Navigating the complex world of health insurance can often feel like deciphering a foreign language, especially when it comes to understanding the different types of network plans available. Two common acronyms you’ll frequently encounter are HMO and POS. While both offer ways to access medical care through a network of providers, they operate with distinct structures and requirements that significantly impact your healthcare choices, costs, and flexibility. Understanding these differences is crucial for making an informed decision that best suits your individual needs and preferences.
Health Maintenance Organization (HMO): A Managed Care Approach
A Health Maintenance Organization (HMO) is a type of managed care health insurance plan that emphasizes coordinated care through a primary care physician (PCP). The fundamental principle of an HMO is to provide comprehensive healthcare services to its members in exchange for a fixed, prepaid fee. This model aims to control costs by managing patient care, encouraging preventive services, and requiring members to utilize a specific network of doctors, hospitals, and other healthcare providers.
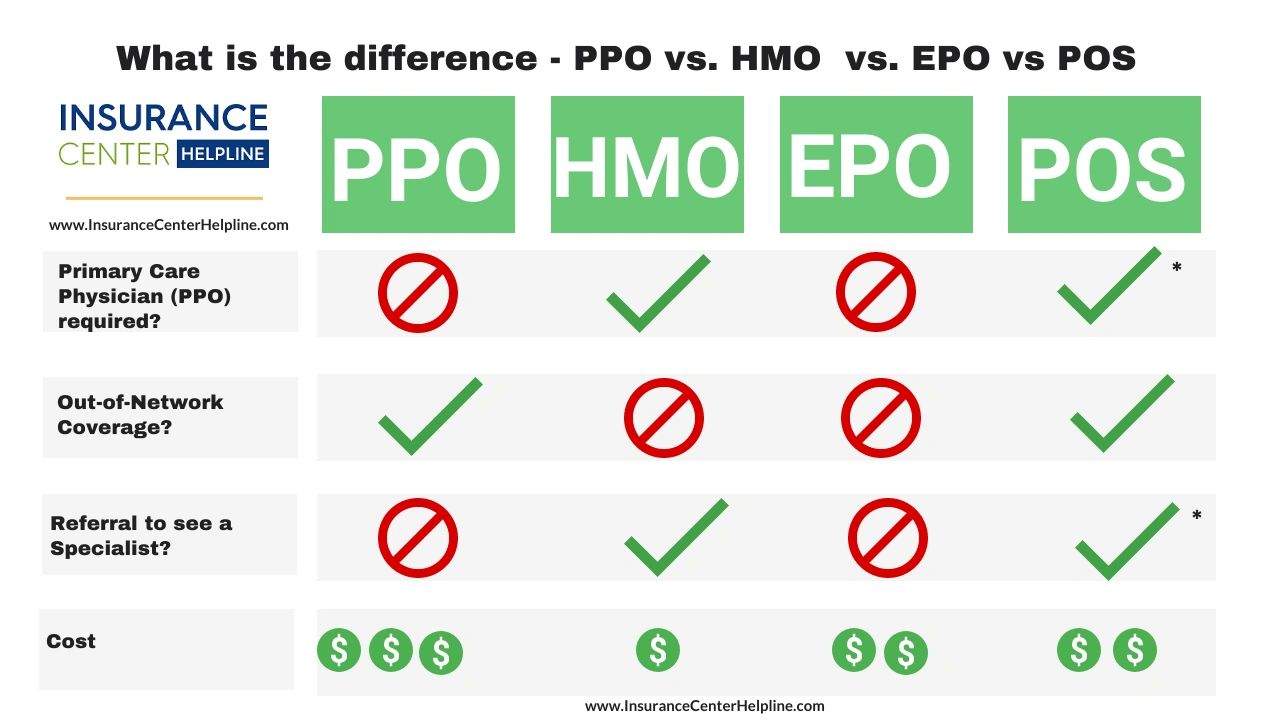
Key Features of HMO Plans
- Primary Care Physician (PCP) Gatekeeper: One of the defining characteristics of an HMO is the requirement to select a PCP from within the plan’s network. This PCP acts as your first point of contact for most healthcare needs and serves as a “gatekeeper.” Before you can see a specialist, you must obtain a referral from your PCP. This referral process is designed to ensure that you are seeing the most appropriate provider for your condition and to help manage overall healthcare utilization.
