Tuberculosis (TB), a formidable infectious disease historically associated with the lungs, can manifest in various organs and systems throughout the body. Among its less common yet significant extrapulmonary presentations is spinal cord tuberculosis, also known as tuberculous spondylitis or Pott’s disease. This insidious infection targets the vertebral bodies, intervertebral discs, and surrounding spinal structures, posing a serious threat to neurological function and overall health. Understanding the pathogenesis, clinical presentation, diagnostic challenges, and treatment modalities of spinal cord TB is crucial for effective management and prevention of potentially devastating sequelae.
Pathogenesis and Spread of Spinal Cord Tuberculosis
Tuberculosis is caused by the bacterium Mycobacterium tuberculosis. While primary infection typically occurs in the lungs via airborne droplets, dissemination to other parts of the body can happen through hematogenous (bloodstream) or lymphatic spread. Spinal cord TB often arises from a distant primary focus, most commonly in the lungs, but also potentially in the genitourinary tract or lymph nodes.

The bacillus, once in the bloodstream, tends to settle in areas with a rich blood supply and relatively poor lymphatic drainage, making the richly vascularized vertebral bodies prime targets. The anterior and superior or inferior aspects of the vertebral bodies are particularly susceptible. From the vertebral body, the infection can spread to the adjacent intervertebral disc, leading to discitis. It can also extend to the anterior longitudinal ligament, paraspinal soft tissues, and the spinal canal.
Anatomical Involvement and Mechanisms of Damage
The spread of infection within the spine creates several pathways for tissue destruction and neurological compromise:
- Vertebral Body Destruction: The inflammatory process triggers osteoclastic activity, leading to bone erosion. This can result in vertebral collapse, kyphotic deformity (a “gibbus” deformity), and instability of the spine.
- Discitis: The intervertebral disc, lacking its own blood supply, is particularly vulnerable once infected. The cartilage degenerates, leading to loss of disc height and further instability.
- Epidural Abscess Formation: Inflammation and pus accumulation can occur in the epidural space, the area surrounding the dura mater. This is a major cause of spinal cord compression. The abscess can extend longitudinally along the spinal canal.
- Granuloma Formation: Tubercles, characteristic granulomatous lesions of TB, can form within the vertebral bone, disc, or epidural space. These granulomas can compress neural structures.
- Psoas Abscess: In thoracic and lumbar spine involvement, the infection can track along the vertebral bodies and anterior longitudinal ligament, forming a psoas abscess in the iliopsoas muscle sheath. This is a common finding in spinal TB and can be a source of diagnostic clues.
- Meningitis: While less common, TB can spread to the meninges, causing tuberculous meningitis, which can also affect the spinal cord.
The slow, indolent nature of TB allows for significant destruction to occur before overt symptoms manifest. This insidious progression contributes to the diagnostic challenges associated with spinal cord TB.
Clinical Manifestations and Symptoms
The clinical presentation of spinal cord TB is often insidious and variable, making early diagnosis difficult. Symptoms can develop over weeks to months and may initially be non-specific. The classic triad of symptoms associated with spinal TB includes:
- Pain: This is the most common symptom, often described as a dull, aching pain that is worse at night. The pain is typically localized to the affected spinal segment and may radiate to the abdomen or extremities. It is often exacerbated by movement and relieved by rest.
- Fever and Constitutional Symptoms: Patients may experience low-grade fever, night sweats, weight loss, and general malaise, similar to pulmonary TB. However, these symptoms can be absent, especially in early stages or in certain populations.
- Neurological Deficits: This is the most concerning manifestation, arising from direct compression of the spinal cord or nerve roots by the inflammatory process, abscess, or vertebral collapse. Neurological deficits can range from mild sensory disturbances to severe motor weakness and paralysis.
Spectrum of Neurological Deficits
The type and severity of neurological deficits depend on the location and extent of spinal cord involvement. Common neurological findings include:
- Radiculopathy: Compression of nerve roots can cause pain, paresthesia (numbness or tingling), and weakness in the distribution of the affected nerve.
- Myelopathy: Compression of the spinal cord itself leads to a constellation of symptoms known as myelopathy. This can manifest as:
- Motor Weakness: Progressive weakness in the limbs, often starting distally and progressing proximally. Spasticity and hyperreflexia may develop.
- Sensory Disturbances: Loss of sensation, including touch, pain, temperature, and proprioception (sense of body position). Sensory levels can be identified on examination.
- Bowel and Bladder Dysfunction: Urinary or fecal incontinence, or retention, can occur due to involvement of the autonomic pathways controlling these functions.
- Sexual Dysfunction: Impotence in men can also be a symptom.
The progression of neurological deficits is often stepwise, with periods of relative stability followed by rapid deterioration, particularly if compression worsens due to abscess expansion or further vertebral collapse.
