Calcium channel blockers are a class of medications primarily used to manage a variety of cardiovascular conditions. They work by affecting the movement of calcium into certain cells, particularly those in the heart and blood vessels. This action leads to a cascade of physiological effects that ultimately help to reduce the workload on the heart and improve blood flow. While their primary application is in treating high blood pressure and certain heart rhythm disorders, they also find utility in managing angina (chest pain) and, in some specific instances, other non-cardiovascular conditions.
How Do Calcium Channel Blockers Work?
The efficacy of calcium channel blockers (CCBs) stems from their specific interaction with calcium channels, which are protein structures embedded in the cell membranes of cardiac muscle cells and smooth muscle cells lining blood vessels. These channels act as gates, regulating the influx of calcium ions (Ca²⁺) into the cell. Calcium plays a critical role in initiating and sustaining muscle contraction.

The Role of Calcium in Cellular Function
In the context of the cardiovascular system, calcium influx triggers several essential processes:
- Cardiac Muscle Contraction: When an electrical impulse reaches a cardiac muscle cell, it opens voltage-gated calcium channels. The influx of calcium ions into the cell causes a release of even more calcium from intracellular stores. This rise in intracellular calcium concentration binds to contractile proteins (actin and myosin), leading to the shortening of muscle fibers and thus, the pumping action of the heart.
- Blood Vessel Smooth Muscle Contraction: Similarly, calcium entry into the smooth muscle cells that form the walls of blood vessels is crucial for maintaining vascular tone. When these smooth muscle cells contract, the blood vessels narrow (vasoconstriction), which increases blood pressure. When they relax, the vessels widen (vasodilation), decreasing blood pressure.
Mechanisms of Action of Calcium Channel Blockers
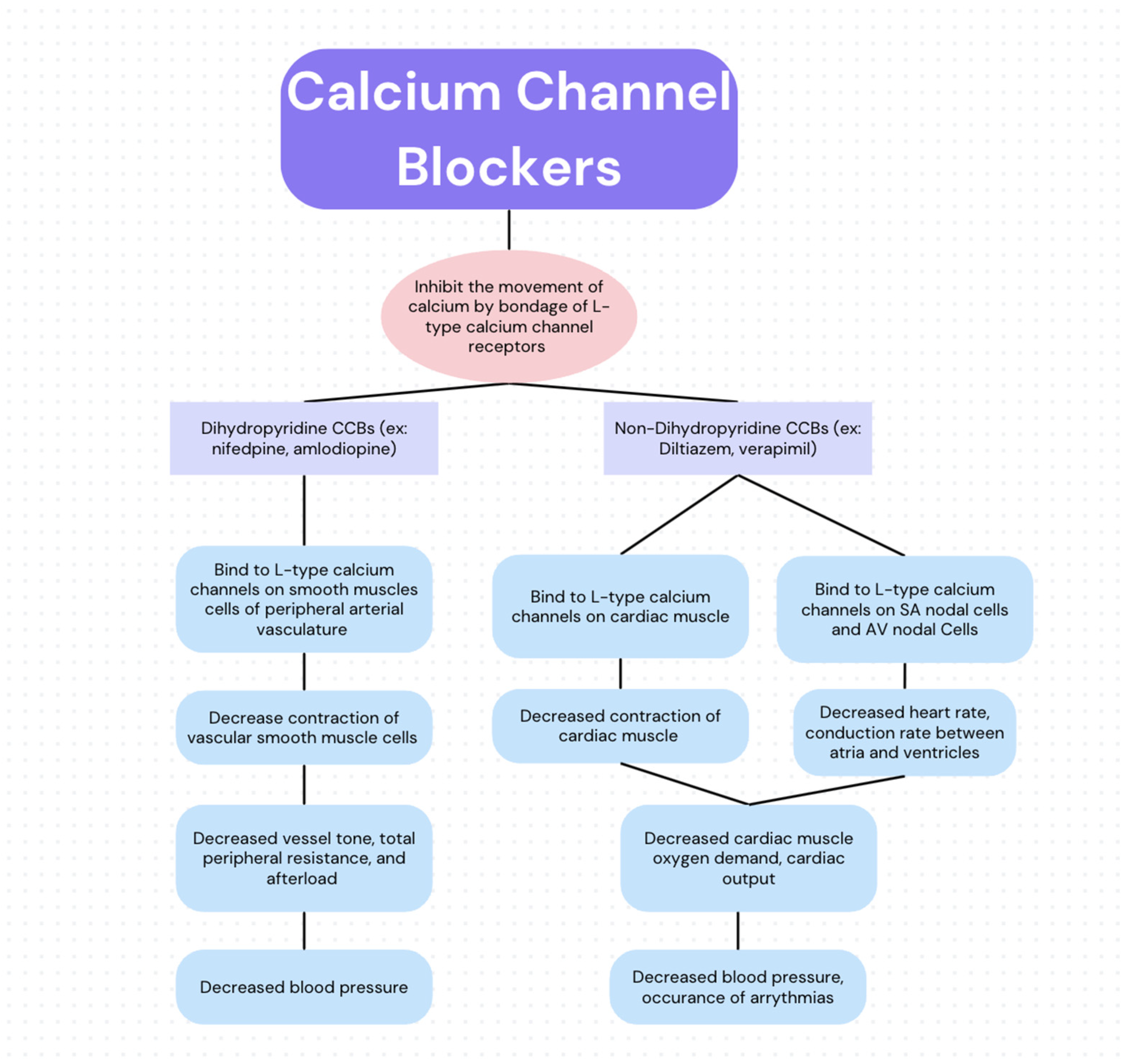
Calcium channel blockers interrupt this process by binding to specific types of calcium channels, primarily L-type calcium channels, and inhibiting the flow of calcium ions into the cells. The specific effects of CCBs depend on their selectivity for different tissues and types of calcium channels. Broadly, CCBs can be categorized based on their primary sites of action and chemical structure, leading to distinct therapeutic outcomes.
