The question of “what is your regular blood pressure” is a fundamental one, touching upon a crucial aspect of personal health and well-being. It’s not merely a number, but a vital sign that offers insights into the health of your cardiovascular system. Understanding what constitutes “regular” blood pressure, why it fluctuates, and how to maintain it is essential for proactive health management. This article will delve into the intricacies of blood pressure, demystifying the readings and empowering you with knowledge to keep your cardiovascular system in optimal condition.
Understanding the Basics of Blood Pressure
Blood pressure is the force of blood pushing against the walls of your arteries as your heart pumps it around your body. This continuous process is essential for delivering oxygen and nutrients to all your tissues and organs. The measurement of blood pressure is expressed as two numbers: the systolic pressure and the diastolic pressure.
Systolic Pressure: The Force During Heartbeats
The systolic pressure, the top number in a blood pressure reading, represents the maximum pressure exerted on your artery walls when your heart contracts, or beats. This contraction pumps blood out into the arteries. A healthy systolic pressure is generally considered to be below 120 mmHg (millimeters of mercury). Elevated systolic pressure can be an indicator of increased strain on the heart and blood vessels.
Diastolic Pressure: The Pressure Between Heartbeats
The diastolic pressure, the bottom number in a blood pressure reading, represents the minimum pressure in your arteries when your heart rests between beats. During this resting phase, the heart chambers refill with blood. A healthy diastolic pressure is generally considered to be below 80 mmHg. While often less emphasized than systolic pressure, consistently high diastolic pressure also signifies potential cardiovascular issues.
What are “Normal” Blood Pressure Ranges?
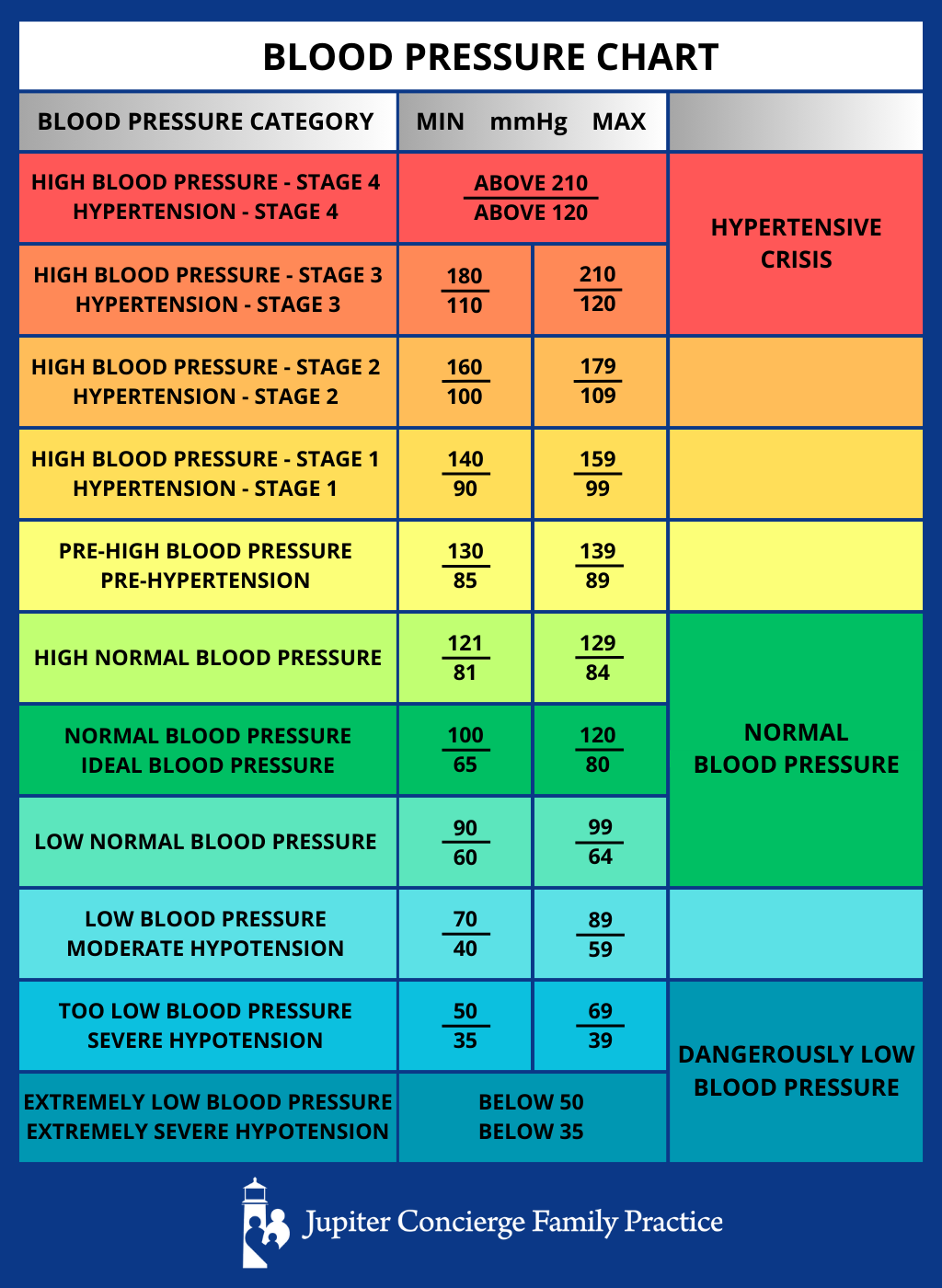
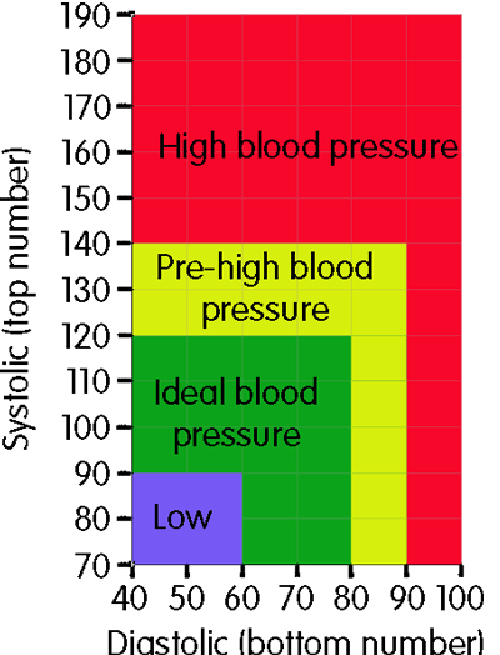
Defining “regular” or “normal” blood pressure is more nuanced than a single set of figures. While the ideal is generally cited as below 120/80 mmHg, individual variations exist. Medical professionals categorize blood pressure readings into several groups to guide diagnosis and treatment:
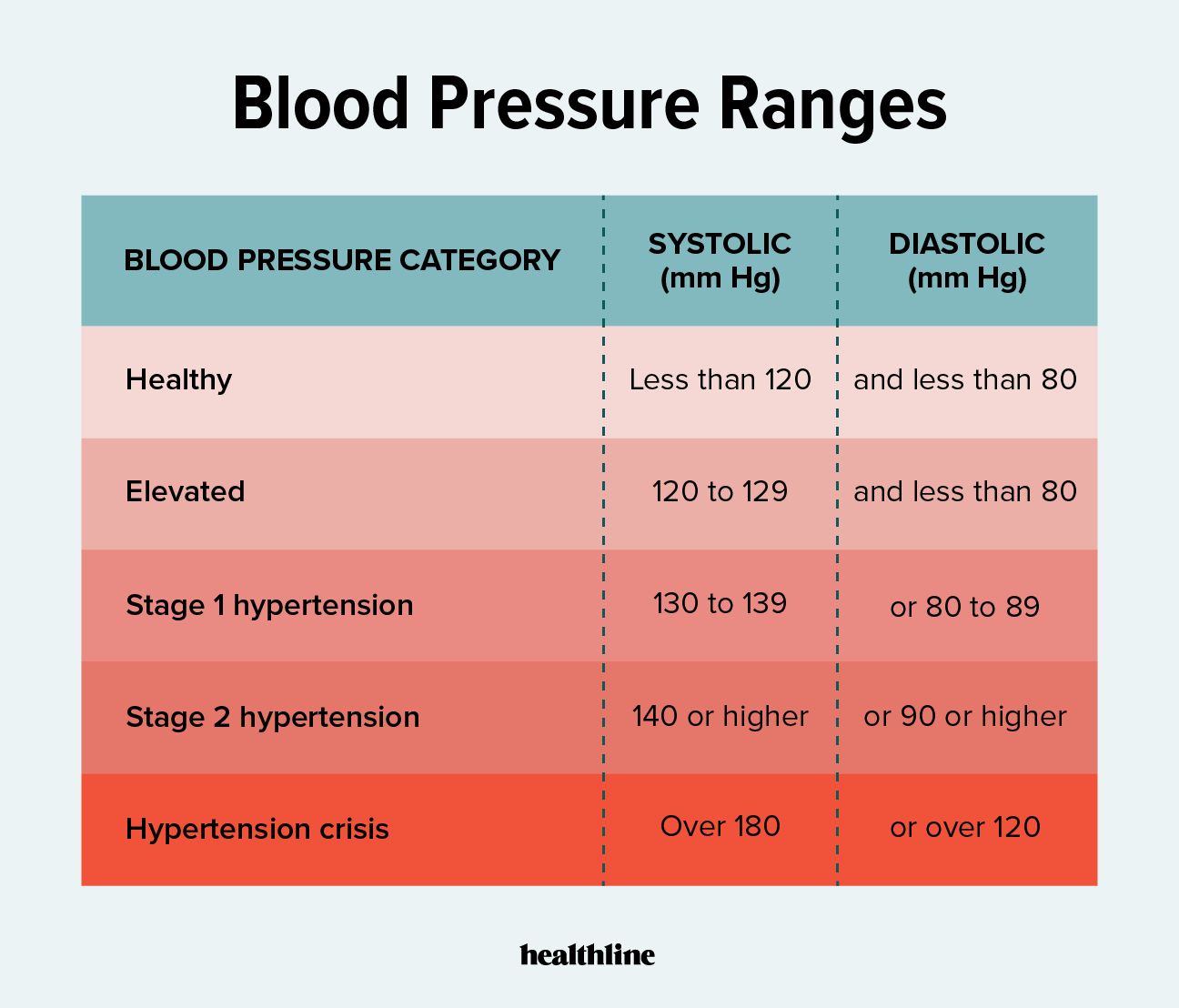
- Normal Blood Pressure: Less than 120/80 mmHg. This indicates a low risk of cardiovascular disease.
- Elevated Blood Pressure: Systolic between 120-129 mmHg and diastolic less than 80 mmHg. At this stage, lifestyle changes are recommended to prevent progression to hypertension.
- Stage 1 Hypertension: Systolic between 130-139 mmHg or diastolic between 80-89 mmHg. This stage requires medical attention and often involves lifestyle modifications and potentially medication.
- Stage 2 Hypertension: Systolic 140 mmHg or higher, or diastolic 90 mmHg or higher. This is a more severe form of high blood pressure that necessitates prompt medical treatment.
- Hypertensive Crisis: Systolic higher than 180 mmHg and/or diastolic higher than 120 mmHg. This is a medical emergency requiring immediate care.
It’s important to note that these categories are guidelines, and a healthcare professional will consider your overall health, age, and other risk factors when interpreting your blood pressure readings.
Factors Influencing Blood Pressure
Your blood pressure is not static; it’s a dynamic measurement that can fluctuate throughout the day and in response to various internal and external factors. Understanding these influences is key to interpreting your readings and identifying potential causes for deviations from your regular baseline.
Physiological Factors
Several inherent bodily processes and conditions can affect blood pressure:
- Heart Rate and Pumping Strength: A faster heart rate or a stronger heart contraction will increase the volume of blood pumped into the arteries per minute, leading to a temporary rise in blood pressure.
- Blood Volume: The total amount of blood circulating in your body plays a significant role. Dehydration can reduce blood volume and thus lower blood pressure, while conditions like fluid retention can increase it.
- Arterial Elasticity: Healthy arteries are flexible and elastic, able to expand and contract with each heartbeat. As arteries stiffen with age or due to conditions like atherosclerosis, they become less compliant, leading to higher blood pressure.