Diagnostic Challenges and Approaches
Diagnosing spinal cord TB is a complex process due to its subtle onset, non-specific symptoms, and the challenges in obtaining definitive microbiological confirmation. A high index of suspicion is paramount, especially in individuals with a history of TB, immunocompromised states (e.g., HIV infection), or those residing in endemic areas.
Imaging Modalities
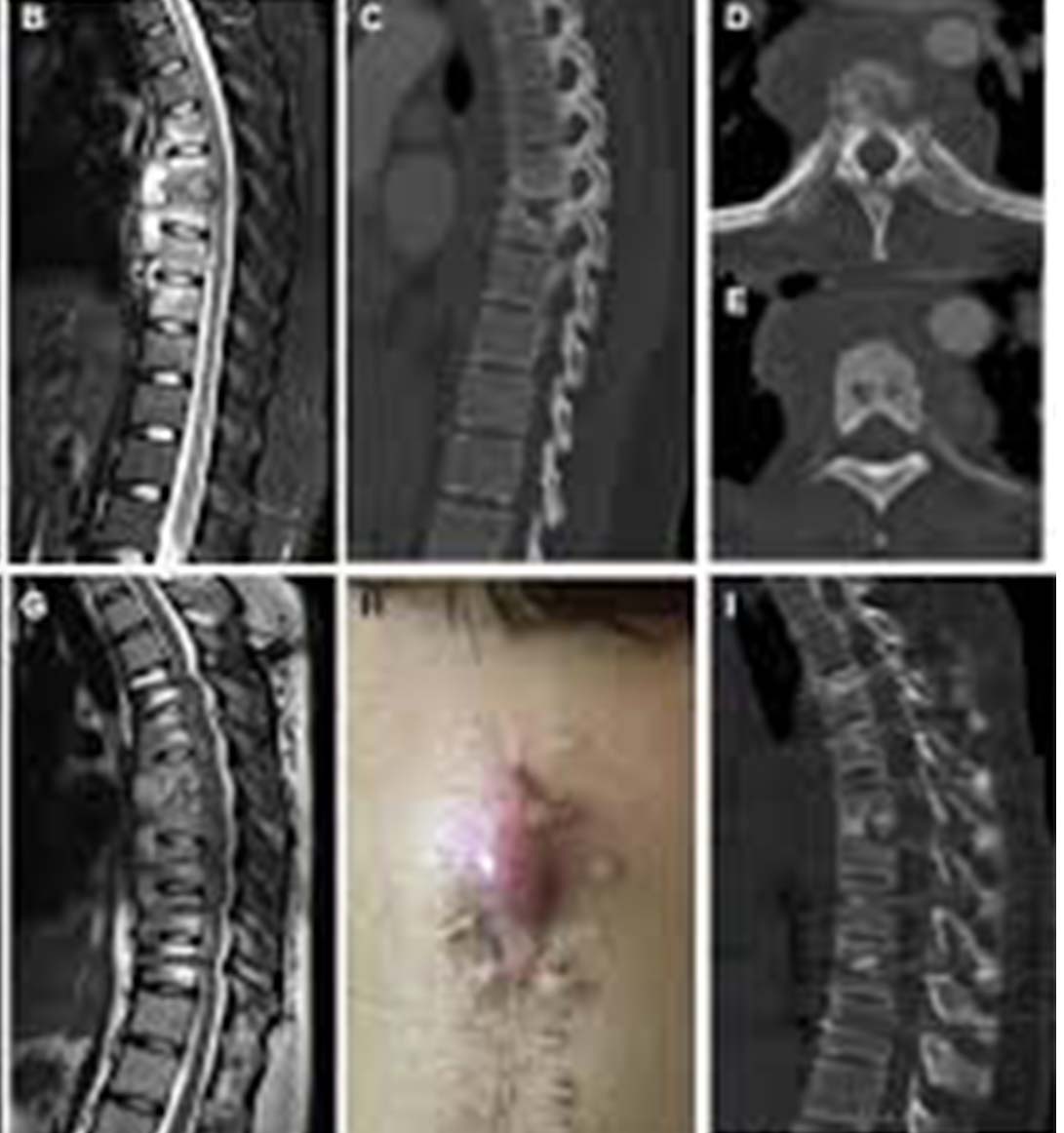
Imaging plays a pivotal role in identifying spinal abnormalities and assessing the extent of disease:
- Plain Radiography (X-rays): Early on, X-rays may be normal. As the disease progresses, characteristic findings include vertebral body destruction (often lytic, with end-plate erosion), disc space narrowing, and kyphotic deformity. However, plain radiography is not sensitive enough for early diagnosis.
