A systemic condition refers to a health issue that affects the entire body or a significant portion of it, rather than being localized to a single organ or body part. This contrasts with localized conditions, which might, for instance, impact only a specific joint or a small area of skin. Systemic conditions often involve complex interactions between various bodily systems, and their manifestations can be widespread and multifaceted. Understanding the systemic nature of a condition is crucial for accurate diagnosis, effective treatment, and managing the overall health and well-being of an individual.
Understanding the Scope of Systemic Illness
The concept of “systemic” implies a broad impact. When a condition is deemed systemic, it signifies that its underlying cause or its effects are not confined. This can stem from various origins:
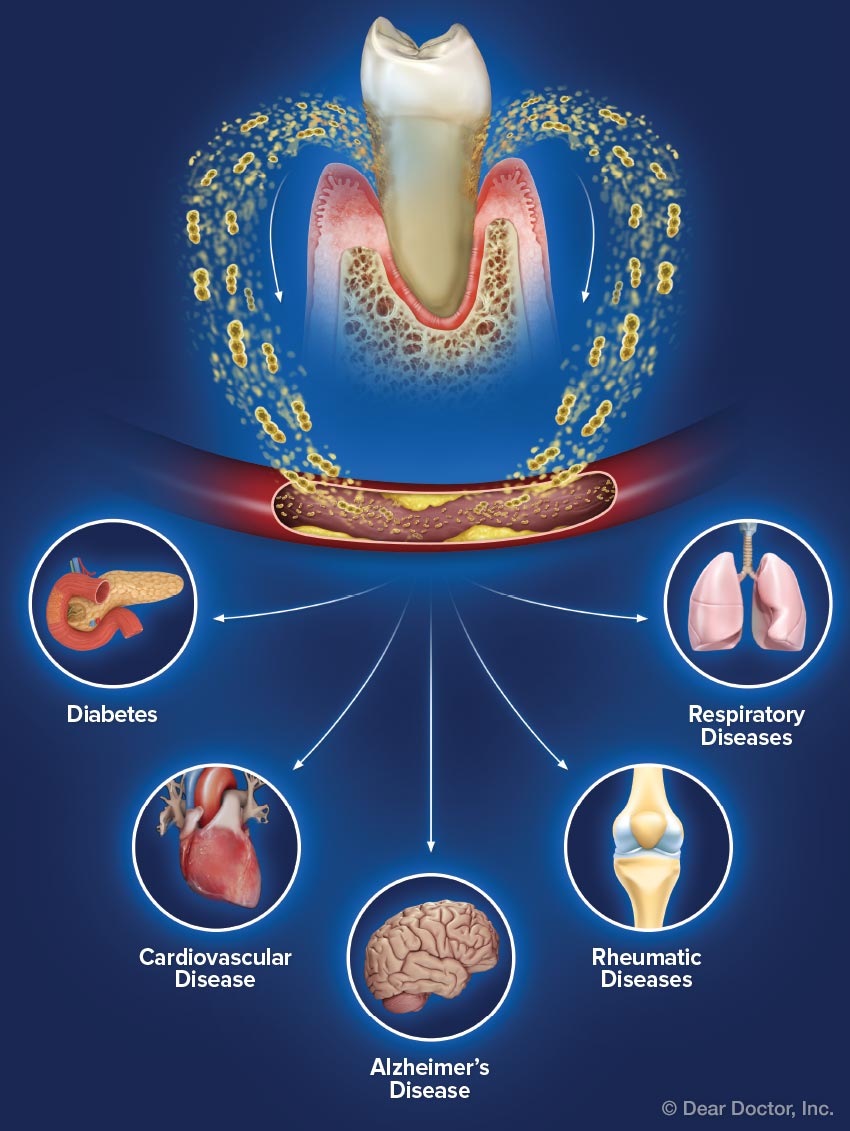
Genetic Predispositions
Many systemic conditions have a strong genetic component. Inherited disorders can predispose individuals to developing specific illnesses that affect multiple organ systems over time. For example, certain autoimmune diseases, metabolic disorders, and hereditary syndromes fall into this category. The genetic blueprint dictates certain vulnerabilities or malfunctions that then manifest system-wide.
Infections and Pathogens
While some infections are localized (like a skin infection), others can become systemic, leading to a widespread response throughout the body. Sepsis, a life-threatening response to infection, is a prime example of a systemic condition where the body’s immune response becomes dysregulated and damages its own tissues and organs. Similarly, viruses like influenza or more severe pathogens can spread throughout the bloodstream and affect multiple organ systems.
