The term “airspace disease” in the lungs, while not a standard clinical diagnosis in the way pneumonia or emphysema are, is a conceptual umbrella used to describe a range of conditions that primarily affect the tiny air sacs within the lungs, known as alveoli. These alveoli are the critical sites where gas exchange occurs – oxygen entering the bloodstream and carbon dioxide being expelled. When these delicate structures are compromised, the fundamental process of breathing is impaired, leading to a variety of symptoms and significant health challenges. Understanding the nature of airspace disease is crucial for appreciating the intricacies of respiratory health and the impact of environmental and internal factors on our ability to breathe.

The Alveolar Landscape: A Foundation for Gas Exchange
To grasp what constitutes “airspace disease,” it’s essential to visualize the lungs’ intricate architecture. Imagine a vast, complex network of branching tubes, from the trachea down to bronchi and bronchioles, eventually terminating in millions of minuscule sacs. These are the alveoli, and their collective surface area is astonishing – roughly the size of a tennis court. Each alveolus is incredibly thin-walled, often just one cell thick, and surrounded by a dense network of capillaries. This close proximity and thin barrier facilitate the rapid diffusion of gases between inhaled air and the blood.
Structure and Function of Alveoli
The alveoli are not merely passive balloons; they are highly specialized structures. They are lined with two main types of cells: type I pneumocytes, which form the structural wall of the alveolus and are responsible for gas exchange, and type II pneumocytes, which produce surfactant. Surfactant is a crucial substance that reduces the surface tension within the alveoli, preventing them from collapsing during exhalation and making it easier to inflate them with each breath. Dust cells, or alveolar macrophages, are also present, acting as the lungs’ immune defense system, clearing inhaled particles and pathogens.
The Importance of Airspace Integrity
The health of these airspaces is paramount. Any condition that damages the alveolar walls, impairs surfactant production, obstructs the air sacs, or fills them with abnormal material directly interferes with this vital gas exchange. This disruption leads to hypoxia (low oxygen levels in the blood) and hypercapnia (high carbon dioxide levels in the blood), both of which can have severe systemic consequences.
Categories of Airspace Disease: From Inflammation to Structural Damage
“Airspace disease” encompasses conditions that disrupt the normal function and structure of the alveoli. These can be broadly categorized based on the underlying pathological process.
Inflammatory and Infectious Processes
One of the most common ways alveoli are affected is through inflammation and infection. When pathogens like bacteria, viruses, or fungi invade the lungs, they can trigger an inflammatory response within the alveolar spaces.
Pneumonia
Pneumonia is perhaps the quintessential example of an airspace disease. It is an infection that inflames the air sacs in one or both lungs. The alveoli may fill with fluid or pus, making it difficult for oxygen to reach the bloodstream. Symptoms can range from mild cough and fever to severe respiratory distress, depending on the causative agent and the extent of the infection. Bacterial pneumonia, often caused by Streptococcus pneumoniae, and viral pneumonia, commonly associated with influenza or COVID-19, are prevalent forms.
Acute Respiratory Distress Syndrome (ARDS)
ARDS is a severe, life-threatening form of lung injury that results in widespread inflammation in the lungs. It’s not a primary disease but rather a complication of other illnesses or injuries, such as severe sepsis, pneumonia, trauma, or pancreatitis. In ARDS, the alveolar-capillary membrane becomes damaged, leading to fluid leakage into the alveoli and severe impairment of gas exchange. This results in profound hypoxemia that is often refractory to conventional oxygen therapy.
Obstructive Processes within the Airspaces
Certain conditions cause the airways leading to and within the alveoli to become narrowed or blocked, impeding airflow and gas exchange.
Chronic Obstructive Pulmonary Disease (COPD)
COPD is a progressive lung disease that makes breathing difficult. While it affects both the airways (bronchioles) and the airspaces (alveoli), a significant component involves the destruction and enlargement of airspaces, a condition known as emphysema. In emphysema, the walls of the alveoli are damaged and lose their elasticity, causing them to become floppy and to collapse during exhalation. This trapping of air in the lungs makes it harder to exhale stale air, reducing the capacity for fresh, oxygen-rich air to enter. Chronic bronchitis, another component of COPD, involves inflammation and excessive mucus production in the bronchioles, further contributing to airflow limitation.
Asthma
While primarily considered an airway disease characterized by reversible bronchoconstriction and inflammation, severe or poorly controlled asthma can lead to air trapping and affect alveolar function indirectly. The persistent inflammation and muscle spasms in the airways can limit the amount of air reaching the alveoli, and in chronic cases, structural changes can occur.
