An apnea event refers to a pause in breathing that occurs during sleep. This temporary cessation of airflow can range in duration from a few seconds to over a minute and can happen multiple times throughout the night. While occasional brief pauses are normal, frequent or prolonged apnea events can be indicative of a serious sleep disorder known as sleep apnea. Understanding the nature of these events, their causes, and their implications is crucial for diagnosing and managing this condition, which can significantly impact overall health and well-being.
The term “apnea” originates from the Greek word “apnoia,” meaning “want of breath.” In the context of sleep, an apnea event is characterized by a complete or near-complete absence of breathing. This interruption in airflow can be detected and measured through various diagnostic methods, primarily polysomnography (PSG), also known as a sleep study. During a PSG, sensors are attached to the body to monitor respiratory effort, airflow, oxygen saturation, brain activity, heart rate, and body movements.
Types of Apnea Events
Apnea events are broadly classified into three main categories, distinguished by their underlying physiological mechanisms:
Obstructive Sleep Apnea (OSA) Events
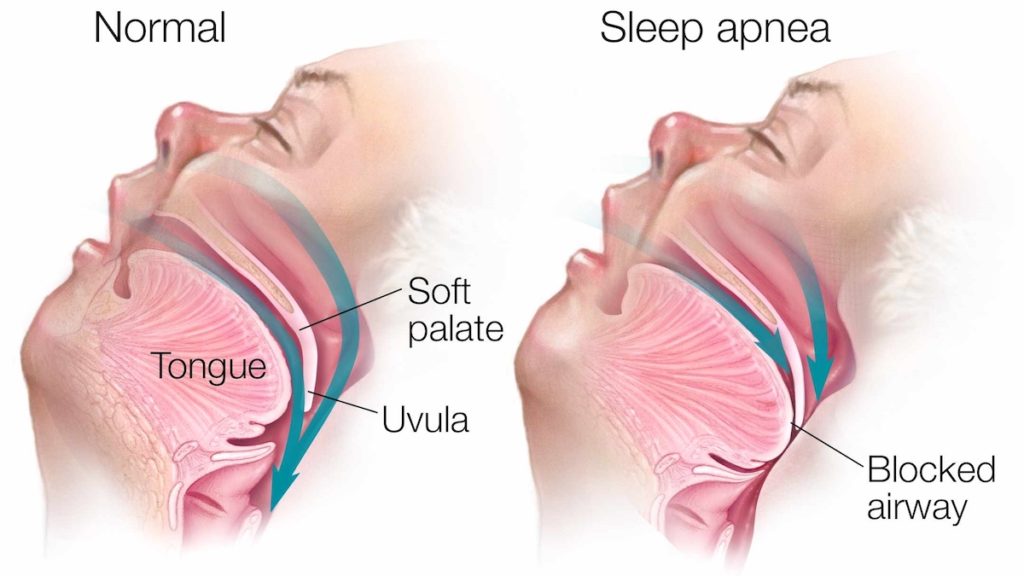
Obstructive sleep apnea events are the most common type and occur when the upper airway becomes physically blocked during sleep. This blockage prevents air from reaching the lungs, even though the individual is still making an effort to breathe.
Mechanism of Obstruction
The primary cause of airway obstruction in OSA is the relaxation of the muscles in the throat during sleep. As these muscles relax, the soft tissues in the back of the throat, including the soft palate, uvula, tongue, and tonsils, can collapse and narrow or completely block the airway. Factors that contribute to this collapse include:
- Excess Body Weight and Obesity: Adipose tissue deposited around the neck can compress the airway, making it more prone to collapse.
- Anatomical Features: A large tongue, a small jaw, enlarged tonsils or adenoids, or a naturally narrow airway can increase the risk.
- Age: The prevalence of OSA increases with age, as muscle tone generally decreases.
- Gender: Men are more commonly diagnosed with OSA than women, though this gap narrows after menopause.
- Alcohol and Sedative Use: These substances further relax throat muscles, exacerbating the risk.
- Smoking: Inflammation and fluid retention in the airway due to smoking can contribute to obstruction.
When an OSA event occurs, the brain detects the lack of oxygen and the buildup of carbon dioxide. This triggers a brief arousal from sleep, often not consciously remembered, which causes the individual to momentarily gasp for air or shift position. This brief arousal helps to reopen the airway, allowing breathing to resume. These arousals, though short, fragment sleep and prevent restorative deep sleep.
Central Sleep Apnea (CSA) Events
Central sleep apnea events are less common than OSA and occur when the brain fails to send the proper signals to the muscles that control breathing. In this case, the airway is typically not blocked, but the respiratory effort itself is reduced or absent.