Environmental and Lifestyle Factors
External factors can also contribute to systemic conditions. Chronic exposure to toxins, prolonged stress, poor diet, lack of exercise, and other lifestyle choices can cumulatively impact the body’s ability to function optimally, leading to systemic imbalances and diseases. For instance, long-term exposure to certain pollutants can affect the respiratory, cardiovascular, and nervous systems.
Autoimmune Diseases
In autoimmune conditions, the body’s immune system mistakenly attacks its own healthy cells and tissues. Because the immune system circulates throughout the entire body, these diseases are inherently systemic. Examples include rheumatoid arthritis, lupus erythematosus, and multiple sclerosis, where inflammation and damage can occur in joints, skin, kidneys, brain, and other organs.
Hormonal Imbalances
The endocrine system, responsible for producing hormones, plays a vital role in regulating numerous bodily functions. Imbalances in hormone production can have widespread effects. Conditions like diabetes mellitus (affecting glucose metabolism across the body), thyroid disorders (impacting metabolism, energy levels, and organ function), and adrenal insufficiency are systemic in nature.
Manifestations and Diagnosis of Systemic Conditions
The widespread nature of systemic conditions often leads to a diverse range of symptoms that may not immediately point to a single organ. This can make diagnosis challenging.
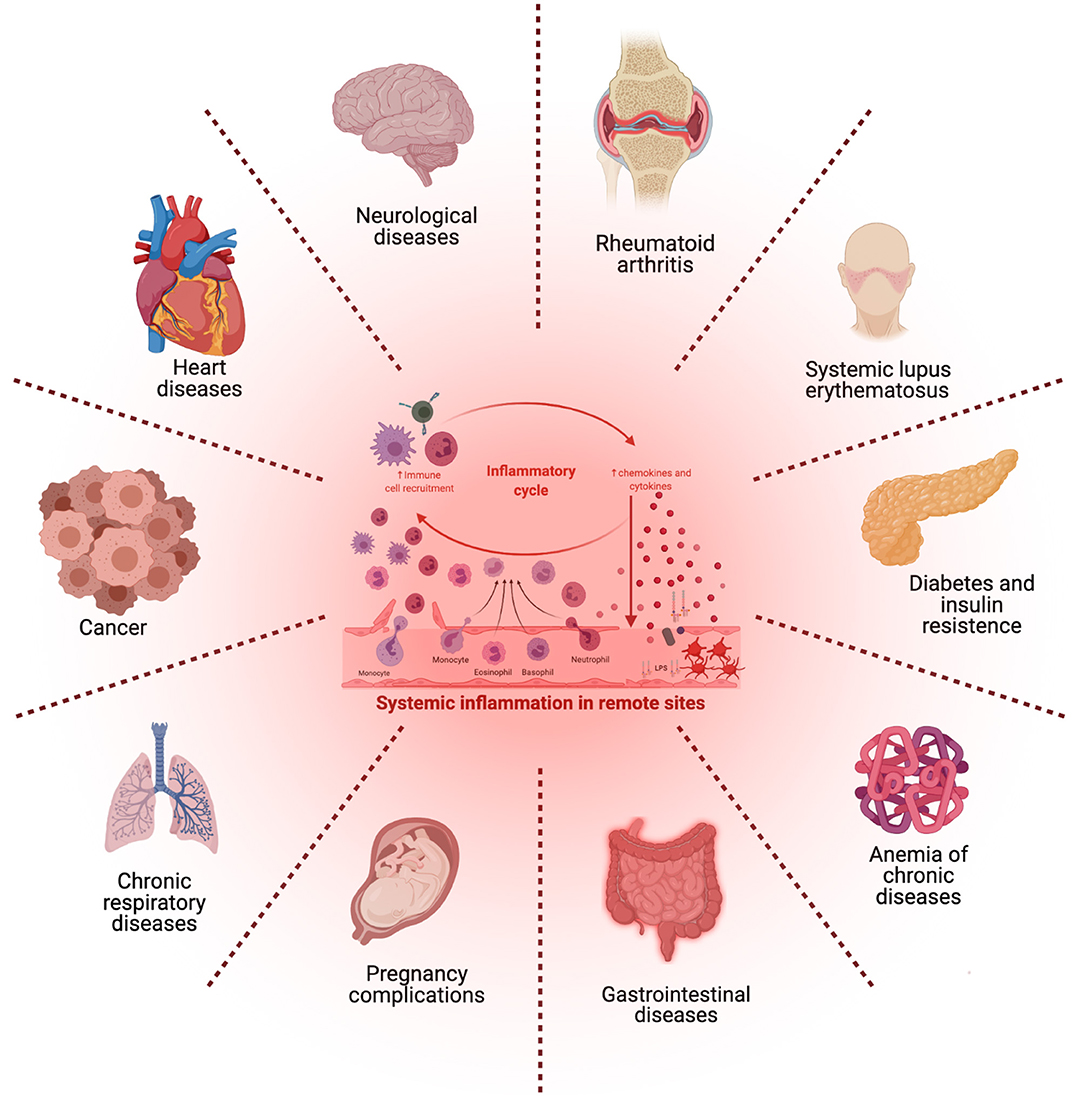
Symptom Diversity
A patient with a systemic condition might present with a constellation of symptoms affecting different parts of their body. For example, someone with lupus might experience joint pain, fatigue, skin rashes, kidney problems, and neurological issues, all stemming from the same underlying autoimmune process. This requires clinicians to look beyond isolated complaints and consider the broader picture.