- Blood Viscosity: The thickness or viscosity of your blood can also influence pressure. Thicker blood requires more force to pump.
- Hormonal Regulation: Hormones like adrenaline (epinephrine) and cortisol can cause temporary increases in blood pressure by constricting blood vessels and increasing heart rate. Conversely, hormones like nitric oxide help relax blood vessels, lowering pressure.
Lifestyle and Environmental Factors
Beyond internal physiology, numerous external influences can impact your blood pressure:
- Diet: Sodium intake is a well-established factor. High sodium levels cause the body to retain water, increasing blood volume and thus blood pressure. Conversely, a diet rich in fruits, vegetables, and whole grains, and low in saturated fats, can help regulate blood pressure. Potassium, magnesium, and calcium also play crucial roles in blood pressure regulation.
- Physical Activity: Regular exercise strengthens the heart and improves circulation, generally leading to lower blood pressure over time. However, strenuous exercise can temporarily elevate blood pressure during the activity.
- Stress and Emotions: Acute stress, anxiety, or strong emotions can trigger the release of stress hormones, causing a temporary surge in blood pressure. Chronic stress can contribute to persistently elevated blood pressure.
- Sleep: Inadequate or poor-quality sleep can disrupt the body’s natural blood pressure regulation mechanisms, potentially leading to higher readings.
- Alcohol Consumption: Moderate alcohol intake may have some cardiovascular benefits, but excessive consumption can significantly raise blood pressure.
- Smoking: Nicotine in tobacco products constricts blood vessels and damages their lining, leading to immediate and long-term increases in blood pressure.
- Caffeine: Caffeine can cause a short-term, temporary increase in blood pressure for some individuals.
- Medications: Certain medications, including some decongestants, birth control pills, and nonsteroidal anti-inflammatory drugs (NSAIDs), can affect blood pressure.
- Temperature: Exposure to extreme heat or cold can influence blood pressure. Heat can cause vasodilation (widening of blood vessels), potentially lowering blood pressure, while cold can cause vasoconstriction (narrowing of blood vessels), potentially raising it.
Measuring and Monitoring Your Blood Pressure
Accurate measurement and consistent monitoring are paramount to understanding your regular blood pressure and detecting any concerning trends. This involves understanding how to obtain reliable readings and recognizing the importance of professional guidance.
How to Get an Accurate Reading
To ensure your blood pressure readings are accurate and representative, follow these guidelines:
- Rest Before Measurement: Sit quietly for at least five minutes before taking a reading. Avoid caffeine, alcohol, smoking, and strenuous exercise for at least 30 minutes beforehand.
- Proper Positioning: Sit in a chair with your back supported and your feet flat on the floor. Do not cross your legs.
- Correct Cuff Placement: Ensure the cuff is the correct size for your arm and is placed directly on your bare skin, about one inch above the bend of your elbow. The artery marker on the cuff should align with the brachial artery.
- Arm Position: Rest your arm on a table or armrest at heart level.
- Avoid Talking: Do not talk while your blood pressure is being measured.
- Multiple Readings: Take two to three readings, waiting one to two minutes between each, and average them to get a more reliable measurement.
- Consistent Time: If monitoring at home, try to take your readings at approximately the same time each day.
Home Blood Pressure Monitoring
Home blood pressure monitoring, also known as self-monitoring, is an invaluable tool for understanding your blood pressure outside of the clinical setting. It can provide a more comprehensive picture of your blood pressure patterns throughout the day and night, helping to identify “white-coat hypertension” (higher readings in a doctor’s office) or “masked hypertension” (normal readings in a doctor’s office but high readings at home).
When using a home blood pressure monitor, it is crucial to:
- Choose a Validated Device: Ensure your home monitor has been validated for accuracy by a recognized organization. Upper arm cuff monitors are generally considered more accurate than wrist monitors.
- Follow Device Instructions: Read and understand the operating manual for your specific device.
- Keep a Log: Record your readings, including the date, time, and any relevant notes (e.g., if you felt stressed, had caffeine, etc.). This log will be extremely useful for your doctor.