Neurological Basis of CSA
CSA is essentially a problem with the central nervous system’s control over the respiratory system. The brainstem, which regulates breathing, may not function optimally, leading to intermittent pauses in respiratory drive. Several conditions can lead to CSA:
- Heart Failure: Congestive heart failure is a significant cause of CSA, often referred to as Cheyne-Stokes respiration, a characteristic pattern of breathing that alternates between hyperventilation and apnea. This is thought to be due to a delay in the blood circulation time and the lung-brain feedback loop.
- Stroke or Brain Injury: Damage to the brainstem or other areas involved in respiratory control can result in CSA.
- High Altitude: At high altitudes, changes in blood gas levels can sometimes trigger CSA.
- Opioid Medications: Certain pain medications, particularly opioids, can suppress respiratory drive and lead to CSA.
- Sleep Apnea Treatment: Paradoxically, some individuals may develop CSA after being treated for OSA with positive airway pressure (PAP) therapy if the underlying CSA is not also addressed.
In CSA events, there is a lack of respiratory effort. The individual may remain still, and the absence of struggling to breathe is a key distinguishing feature from OSA. Similar to OSA, these events can lead to reduced oxygen levels and sleep disruption.
Mixed or Complex Sleep Apnea Events
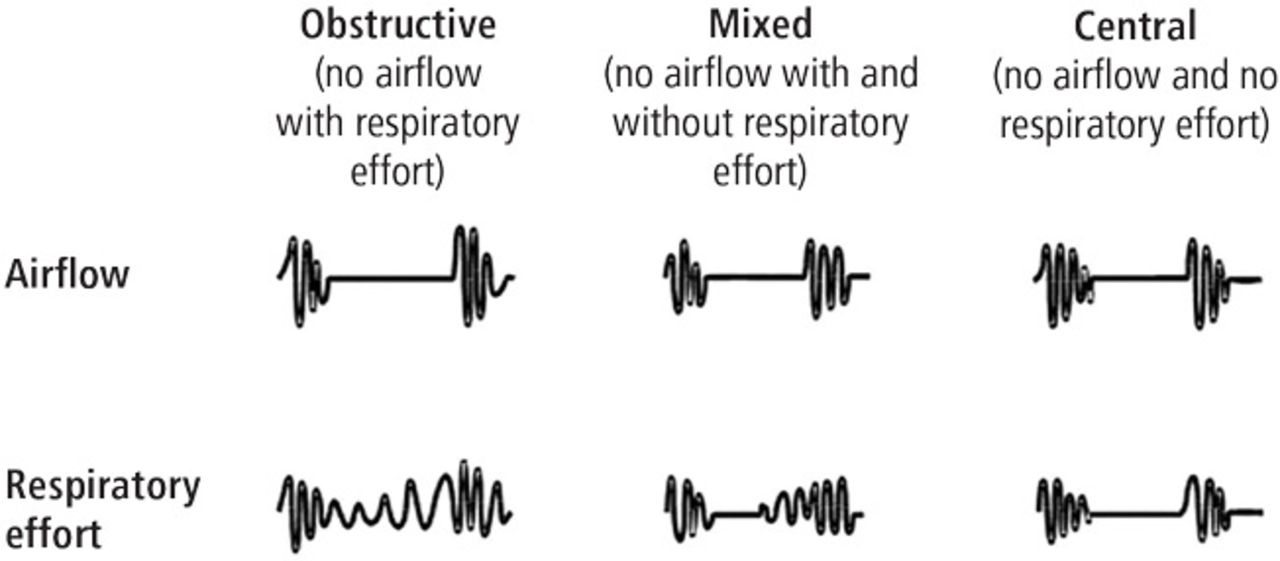
Mixed sleep apnea, also known as complex sleep apnea, is a combination of both obstructive and central sleep apnea events. It typically begins as an obstructive event, with the airway becoming blocked, but then transitions into a central event where the brain temporarily stops signaling for breathing.
The Transition Phenomenon
The development of mixed sleep apnea can be complex. In some cases, individuals who are treated for OSA with PAP therapy may develop CSA. This phenomenon, sometimes termed “treatment-emergent central sleep apnea,” suggests that the positive pressure, while effectively opening the airway, can sometimes disrupt the delicate feedback mechanisms that regulate breathing. The continuous positive airway pressure might, in certain individuals, lead to a situation where the brain overcompensates, temporarily halting respiratory drive.
