The term “EC fistula” is not a recognized or standard medical term. It is highly probable that this is a typographical error, a misunderstanding of a medical term, or a highly specialized jargon within a very specific field not publicly documented. Without further context, it is impossible to definitively identify what “EC fistula” refers to.
However, if we were to deconstruct the term based on common medical terminology and potential misspellings or abbreviations, we can explore several possibilities. The word “fistula” itself refers to an abnormal connection or passageway between two organs or between an organ and the outside of the body. This connection is typically a result of injury, infection, or inflammation.

Let’s consider potential interpretations of “EC”:
Possible Interpretations of “EC”
Given the limitations, we will explore some plausible interpretations that could lead to a medical or scientific context for a “fistula.”
Enterocutaneous Fistula (ECF)
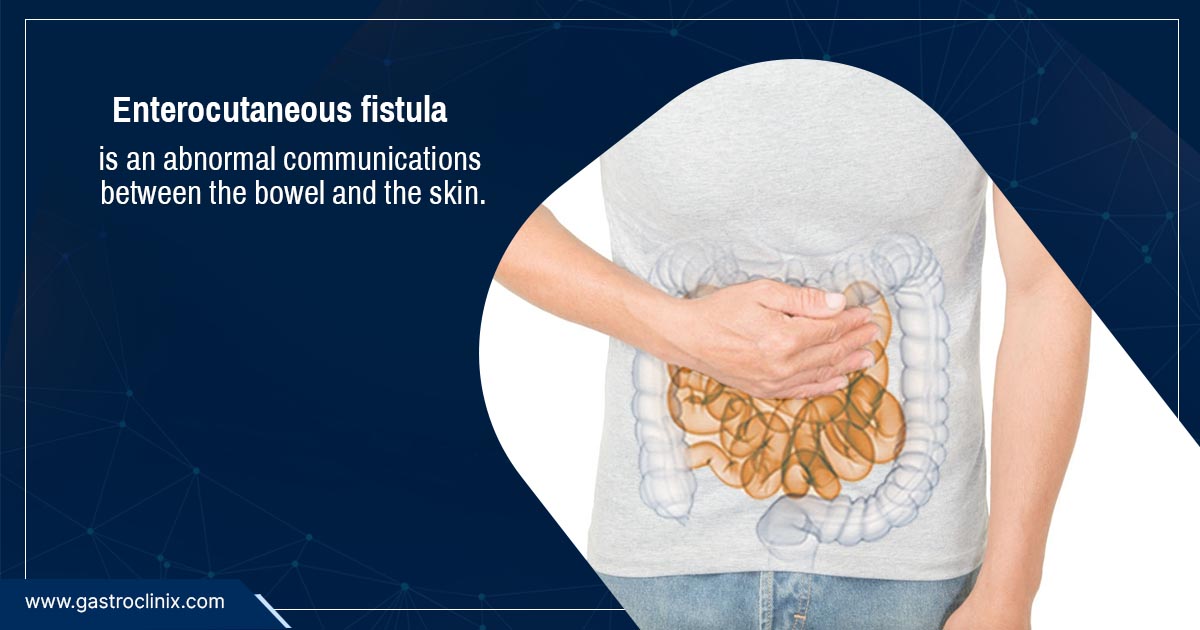
The most likely interpretation, based on common medical abbreviations and the structure of the word, is that “EC” is a shorthand for “enterocutaneous.” An enterocutaneous fistula (ECF) is an abnormal connection between the small intestine (enteric) and the skin (cutaneous). This means that instead of digested food passing normally through the intestines and being eliminated as waste, it leaks out through an opening in the skin.
Causes of Enterocutaneous Fistulas
ECFs are serious medical conditions that can arise from a variety of causes, often related to damage or dysfunction within the gastrointestinal tract. The most frequent culprits include:
- Surgical Complications: Surgery involving the abdomen, particularly bowel resections or repairs, is a leading cause. Complications such as anastomotic leaks (where surgical connections between bowel segments fail to heal properly), unintentional injury to the bowel during surgery, or infection at the surgical site can all lead to ECF formation.
- Inflammatory Bowel Disease (IBD): Conditions like Crohn’s disease, which causes chronic inflammation throughout the digestive tract, can lead to the formation of fistulas. In severe cases, this inflammation can erode through the intestinal wall and connect to the skin.
- Radiation Therapy: Patients who have undergone radiation therapy to the abdomen for conditions like cancer can develop damage to the intestinal lining and surrounding tissues. This radiation-induced enteritis can weaken the bowel wall and predispose it to fistula formation.
- Malignancy: Cancers of the gastrointestinal tract, such as colorectal cancer or small bowel tumors, can invade the bowel wall and create fistulas, either directly to the skin or to other organs, which can then secondarily lead to a cutaneous fistula.