Types of Calcium Channel Blockers
Calcium channel blockers are generally divided into three main classes, distinguished by their chemical structure and their effects on the heart and blood vessels:
Dihydropyridines (DHPs)
Dihydropyridine CCBs are characterized by their potent vasodilatory effects. They primarily target the L-type calcium channels in the smooth muscle cells of blood vessels.
- Mechanism: By blocking calcium entry into vascular smooth muscle cells, DHPs cause these muscles to relax, leading to vasodilation (widening of blood vessels). This reduced peripheral resistance makes it easier for the heart to pump blood, thereby lowering blood pressure.
- Therapeutic Uses: DHPs are highly effective in treating hypertension (high blood pressure). They are also used to manage chronic stable angina.
- Examples: Common dihydropyridines include amlodipine (Norvasc), nifedipine (Procardia XL, Adalat CC), and felodipine (Plendil).
- Key Characteristics: These agents tend to have a more pronounced effect on blood vessels than on the heart’s electrical system or contractility. Side effects often relate to vasodilation, such as flushing, headache, and peripheral edema (swelling in the ankles and feet).
Non-dihydropyridines (Non-DHPs)
Non-dihydropyridine CCBs have a dual effect, impacting both the heart muscle and the blood vessels. They are further subdivided into two distinct groups: phenylalkylamines and benzothiazepines.
- Phenylalkylamines (e.g., Verapamil): Verapamil exhibits significant effects on both cardiac contractility and heart rate. It slows down the electrical conduction through the atrioventricular (AV) node, which is crucial for regulating the heart’s rhythm. This makes it effective for treating supraventricular tachycardias (rapid heart rhythms originating in the atria) and for rate control in atrial fibrillation. It also has vasodilatory properties, though generally less potent than DHPs.
- Benzothiazepines (e.g., Diltiazem): Diltiazem shares properties with both verapamil and the dihydropyridines. It reduces heart rate and contractility and also causes vasodilation. This balanced profile makes it a versatile option for hypertension, angina, and certain arrhythmias.
- Therapeutic Uses: Non-DHPs are used for hypertension, chronic stable angina, and supraventricular arrhythmias.
- Key Characteristics: Compared to DHPs, non-DHPs can have more pronounced effects on the heart, potentially leading to bradycardia (slow heart rate) or decreased cardiac output. They are generally not recommended for patients with certain heart conditions, such as severe heart failure with reduced ejection fraction.
Other Less Common Classes
While the above two categories represent the vast majority of CCBs used clinically, some older or less frequently prescribed agents exist, such as certain older dihydropyridines with different pharmacological profiles. However, for practical purposes, the DHP and non-DHP classifications are most relevant.
Therapeutic Applications of Calcium Channel Blockers
Calcium channel blockers are a cornerstone in the management of several cardiovascular diseases due to their ability to modulate cardiac function and vascular tone.
Management of Hypertension
Hypertension, or high blood pressure, is a major risk factor for heart disease, stroke, and kidney problems. CCBs effectively lower blood pressure by:
- Vasodilation: Dihydropyridines, in particular, relax the smooth muscles in the walls of arteries, causing them to widen. This decreases the resistance the heart has to pump against, thus lowering blood pressure.
- Reduced Cardiac Output: Non-dihydropyridines can also decrease the force of heart contractions and slow the heart rate, which contributes to lowering blood pressure.
CCBs are often used as first-line therapy for hypertension, either alone or in combination with other antihypertensive medications like ACE inhibitors, ARBs, or diuretics. Their effectiveness and tolerability profile make them a valuable tool for achieving and maintaining target blood pressure levels.
