Clostridioides difficile, commonly known as C. diff, is a bacterium that can cause a serious and potentially life-threatening infection of the colon. The infection arises when the normal balance of bacteria in the gut is disrupted, allowing C. diff to overgrow and release toxins. These toxins damage the lining of the colon, leading to inflammation, diarrhea, and other severe symptoms. While C. diff can be found in the environment, it is most commonly associated with healthcare settings, where its spread can be facilitated through contaminated surfaces and inadequate hygiene practices. Understanding the nature of C. diff, its transmission, symptoms, diagnosis, and treatment is crucial for both healthcare professionals and the general public to prevent and manage this challenging infection.
Understanding the Bacterium and Its Mechanisms
-
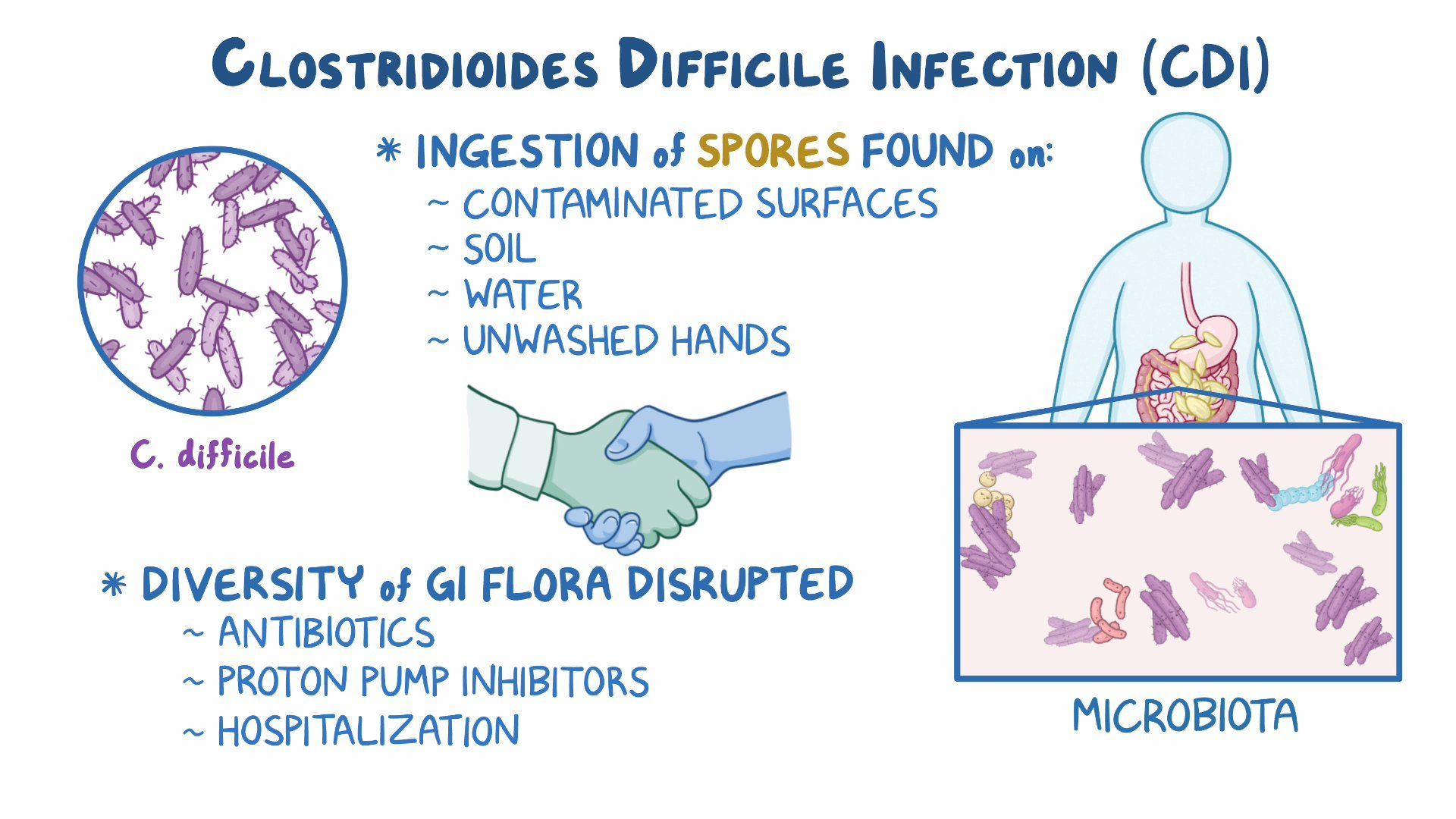
The Nature of Clostridioides difficile: Clostridioides difficile is a Gram-positive, anaerobic, spore-forming bacterium. This means it thrives in environments with low oxygen and can survive for extended periods in the form of spores, which are highly resistant to heat, drying, and disinfectants. These spores are the primary means of transmission. They can be shed in the feces of infected individuals and can persist on surfaces in hospitals and other healthcare facilities for months. Ingesting these spores is what leads to infection.