- Consult Your Doctor: Share your home monitoring log with your healthcare provider. They will interpret the readings in the context of your overall health and advise on further steps.
When to Seek Professional Medical Advice
While home monitoring is beneficial, it is not a substitute for professional medical care. You should consult your doctor if:
- You have consistently elevated readings: If your home readings are regularly above the normal range (e.g., above 130/80 mmHg), even without symptoms, it’s important to get a professional evaluation.
- You experience symptoms: Symptoms such as severe headaches, dizziness, shortness of breath, chest pain, nosebleeds, or vision changes can indicate a hypertensive crisis or other serious condition. Seek immediate medical attention.
- Your blood pressure fluctuates dramatically: Significant and unexplained swings in your blood pressure warrant medical investigation.
- You have underlying health conditions: Individuals with diabetes, kidney disease, heart conditions, or a family history of cardiovascular disease should monitor their blood pressure closely and consult their doctor regularly.
Maintaining a Healthy Blood Pressure
Understanding your regular blood pressure is the first step; maintaining it within a healthy range is the ongoing objective. Fortunately, many lifestyle choices can significantly impact your cardiovascular health and contribute to optimal blood pressure.
Dietary Strategies for Blood Pressure Control
A heart-healthy diet is a cornerstone of blood pressure management. Key dietary considerations include:
- Reduce Sodium Intake: Aim for no more than 2,300 milligrams of sodium per day, and ideally less than 1,500 mg, especially if you have hypertension. Read food labels carefully, as much of our sodium intake comes from processed and packaged foods.
- Increase Potassium Intake: Potassium helps balance sodium levels and relax blood vessel walls. Excellent sources include bananas, sweet potatoes, spinach, beans, and yogurt.
- Emphasize Fruits and Vegetables: These are packed with vitamins, minerals, and fiber that support cardiovascular health. The DASH (Dietary Approaches to Stop Hypertension) diet is a well-researched eating plan that emphasizes these foods.
- Choose Whole Grains: Opt for whole wheat bread, brown rice, and oats over refined grains. Whole grains are rich in fiber and nutrients.
- Lean Protein Sources: Incorporate fish, poultry without skin, beans, and nuts into your diet. Limit red meat and processed meats.
- Healthy Fats: Use olive oil, avocados, and nuts instead of saturated and trans fats found in fried foods and many processed snacks.
- Limit Added Sugars: High sugar intake can contribute to weight gain and inflammation, both of which can negatively impact blood pressure.
The Role of Physical Activity
Regular physical activity is one of the most effective ways to lower and maintain healthy blood pressure.
- Aerobic Exercise: Aim for at least 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity aerobic activity per week. Examples include brisk walking, jogging, swimming, cycling, and dancing.
- Strength Training: Incorporate muscle-strengthening activities at least two days a week. This can help improve your overall metabolism and cardiovascular health.
- Consistency is Key: Regularity is more important than intensity. Find activities you enjoy and can stick with long-term.
- Consult Your Doctor: Before starting any new exercise program, especially if you have existing health conditions, consult your healthcare provider.
Lifestyle Modifications for Long-Term Health
Beyond diet and exercise, several other lifestyle changes can contribute to a healthier blood pressure:
- Stress Management: Chronic stress can wreak havoc on your health. Explore relaxation techniques such as deep breathing exercises, meditation, yoga, spending time in nature, or engaging in hobbies.
- Adequate Sleep: Aim for 7-9 hours of quality sleep per night. Establish a regular sleep schedule and create a conducive sleep environment.
- Weight Management: If you are overweight or obese, losing even a small amount of weight can significantly lower your blood pressure.
- Limit Alcohol: If you drink alcohol, do so in moderation. For women, this means up to one drink per day, and for men, up to two drinks per day.
- Quit Smoking: Smoking is a major risk factor for heart disease and hypertension. Quitting can have immediate and profound positive effects on your blood pressure and overall health.
- Regular Check-ups: Attend all scheduled medical appointments and discuss any concerns about your blood pressure with your doctor. They can provide personalized advice and monitor your progress.
By understanding what your regular blood pressure is, the factors that influence it, and by actively implementing healthy lifestyle strategies, you can take significant steps towards protecting your cardiovascular health and ensuring a longer, healthier life.
