Bone marrow, a spongy tissue found within bones, plays a critical role in our body’s health and survival. It is a dynamic organ, constantly producing new cells and adapting to the body’s needs. While often discussed as a singular entity, bone marrow actually exists in two primary forms: red bone marrow and yellow bone marrow. Understanding the distinctions between these two types is fundamental to grasping their respective functions and their impact on overall physiological well-being.
The Genesis and Evolution of Bone Marrow Types
The differentiation between red and yellow bone marrow is not static; it’s a process that evolves throughout an individual’s lifespan. This transformation is driven by changing metabolic demands and the body’s growth and development.
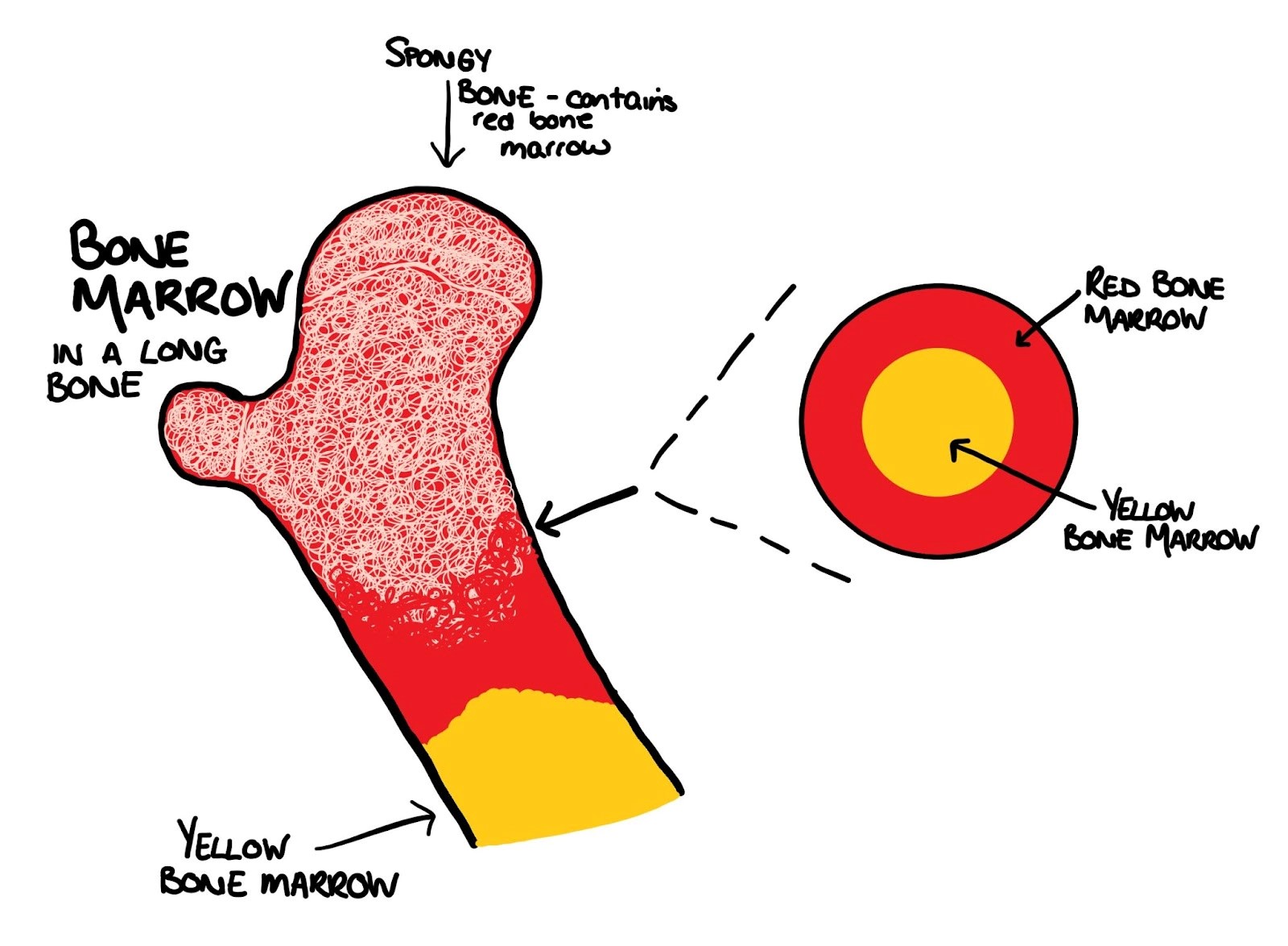
From Red to Yellow: A Lifelong Transition
From birth, the majority of our bone marrow is red. This red marrow is the powerhouse of hematopoiesis, the process of blood cell formation. It is rich in hematopoietic stem cells, which have the remarkable ability to differentiate into all types of blood cells: red blood cells, white blood cells, and platelets. As we age, however, the proportion of red bone marrow gradually decreases, particularly in the long bones of our limbs. This transition is a natural and expected phenomenon.