-
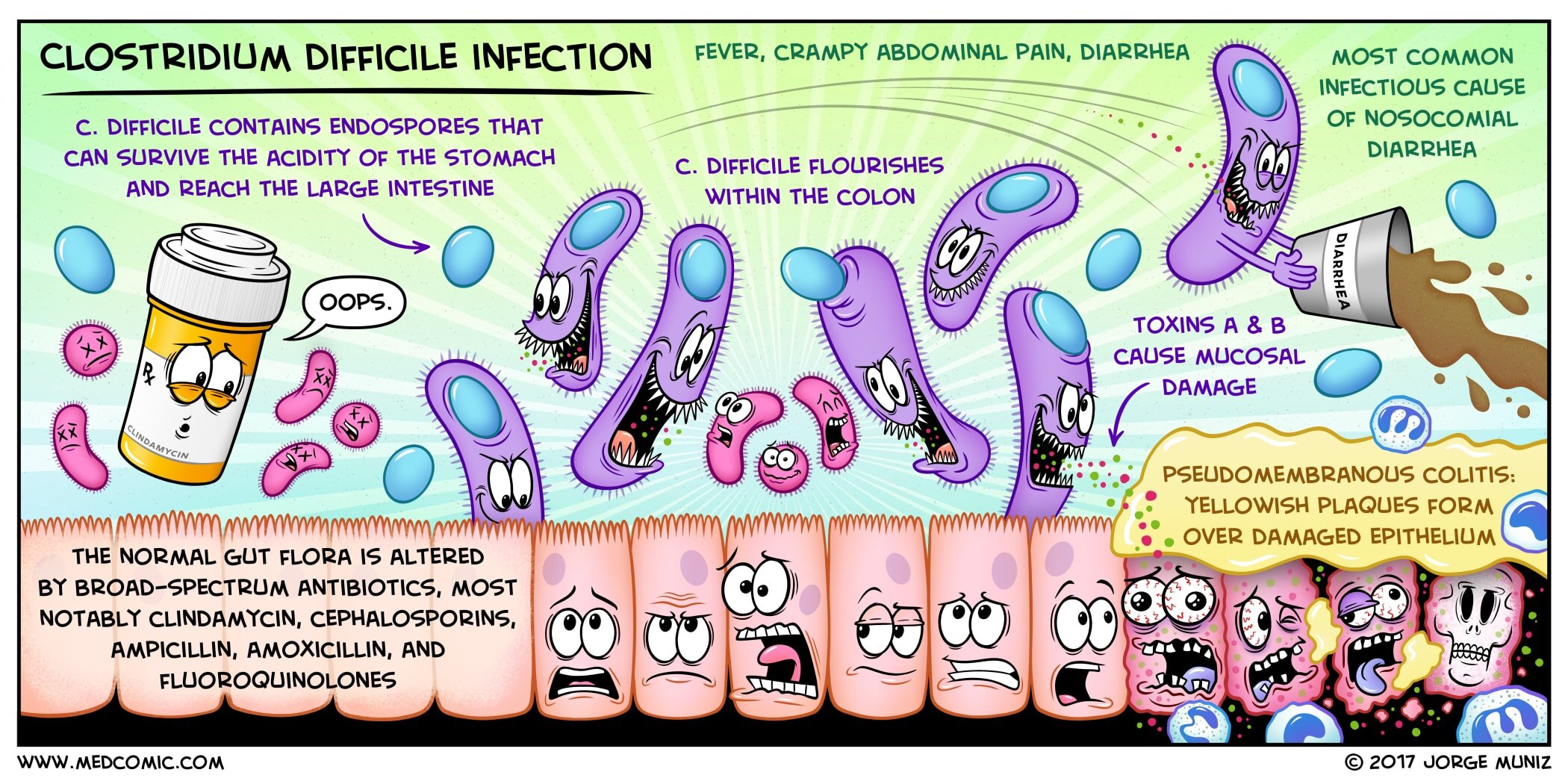
Disruption of Gut Microbiota: The human gut harbors a complex ecosystem of trillions of bacteria, collectively known as the gut microbiota. This diverse community plays a vital role in digestion, nutrient absorption, immune system development, and protection against pathogens. Antibiotics, while essential for treating bacterial infections, are a major disruptor of this delicate balance. Broad-spectrum antibiotics, in particular, can kill off beneficial bacteria that normally keep C. diff in check, creating an opportunity for the opportunistic C. diff to proliferate.
-
Toxin Production and Colonic Damage: Once C. diff spores germinate into active bacteria in the colon, they can produce toxins. The two primary toxins of concern are Toxin A (TcdA) and Toxin B (TcdB). These toxins bind to the cells lining the colon (epithelial cells) and cause damage. TcdA is an enterotoxin, meaning it primarily affects the small intestine and colon, leading to fluid secretion and inflammation. TcdB is a cytotoxin, directly damaging the colonic cells. The combined action of these toxins results in an inflammatory response, characterized by the infiltration of white blood cells and the formation of pseudomembranes – patches of inflammatory cells, fibrin, and dead tissue that adhere to the colon wall. This pseudomembranous colitis is a hallmark of severe C. diff infection.
