This query, “what is ciprofloxacin good for?”, falls squarely into the realm of medical information and pharmacology. It directly addresses the uses and indications of a specific pharmaceutical compound. Therefore, this article will focus on the medical applications and therapeutic benefits of ciprofloxacin, providing an in-depth understanding for those seeking this specific knowledge.
Understanding Ciprofloxacin: A Powerful Fluoroquinolone Antibiotic
Ciprofloxacin is a synthetic chemotherapeutic agent belonging to the fluoroquinolone class of antibiotics. Its primary mechanism of action involves inhibiting bacterial DNA replication, transcription, repair, and recombination. It achieves this by targeting two essential bacterial enzymes: DNA gyrase (also known as topoisomerase II) and topoisomerase IV. These enzymes are crucial for unwinding and separating bacterial DNA, processes vital for cell division and survival. By blocking their activity, ciprofloxacin effectively halts the growth and proliferation of susceptible bacteria, leading to their death.
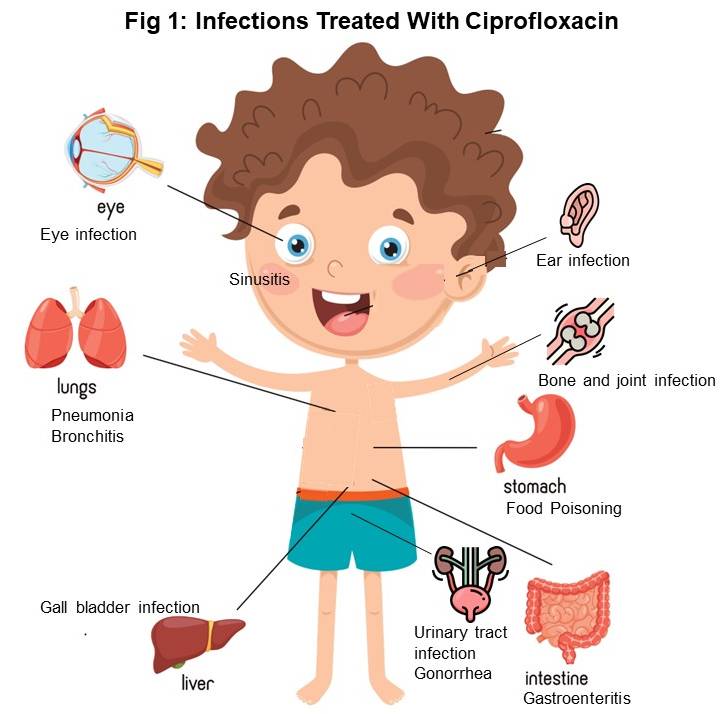
The Broad Spectrum of Activity
One of the key reasons ciprofloxacin is widely prescribed is its broad spectrum of activity against a diverse range of bacterial pathogens. This includes both Gram-positive and Gram-negative bacteria, as well as some atypical organisms. This broad efficacy makes it a valuable tool for treating infections caused by bacteria that are not easily eradicated by other antibiotic classes.
- Gram-Negative Bacteria: Ciprofloxacin is particularly effective against many common Gram-negative pathogens. This includes Escherichia coli (E. coli), a frequent cause of urinary tract infections, traveler’s diarrhea, and other gastrointestinal and systemic infections. It is also potent against Pseudomonas aeruginosa, a notorious opportunistic pathogen often associated with hospital-acquired infections, especially in individuals with weakened immune systems or chronic lung conditions like cystic fibrosis. Other susceptible Gram-negative bacteria include Haemophilus influenzae, Klebsiella pneumoniae, and Salmonella species.
- Gram-Positive Bacteria: While its activity against Gram-positive bacteria is generally less pronounced than against Gram-negative organisms, ciprofloxacin remains effective against certain important Gram-positive pathogens. These include some strains of Staphylococcus aureus (though methicillin-resistant Staphylococcus aureus, or MRSA, is often resistant) and Streptococcus pneumoniae, a common cause of pneumonia and meningitis.