The shift from red to yellow marrow is primarily due to the replacement of hematopoietic tissue with adipose tissue, or fat. This doesn’t mean the red marrow disappears entirely; it becomes concentrated in specific areas of the skeleton. The conversion is a testament to the body’s efficiency, as the demand for extensive blood cell production diminishes with maturity.
The Distinct Roles of Red and Yellow Bone Marrow
The functional differences between red and yellow bone marrow are directly related to their cellular composition and the physiological needs they serve.
Red Bone Marrow: The Blood Cell Factory
Red bone marrow is characterized by its vibrant color, owing to the high concentration of red blood cells and the blood vessels that supply it. Its primary function is hematopoiesis, the continuous production of essential blood components.
Hematopoiesis: The Core Function
Within the intricate network of red bone marrow reside hematopoietic stem cells (HSCs). These multipotent stem cells are the precursors to all blood cell lineages. Under the influence of various growth factors and cytokines, HSCs differentiate into myeloid and lymphoid progenitors.
- Erythropoiesis: The production of red blood cells (erythrocytes) is a major output of red bone marrow. Red blood cells are crucial for oxygen transport throughout the body. The process involves several stages, from erythroblasts to reticulocytes, before maturing into functional erythrocytes.
- Leukopoiesis: Red bone marrow is also responsible for generating all types of white blood cells (leukocytes), which are vital for the immune system’s defense against pathogens. This includes neutrophils, eosinophils, basophils, monocytes, and lymphocytes (although some lymphocytes mature outside the bone marrow).
- Thrombopoiesis: The production of platelets (thrombocytes) also occurs in red bone marrow. Platelets are essential for blood clotting, preventing excessive bleeding after injury.
Location and Accessibility
In adults, red bone marrow is primarily found in the flat bones of the skeleton, such as the sternum (breastbone), ribs, vertebrae (spine), pelvis, and the ends of long bones (epiphyses) like the femur (thigh bone) and humerus (upper arm bone). These locations are strategically important, providing a protected and accessible site for continuous blood cell production. The relative abundance of red marrow in these areas is crucial for maintaining adequate blood counts throughout life.
Yellow Bone Marrow: A Reserve and Energy Source
Yellow bone marrow, as its name suggests, has a yellowish hue due to its high fat content. While it does not actively participate in blood cell production in the same way as red marrow, it serves important complementary roles.
Adipose Tissue and Energy Storage
The predominant component of yellow bone marrow is adipose tissue, which consists of adipocytes (fat cells). This stored fat serves as a significant energy reserve for the body. In times of prolonged fasting or increased energy demand, the body can mobilize these fat stores to release energy. This function becomes particularly important during periods of starvation or significant illness when nutritional intake is compromised.
Potential for Red Marrow Conversion
A crucial aspect of yellow bone marrow’s function is its potential to revert to red bone marrow under certain circumstances. If the body experiences significant blood loss or increased demand for blood cell production (e.g., during severe anemia or after chemotherapy), yellow bone marrow can be stimulated to convert back into red bone marrow. This remarkable plasticity allows the body to augment its blood-producing capacity when critically needed.
Supportive and Mechanical Roles
The fatty matrix of yellow bone marrow also contributes to the structural integrity and mechanical properties of bones. It acts as a cushioning agent and can help to absorb shock, protecting the bone from damage.
Distribution in Adults
In adults, yellow bone marrow predominantly occupies the central cavities of the long bones, such as the shafts (diaphyses) of the femur and humerus. As mentioned earlier, this is the site where red marrow has been largely replaced by fat with age.