- Network Restrictions: HMO plans restrict your care to providers who are within the plan’s network. If you seek care from a provider outside of the network, the HMO typically will not cover the costs, except in cases of true medical emergencies. This means you need to be diligent in verifying that your preferred doctors and hospitals are part of your chosen HMO’s network before enrolling.
- Referral Requirements: As mentioned, referrals from your PCP are generally mandatory for seeing specialists. This applies to everything from cardiologists and dermatologists to mental health professionals. While this can sometimes add an extra step to your healthcare journey, it ensures that your PCP is aware of all your medical treatments and can help coordinate your care effectively.
- Cost-Effectiveness: HMOs are often praised for their affordability. They typically have lower monthly premiums, lower deductibles, and lower out-of-pocket costs (copayments and coinsurance) compared to other types of insurance plans. This is largely due to the controlled network and the focus on preventive care, which can help reduce the need for more expensive treatments down the line.
- Emphasis on Preventive Care: HMOs have a strong incentive to promote preventive care and wellness programs. By encouraging members to get regular check-ups, screenings, and vaccinations, they aim to catch health issues early, when they are often easier and less costly to treat. This focus can lead to better long-term health outcomes for members.
- No Out-of-Network Coverage (Except Emergencies): It’s crucial to reiterate that outside of emergencies, HMOs do not provide coverage for care received from out-of-network providers. This is a significant consideration for individuals who may have established relationships with doctors not included in a specific HMO’s network or who live in areas with limited network options.
Point of Service (POS) Plans: A Hybrid Approach
A Point of Service (POS) plan offers a blend of features found in both HMOs and Preferred Provider Organizations (PPOs). POS plans provide members with flexibility in choosing their healthcare providers, allowing them to seek care both in-network and out-of-network. However, they still incorporate some of the managed care elements characteristic of HMOs, such as the requirement for a PCP and referrals for specialist care. The “point of service” refers to the decision you make at the time you seek care – whether to use an in-network provider or go out-of-network.
Key Features of POS Plans
- Primary Care Physician (PCP) Requirement: Similar to HMOs, POS plans typically require you to designate a PCP from within the plan’s network. This PCP is responsible for coordinating your care and providing referrals to specialists. This managed care aspect helps to control costs and ensure that your healthcare is integrated.
- Network Flexibility: While you are encouraged to use in-network providers for the lowest out-of-pocket costs, POS plans offer the option to seek care from out-of-network providers. This provides greater freedom and choice compared to a traditional HMO.
- Referral Requirements (In-Network vs. Out-of-Network): The referral process in a POS plan often depends on whether you are staying within the network or going out-of-network. If you see an in-network specialist, you will likely need a referral from your PCP. However, if you choose to see an out-of-network specialist, you may not need a referral, but your cost-sharing responsibilities will be significantly higher.
- Cost-Sharing Variations: The cost of care under a POS plan varies depending on whether you use in-network or out-of-network providers.
- In-Network Care: When you use in-network providers, your out-of-pocket costs will generally be lower, similar to an HMO. You’ll typically pay copayments for doctor visits and services.
- Out-of-Network Care: When you opt for out-of-network care, you will likely face higher costs. This often includes a higher deductible, higher coinsurance (a percentage of the cost of the service), and potentially a separate, higher out-of-pocket maximum for out-of-network services. The plan may also only cover a percentage of what it considers the “usual and customary” charge for the service, leaving you responsible for the difference.
- Claim Filing for Out-of-Network Services: If you receive out-of-network care, you will usually be responsible for paying the provider upfront and then submitting a claim to your insurance company for reimbursement. This is a significant difference from HMOs, where the network providers typically handle all billing directly with the insurance company.