Interstitial Lung Diseases (ILDs)

These are a broad group of disorders that cause scarring (fibrosis) of the lung tissue, specifically the interstitium – the tissue and space around the air sacs. However, many ILDs also significantly impact the alveoli themselves.
Idiopathic Pulmonary Fibrosis (IPF)
IPF is a chronic, progressive fibrotic lung disease of unknown cause. It leads to the thickening and scarring of the alveolar walls, making them stiff and less able to expand. As fibrosis progresses, the alveoli become increasingly dysfunctional, leading to severe shortness of breath and impaired oxygen uptake. The scarring can also disrupt the capillary network surrounding the alveoli.
Sarcoidosis
Sarcoidosis is an inflammatory disease characterized by the formation of granulomas (collections of inflammatory cells) in various organs, including the lungs. In the lungs, these granulomas can develop in the interstitium and within the alveolar walls, leading to inflammation, thickening, and eventually fibrosis, affecting gas exchange.
Neoplastic Processes
Cancerous growths within the lungs can also manifest as airspace disease.
Alveolar Cell Carcinoma (Bronchioloalveolar Carcinoma)
A subtype of non-small cell lung cancer, alveolar cell carcinoma (now often referred to as adenocarcinoma in situ or minimally invasive adenocarcinoma) arises from the cells lining the alveoli. It can spread along the alveolar walls, mimicking pneumonia with fluid or consolidation in the airspaces, making it challenging to diagnose.
Environmental and Occupational Exposures
Inhaled substances can directly damage the alveoli, leading to chronic airspace disease.
Pneumoconiosis
This group of lung diseases is caused by inhaling dust particles, such as silica (silicosis), coal dust (coal worker’s pneumoconiosis or black lung disease), or asbestos fibers (asbestosis). These inhaled particles trigger inflammation and fibrosis in the lung tissue, including the alveolar spaces, leading to impaired gas exchange and progressive lung damage. Asbestosis, in particular, directly affects the alveolar walls and interstitium, leading to shortness of breath and an increased risk of mesothelioma and lung cancer.
Diagnosing and Managing Airspace Disease
The diagnosis of airspace disease relies on a combination of clinical assessment, imaging techniques, and physiological tests.
Clinical Evaluation and Symptomatology
Patients with airspace disease typically present with a constellation of symptoms, including:
- Dyspnea (Shortness of Breath): This is the hallmark symptom, often worsening with exertion.
- Cough: Can be dry or productive, depending on the underlying cause.
- Chest Pain: May be sharp or dull, and can be associated with breathing.
- Fatigue: Due to the body’s struggle to obtain sufficient oxygen.
- Wheezing: More common in obstructive processes like asthma or severe COPD.
- Cyanosis: A bluish discoloration of the skin, lips, and nail beds, indicating low blood oxygen levels.