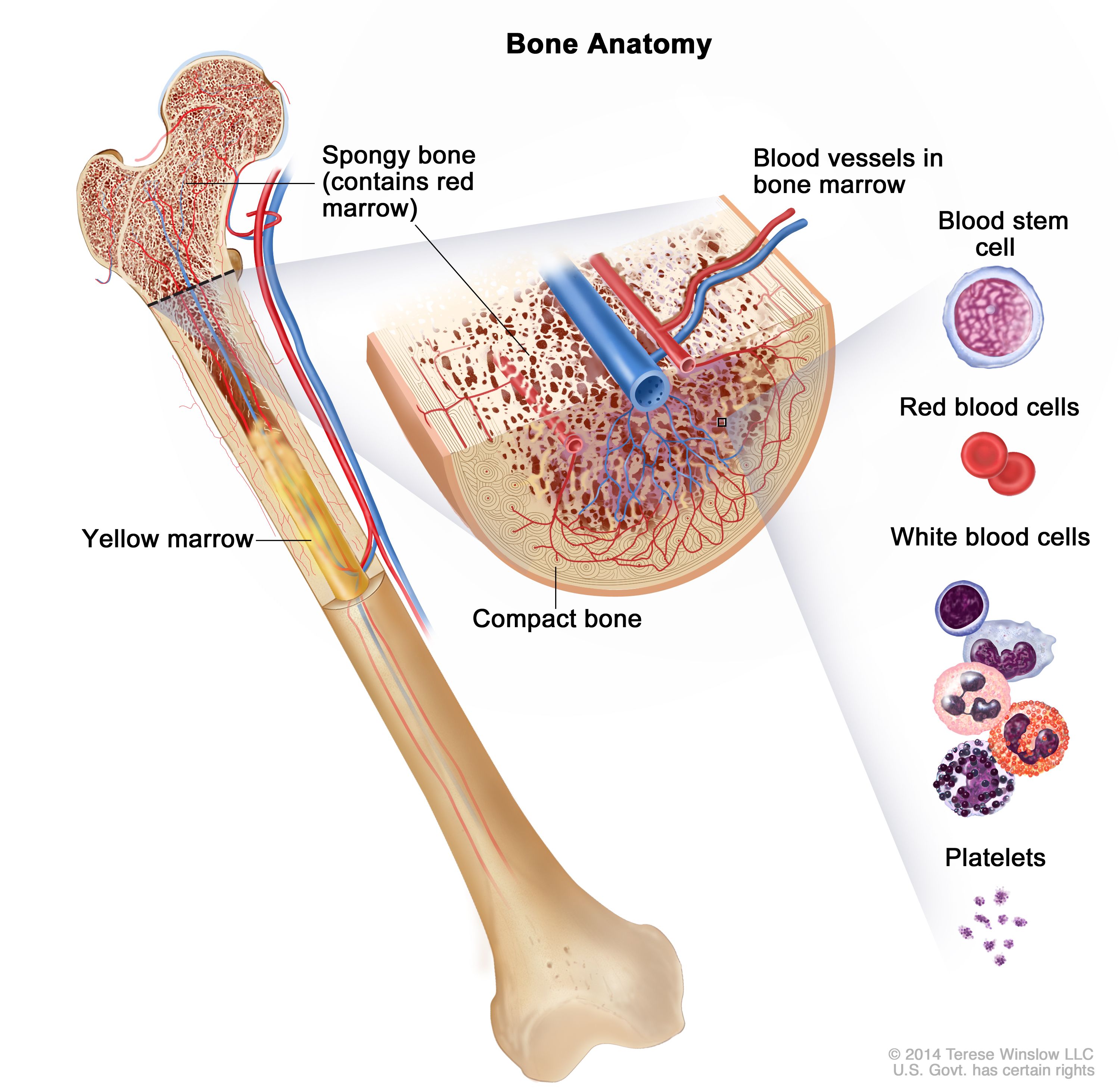
Implications of Bone Marrow Types in Health and Disease
The distinct characteristics and functions of red and yellow bone marrow have significant implications for various physiological processes and can be indicative of underlying health conditions.
