In an increasingly complex healthcare landscape, where costs continually rise and the demand for flexible, personalized benefits intensifies, innovative solutions are paramount. Among these, Health Reimbursement Arrangements (HRAs) stand out as a significant development, representing a unique blend of financial innovation and technological enablement in employer-sponsored healthcare. While not “insurance” in the traditional sense, HRAs function as employer-funded accounts designed to reimburse employees for qualified medical expenses and, in many cases, health insurance premiums. This system embodies a forward-thinking approach to benefits, leveraging structured financial mechanisms and often digital platforms to offer unprecedented flexibility and control.
From the perspective of “Tech & Innovation,” HRAs are more than just a financial tool; they are a testament to the power of structured innovation in addressing complex socio-economic challenges. They represent a shift from one-size-fits-all group health plans to a more consumer-driven model, facilitated by advanced administrative technologies. The ability to customize, administer, and integrate these plans effectively relies heavily on robust software, data analytics, and user-friendly digital interfaces that manage reimbursements, track expenses, and ensure regulatory compliance. This article delves into the core mechanics of HRAs, explores their diverse applications, highlights the technological underpinnings that enable their success, and considers their evolving role in modern benefits strategy.
Decoding the HRA Framework: A Technological Leap in Benefit Design
At its core, an HRA is an employer-funded, tax-advantaged account that employees can use to pay for qualified medical expenses. Unlike traditional health insurance, the funds in an HRA are not pre-paid premiums; rather, they are set aside by the employer and used to reimburse employees after they incur eligible costs. This model is a significant departure from conventional benefits, demanding innovative administrative solutions to manage the flow of funds, eligibility, and expense verification. The innovation lies not just in the financial structure but equally in the technology that makes it feasible for businesses of all sizes to offer such a sophisticated benefit.

Core Mechanics and Digital Administration
The fundamental operation of an HRA is elegantly simple yet requires sophisticated backend technology. An employer sets an annual allowance for each eligible employee. When an employee incurs a qualified medical expense (e.g., doctor visit co-pay, prescription, deductible payment, or even health insurance premiums, depending on the HRA type), they submit a claim to their HRA administrator. The administrator, typically a third-party provider leveraging specialized software platforms, verifies the expense against IRS guidelines and the specific HRA plan design. Upon approval, the employee is reimbursed from the employer’s designated HRA funds.
This process, while seemingly straightforward, is ripe for technological integration. Digital administration platforms are crucial for:
- Claim Submission & Processing: Allowing employees to submit claims easily via web portals or mobile apps, often with features like photo upload for receipts, significantly streamlines the process. Automated verification tools can flag common errors or suspicious claims.
- Eligibility Tracking: Managing who is eligible, what expenses are covered, and what balances remain requires dynamic databases and real-time updates.
- Compliance & Reporting: HRAs are subject to various IRS and federal regulations (e.g., ERISA, ACA). Advanced software solutions ensure plans remain compliant, generate necessary reports, and update automatically with regulatory changes, significantly reducing administrative burden and risk for employers.
- Communication & Education: Digital portals serve as central hubs for employees to understand their HRA, view their balance, check claim status, and access educational resources, fostering greater engagement and informed healthcare decisions.

The Evolution of Employer-Sponsored Health Tech
The advent and popularization of HRAs mark an evolutionary step in employer-sponsored health benefits, driven by technological advancements. Historically, employers either offered a traditional group health plan or nothing at all. The HRA, particularly newer iterations like the Individual Coverage HRA (ICHRA), represents a paradigm shift towards defined contribution healthcare. This shift is empowered by:
- Platform Agnosticism: Modern HRA platforms can integrate with a wide array of individual health insurance plans, allowing employees unprecedented choice.
- Scalability: Digital solutions allow HRAs to be administered effectively for companies of all sizes, from small businesses using Qualified Small Employer HRAs (QSEHRAs) to large enterprises implementing ICHRAs for thousands of employees across diverse workforces.
- Data-Driven Customization: The technological infrastructure collects valuable data on utilization patterns, helping employers fine-tune their HRA offerings, optimize allowances, and understand employee needs better, leading to more strategic benefits design.