Transmission Pathways and Risk Factors
-
Healthcare-Associated Infections (HAIs): C. diff is a leading cause of healthcare-associated infections worldwide. Patients in hospitals, nursing homes, and other long-term care facilities are at increased risk due to several factors. These include prolonged stays, the widespread use of antibiotics, underlying health conditions, and the presence of a high concentration of C. diff spores in the environment. Healthcare workers can also inadvertently spread C. diff through inadequate hand hygiene or contaminated equipment.
-
Community-Acquired C. diff: While less common, C. diff infections can also be acquired in the community, outside of healthcare settings. This can occur if an individual comes into contact with C. diff spores in the environment, such as through contaminated food or water, or through close contact with someone who is infected. Individuals who have recently been hospitalized or have taken antibiotics, even within the past few months, can also be at higher risk of developing community-acquired C. diff.
- Key Risk Factors: Several factors significantly increase an individual’s susceptibility to C. diff infection. The most prominent risk factor is the use of antibiotics, especially broad-spectrum agents, as they disrupt the gut’s natural defenses. Advanced age (over 65) is another significant risk factor, as the gut microbiota tends to become less resilient with age. Weakened immune systems, due to conditions like cancer, HIV, or immunosuppressant medications, also make individuals more vulnerable. Previous C. diff infection significantly increases the risk of recurrence. Finally, gastrointestinal surgery or procedures that affect the colon can alter the gut environment and increase susceptibility.
Recognizing the Symptoms and Complications
-
Common Symptoms: The most prevalent symptom of C. diff infection is diarrhea, which can range from mild and watery to severe and bloody. The diarrhea is often frequent and may be accompanied by abdominal cramping and pain. Other common symptoms include fever, loss of appetite, nausea, and a general feeling of being unwell. The severity of symptoms can vary widely, from mild discomfort to life-threatening illness.
-
Severe Complications: In some cases, C. diff infection can lead to serious and life-threatening complications. Pseudomembranous colitis, as mentioned earlier, is a severe inflammation of the colon characterized by the formation of pseudomembranes. This can lead to significant pain, fever, and impaired colonic function. A more severe form of C. diff infection is toxic megacolon, where the colon becomes severely dilated and inflamed, potentially leading to perforation. Bowel perforation, a hole in the colon wall, is a surgical emergency that can lead to peritonitis and sepsis. Sepsis, a life-threatening response to infection, can occur if C. diff bacteria or their toxins enter the bloodstream. Dehydration is also a significant concern due to severe diarrhea and can lead to electrolyte imbalances.
-
Recurrent Infections: A significant challenge with C. diff is the high rate of recurrence. Approximately 20-30% of individuals who experience a primary C. diff infection will develop a recurrent infection within weeks or months. This recurrence is often attributed to incompletely cleared spores or a persistent disruption of the gut microbiota, making it difficult for the beneficial bacteria to re-establish themselves and suppress C. diff regrowth. Recurrent infections can be more severe and lead to a greater risk of complications.
Diagnosis and Treatment Strategies
-
Diagnostic Methods: Diagnosing C. diff infection typically involves stool testing. Nucleic acid amplification tests (NAATs) are highly sensitive and can detect the genetic material of C. diff quickly. Enzyme immunoassay (EIA) tests can detect the presence of C. diff toxins, which is crucial for confirming active infection and the potential for severe illness. In some cases, especially when complications like toxic megacolon are suspected, a colonoscopy may be performed to visualize the colon and obtain biopsies for examination.
-
Antibiotic Therapy: The cornerstone of C. diff treatment is the discontinuation of the offending antibiotic (if applicable) and the initiation of specific antibiotics designed to target C. diff. Historically, vancomycin (oral administration) and metronidazole have been the primary treatment options. However, fidaxomicin, a newer antibiotic, has shown superior efficacy in preventing recurrence and is increasingly being used, particularly for initial or recurrent infections. The duration of antibiotic therapy typically ranges from 10 to 14 days, depending on the severity of the infection and the chosen medication.
-
Addressing Recurrent Infections: Managing recurrent C. diff infections requires a more nuanced approach. In addition to standard antibiotic therapies, fecal microbiota transplantation (FMT) has emerged as a highly effective treatment for recurrent C. diff. FMT involves transplanting stool from a healthy donor into the patient’s colon, typically via colonoscopy, enema, or nasogastric tube. This procedure aims to restore a healthy and diverse gut microbiota, which can effectively suppress C. diff colonization and prevent future recurrences. Other strategies for preventing recurrence include prolonged courses of vancomycin or fidaxomicin, as well as the use of newer investigational therapies.
-
Prevention and Infection Control: Preventing the spread of C. diff is paramount, especially in healthcare settings. Rigorous hand hygiene with soap and water is essential, as alcohol-based hand sanitizers are not effective against C. diff spores. Healthcare facilities must implement strict environmental cleaning and disinfection protocols to eliminate spores from surfaces. Patients with suspected or confirmed C. diff infection should be placed in contact precautions, which involve the use of gowns and gloves by healthcare personnel. Judicious use of antibiotics and prompt identification and isolation of infected patients are also critical in curbing C. diff outbreaks.