- Balance Billing Potential: Because out-of-network providers are not bound by the contracted rates of your POS plan, they may bill you for the difference between their charges and what your insurance company deems reasonable or allows. This is known as “balance billing” and can lead to unexpected and substantial costs if not carefully managed.
Comparing HMO and POS: Key Differences at a Glance
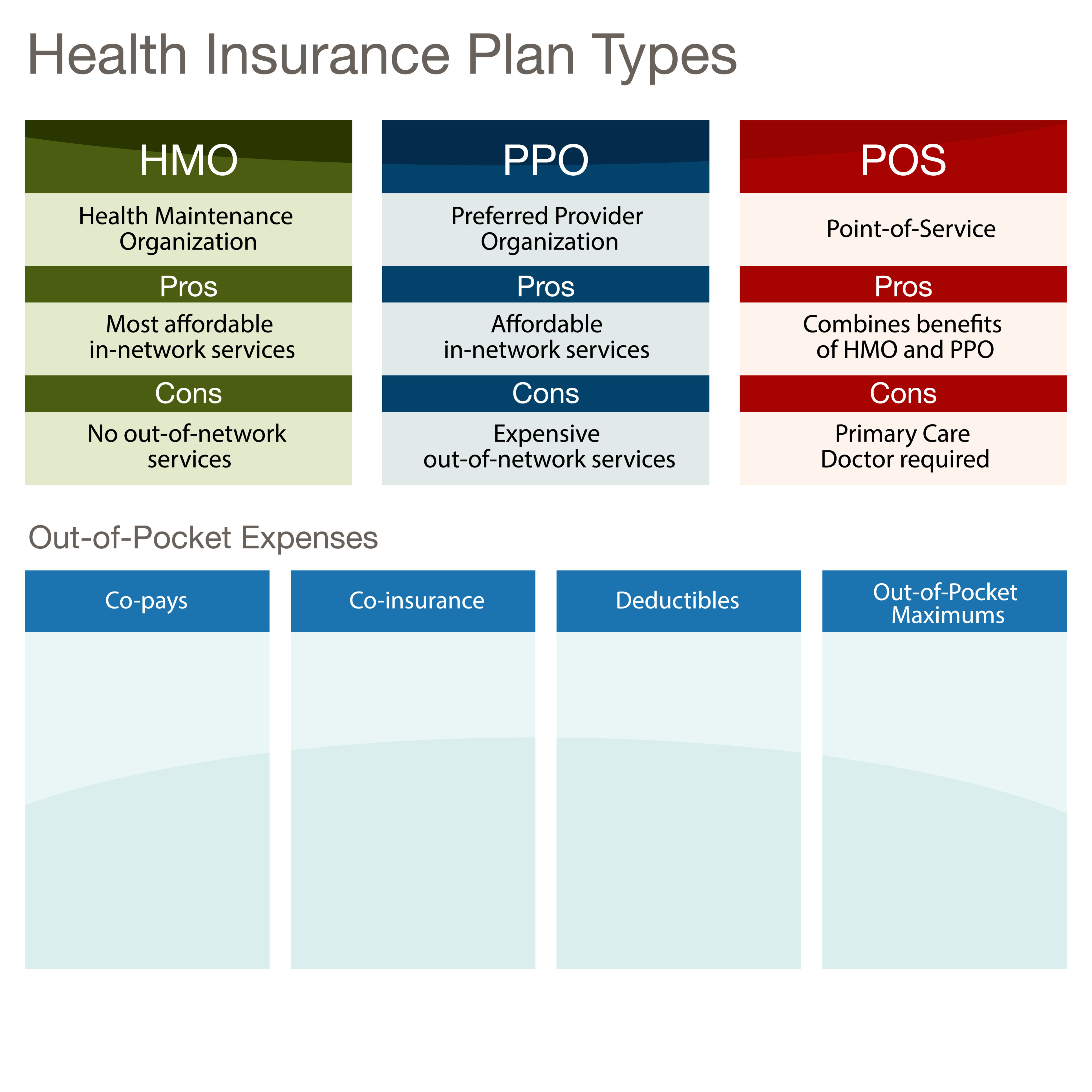
When deciding between an HMO and a POS plan, understanding their core distinctions is paramount. The primary trade-offs revolve around cost, flexibility, and the level of control the insurance plan exerts over your healthcare choices.