Hematological Disorders and Bone Marrow Function
Disruptions in bone marrow function are at the heart of many hematological disorders.
Leukemia and Myelodysplastic Syndromes
Diseases like leukemia involve the uncontrolled proliferation of abnormal white blood cells originating in the bone marrow. This overgrowth can crowd out normal hematopoietic cells, impairing the production of red blood cells, healthy white blood cells, and platelets, leading to anemia, increased susceptibility to infection, and bleeding tendencies. Similarly, myelodysplastic syndromes (MDS) are a group of blood cancers where the bone marrow doesn’t produce enough healthy blood cells.
Anemia and Bone Marrow Failure
Anemia, a deficiency in red blood cells or hemoglobin, can arise from various causes, including insufficient production by the bone marrow. Conditions like aplastic anemia involve the failure of the bone marrow to produce all types of blood cells. Investigating bone marrow function, often through a biopsy, is a crucial diagnostic step in understanding and treating such conditions.
Bone Marrow Transplantation
Bone marrow transplantation (also known as stem cell transplantation) is a life-saving procedure used to treat various cancers and blood disorders. In this procedure, diseased or damaged bone marrow is replaced with healthy stem cells, either from the patient or a donor. The transplanted stem cells then engraft in the recipient’s bone marrow and begin to produce healthy blood cells. The success of these transplants hinges on the regenerative capacity of hematopoietic stem cells, which are primarily found in red bone marrow.
The Role of Fat in Yellow Bone Marrow
The presence of adipose tissue in yellow bone marrow is not merely a passive storage mechanism.
Metabolic Syndrome and Bone Marrow Adiposity
Emerging research suggests a potential link between increased bone marrow adiposity (excessive fat in the yellow bone marrow) and metabolic disorders like obesity and type 2 diabetes. While the exact mechanisms are still being elucidated, it is hypothesized that increased fat accumulation within the bone marrow could disrupt local microenvironments, potentially impairing hematopoietic stem cell function and contributing to systemic inflammation.
Nutritional Status and Bone Marrow Reserve
The fat stored in yellow bone marrow represents a vital energy reserve. Individuals with poor nutritional status or prolonged periods of caloric restriction may experience a decrease in yellow bone marrow volume as the body utilizes its fat stores. Conversely, in conditions of severe obesity, bone marrow adiposity can be significantly increased.
Diagnostic Procedures Involving Bone Marrow
The examination of bone marrow is a cornerstone in the diagnosis and management of a wide array of hematological and oncological conditions.
Bone Marrow Aspiration and Biopsy
A bone marrow aspiration and biopsy are two procedures that are often performed together to obtain samples of bone marrow for laboratory analysis. These procedures typically involve inserting a needle into a bone, most commonly the posterior iliac crest (back of the hip bone), to extract a liquid sample (aspiration) and a small core of tissue (biopsy).
What is Assessed?
Pathologists examine these samples under a microscope to evaluate the cellularity of the marrow, the presence and proportion of different blood cell precursors, and to identify any abnormal cells or infiltrates.
- Cellularity: This refers to the proportion of hematopoietic cells to fat cells in the bone marrow. In healthy adults, the cellularity of red bone marrow is typically between 30-70%, decreasing with age.
- Differential Count: This involves counting the different types of immature and mature blood cells present. Deviations from normal ranges can indicate specific diseases.
- Morphology: The shape and appearance of the cells are meticulously scrutinized for abnormalities that may suggest malignancy or other disorders.
- Cytogenetics and Molecular Studies: Advanced tests can be performed on bone marrow cells to detect chromosomal abnormalities or specific gene mutations that are characteristic of certain blood cancers.