- Computed Tomography (CT) Scan: CT scans provide more detailed cross-sectional images of the bone and soft tissues. They are excellent for visualizing vertebral body destruction, disc involvement, and the presence of paravertebral or epidural collections (abscesses). CT-guided biopsy can also be performed.
- Magnetic Resonance Imaging (MRI): MRI is the gold standard for evaluating spinal cord TB. It offers superior visualization of soft tissues, including the spinal cord, meninges, and epidural space. MRI can detect early inflammatory changes, epidural abscesses, intramedullary lesions, and signal changes within the spinal cord indicative of compression or inflammation (myelitis). It also helps assess the extent of cord compression and guiding surgical intervention. Gadolinium contrast enhancement is crucial for delineating abscesses and inflammatory lesions.
Microbiological Confirmation
While imaging can strongly suggest the diagnosis, definitive confirmation relies on microbiological evidence:
- Acid-Fast Bacilli (AFB) Smear and Culture: Samples for AFB smear and culture can be obtained from various sites, including:
- Aspiration: Percutaneous or surgical aspiration of pus from paravertebral, epidural, or psoas abscesses.
- Biopsy: Surgical or CT-guided biopsy of involved vertebral bodies, discs, or paravertebral masses.
- Sputum: If pulmonary TB is suspected or confirmed.
- Urine or Other Fluids: If extrapulmonary TB in other sites is present.
Culture is the most sensitive method but has a long turnaround time (several weeks).
- Nucleic Acid Amplification Tests (NAATs): Rapid molecular tests like GeneXpert MTB/RIF can detect Mycobacterium tuberculosis DNA in clinical samples and also identify rifampicin resistance. These tests offer faster results than culture and are increasingly used.
- Histopathology: Biopsy specimens can also be examined histopathologically for caseating granulomas, the hallmark of TB.
Other Diagnostic Considerations
- Blood Tests: Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) are often elevated, indicating inflammation, but are non-specific.
- HIV Testing: In endemic regions or in individuals with risk factors, HIV co-infection is common and can influence the presentation and treatment of TB.
Management and Treatment Strategies
The management of spinal cord TB is multifaceted, involving a combination of anti-tuberculosis chemotherapy, surgical intervention, and supportive care. The primary goals are to eradicate the infection, prevent further neurological damage, correct deformities, and restore function.
Anti-Tuberculosis Chemotherapy
Standard anti-TB drug regimens are the cornerstone of treatment. The duration and specific drugs used depend on factors such as the presence of drug resistance, extent of disease, and patient’s immune status. A typical intensive phase involves a combination of four drugs:
- Isoniazid (INH)
- Rifampicin (RIF)
- Pyrazinamide (PZA)
- Ethambutol (EMB)
This intensive phase is usually followed by a continuation phase with two drugs, typically isoniazid and rifampicin, for a total treatment duration of 6 to 12 months, or longer in cases of drug resistance or extensive disease. Drug susceptibility testing is crucial to guide treatment, especially in areas with high rates of multidrug-resistant TB (MDR-TB) or extensively drug-resistant TB (XDR-TB).
Surgical Intervention
Surgery is indicated in specific situations, primarily when there is significant neurological compromise due to spinal cord compression, spinal instability, or severe deformity.
- Decompression: Surgical decompression aims to relieve pressure on the spinal cord and nerve roots caused by epidural abscesses, granulomas, or collapsed vertebral bodies. This can be achieved through anterior or posterior approaches, depending on the location of the lesion.
- Debridement: Removal of necrotic tissue, caseous material, and pus to reduce the bacterial load and promote healing.
- Stabilization and Reconstruction: Spinal fusion may be necessary to stabilize the spine, especially after extensive vertebral body destruction or if there is significant instability. Bone grafting or the use of instrumentation (e.g., rods and screws) may be employed to achieve stability and correct deformity.
- Drainage of Abscesses: Large abscesses, particularly psoas abscesses, may require surgical or percutaneous drainage.
The timing and extent of surgical intervention are critical and should be carefully considered in conjunction with medical management.

Supportive Care and Rehabilitation
- Pain Management: Effective pain control is essential for patient comfort and mobility.
- Nutritional Support: Adequate nutrition is vital for healing and immune function.
- Physical and Occupational Therapy: Rehabilitation plays a crucial role in restoring motor function, improving mobility, and maximizing independence for patients with neurological deficits. This may include exercises to strengthen muscles, improve balance, and adapt to any permanent disabilities.
- Management of Complications: Prompt recognition and management of complications such as pathological fractures, spinal deformity progression, and neurological deterioration are important.
Spinal cord TB, while a serious condition, can be effectively managed with early diagnosis and a comprehensive treatment approach. Continued research into more rapid diagnostic methods and optimized treatment regimens remains vital to improve outcomes for affected individuals worldwide.
