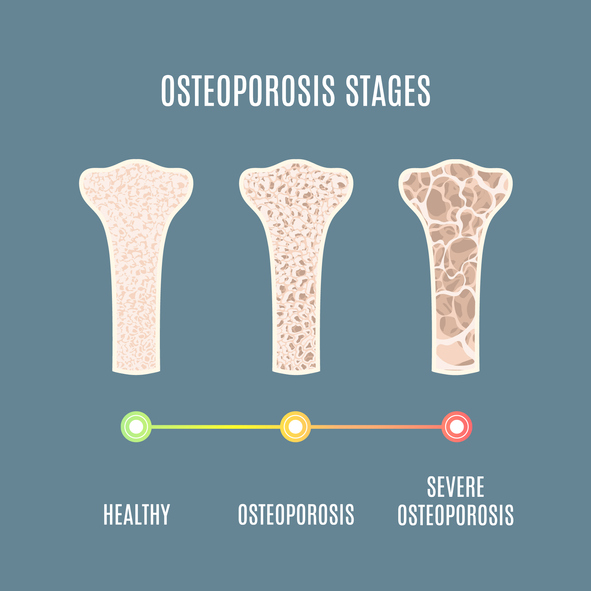
Osteoporosis is often called a “silent disease” because bone loss occurs without symptoms until a fracture happens. Fortunately, medical science has advanced significantly, offering a variety of treatments designed to slow bone loss, increase bone density, and—most importantly—prevent life-altering fractures.
If you or a loved one are navigating a diagnosis, here is a breakdown of the primary osteoporosis treatments available today.
1. Bisphosphonates: The Most Common Prescription
Bisphosphonates are the most frequently prescribed medications for osteoporosis. They work by slowing down the cells that break down bone (osteoclasts), allowing the bone-building cells to keep pace.
- Common drugs: Alendronate (Fosamax), Risedronate (Actonel), Ibandronate (Boniva), and Zoledronic acid (Reclast).
- Delivery: These can be taken as daily or weekly pills, or as a yearly intravenous (IV) infusion.
- Key Consideration: Oral bisphosphonates must be taken on an empty stomach with a full glass of water, and you must remain upright for 30–60 minutes to prevent esophageal irritation.
2. Monoclonal Antibody Medications (Denosumab)
For those who cannot tolerate bisphosphonates or have significantly low bone density, Denosumab (Prolia) is a common alternative.
- How it works: It prevents the development of osteoclasts, significantly reducing bone resorption.
- Delivery: It is administered as an injection under the skin once every six months.
- Note: Unlike bisphosphonates, if you stop taking Denosumab, the benefits wear off quickly, so it is vital to maintain a strict schedule or transition to another medication.
3. Bone-Building (Anabolic) Agents
While most treatments slow bone loss, anabolic agents actually stimulate the body to produce new bone. These are typically reserved for people with very low bone density or a history of multiple fractures.

- Teriparatide (Forteo) and Abaloparatide (Tymlos): These are synthetic versions of the parathyroid hormone. They require daily self-injections for up to two years.
- Romosozumab (Evenity): This is a newer “dual-acting” drug that both increases bone formation and decreases bone breakdown. It is given as a monthly injection at a doctor’s office for one year.
4. Hormone Replacement Therapy (HRT)
Since the drop in estrogen during menopause is a primary cause of bone loss in women, Hormone Replacement Therapy can be used to maintain bone density.
- Estrogen Therapy: Effective for preventing bone loss in postmenopausal women.
- SERMs (Raloxifene): Selective Estrogen Receptor Modulators provide the bone-strengthening benefits of estrogen without some of the risks associated with traditional HRT.
5. Essential Supplements: The Foundation
Medication alone is often not enough. Your body needs the “raw materials” to build bone.
- Calcium: The primary building block of bone. Most adults need 1,000 to 1,200 mg per day through diet or supplements.
- Vitamin D: Essential for calcium absorption. Many people with osteoporosis require Vitamin D3 supplements, as it is difficult to get enough from sunlight and food alone.
6. Lifestyle and Physical Therapy
Treatment is most effective when paired with a “bone-healthy” lifestyle:
- Weight-Bearing Exercise: Activities like walking, jogging, dancing, and weightlifting stress the bones in a healthy way, signaling them to grow stronger.
- Fall Prevention: Since the goal of treatment is to prevent fractures, physical therapy to improve balance and “fall-proofing” your home (removing rugs, improving lighting) is a critical part of a treatment plan.
- Avoiding Bone Depletors: Quitting smoking and limiting alcohol consumption are essential, as both interfere with the body’s ability to maintain bone mass.
Conclusion: Which Treatment is Right for You?
The “best” osteoporosis treatment depends on your age, sex, bone density (T-score), and history of previous fractures. Many doctors now use a “sequential” approach—starting with a bone-builder for a year or two and then switching to a bisphosphonate to “lock in” the gains.
Always consult with a healthcare professional (such as an endocrinologist or rheumatologist) to develop a personalized plan tailored to your specific health profile.