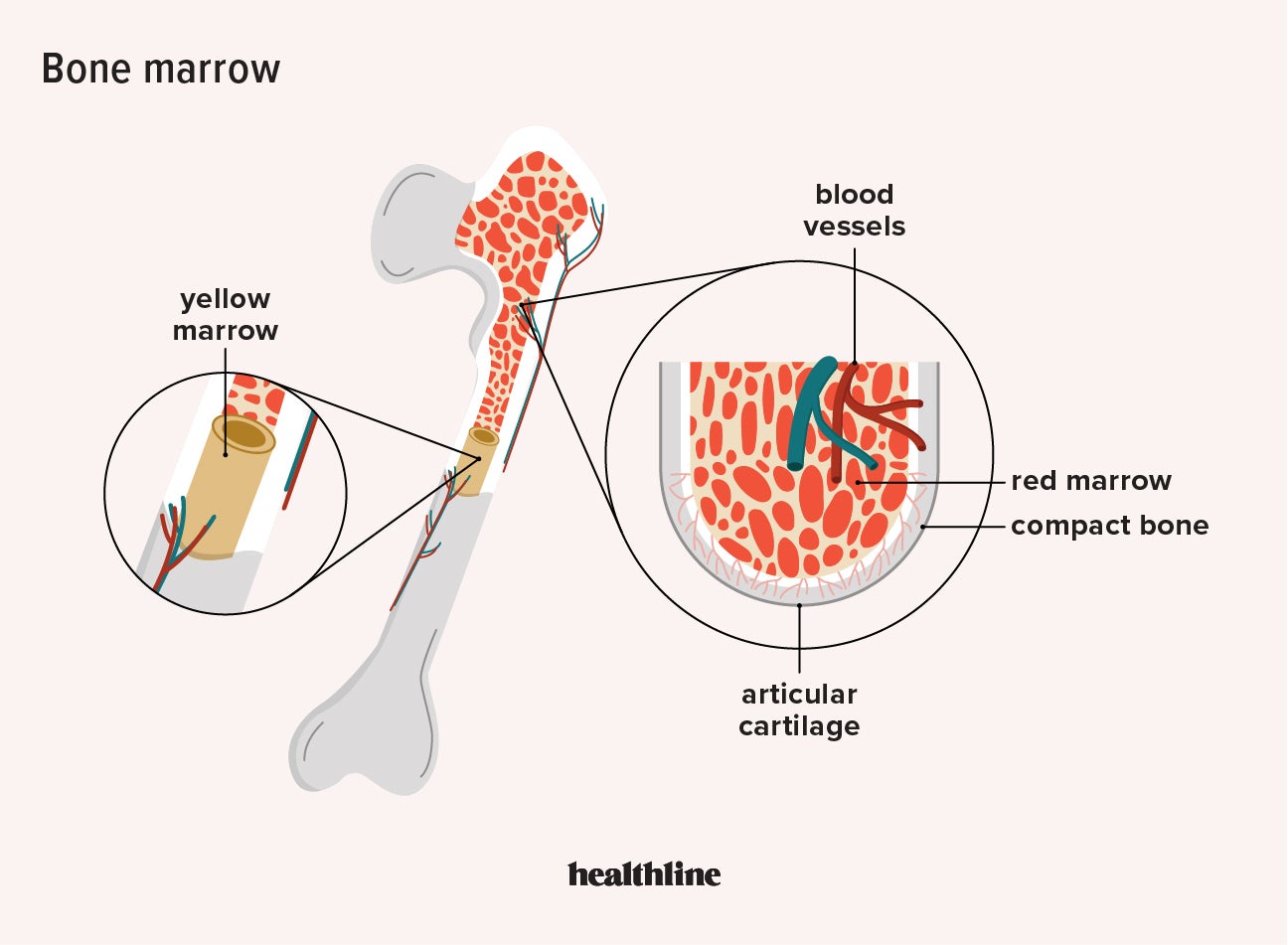
Interpreting Bone Marrow Findings
The interpretation of bone marrow findings is complex and requires specialized expertise. The findings from an aspiration and biopsy, when correlated with a patient’s clinical presentation and other laboratory tests, provide crucial information for diagnosis, prognosis, and treatment planning. For example, an increased number of blast cells in the bone marrow is a hallmark of acute leukemia. Conversely, a hypocellular marrow with a predominance of fat cells might suggest aplastic anemia or recovery from chemotherapy.
In conclusion, the distinction between red and yellow bone marrow is fundamental to understanding hematopoiesis, energy metabolism, and bone health. Red bone marrow, the active site of blood cell production, is crucial for oxygen transport, immunity, and hemostasis. Yellow bone marrow, rich in fat, serves as an energy reserve and possesses the remarkable ability to transform into red marrow when needed. The interplay between these two forms of marrow is a sophisticated biological process that underpins our overall health and resilience.