Diverse HRA Models: Tailored Solutions through Configurable Platforms
One of the most innovative aspects of HRAs is their adaptability. Unlike a single, monolithic insurance product, HRAs come in several distinct models, each designed to meet specific employer needs and employee demographics. This customization is largely enabled by highly configurable digital platforms that can implement varying rules, eligibility criteria, and integration requirements.
ICHRA: Enabling Individual Control with Digital Tools
The Individual Coverage HRA (ICHRA), introduced in 2020, is perhaps the most revolutionary HRA model. It allows employers of any size to offer tax-free reimbursements for individual health insurance premiums and other qualified medical expenses. Employees purchase their own individual health insurance plan, either on or off the public marketplace, and the ICHRA then reimburses them for premiums and other out-of-pocket costs up to an employer-set allowance.
The “tech” in ICHRA is critical:
- Marketplace Integration: Employees often use digital marketplaces to select individual health plans. HRA administration platforms must integrate seamlessly, allowing verification that an employee is enrolled in qualifying individual coverage before reimbursements can be made.
- Personalization at Scale: ICHRAs allow employers to offer different allowances based on legitimate employee classes (e.g., age, family size, geographic location). Managing these complex rules for potentially thousands of employees requires sophisticated software logic and robust data management.
- Compliance Verification: Ensuring that employees are enrolled in individual health plans meeting minimum essential coverage requirements is a key compliance challenge, handled by automated verification processes within HRA platforms.
QSEHRA & GCHRA: Streamlining Small Business Health Strategies
The Qualified Small Employer HRA (QSEHRA) and the Group Coverage HRA (GCHRA) represent other innovative applications of the HRA model, each addressing specific market needs:
- QSEHRA (Small Business Focus): Designed for businesses with fewer than 50 full-time employees that do not offer a traditional group health plan. QSEHRAs allow small businesses to reimburse employees for individual health insurance premiums and qualified medical expenses within IRS-defined limits. The innovation here is enabling small businesses, often resource-constrained, to offer a valuable health benefit without the administrative complexity or cost of a full group plan. Digital platforms simplify the administration, making it accessible even for businesses without dedicated HR departments.
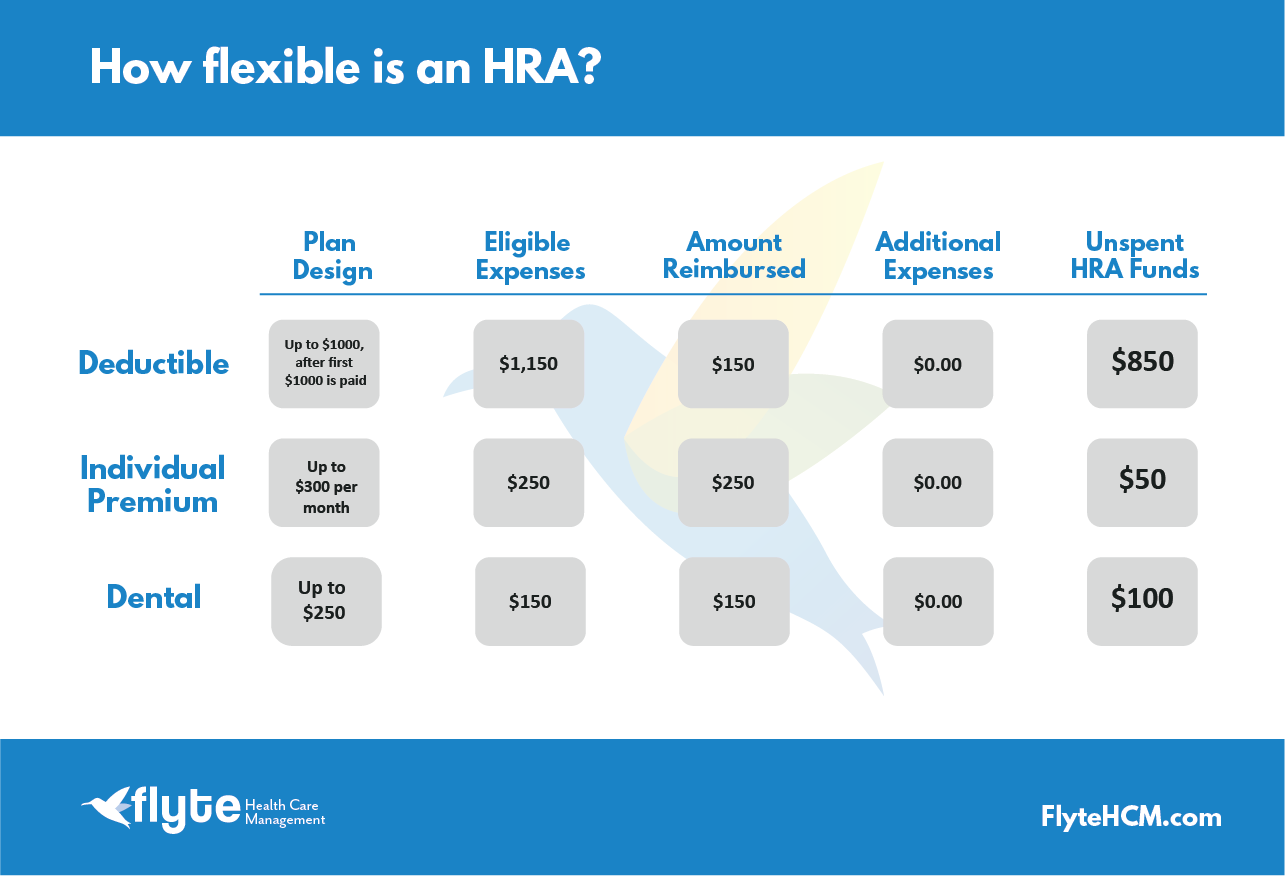