- Atypical Pathogens: Ciprofloxacin also demonstrates activity against certain atypical bacteria, which lack a typical cell wall structure and thus do not respond to many standard antibiotics. This includes Mycoplasma pneumoniae and Chlamydia pneumoniae, which are common causes of respiratory infections.
Mechanism of Action: Targeting Bacterial DNA Synthesis
The precise molecular mechanism by which ciprofloxacin exerts its bactericidal effect is well-understood and central to its therapeutic value.
- Inhibition of DNA Gyrase: In Gram-negative bacteria, DNA gyrase plays a pivotal role in introducing negative supercoils into bacterial DNA. This supercoiling is essential for packaging the large bacterial chromosome within the cell and for facilitating DNA replication and transcription. Ciprofloxacin binds to and inhibits DNA gyrase, preventing it from performing its supercoiling function. This leads to the accumulation of positively supercoiled DNA, which is structurally unstable and disrupts essential cellular processes.
- Inhibition of Topoisomerase IV: In both Gram-negative and Gram-positive bacteria, topoisomerase IV is responsible for decatenation, the process of separating replicated circular DNA molecules. After DNA replication, the two daughter chromosomes are intertwined (catenated). Topoisomerase IV cleaves and rejoins the DNA strands to disentangle them, allowing for proper segregation into daughter cells. Ciprofloxacin also targets and inhibits topoisomerase IV, preventing this crucial separation step. The inability to properly segregate DNA halts cell division and leads to cell death.
Key Indications: Where Ciprofloxacin Shines Therapeutically
Ciprofloxacin’s broad spectrum of activity and potent bactericidal properties make it a first-line or highly effective treatment option for a wide array of bacterial infections. Its efficacy is often determined by the susceptibility of the specific bacterial pathogen involved, which is typically assessed through antibiotic susceptibility testing.
Urinary Tract Infections (UTIs)
Ciprofloxacin is a cornerstone in the management of complicated and uncomplicated urinary tract infections. Its ability to achieve high concentrations in urine and prostatic fluid makes it particularly effective against common uropathogens like E. coli.
- Uncomplicated UTIs: While often reserved for more severe or recurrent cases due to concerns about resistance, ciprofloxacin can be used for uncomplicated UTIs, especially when other agents are not suitable.
- Complicated UTIs: This includes infections involving structural or functional abnormalities of the urinary tract, such as kidney stones, prostatic enlargement, or catheterization. Ciprofloxacin’s broad spectrum is advantageous in these situations as it can cover a wider range of potential pathogens, including Pseudomonas aeruginosa.
- Prostatitis: Inflammation of the prostate gland, often caused by bacterial infection, can be challenging to treat due to the poor penetration of many antibiotics into prostatic tissue. Ciprofloxacin’s excellent penetration into prostatic fluid makes it a highly effective choice for bacterial prostatitis.
Respiratory Tract Infections
While not always the initial choice for all respiratory infections due to evolving resistance patterns and the availability of other effective agents, ciprofloxacin remains a vital treatment for specific types of respiratory infections, particularly those involving Gram-negative bacteria.
- Pseudomonas aeruginosa Pneumonia: In patients with conditions like cystic fibrosis or those who are immunocompromised, Pseudomonas aeruginosa can cause severe pneumonia. Ciprofloxacin is often a critical component of treatment regimens for these infections, sometimes used in combination with other antibiotics.
- Anthrax: Ciprofloxacin is a recommended treatment for inhalational and cutaneous anthrax, caused by Bacillus anthracis. Its effectiveness in eradicating this dangerous pathogen makes it a crucial medication in bioterrorism preparedness.
- Legionnaires’ Disease: Caused by Legionella pneumophila, Legionnaires’ disease is a severe form of pneumonia. Ciprofloxacin is highly effective against Legionella species and is a preferred treatment option.
