The human body is a marvel of intricate biological processes, constantly working to maintain equilibrium and protect itself from harm. Among the key players in this complex defense system is fibrinogen, a protein primarily synthesized by the liver. Its role is paramount in the process of blood coagulation, the vital mechanism that stops bleeding when a blood vessel is injured. However, an elevated level of fibrinogen in the blood, often detected through routine blood tests, can signify a range of underlying physiological states and potential health concerns. Understanding what elevated fibrinogen means requires delving into its function, the reasons for its increase, and the implications for overall health.
The Role of Fibrinogen in Hemostasis
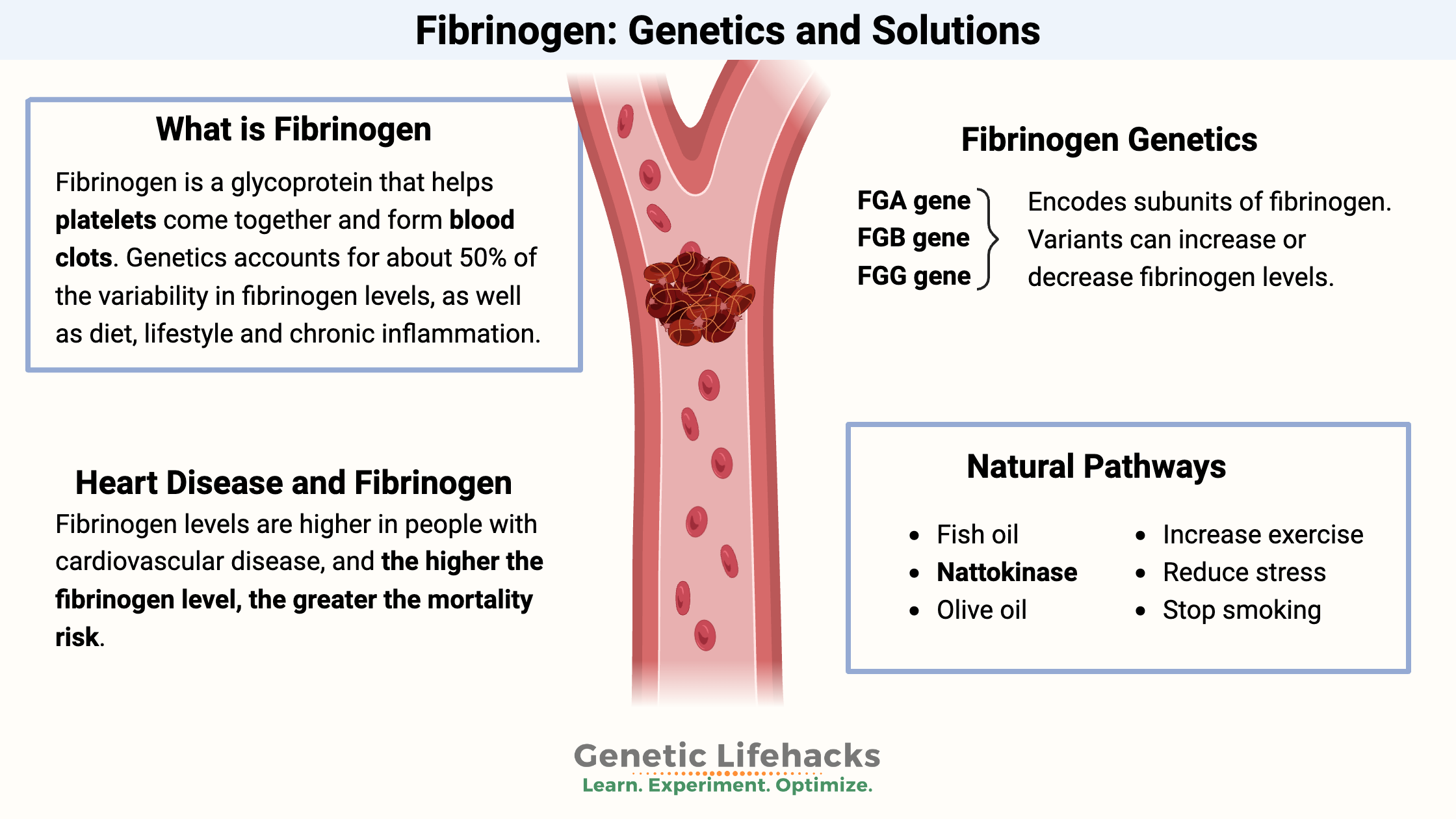
Fibrinogen, also known as Factor I, is a soluble glycoprotein that circulates in the bloodstream. Its primary function is to act as a precursor to fibrin, an insoluble protein that forms the meshwork of a blood clot. When an injury occurs, such as a cut or a bruise, a cascade of biochemical reactions is initiated, culminating in the conversion of fibrinogen into fibrin by the enzyme thrombin. These fibrin strands then weave together, trapping blood cells and platelets to form a stable clot, effectively sealing the damaged blood vessel and preventing excessive blood loss.