Treatment of Angina
Angina is chest pain or discomfort that occurs when the heart muscle doesn’t get enough oxygen-rich blood. This typically happens during physical exertion or emotional stress. CCBs help to relieve and prevent angina by:
- Reducing Myocardial Oxygen Demand: By slowing the heart rate and decreasing the force of contractions (especially non-DHPs), CCBs reduce the amount of oxygen the heart muscle needs.
- Increasing Myocardial Oxygen Supply: Dihydropyridines improve blood flow to the heart muscle by dilating the coronary arteries, which supply blood to the heart itself. This can help to overcome blockages in these arteries and ensure adequate oxygen delivery.
CCBs are particularly useful for patients with vasospastic angina (Prinzmetal’s angina), where the coronary arteries narrow unexpectedly due to spasms.
Management of Arrhythmias
Certain calcium channel blockers, primarily the non-dihydropyridines like verapamil and diltiazem, play a significant role in managing irregular heart rhythms (arrhythmias). Their ability to slow conduction through the AV node is key:
- Rate Control in Atrial Fibrillation: In atrial fibrillation, the upper chambers of the heart (atria) beat chaotically, leading to a rapid and irregular ventricular response. Non-DHPs can slow down the rate at which these impulses are transmitted to the ventricles, resulting in a more controlled and less damaging heart rate.
- Termination of Supraventricular Tachycardias: Some types of rapid heart rhythms originating above the ventricles can be terminated by the AV nodal blocking effects of verapamil and diltiazem.
It’s important to note that CCBs are generally not used for arrhythmias originating in the ventricles, and their use in patients with certain types of heart block requires careful consideration.
Other Potential Applications
While less common, calcium channel blockers may be prescribed for other conditions:
- Raynaud’s Phenomenon: This condition involves spasms of small blood vessels, typically in the fingers and toes, causing them to become cold and numb. CCBs, particularly dihydropyridines, can help by relaxing these blood vessels and improving blood flow.
- Migraine Prophylaxis: Some studies suggest that certain CCBs might be effective in preventing migraines, though they are not a first-line treatment.
- Pulmonary Hypertension: In specific types of pulmonary hypertension, certain CCBs may be used to help relax the blood vessels in the lungs.
Side Effects and Precautions
Like all medications, calcium channel blockers can cause side effects. The nature and severity of these effects often depend on the specific type of CCB and the individual patient.
Common Side Effects
- Peripheral Edema: Swelling in the ankles and feet is a common side effect, particularly with dihydropyridines, due to vasodilation.
- Headache and Flushing: These are also related to the vasodilatory effects of CCBs.
- Constipation: This is more frequently observed with verapamil.
- Dizziness and Lightheadedness: This can occur if blood pressure drops too low.
- Bradycardia: A slow heart rate, especially with non-dihydropyridines.
- Gastrointestinal Upset: Nausea or stomach discomfort.
Serious Side Effects and Precautions
- Heart Failure: Non-dihydropyridines can worsen heart failure in some individuals by reducing contractility. They are generally contraindicated in patients with significantly impaired left ventricular function.
- Heart Block: In individuals with pre-existing conduction abnormalities, CCBs can exacerbate heart block.
- Hypotension: Excessive lowering of blood pressure can lead to dizziness, fainting, and falls.
- Gingival Hyperplasia: An overgrowth of gum tissue can occur with long-term use of certain CCBs, particularly nifedipine.
- Drug Interactions: CCBs can interact with other medications, including beta-blockers (increasing the risk of bradycardia and heart failure), grapefruit juice (which can increase the levels of some CCBs), and certain antifungal or antibiotic medications.
Precautions:
- Patients with certain pre-existing conditions, such as severe heart failure, significant bradycardia, or certain types of heart block, may not be suitable candidates for CCB therapy.
- It is crucial for patients to inform their healthcare provider about all other medications, supplements, and herbal remedies they are taking to avoid potentially dangerous interactions.
- CCBs should be taken exactly as prescribed, and patients should not stop taking them abruptly without consulting their doctor, as this can lead to a rebound increase in blood pressure or chest pain.

Conclusion
Calcium channel blockers are a diverse and essential group of medications that play a critical role in managing a wide spectrum of cardiovascular conditions. By modulating the influx of calcium ions into cardiac and vascular smooth muscle cells, they effectively lower blood pressure, alleviate chest pain, and control abnormal heart rhythms. Understanding the different classes of CCBs, their specific mechanisms of action, and their therapeutic applications, alongside potential side effects and necessary precautions, is paramount for both healthcare professionals and patients to ensure optimal and safe treatment outcomes. As research continues, the understanding and application of these vital drugs will undoubtedly evolve, further enhancing their contribution to cardiovascular health.