Diagnostic Tools
- Chest X-ray: Can reveal infiltrates, consolidation, hyperinflation, or signs of fibrosis in the lungs, indicative of alveolar involvement.
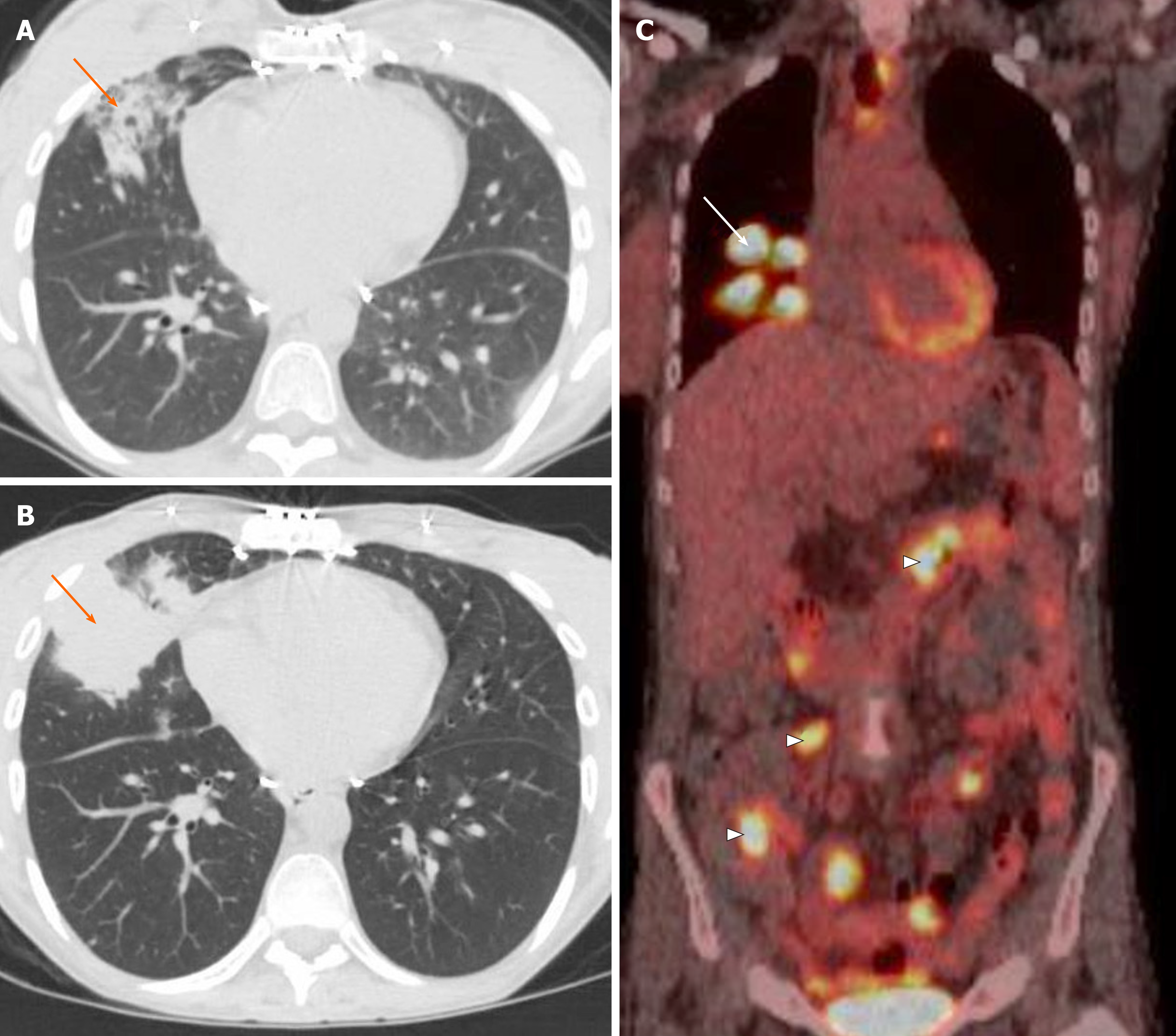
- Computed Tomography (CT) Scan: Provides more detailed images of the lung parenchyma, allowing for better visualization of alveolar damage, interstitial changes, and small nodules.
- Pulmonary Function Tests (PFTs): Measure lung volumes, capacities, and flow rates, helping to assess the severity of airflow obstruction or restriction and the efficiency of gas exchange (e.g., diffusing capacity of the lungs for carbon monoxide, DLCO).
- Arterial Blood Gas (ABG) Analysis: Measures oxygen and carbon dioxide levels in the arterial blood, providing direct evidence of impaired gas exchange.
- Bronchoscopy and Biopsy: In some cases, a bronchoscope can be inserted to visualize airways and collect samples (biopsies) from lung tissue for microscopic examination to determine the specific cause of the disease.
Treatment Approaches
Treatment for airspace disease is highly dependent on the underlying cause. General management strategies often include:
- Pharmacological Therapies:
- Antibiotics: For bacterial infections.
- Antivirals: For viral infections.
- Bronchodilators and Inhaled Corticosteroids: To manage airway inflammation and obstruction in conditions like COPD and asthma.
- Anti-inflammatory Medications: To reduce inflammation in conditions like sarcoidosis.
- Antifibrotic Agents: For progressive fibrotic lung diseases like IPF.
- Oxygen Therapy: Supplemental oxygen is crucial for individuals with chronic hypoxemia to improve oxygenation and reduce the strain on the heart.
- Pulmonary Rehabilitation: A comprehensive program that includes exercise training, education, and support to improve the functional capacity and quality of life for individuals with chronic lung disease.
- Lifestyle Modifications: Smoking cessation is paramount for many airspace diseases, particularly COPD and those related to environmental exposures. Avoiding irritants and allergens is also important.
- Surgical Interventions: In select cases, lung transplantation may be considered for end-stage lung disease.
The Broader Implications of Airspace Health
The concept of “airspace disease” highlights the profound vulnerability of the lungs’ gas exchange units. Factors such as air pollution, occupational hazards, genetic predispositions, and even infectious agents can all contribute to the degradation of these delicate structures. Recognizing the diverse array of conditions that fall under this conceptual umbrella underscores the importance of preventive measures, early diagnosis, and comprehensive management strategies to preserve lung function and ensure the fundamental ability to breathe. The health of our lung’s airspaces is directly linked to our overall well-being, making their protection a critical aspect of public health.