- GCHRA (Complementing Group Plans): Also known as a “Deductible HRA,” a GCHRA is used by employers of any size to supplement a traditional group health plan. Typically, it reimburses employees for out-of-pocket medical expenses, such as deductibles, co-pays, and co-insurance, that are not covered by the primary group plan. This is an innovative way to make high-deductible health plans more attractive and affordable, with technology managing the interplay between the HRA and the underlying group plan’s benefits.
The Technological Edge: Benefits and Impact for Stakeholders
The technological infrastructure underpinning HRAs delivers significant benefits to both employers and employees, driving greater efficiency, personalization, and strategic advantage in healthcare.
Empowering Employees through Digital Access and Choice
For employees, HRAs, particularly ICHRA and QSEHRA, represent a leap forward in personal choice and control over their healthcare. The technological innovation allows for:
- Personalized Plan Selection: Employees can choose individual health insurance plans that best fit their specific needs, doctors, and prescription requirements, rather than being confined to a single employer-selected option. This is facilitated by access to individual health insurance marketplaces, often linked or understood by HRA platforms.
- Simplified Expense Management: User-friendly mobile apps and web portals make submitting claims, tracking balances, and understanding eligible expenses straightforward. This reduces administrative friction and empowers employees to actively manage their healthcare spending.
- Financial Predictability: By knowing their HRA allowance upfront, employees can better budget for healthcare costs, especially when paired with high-deductible health plans. Digital tools often provide real-time balance updates, further aiding financial planning.
Optimizing Employer Strategies with Data-Driven Insights
Employers gain substantial advantages from the innovative design and technological administration of HRAs:
- Cost Control and Predictability: HRAs allow employers to set a fixed contribution amount per employee, making healthcare costs predictable year-over-year. This contrasts sharply with traditional group plans where premium increases can be volatile.
- Administrative Efficiency: Modern HRA platforms automate much of the administrative burden, from eligibility checks to reimbursement processing and compliance reporting. This frees up HR staff to focus on more strategic initiatives.
- Strategic Benefits Design: Advanced analytics capabilities within HRA platforms can provide insights into employee utilization patterns and preferences. This data can inform future benefit design, allowing employers to refine allowances and offerings to maximize employee satisfaction and cost-effectiveness.