The Diagnostic Process
Diagnosing a systemic condition typically involves a comprehensive approach:
- Detailed Medical History: Gathering information about the patient’s symptoms, their duration, progression, and any relevant family history is crucial.
- Thorough Physical Examination: A complete physical assessment helps identify signs and symptoms that might be indicative of systemic involvement across different organ systems.
- Laboratory Tests: Blood tests, urine tests, and other biochemical analyses can reveal markers of inflammation, organ dysfunction, hormonal imbalances, or the presence of specific pathogens.
- Imaging Studies: X-rays, CT scans, MRIs, and ultrasounds can provide detailed views of internal organs and tissues, helping to assess the extent of any damage or abnormalities.
- Biopsies: In some cases, a tissue sample may be taken for microscopic examination to identify cellular changes or the presence of disease.
- Specialized Consultations: Depending on the suspected condition, specialists from various fields (e.g., rheumatology, endocrinology, neurology, infectious diseases) may be consulted to provide expert evaluation.
The Importance of Early Detection
Early detection of systemic conditions is paramount. The longer these diseases progress unchecked, the more likely they are to cause irreversible damage to multiple organs. Prompt diagnosis and intervention can significantly improve treatment outcomes, slow disease progression, and enhance the patient’s quality of life.
Managing Systemic Conditions
The management of systemic conditions is often complex and requires a multidisciplinary approach, focusing on addressing the root cause, managing symptoms, and preventing further complications.
Treatment Modalities
Treatment strategies are tailored to the specific condition but generally aim to:
- Address the Underlying Cause: If the condition is caused by an infection, antibiotics or antivirals might be used. For autoimmune diseases, immunosuppressants or immunomodulatory drugs are common. Genetic disorders may require specific gene therapies or enzyme replacement.
- Manage Symptoms: Pain relief, anti-inflammatory medications, and therapies to improve organ function are often necessary to alleviate the patient’s suffering and maintain quality of life.
- Prevent Complications: Regular monitoring and proactive management of potential complications in affected organ systems are essential. For instance, individuals with diabetes need careful management of blood sugar to prevent cardiovascular and neurological issues.
- Lifestyle Modifications: In many cases, significant lifestyle changes are required. This can include dietary adjustments, regular exercise, stress management techniques, and avoiding triggers that exacerbate the condition.
The Role of a Multidisciplinary Team
Effective management of systemic conditions frequently involves a team of healthcare professionals working collaboratively. This team may include:
- Primary Care Physicians: Often the first point of contact, responsible for initial diagnosis and ongoing coordination of care.
- Specialist Physicians: Experts in specific organ systems or disease categories (e.g., cardiologists, nephrologists, neurologists, oncologists).
- Nurses: Providing patient education, monitoring, and support.
- Pharmacists: Ensuring appropriate medication management and identifying potential drug interactions.
- Physical and Occupational Therapists: Helping patients regain function and adapt to limitations.
- Dietitians: Providing nutritional guidance to support overall health and manage specific conditions.
- Mental Health Professionals: Addressing the psychological impact of chronic illness.

Prognosis and Long-Term Outlook
The prognosis for systemic conditions varies widely depending on the specific disease, its severity, the individual’s overall health, and the effectiveness of treatment. Some systemic conditions can be effectively managed, allowing individuals to lead relatively normal lives, while others may be chronic and progressive, requiring lifelong management and potentially leading to significant disability or reduced lifespan. Ongoing research continues to improve understanding of these complex conditions, leading to new diagnostic tools and more effective therapeutic interventions. The focus in managing systemic conditions is to achieve the best possible outcome, balancing the management of the disease with the preservation of the patient’s quality of life.