Gastrointestinal Infections
Ciprofloxacin plays a significant role in treating various bacterial infections of the gastrointestinal tract, particularly those caused by invasive pathogens.
- Shigellosis: Caused by Shigella species, shigellosis is characterized by severe diarrhea, fever, and abdominal cramps. Ciprofloxacin can help shorten the duration of illness and reduce the severity of symptoms by targeting Shigella.
- Salmonellosis (Typhoid and Paratyphoid Fever): Invasive infections caused by Salmonella Typhi and Salmonella Paratyphi (typhoid and paratyphoid fever) are serious systemic illnesses. Ciprofloxacin is a highly effective antibiotic for treating these conditions, particularly in regions where fluoroquinolone resistance is not yet widespread.
- Traveler’s Diarrhea: Ciprofloxacin is often prescribed prophylactically or therapeutically for traveler’s diarrhea, most commonly caused by enterotoxigenic E. coli. It can rapidly alleviate symptoms such as watery diarrhea, abdominal pain, and nausea.
Bone and Joint Infections
Bacterial infections of bones (osteomyelitis) and joints (septic arthritis) can be challenging to treat due to poor blood supply to the affected tissues and the potential for bone destruction. Ciprofloxacin’s excellent penetration into bone and synovial fluid, combined with its broad spectrum, makes it a valuable option.
- Osteomyelitis: It can be used to treat osteomyelitis caused by susceptible bacteria, particularly when Gram-negative organisms are involved.
- Septic Arthritis: Ciprofloxacin can be effective in treating septic arthritis, especially when caused by Gram-negative bacteria or when surgical intervention is not feasible or as an adjunct to surgery.
Other Significant Indications
Beyond the primary categories, ciprofloxacin is indicated for a range of other bacterial infections:
- Infectious Diarrhea: For severe bacterial diarrhea caused by pathogens like Campylobacter species, ciprofloxacin can be an effective treatment.
- Skin and Soft Tissue Infections: While not typically a first-line agent for uncomplicated skin infections due to concerns about resistance, it may be used for specific types of complicated skin and soft tissue infections, especially those involving Gram-negative bacteria or where other options are contraindicated.
- Intra-abdominal Infections: In combination with other agents, ciprofloxacin can be part of the treatment regimen for certain intra-abdominal infections, particularly those involving Gram-negative Enterobacteriaceae.
- Bacterial Conjunctivitis and Corneal Ulcers: Ophthalmic formulations of ciprofloxacin are used to treat bacterial infections of the eye, including conjunctivitis and more serious corneal ulcers.
- Surgical Prophylaxis: In certain surgical procedures, particularly those involving the gastrointestinal tract or where there is a high risk of Gram-negative infections, ciprofloxacin may be used prophylactically to prevent post-operative infections.
Considerations and Precautions: Responsible Use of Ciprofloxacin
Despite its considerable therapeutic benefits, the use of ciprofloxacin is associated with potential side effects and the growing concern of antibiotic resistance. Therefore, its prescription and use require careful consideration and adherence to guidelines.
Adverse Effects and Safety Profile
Like all medications, ciprofloxacin can cause adverse effects, ranging from mild to severe.
- Common Side Effects: These often include gastrointestinal disturbances such as nausea, vomiting, diarrhea, and abdominal pain. Central nervous system effects like headache, dizziness, and restlessness can also occur.
- Serious Side Effects: More serious adverse effects, though less common, necessitate immediate medical attention. These include:
- Tendonitis and Tendon Rupture: Fluoroquinolones, including ciprofloxacin, have a boxed warning for the risk of tendonitis and tendon rupture, which can occur at any time during treatment. The Achilles tendon is most commonly affected.
- Peripheral Neuropathy: Ciprofloxacin can cause nerve damage, leading to symptoms such as pain, burning, tingling, numbness, and weakness, which may be irreversible.