This hemostatic process is crucial for survival. Without it, even minor injuries could lead to life-threatening hemorrhages. Fibrinogen’s role is not limited to simply forming a clot; it also plays a part in wound healing and tissue repair by providing a scaffold for migrating cells and promoting cell growth.
However, like many biological processes, fibrinogen levels are tightly regulated. While normal levels are essential for adequate clotting, deviations from the expected range can be indicative of significant physiological changes.
Causes of Elevated Fibrinogen Levels
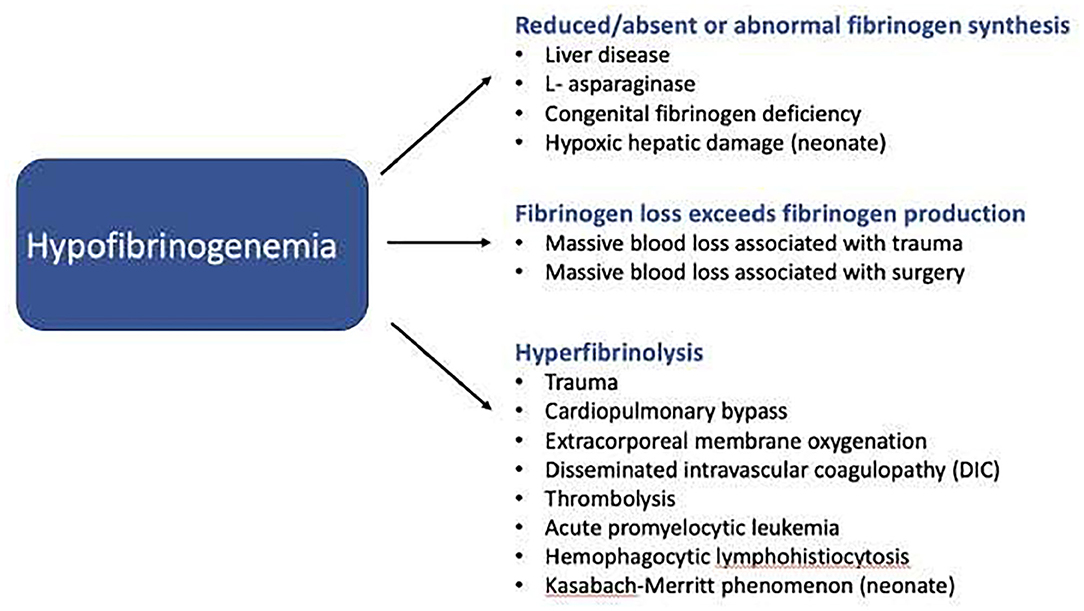
Elevated fibrinogen levels, medically termed hyperfibrinogenemia, are not a disease in themselves but rather a sign that something is amiss within the body. The increase in fibrinogen is often a response to inflammation, infection, or tissue damage. The liver, in its role as a crucial metabolic organ, ramps up fibrinogen production in these situations as part of the acute-phase response. This response is designed to bolster the body’s defenses and initiate repair mechanisms.
Several factors can contribute to elevated fibrinogen:
Inflammation and Infection
One of the most common reasons for elevated fibrinogen is the presence of inflammation. This can be acute, such as from an infection (bacterial, viral, or fungal), or chronic, as seen in autoimmune diseases like rheumatoid arthritis or inflammatory bowel disease. During inflammation, various cytokines are released, signaling the liver to increase the synthesis of acute-phase proteins, including fibrinogen. The elevated fibrinogen can contribute to increased blood viscosity, which may exacerbate inflammatory conditions by impairing microcirculation.
Tissue Injury and Trauma
Any form of tissue damage, from minor bruising to significant trauma like surgery or accidents, will trigger an increase in fibrinogen. The body mobilizes its clotting factors to repair the damaged tissue and prevent bleeding. Post-surgical patients often exhibit elevated fibrinogen levels, which typically normalize as they recover.
Cardiovascular Disease Risk Factors
Perhaps one of the most significant associations with elevated fibrinogen is its role as an independent risk factor for cardiovascular disease, including heart attacks and strokes. Elevated fibrinogen contributes to a pro-thrombotic state, meaning the blood is more prone to clotting. This increased risk is multifactorial:
- Increased Blood Viscosity: Higher fibrinogen levels make blood thicker and more viscous, impeding blood flow, particularly in smaller vessels. This can increase the workload on the heart and contribute to hypertension.
- Enhanced Platelet Aggregation: Fibrinogen acts as a bridge between platelets, facilitating their aggregation and the formation of blood clots. Elevated fibrinogen can enhance this process, making clot formation more likely.
