weight loss, rapid or irregular heartbeat, nervousness, irritability, tremors, increased sweating, and difficulty sleeping. Graves’ disease is the most common cause of hyperthyroidism. Treatment options include anti-thyroid medications, radioactive iodine therapy to destroy overactive thyroid cells, or surgery to remove part or all of the thyroid gland.
Thyroid Nodules and Cancer
Endocrinologists also evaluate and manage thyroid nodules, which are lumps that can form in the thyroid gland. While most thyroid nodules are benign (non-cancerous), some can be cancerous. They use imaging techniques like ultrasound and fine-needle aspiration biopsy to diagnose thyroid nodules and cancer. If cancer is detected, they coordinate treatment, which often involves surgery, radioactive iodine therapy, and hormone suppression.
Adrenal Gland Disorders
The adrenal glands, situated atop the kidneys, produce a variety of essential hormones, including cortisol, aldosterone, and adrenaline. These hormones play critical roles in stress response, blood pressure regulation, metabolism, and the balance of electrolytes like sodium and potassium.
Cushing’s Syndrome
Cushing’s syndrome is a condition caused by prolonged exposure to high levels of cortisol. This can be due to the body producing too much cortisol, or from taking corticosteroid medications. Symptoms include weight gain (particularly in the face and abdomen), thin and easily bruised skin, stretch marks, high blood pressure, and muscle weakness. Treatment aims to reduce cortisol levels through medication, surgery, or radiation, depending on the underlying cause.

Addison’s Disease
Addison’s disease, also known as primary adrenal insufficiency, occurs when the adrenal glands do not produce enough cortisol and often aldosterone. This can lead to fatigue, muscle weakness, weight loss, low blood pressure, and skin darkening. It is typically an autoimmune condition. Treatment involves hormone replacement therapy with corticosteroids and mineralocorticoids.
Pheochromocytoma
Pheochromocytomas are rare tumors that develop in the adrenal medulla, the inner part of the adrenal gland. These tumors produce excessive amounts of adrenaline and noradrenaline, leading to episodes of very high blood pressure, headaches, palpitations, and sweating. Surgical removal of the tumor is the primary treatment.
Reproductive Endocrinology
Reproductive endocrinology focuses on the hormonal aspects of reproduction in both males and females. This includes issues related to puberty, fertility, and menopause.
Polycystic Ovary Syndrome (PCOS)
PCOS is a common hormonal disorder among women of reproductive age. It is characterized by irregular menstrual periods, excess androgens (male hormones) which can cause symptoms like acne and excess facial or body hair, and polycystic ovaries (ovaries containing numerous small follicles). PCOS can also contribute to insulin resistance and increase the risk of Type 2 diabetes and cardiovascular disease. Management often involves lifestyle changes, hormonal birth control pills, and medications to address insulin resistance.
Infertility
Endocrinologists play a vital role in diagnosing and treating infertility. They investigate hormonal imbalances that can affect ovulation in women or sperm production in men. This may involve testing hormone levels, performing diagnostic imaging, and recommending treatments such as ovulation induction medications or surgery.
Menopause and Hormone Replacement Therapy (HRT)
Menopause marks the end of a woman’s reproductive years, characterized by a decline in estrogen and progesterone production. This can lead to symptoms like hot flashes, vaginal dryness, mood changes, and bone loss. Endocrinologists can help manage these symptoms through hormone replacement therapy (HRT), carefully weighing the benefits and risks for each individual.
Growth Disorders
The pituitary gland, often referred to as the “master gland,” plays a crucial role in regulating growth and development through the production of growth hormone (GH).
Growth Hormone Deficiency
In children, a deficiency in growth hormone can lead to stunted growth and short stature. Endocrinologists diagnose this condition and can prescribe synthetic growth hormone therapy to promote normal growth. In adults, growth hormone deficiency can manifest as fatigue, decreased muscle mass, and changes in body composition.
Acromegaly and Gigantism
Conversely, an overproduction of growth hormone, usually due to a pituitary tumor, can cause acromegaly in adults and gigantism in children. Acromegaly is characterized by the enlargement of hands, feet, and facial features. Gigantism results in excessive height. Treatment typically involves surgery to remove the tumor, radiation therapy, or medications to control hormone levels.
The Role of the Endocrinologist in Patient Care
An endocrinologist’s approach to patient care is comprehensive and highly individualized. It begins with a detailed medical history and physical examination, followed by targeted diagnostic tests.
Diagnosis and Testing
Diagnostic tools employed by endocrinologists are diverse and include:
- Blood Tests: To measure hormone levels, glucose levels, cholesterol, and other metabolic markers.
- Urine Tests: To assess hormone excretion and kidney function.
- Imaging Studies: Ultrasound, CT scans, and MRI scans are used to visualize endocrine glands and detect tumors or abnormalities.
- Stimulation and Suppression Tests: These tests help determine how the endocrine glands respond to specific stimuli, providing insights into their function.
- Genetic Testing: For inherited endocrine disorders.
Treatment and Management
Once a diagnosis is established, the endocrinologist develops a personalized treatment plan. This may involve:
- Medications: A wide range of pharmaceutical interventions are used to correct hormone imbalances, manage symptoms, and prevent complications.
- Hormone Replacement Therapy: Administering synthetic hormones to compensate for deficiencies.
- Lifestyle Modifications: Guidance on diet, exercise, and stress management is often integral to treatment, particularly for conditions like diabetes and obesity.
- Surgery and Radiation Therapy: For conditions involving tumors of endocrine glands.
- Patient Education: A cornerstone of endocrinology is empowering patients with knowledge about their condition, treatment, and self-management strategies. Regular follow-up appointments are crucial for monitoring progress, adjusting treatment, and addressing any emerging concerns.
In essence, an endocrinology doctor is a highly specialized physician who navigates the complex world of hormones and glands to diagnose, treat, and manage a vast spectrum of endocrine disorders. Their expertise is vital for maintaining hormonal balance and ensuring the optimal functioning of the human body.