- Central Nervous System Effects: Seizures, psychiatric reactions (e.g., anxiety, confusion, hallucinations, depression), and increased intracranial pressure have been reported.
- Cardiovascular Effects: QT interval prolongation, which can lead to serious heart rhythm abnormalities (torsades de pointes), is a potential concern, particularly in individuals with pre-existing cardiac conditions or those taking other QT-prolonging medications.
- Photosensitivity: Increased sensitivity to sunlight, leading to sunburns, is a common side effect. Patients should be advised to avoid excessive sun exposure and use sunscreen.
- Clostridioides difficile-Associated Diarrhea: Like many antibiotics, ciprofloxacin can disrupt the normal gut flora, leading to an overgrowth of Clostridioides difficile, causing severe diarrhea.
Antibiotic Resistance: A Growing Challenge
The overuse and misuse of antibiotics, including ciprofloxacin, have contributed significantly to the global rise of antibiotic resistance. This phenomenon occurs when bacteria evolve mechanisms to withstand the effects of antibiotics, rendering them ineffective.
- Mechanisms of Resistance: Bacteria can develop resistance to ciprofloxacin through various mechanisms, including mutations in the DNA gyrase and topoisomerase IV genes, alterations in drug efflux pumps that actively expel the antibiotic from the bacterial cell, or modifications in drug permeability.
- Implications of Resistance: The emergence of ciprofloxacin-resistant strains of common pathogens poses a serious threat to public health. It limits treatment options, leads to prolonged illnesses, increases healthcare costs, and can result in higher rates of morbidity and mortality.
- Stewardship and Prudent Use: To combat antibiotic resistance, it is crucial to practice antibiotic stewardship. This involves prescribing ciprofloxacin only when indicated, using the shortest effective duration of therapy, selecting the narrowest spectrum antibiotic that will be effective, and ensuring appropriate dosing. Patient education on completing the full course of antibiotics as prescribed is also vital, even if symptoms improve.
Drug Interactions
Ciprofloxacin can interact with other medications, potentially altering their efficacy or increasing the risk of adverse effects.
- Cations: Ciprofloxacin absorption can be significantly reduced by divalent and trivalent cations, such as those found in antacids (calcium, magnesium, aluminum), iron supplements, and zinc supplements. These medications should ideally be taken at least two hours before or six hours after ciprofloxacin.
- Theophylline: Ciprofloxacin can inhibit the metabolism of theophylline, a medication used for respiratory conditions, leading to potentially toxic levels.
- Warfarin: Ciprofloxacin can potentiate the anticoagulant effect of warfarin, increasing the risk of bleeding.
- Caffeine: Ciprofloxacin can slow the metabolism of caffeine, potentially leading to increased nervousness, insomnia, and heart palpitations.

Conclusion: Ciprofloxacin’s Enduring Role in Modern Medicine
Ciprofloxacin remains a vital and powerful antibiotic in the armamentarium against bacterial infections. Its broad spectrum of activity, potent bactericidal action, and favorable pharmacokinetic properties make it indispensable for treating a wide range of serious infections, particularly those caused by Gram-negative pathogens. From complicated urinary tract infections and severe respiratory illnesses to gastrointestinal infections and bone infections, ciprofloxacin has saved countless lives and continues to be a cornerstone of antimicrobial therapy.
However, its effectiveness is intrinsically linked to responsible use. The growing threat of antibiotic resistance necessitates a vigilant approach to prescribing and patient adherence. Understanding the indications, potential side effects, drug interactions, and the paramount importance of antibiotic stewardship is crucial for maximizing the benefits of ciprofloxacin while minimizing its risks. As medical science advances, ongoing research into new antibiotics and strategies to combat resistance will further shape the landscape of antimicrobial treatment, ensuring that valuable medications like ciprofloxacin continue to serve their critical role in protecting public health for years to come.