- Infections: Severe abdominal infections, such as intra-abdominal abscesses, can sometimes erode into the bowel and the abdominal wall, creating an abnormal connection.
- Trauma: Blunt or penetrating abdominal trauma can cause direct injury to the intestines and abdominal wall, potentially leading to the development of a fistula.
Symptoms and Diagnosis of Enterocutaneous Fistulas
The presentation of an ECF can vary depending on its size, location, and the amount of intestinal contents that are leaking. However, common symptoms include:
- Drainage from an Abdominal Wound: This is the hallmark symptom. The drainage can be clear, yellowish, or greenish and often contains digestive enzymes, leading to skin irritation and breakdown. The volume of drainage can range from minimal to substantial.
- Abdominal Pain: Pain is often localized around the fistula site and can be generalized if there is associated infection or inflammation.
- Dehydration and Electrolyte Imbalances: Significant loss of intestinal fluid and electrolytes can lead to dehydration, electrolyte disturbances (such as low potassium or sodium), and malabsorption, resulting in weight loss and malnutrition.
- Fever and Sepsis: If the fistula is associated with infection, fever, chills, and signs of sepsis can develop.
- Skin Irritation and Breakdown: The digestive enzymes present in the drainage are highly corrosive and can cause severe chemical burns, excoriation, and breakdown of the surrounding skin.
Diagnosis typically involves a thorough medical history, physical examination, and various imaging studies. These may include:

- Imaging Studies: Contrast studies (e.g., barium swallow or small bowel follow-through) can help visualize the abnormal tract. CT scans and MRI scans can also identify the fistula, its tract, and any associated complications like abscesses.
- Endoscopy: While not always diagnostic for ECFs directly, endoscopy can be used to assess the underlying intestinal condition (e.g., IBD or malignancy) that may have led to the fistula.
Management of Enterocutaneous Fistulas
The management of ECFs is complex and often requires a multidisciplinary approach involving surgeons, gastroenterologists, nutritionists, and wound care specialists. The primary goals of treatment are to:
- Control Drainage: This involves managing the output from the fistula. Appliances designed to collect the drainage and protect the surrounding skin are crucial.
- Support Nutrition: Patients with ECFs often cannot absorb nutrients adequately through their normal digestive tract. Nutritional support, typically via total parenteral nutrition (TPN) administered intravenously, is essential to maintain hydration, provide calories, and promote healing.
- Treat Underlying Cause: Addressing the root cause of the fistula is paramount. This may involve treating infections with antibiotics, managing IBD with medications, or surgically removing tumors.
- Promote Healing and Closure: Many ECFs will spontaneously close with conservative management, especially if the underlying cause is addressed and nutritional support is adequate. However, some fistulas, particularly those with underlying disease, large size, or associated infection, may require surgical intervention.
Surgical closure of an ECF involves excising the abnormal tract and repairing the bowel defect. This is often a technically challenging procedure and carries its own risks.
Other Less Likely Interpretations
While ECF is the most probable interpretation, a remote possibility exists for other meanings of “EC.”
Endometrial-Colonic Fistula
This refers to an abnormal connection between the endometrium (the lining of the uterus) and the colon. These are extremely rare and are typically associated with conditions like endometriosis that has spread to the pelvic organs or following pelvic surgery or radiation. Symptoms might include rectal bleeding, pain during menstruation, or bowel changes coinciding with the menstrual cycle.
Electrocautery Fistula
In surgical contexts, “EC” might refer to electrocautery, a technique used to cut tissue or stop bleeding using heat generated by an electric current. While direct causation of a fistula by electrocautery alone is uncommon, unintended thermal injury during a procedure that uses electrocautery could, in rare circumstances, contribute to tissue damage leading to fistula formation. This is more of a contributing factor than a direct diagnosis of a specific fistula type.
Endoscopic Cholangiography Fistula
This is a highly speculative interpretation. Endoscopic retrograde cholangiopancreatography (ERCP) is a procedure used to diagnose and treat problems in the bile and pancreatic ducts. While complications from ERCP can occur, including pancreatitis or bleeding, the formation of a fistula directly termed “Endoscopic Cholangiography Fistula” is not a recognized entity. If a fistula were to form, it would likely be described by its anatomical location (e.g., a bile duct to intestine fistula).
Conclusion
Given the ambiguity of the term “EC fistula,” the most robust and medically relevant interpretation points to an Enterocutaneous Fistula (ECF). This is a serious condition characterized by an abnormal connection between the small intestine and the skin, leading to leakage of intestinal contents. Understanding the causes, symptoms, and management strategies for ECFs is critical for healthcare professionals and patients alike. Without further clarification, any other interpretation of “EC fistula” remains speculative. The precise identification of medical terms is paramount for accurate diagnosis and effective treatment.