- Endothelial Dysfunction: Inflammation, often linked to elevated fibrinogen, can damage the endothelium, the inner lining of blood vessels. This dysfunction can lead to the buildup of plaque (atherosclerosis) and increase the risk of clot formation within arteries.
- Association with Other Risk Factors: Elevated fibrinogen often coexists with other cardiovascular risk factors such as obesity, diabetes, smoking, and high cholesterol, creating a synergistic increase in risk.
Other Conditions
Beyond inflammation and cardiovascular risks, elevated fibrinogen can also be associated with:
- Malignancy: Cancers, particularly advanced ones, can trigger an inflammatory response and lead to increased fibrinogen levels. This is sometimes referred to as a paraneoplastic syndrome.
- Pregnancy: Fibrinogen levels naturally increase during pregnancy, which is a physiological adaptation to prepare the body for potential blood loss during childbirth. This elevation is generally considered normal.
- Oral Contraceptives and Hormone Replacement Therapy: Estrogen-containing medications can stimulate the liver to produce more fibrinogen, leading to slightly elevated levels.
- Certain Genetic Disorders: While less common, rare genetic mutations can lead to inherited conditions causing abnormally high fibrinogen levels.
Interpreting Elevated Fibrinogen: Clinical Significance and Management
Detecting elevated fibrinogen levels typically occurs as part of a routine blood panel or when investigating specific symptoms. The interpretation of these results is crucial and should always be done in conjunction with a healthcare professional. A single elevated reading may not be cause for immediate alarm, but persistent elevation or a significant increase warrants further investigation.
Diagnostic Considerations
When elevated fibrinogen is identified, a physician will consider several factors to determine the underlying cause:
- Patient History: A thorough review of the patient’s medical history, including existing conditions, medications, lifestyle, and recent events (e.g., illness, surgery), is essential.
- Physical Examination: A physical exam can help identify signs of inflammation, infection, or cardiovascular issues.
- Further Blood Tests: Additional blood tests may be ordered to assess for markers of inflammation (e.g., C-reactive protein – CRP), infection (e.g., white blood cell count), or other underlying conditions. Specific tests may be done to rule out coagulation disorders or genetic predispositions.
- Imaging Studies: Depending on the suspected cause, imaging techniques like ultrasound, CT scans, or MRI may be employed.
Management and Treatment
The management of elevated fibrinogen is primarily directed at treating the underlying cause.
- Treating Inflammation and Infection: If an infection or inflammatory disease is identified, appropriate antibiotics, antiviral medications, or anti-inflammatory drugs will be prescribed. For autoimmune conditions, therapies aimed at suppressing the immune system may be used.
- Lifestyle Modifications for Cardiovascular Health: For individuals with elevated fibrinogen as a cardiovascular risk factor, comprehensive lifestyle changes are paramount. This includes:
- Healthy Diet: Emphasizing fruits, vegetables, whole grains, lean proteins, and healthy fats, while limiting saturated and trans fats, sodium, and added sugars.
- Regular Exercise: Aiming for at least 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity activity per week, along with muscle-strengthening exercises.
- Weight Management: Achieving and maintaining a healthy body weight can significantly reduce cardiovascular risk.
- Smoking Cessation: Quitting smoking is one of the most impactful steps an individual can take to improve cardiovascular health.
- Moderate Alcohol Consumption: If alcohol is consumed, it should be in moderation.
- Medications: In some cases, medications may be prescribed to manage specific conditions contributing to elevated fibrinogen, such as antihypertensives, statins for cholesterol management, or anticoagulants if a thrombotic event is a significant concern. Research is also ongoing into the potential benefits of certain medications that may directly influence fibrinogen levels or their impact on cardiovascular risk.

Prognosis and Long-Term Outlook
The prognosis for individuals with elevated fibrinogen depends heavily on the underlying cause and the effectiveness of treatment. If the elevation is due to a temporary condition like a mild infection or minor surgery, fibrinogen levels will typically return to normal as the body recovers.
However, when elevated fibrinogen is a persistent marker of chronic inflammation or a significant risk factor for cardiovascular disease, long-term management is crucial. Regular monitoring of fibrinogen levels, along with other cardiovascular risk markers, allows healthcare providers to track progress and adjust treatment strategies as needed. Proactive management and adherence to medical advice can significantly mitigate the risks associated with persistently high fibrinogen levels, promoting a healthier and longer life.
In conclusion, elevated fibrinogen is a complex biomarker that signals an underlying physiological response, most commonly related to inflammation, infection, tissue injury, or cardiovascular disease risk. Its interpretation requires a comprehensive clinical assessment, and its management focuses on addressing the root cause. By understanding the significance of elevated fibrinogen and working closely with healthcare professionals, individuals can take proactive steps to manage their health and reduce potential risks.