The diagnosis of mixed sleep apnea requires careful evaluation during a sleep study to identify the presence and proportion of both obstructive and central events. The management strategy for mixed sleep apnea is often tailored to the dominant type of event or may involve more complex treatment approaches.
Consequences of Apnea Events
Regardless of the type, frequent and significant apnea events during sleep can have profound negative consequences on an individual’s health. The repeated episodes of oxygen deprivation (hypoxia) and the fragmented sleep pattern disrupt the body’s normal functioning.
Physiological Impacts
- Cardiovascular Strain: The recurrent drops in blood oxygen levels and the surges in heart rate and blood pressure during arousals place significant strain on the cardiovascular system. This increases the risk of hypertension, heart attack, stroke, arrhythmias, and heart failure.
- Metabolic Disturbances: Sleep apnea is linked to insulin resistance, type 2 diabetes, and metabolic syndrome. The stress on the body from disrupted sleep and oxygen deprivation can interfere with hormone regulation and glucose metabolism.
- Cognitive Impairment: Chronic sleep fragmentation and hypoxia can impair cognitive functions such as memory, concentration, attention, and decision-making. This can lead to daytime sleepiness, reduced productivity, and an increased risk of accidents.
- Respiratory Issues: While primarily a breathing disorder, the chronic stress on the respiratory system can exacerbate existing lung conditions or contribute to the development of pulmonary hypertension.
- Hormonal Imbalances: Sleep plays a critical role in the regulation of various hormones, including growth hormone, cortisol, and appetite-regulating hormones. Disrupted sleep due to apnea events can lead to imbalances in these hormones, affecting mood, energy levels, and weight management.
Impact on Quality of Life
Beyond the direct physiological impacts, apnea events can severely diminish an individual’s quality of life.
- Excessive Daytime Sleepiness (EDS): This is one of the most common and debilitating symptoms of sleep apnea. Individuals may feel excessively tired throughout the day, leading to difficulties in daily activities, work, and social interactions.
- Morning Headaches: The fluctuating oxygen and carbon dioxide levels during the night can lead to headaches upon waking.
- Mood Disturbances: Chronic sleep deprivation and the stress associated with apnea events can contribute to irritability, anxiety, and depression.
- Relationship Strain: Loud snoring, gasping for air, and restless sleep can disrupt the sleep of bed partners, leading to strain on relationships.
- Reduced Libido: Fatigue, hormonal changes, and the general impact on well-being can lead to a decreased sex drive.
Diagnosis and Management
The diagnosis of apnea events and the underlying sleep apnea condition relies on a comprehensive evaluation, typically starting with a physician’s assessment of symptoms and medical history.
Diagnostic Tools
- Polysomnography (PSG): As mentioned earlier, a full-night PSG is the gold standard for diagnosing sleep apnea. It provides detailed data on breathing patterns, oxygen levels, brain activity, and other physiological parameters to identify and quantify apnea events.
- Home Sleep Apnea Testing (HSAT): For individuals with a high probability of moderate to severe OSA and no significant co-existing medical conditions, a HSAT may be used. These devices monitor fewer parameters than a PSG but can effectively detect significant breathing disruptions.

Treatment Strategies
The management of apnea events is aimed at preventing airway obstruction or stimulating proper respiratory drive to ensure continuous breathing during sleep.
- Positive Airway Pressure (PAP) Therapy: This is the most common and effective treatment for OSA and often for mixed sleep apnea. Devices like CPAP (Continuous Positive Airway Pressure), BiPAP (Bilevel Positive Airway Pressure), and APAP (Automatic Positive Airway Pressure) deliver pressurized air through a mask worn during sleep, keeping the airway open.
- Oral Appliances: For mild to moderate OSA, custom-fitted oral appliances can be effective. These devices reposition the jaw and tongue to keep the airway open.
- Lifestyle Modifications: Weight loss, avoiding alcohol and sedatives before bed, quitting smoking, and changing sleep position can significantly improve or resolve mild OSA.
- Surgery: In some cases, surgical procedures to remove excess tissue in the throat, correct jaw alignment, or improve nasal airflow may be considered, particularly for OSA.
- Treatment for Central Sleep Apnea: CSA management can be more complex. It may involve treating the underlying medical condition (e.g., heart failure), using adaptive servo-ventilation (ASV) devices that adjust airflow based on breathing patterns, or using supplemental oxygen. Medications are sometimes used to stimulate breathing.
Understanding the intricacies of apnea events is fundamental to recognizing sleep apnea as a serious medical condition. By identifying these breathing pauses and their underlying causes, healthcare professionals can implement effective strategies to restore healthy sleep, improve overall health, and enhance the quality of life for affected individuals.