- Attraction and Retention: Offering flexible and competitive health benefits, enabled by HRAs, is a powerful tool for attracting and retaining top talent, demonstrating an employer’s commitment to employee well-being through innovative benefit solutions.
Navigating the Digital Landscape: Eligibility and Integration Challenges
Implementing an HRA effectively requires careful consideration of eligibility rules and seamless integration with existing systems. The “Tech & Innovation” aspect here revolves around building robust systems that can handle complexity, ensure compliance, and provide a unified user experience.
Ensuring Compliance via Robust Tech Solutions
HRAs are governed by a complex web of federal regulations, including the Affordable Care Act (ACA), ERISA, and IRS codes. Non-compliance can lead to significant penalties. This is where advanced compliance technology becomes invaluable:
- Automated Compliance Checks: HRA platforms are designed to automatically enforce rules such as affordability requirements (for ICHRAs), maximum contribution limits (for QSEHRAs), and HIPAA privacy regulations.
- Reporting & Disclosure: Generating accurate annual reports, like those required by the ACA, is automated, simplifying a potentially burdensome task for employers.
- Real-time Regulatory Updates: Leading HRA technology providers continuously monitor regulatory changes and update their platforms, ensuring that clients remain compliant without manual intervention.
Seamless Integration with Modern Health Platforms
For HRAs to be truly innovative and effective, they must integrate smoothly with other healthcare and HR technologies. This includes:
- Payroll Systems: To facilitate accurate contributions and manage employee deductions where applicable.
- HRIS (Human Resources Information Systems): For employee data synchronization, ensuring accurate eligibility and enrollment information.
- Individual Insurance Marketplaces: Especially for ICHRAs, the ability to verify individual plan enrollment is paramount and requires data exchange or verification protocols.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): Employees often have multiple benefit accounts, and good HRA platforms can provide a consolidated view or at least ensure compatibility, preventing potential conflicts or inefficiencies.
The Future of HRA: Continuous Innovation in HealthTech
The evolution of HRAs is far from complete. As healthcare technology continues to advance, so too will the capabilities and applications of these innovative financial arrangements. The future will likely see an even deeper integration of artificial intelligence, predictive analytics, and enhanced user experience design.
AI and Predictive Analytics in HRA Optimization
Artificial intelligence and machine learning hold immense potential for further optimizing HRA design and administration. AI could be used to:
- Personalize Allowances: Beyond standard classifications, AI could analyze individual health risk factors, past utilization, and demographic data to recommend highly personalized HRA allowances, maximizing value for both employer and employee.
- Predict Healthcare Costs: Leveraging vast datasets, AI could provide more accurate predictions of future healthcare costs, helping employers set HRA allowances more strategically and manage financial risk.
- Automate Claim Verification: Advanced AI could further streamline claim processing, quickly identifying fraudulent claims or automatically approving common, low-risk expenses, reducing manual review.
Enhancing User Experience through Advanced Digital Interfaces
The user experience (UX) of HRA platforms will continue to evolve, moving towards more intuitive, proactive, and integrated digital interfaces:
- Proactive Guidance: Future platforms could use AI to offer proactive advice to employees on how to best utilize their HRA funds, recommend cost-effective providers, or even suggest preventive care based on their health profile.
- Gamification and Engagement: Incorporating gamification elements could encourage healthier behaviors and more engaged management of healthcare finances.
- Consolidated Health Wallets: Imagine a single digital “health wallet” that seamlessly integrates HRA funds with HSAs, FSAs, and even loyalty programs, providing a holistic view and management tool for all health-related financial resources.
In conclusion, “what is an HRA insurance” unveils a fascinating area of “Tech & Innovation” within the broader health and financial technology landscape. HRAs are not merely a product; they are an innovative framework that leverages sophisticated digital platforms, data-driven insights, and configurable structures to redefine employer-sponsored healthcare. By empowering employees with choice and giving employers predictable cost control and administrative efficiency, HRAs stand as a prime example of how technology and innovative design can address complex societal needs, signaling a vibrant future for consumer-driven healthcare.