| Feature | HMO (Health Maintenance Organization) | POS (Point of Service) |
|---|---|---|
| Primary Care Physician | Required; acts as gatekeeper for referrals. | Required; acts as gatekeeper for referrals. |
| Network Coverage | Exclusive to in-network providers (except emergencies). | Covers both in-network and out-of-network providers. |
| Referrals | Required for all specialist visits. | Required for in-network specialists; may not be required for out-of-network, but costs are higher. |
| Out-of-Pocket Costs | Generally lower premiums, deductibles, and copayments. | Lower costs for in-network care; higher costs (deductibles, coinsurance) for out-of-network care. |
| Flexibility | Limited; confined to network providers. | More flexible; allows choice of out-of-network providers at a higher cost. |
| Claim Filing | Providers handle all billing with the insurance company. | You may need to file claims for out-of-network services. |
| Cost Control Focus | High; managed care through PCP and strict network adherence. | Moderate; combines managed care with flexibility, leading to potentially higher overall costs. |
| Best Suited For | Individuals who prioritize lower costs and are comfortable with a PCP directing their care within a defined network. | Individuals who want the option to see out-of-network providers occasionally but prefer lower costs when staying in-network. |
Making the Right Choice: Factors to Consider
The decision between an HMO and a POS plan is highly personal and depends on a variety of individual circumstances. There is no one-size-fits-all answer, and what works best for one person might not be ideal for another.
Consider Your Healthcare Needs
- Do you have specific doctors or specialists you want to continue seeing? If these providers are not in a particular HMO’s network, an HMO might be a non-starter unless you’re willing to switch. A POS plan offers more leeway here, though you’ll incur higher costs for out-of-network visits.
- What is your health status and are you likely to need frequent specialist care? If you anticipate needing many specialist visits, the referral requirements of an HMO might feel restrictive. However, the cost savings of an HMO for these visits (when within the network) could be significant. A POS plan offers more freedom, but you must be prepared for the higher out-of-pocket expenses for out-of-network specialists.
- Do you value preventive care and a coordinated approach to your health? Both HMOs and POS plans encourage this through the PCP model. However, HMOs are often more structured and financially incentivized to provide extensive preventive services.
Evaluate Your Financial Situation
- What is your budget for monthly premiums and out-of-pocket expenses? HMOs generally offer the lowest premiums and out-of-pocket costs. If minimizing these expenses is your top priority and you’re comfortable with the network limitations, an HMO is likely the more economical choice.
- Are you willing to pay more for greater flexibility? POS plans typically have higher premiums than HMOs and significantly higher costs for out-of-network care. If you believe the ability to see an out-of-network provider is worth the extra expense, a POS plan might be a better fit.
- How much risk are you willing to take regarding unexpected medical bills? With an HMO, you have a predictable cost structure as long as you stay in-network. With a POS plan, there’s a greater potential for unexpected costs if you frequently utilize out-of-network services without understanding the plan’s limitations and coverage.

Understand the Network
- Research the provider network thoroughly: Before enrolling in any plan, examine the list of doctors, hospitals, and other healthcare facilities included in the network. Are your preferred providers included? Are there enough providers in your area to meet your needs?
- Consider the geographical area: If you travel frequently or live in a region with limited healthcare options, the robustness of the network in those areas becomes a critical factor. An HMO with a sparse network in your travel destinations could be problematic.
In conclusion, both HMO and POS plans are valuable tools for accessing healthcare, each with its own strengths and weaknesses. An HMO offers a cost-effective, managed care approach where a PCP guides your healthcare journey within a defined network. A POS plan provides more flexibility by allowing out-of-network care, albeit at a higher cost, while still maintaining the benefits of a PCP and a primary network. By carefully considering your personal needs, financial circumstances, and the specifics of each plan’s network, you can confidently select the health insurance option that best supports your well-being.
